International Archives of Urology and Complications
Anatomic, Clinical and Therapeutic Aspects of Circumcision Accidents in Yaounde, Cameroon
Mouafo Tambo FF1*, Ditope JJ1, Fossi G1, Fadi S1, Nyanit Bob D1, Mbouche L1, Andze OG1 and Sosso MA2
1Pediatric Surgery Service, Yaoundé Gynaeco-Obstetric and Pediatric Hospital (YGOPH), Cameroon
2Department of surgery and specialties, Faculty of Medicine and Biomedical Sciences, University of Yaoundé I, Cameroon
*Corresponding author: Pr Mouafo Tambo Faustin, Pediatric Surgery Service, Yaounde Gynaeco-Obstetric and Pediatric Hospital (YGOPH), PO 4362, Yaounde, Cameroon, Tel: 00237696098325, E-mail: faustintambo@yahoo.fr
Int Arch Urol Complic, IAUC-2-014, (Volume 2, Issue 1), Original Article; ISSN: 2469-5742
Received: March 01, 2016 | Accepted: May 04, 2016 | Published: May 06, 2016
Citation: Mouafo TFF, Ditope JJ, Fossi G, Fadi S, Nyanit BD, et al. (2016) Anatomic, Clinical and Therapeutic Aspects of Circumcision Accidents in Yaounde, Cameroon. Int Arch Urol Complic 2:014. 10.23937/2469-5742/1510014
Copyright: © 2016 Mouafo TFF, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Complications arising from local circumcision methods and practice in our environment need to be taken seriously, as they pose major therapeutic difficulties such as the functional outcome, as well as cosmesis. These complications could, in certain cases, be life threatening.
Objective: The aim of this study was to describe the anatomo-clinical and therapeutic aspects of circumcision misharps at the Yaoundé Gynaeco-Obstetric and Pediatric Hospital (HGOPY).
Methodology: It was a retrospective and descriptive study including all patients aged 0-15 years that were managed for complications related to circumcision over a period of 10 years at the pediatric surgery service of the Yaoundé Gynaeco-Obstetric and Pediatric Hospital (HGOPY).
Results: We recorded 15 treated cases. The average age of the patients was 5.57 years ranging from 7 months to 14 years. The mean interval between circumcision and occurrence of the complication(s) was 10 months 3 hours to 2 years. The reason of the circumcision in all cases was ritual.
The complications were predominantly urethral fistulas (53.3%), followed by total amputation of the glans (13.4%) and/or the penis (6.7%). Surgical procedures performed were: repair of urethral fistula (46.7%), meatoplasty (13.4%), wet dressing (6.7%), buccal mucosal graft uretroplasty (6.7%), refashioning on account of buried penis (6.7%), vesicostomy (6.7%) and hemostasis (6.7%).
Conclusion: Complications arising from the practice of circumcision in our local setup are severe, and major surgical procedures are usually required for their correction in order to remedy to these complications.
Keywords
Circumcision accidents, Anatomo-clinical, Treatment, HGOPY, Yaoundé, Cameroun
Introduction
Circumcision accidents refer to any complications that occur during the surgical removal of the prepuce. These complications are quite common in our daily pediatric surgical practice [1]. In most of our African communities, circumcision is carried out as a ritual, and is often performed by traditional healers and paramedical staff who lack adequate knowledge of anatomy and safe asepsis [1,2]. Although this procedure is considered simple, the complications that can occur are varied and include functional outcome and cosmetic appearance and even life threatening lesions in some occasions [3]. So in the light of the analysis of 15 circumcision accidents treated in the pediatric surgery service of the Yaoundé Gynaeco-Obstetric and Pediatric Hospital HGOPY, we wanted to report our experience in the management of these injuries.
The aim of this study was to describe the anatomic, clinical and therapeutic aspects of circumcision accidents at reference hospital in Yaoundé, Cameroon.
Patients and Methods
This was a retrospective and descriptive study, of all children who presented with complications related to circumcision over a period of 10 years, dating from (September 2005 to September 2015) at the pediatric surgery service of the Yaoundé Gyneco-obstetric and Pediatric hospital. Included in this study were all male children patients aged between 0 to 15 years managed for a circumcision accidents in our center. Excluded from the study were; circumcision accidents that occurred in patients without any indication of circumcision. The parameters retrieved for data collection included age, time to consultation, indication of circumcision, level of qualification of the staff, place of circumcision, HIV serology, lesions observed, surgical treatment and outcome. An anesthetist review was done for each patient. Surgery was performed in an operating theatre under general anesthesia and a psychological support for children and parents was systematic.
![]()
Table 1: Distribution according to the observed lesions.
