Clinical Medical
Reviews and Case Reports
HIV-Infected Patient with Refractory Giardiasis and Lingua Villosa Nigra: A Case Report
Nina Yancheva1*, Nina Tsvetkova2, Maria Nikolova2, Ivo Alexiev2 and Tatyana Tchervenyakova1
1Department for Acquired Immune Deficiency, Medical University, Sofia, Bulgaria
2National Center of Infectious and Parasitic Disease, Sofia, Bulgaria
*Corresponding author: Nina Yancheva, Department for Acquired Immune Deficiency, SHATIPB "Prof.Ivan Kirov", Medical University, blvd. Akademik Ivan Geshov, 17, Sofia, Bulgaria, E-mail: dr.yancheva@abv.bg
Clin Med Rev Case Rep, CMRCR-3-126, (Volume 3, Issue 8), Case Report; ISSN: 2378-3656
Received: June 09, 2016 | Accepted: August 19, 2016 | Published: August 22, 2016
Citation: Yancheva N, Tsvetkova N, Nikolova M, Alexiev I, Tchervenyakova T (2016) HIVInfected Patient with Refractory Giardiasis and Lingua Villosa Nigra: A Case Report. Clin Med Rev Case Rep 3:126. 10.23937/2378-3656/1410126
Copyright: © 2016 Yancheva N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Giardia lamblia is a protozoan parasite that can cause diarrhea in both HIV-positive and HIV-negative patients. The most frequent complaints associated with Giardia infection are loose, bulky, frothy and/or greasy stool with the absence of blood or mucus, flatulence, bloating, anorexia, cramps and foul belching. We report the case of a 34-year-old HIV-infected male patient with refractory giardiasis. He had two relapses of giardiasis with nausea, loss of appetite, diarrhea, bloating, foul belching and weight loss. An interesting finding from the physical exam of the patient was the presence of lingua villosa nigra during the second relapse of giardiasis. The patient was treated consecutively with Metronidazole, Albendazole and again Metronidazole. After the final course with Metronidazole, the patient was treated successfully and his tongue returned to normal.
Keywords
Giardia lamblia, HIV, Lingua villosa nigra
Introduction
Giardia lamblia is a protozoan parasite that colonizes the upper portions of the small intestine. It is the most common protozoan isolated from human stools and can cause diarrhea and intestinal malabsorption in both HIV-positive and HIV-negative patients [1-4]. The prevalence rate of diarrhea caused by Giardia lamblia in AIDS patients is higher than in those without AIDS, due to humoral immune defect in AIDS patients [5].
The drug of choice for the treatment of giardiasis is Metronidazole (cure rates approximately 85%) [6]. Other effective drugs include: quinacrine, tinidazole, furazolidone, albendazole and paramomycin [7].
There are several causes of treatment failures: reinfection, inadequate drug levels, immunosuppression, resistance to the drug, sequestration in the gallbladder or pancreatic ducts and unknown reasons [8]. Relapse may be found in AIDS patients. Combination of two or more drugs for a longer duration is the treatment modality to treat refractory giardiasis [7,8].
Case Presentation
We present a 34-year-old HIV- infected MSM, diagnosed in April 2014 in the stage of primary HIV infection. The patient's first CD4 T cell count was 793 cells/μL and the plasma level of HIV RNA was 105 000 000 copies/μl. We followed up the patient every 4 months. He had giardiasis diagnosed in December 2015 on the occasion of the sudden onset of the next complaints: nausea, loss of appetite, watery diarrhea, bloating, foul belching and weight loss of 4 kg for 7 days. The physical examination revealed dehydration symptoms of the second grade, as well the mild abdominal tenderness. The patient's CD4 T cell count was 484 cells/μL and the plasma level of HIV RNA was 396,448 copies/μl. The laboratory examinations revealed leukocytosis again (WBc were 12 G/l) and no other abnormalities. The Diagnosis of giardiasis was confirmed by two methods: morphodiagnostic test - finding cysts in feces and immunofluorescence assay (IFA) of the feces. The patient received a 7-day course of oral Metronidazole, 750 mg given t.i.d. After the treatment the symptoms resolved and the examination of stool samples and IFA became negative.
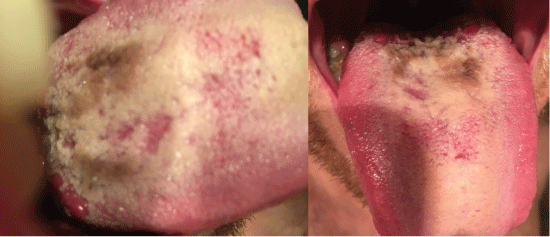
In January 2016 the patient had similar complaints: nausea, loss of appetite, mushy diarrhea, bloating and belching. The physical examination revealed a black discoloration of the tongue - lingua villosa nigra (Figure 1). The throat culture was negative. The patient did not smoke or use oral tobacco products, and he was not taking any bismuth-containing compounds or antibiotics.
.
Figure 1: Lingua villosa nigra in HIV-infected patients with refractory giardiasis.