View Table 1
Results
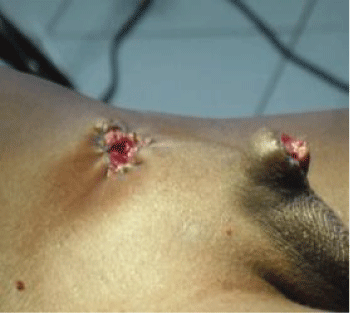
We recorded fifteen cases. The annual frequency was 1.5 cases per year. The average age of patients was 5.5 years, ranging from 7 months to 14 years. The average time to consultation was 41 weeks, ranging from three hours to two years after the circumcision. The indication of the circumcision was ritual for all our patients. Circumcision was performed by a nurse in all cases who happened to be a family relative in 3 patients (20%). The parental home was the most frequent place of circumcision (n = 8), corresponding to 53.3% of our cases, followed by peripheral hospitals in 4 patients (26.7%). In 3 patients (20%) the facility where circumcision was performed could not be retrieved. HIV serology testing was done in only 3 patients and results came back negative. The complications observed are listed in table I. They were largely dominated by urethral fistulas (Figure 1), which accounted for 53.3% (n = 8) of our cases. Table 2 represents the surgical procedures performed. The treatment offered varied, from simple wet dressing, vesicostomy (Figure 2) to buccal mucosa flap urethroplasty. Morbidity in our series was associated to recurrence of urethral fistulas (n = 2) and poor aesthetic results. No deaths were recorded.
.
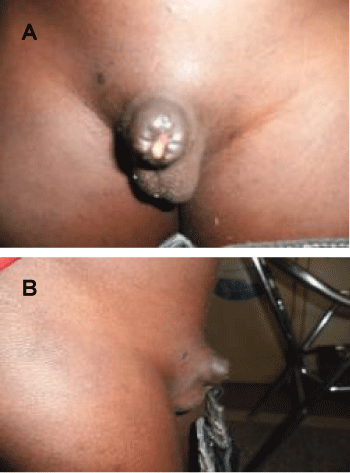
Figure 3: (A) Penile shaft amputation in a 10 years old boy AP view; (B) penile shaft amputation in a 10 years old boy Lateral view.
View Figure 3
![]()
Table 2: Distribution according to the surgical treatment and indications.
View Table 2
Discussion
The hospital frequency of 1.5 cases of circumcision accidents per year reported in our study does not reflect the reality in our setting since many of these accidents occur outside of hospitals and are not registered. The mean age patient in our series was 5.5 years (7 months to 14 years). In 2006, Okeke et al. [4] in Nigeria reported 9.3% of circumcision accidents in children aged from 8 days to 13 months. The lesions were dominated by fistulas in our study, which accounted for more than half of the cases. This finding is consistent with the findings of other African authors [2,5,6]. Total or partial amputations of the glans and/or the penile shaft (Figure 3) were not uncommon in our study (n = 3) and can be explained by the lack of knowledge of anatomy and the use of inadequate anesthesia during the procedure. In addition, the circumcision was usually carried out at home. These amputations affect the functional outcome of the penis and urethra. They are an indication of phalloplasty. It is challenging procedure and we lack this experience in our center. On the other hand, post-circumcision bleeding might sometimes requires blood transfusion. Ahmed A et al. [7] in Nigeria reported 3 cases of post-circumcision penile hemorrhage requiring blood transfusion. Meatal stenosis is a late complication which can occur at any time from the circumcision procedure and might be difficult to be linked to it. Urethral obstruction will result in subsequent distension of the upper urinary tract. Surgical management by meatoplasty is thus urgent in these cases [1,2,5].
Major surgeries are required to correct circumcision accidents, so circumcision should not be considered as an otherwise simple procedure. Hospital circumcisions carried out in an operating room under general anesthesia to ensure healing without sequelae should be encouraged. Further, the negative psychological impact of these complications on children and their families is quite important. Psychological support for the patients and their parents should therefore be part of the management.
Conclusion
Accidents arising from the routine practice of circumcision in our setting are common and could be life threatening on certain occasions. For these reasons, circumcision should be considered as a major surgical procedure. Moreover, these complications are challenging to manage, hence emphasis should be placed on the need for hospital circumcision to be performed by experts, as well as regular supervision of traditional healers and/or paramedical staff who carry out this procedure.
Acknowledgements
We thank the staff and management team of the Yaoundé Gynaeco-Obstetric and Pediatric Hospital.
Ethical Statement
Ethical clearance was obtained from the ethics committee of the Yaoundé Gynaeco-Obstetric and Pediatric Hospital and an informed consent was signed by all the parents or legal tutors of the children.
References
-
Tambo FF (2012) [Circumcision accidents in Yaounde, Cameroon: a report on five cases]. Prog Urol 22: 63-66.
-
Sylla C, Diao B, Diallo AB, Fall PA, Sankale AA, et al. (2003) [Complications of circumcision. Report of 63 cases]. Prog Urol 13: 266-272.
-
Cairns JT (2007) Re: Circumcision: A minor procedure? Paediatr Child Health 2007;12(4):311-2. Paediatr Child Health 12: 612.
-
Okeke LI, Asinobi AA, Ikuerowo OS (2006) Epidemiology of complications of male circumcision in Ibadan, Nigeria. BMC Urol 6: 21.
-
Dieth AG, Moh-Ello N, Fiogbe M, Yao KJ, Tembely S, et al. (2008) [Accidents of circumcision in children in Abidjan, Cote d'Ivoire]. Bull Soc Pathol Exot 101: 314-315.
-
Ikuerowo SO, Bioku MJ, Omisanjo OA, Esho JO (2014) Urethrocutaneous fistula complicating circumcision in children. Niger J Clin Pract 17: 145-148.
-
Ahmed A, Mbibi NH, Dawam D, Kalayi GD (1999) Complications of traditional male circumcision. Ann Trop Paediatr 19: 113-117.