View Figure 1
The patient was treated with oral albendazole, 400 mg given q.d. for 7 days because of recurrent symptoms and repeatedly positive results of IFA and examinations of stool samples. The symptoms improved, but the stool samples were positive for Giardia after treatment. In February 2016, he received a 14-day course of oral Metronidazole, 750 mg given t.i.d., and started highly active aniretroviral therapy (HAART). The HAART regimen includes tenofovir (TDF) plus emtricitabine (FTC) plus boosted darunavir (DRV/r). After the treatment with Metronidazole and one month antiretroviral therapy diarrhea had resolved and the patient was gaining weight. His tongue returned to normal. Results of stool samples for cysts and IFA became negative in March 2016. Despite having received regimen of HAART, the patient's CD4 cell count decreased to 445 cells/μL, probably associated with a co-infection with Giardia. The plasma level of HIV RNA, however decreased significantly to 1224 copies/μl.
Discussion
Giardiasis are relatively common in homosexual populations [3,5]. HIV-infected patients with low CD4 counts who are infected with Giardia develop severe and sometimes life-threatening disease. Although B cell dysfunction has traditionally been thought to increase both susceptibility to infection with Giardia and the rate of treatment failure, more recent evidence indicates that T cells may be important [9,10].
The presented patient is in the second stage of HIV infection. Most of the observed symptoms in the patient are characteristic of giardiasis. But the patient had also a symptom, not very specific for the disease - lingua villosa nigra. This is a benign condition characterised by a hair-like coating on the dorsum of the tongue. Various etiological factors have been associated with this condition - chronic tobacco, social habits such as heavy drinking of coffee, tea, use of mouthwashes, drugs like oral erythromycin, topical or systemic antibiotics and steroids [11]. Bacterial and fungal overgrowth have also been thought to play a role [12]. We excluded these etiological factors in our patient and we consider that the condition is most likely associated with giardiasis.
Initially the patient was treated with Metronidazole and the infection was temporarily eradicated. Other potentially useful drugs were used - Albendazole has known for its in vitro and in vivo efficacy in the treatment of patients with giardiasis [13,14]. However, although at the time when the symptoms were suppressed, the microscopic stool examination remained positive. The second course of treatment with Metronidazole was more continuous continued and efficient. We consider that starting HAART and decreasing of the viral load of HIV plays also an important role in the effective treatment of giardiasis.
Disclosure
The authors state that they have no conflict of interest directly relevant to the content of this article.
References
-
Angarano G, Maggi P, Di Bari MA, Larocca AM, Congedo P, et al. (1997) Giardiasis in HIV: a possible role in patients with severe immune deficiency. Eur J Epidemiol 13: 485-487.
-
Chavan N, Chavan S (2014) Intestinal parasitic infections in HIV infected patients. Int J Curr Microbiol App Sci 3: 265-270.
-
Feitosa G, Bandeira AC, Sampaio DP, Badaró R, Brites C (2001) High prevalence of giardiasis and stronglyloidiasis among HIV-infected patients in Bahia, Brazil. Braz J Infect Dis 5: 339-344.
-
Hill D, Nash T (1999) Intestinal flagellate and ciliate infections. In: Guerrant RL, Walker DH, Weller PF, Tropical infectious diseases: principles, pathogens, and practice. Churchill Livingstone, Philadelphia p, 703-712.
-
Moolasart P (1999) Giardia lamblia in AIDS patients with diarrhea. J Med Assoc Thai 82: 654-659.
-
Lopez-Velez R, Batlle C, Jiménez C, Navarro M, Norman F, et al. (2010) Short Course Combination Therapy for Giardiasis after Nitroimidazole Failure. Am J Trop Med Hyg 83: 171-173.
-
Nash TE, Ohl CA, Thomas E, Subramanian G, Keiser P, et al. (2001) Treatment of Patients with Refractory Giardiasis. Clin Infect Dis 33: 22-28.
-
8. Yadav P, Tak V, Mirdha BR, Makharia GK (2014) Refractory giardiasis: A molecular appraisal from a tertiary care centre in India. Ind J Med Microb 32: 378-382.
-
Janoff EN, Smith PD, Blaser MJ (1988) Acute antibody responses to Giardia lamblia are depressed in patients with AIDS. J Infect Dis 157: 798-804.
-
Singer SM, Nash TE (2000) T-cell-dependent control of acute Giardia lamblia infections in mice. Infect Immun 68: 170-175.
-
Motallebnejad M, Babaee N, Sakhdari S, Tavasoli M (2008) An epidemiologic study of tongue lesions in 1901 Iranian dental outpatients. J Contemp Dent Pract 9: 73-80.
-
Yuca K, Calka O, Kiroglu AF, Akdenix N, Cankaya H (2004) Hairy tongue: A case report. Acta Otorhinolaryngol Belg 58: 161-163.
-
Edlind TD, Hang TL, Chakraborty PR (1990) Activity of the anthelmintic benzimidazoles against Giardia lamblia in vitro. J Infect Dis 162: 1408-1411.
-
Meloni BP, Thompson RC, Reynoldson JA, Seville P (1990) Albendazole: a more effective antigiardial agent in vitro than metronidazole or tinidazole. Trans R Soc Trop Med Hyg 84: 375-379.





