Chronic total coronary occlusions (CTO) are found in approximately 15-30% of patients who undergo coronary angiography for suspected or known coronary artery disease. Speckle Tracking Echocardiography (STE) is a novel technology to assessing modifications of myocardial deformation with higher accuracy than the simple visual of regional wall motion.
The study was to evaluate, using STE applied to dobutamine stress echocardiography (DSE), changes in echo parameters before and after successful recanalization of a CTO.
Eleven patients with subacute or chronic coronary syndromes and angiographic evidence of CTO, scheduled for reopening by percutaneous coronary angioplasty, underwent DSE, using standard protocol, before and 3 months after CTO recanalization. The acquisition of Echo images was performed at baseline and peak stress.
Left ventricular ejection fraction (EF), volumes, wall motion score index, parameters of diastolic flow, tissue velocities at mitral annulus, global longitudinal strain (GLS), strain rate (SR), systolic and diastolic longitudinal functional reserve (SLR and DLR respectively) were obtained at baseline and at peak stress before and after percutaneous coronary angioplasty (PCI).
The mean follow-up after PCI was 3.09 ± 1 months. Statistical analysis showed significant improvement after PCI in EF, comparing to baseline (P < 0.03) and stress peak (P < 0.001) in systolic SR from the 4 chamber-view (P < 0.02), in DLR (P < 0.01), but there were no significant changes for SLR, GLS and SR.
Stress echocardiography associated with new imaging techniques, such as STE provides further improvements of diagnostic accuracy in CTO patients.
Chronic total coronary occlusions, Stress echocardiography, Speckle tracking echo
Chronic total coronary occlusions (CTO) are found in approximately 15-30% of patients who undergo coronary angiography for suspected or known coronary artery disease (CAD) [1]. Current data on the benefits of CTO recanalization are derived only from observational studies; thus, until now, many uncertainties remain about the proper selection of patients for adequate revascularization in order to have clear clinical and functional benefits. Latest evidences suggest that the factors that should be taken into account to guide the choice of CTO treatment include: patient's symptoms on optimal medical therapy, patient's clinical characteristics (age, comorbidity), localization and extension of concomitant CAD, ventricular function, degree of myocardial ischemia on optimal medical therapy and presence of viable myocardium [2].
Diagnostic accuracy of dobutamine stress echo (DSE) for detection of ischemic myocardium has high levels of sensitivity (80%) and specificity (77%) [3]; regarding viable myocardium accuracy detection, sensitivity values are from 71% up to 97% and specificity values from 63% up to 95%, from different experiences available [4]. Therefore, information obtained by this method is well correlated with those derived from other non-invasive diagnostic imaging techniques.
Speckle Tracking Echocardiography (STE), a novel technology recently applied also to stress echocardiography, has allowed assessing modifications of myocardial deformation with higher accuracy than the simple visual assessment of regional wall motion for the diagnosis of significant coronary stenosis [5]; STE has also been successfully tested to identify myocardial viability by DSE [6].
Despite the presence of several studies that evaluate ventricular function and other echocardiographic parameters in patients who undergo successful CTO recanalization, there are no data about the usefulness that stress echocardiography, associated with STE, can provide in the assessment of this lesions subset.
The aim of this study was to evaluate, using STE applied to DSE, changes in echo parameters before and after successful recanalization of a chronically occluded vessel.
From October 2012 to February 2014, eighteen patients with subacute or chronic coronary syndromes and angiographic evidence of CTO, scheduled for reopening, underwent DSE before and 3 months after CTO recanalization; among them, 7 patients were excluded because of unsuccessful attempts of CTO reopening. Therefore, 11 patients successfully treated by percutaneous coronary angioplasty (PCI) had a 3 months echocardiographic follow-up by additional DSE.
DSE was performed using standard protocol with intravenous infusion of dobutamine by incremental doses every 3 minutes (from 5 mcg/kg/min up to 40 mcg/kg/min). If theoretical maximum heart rate was not reach, atropine 1 mg was administered in fractioned doses over 4 minutes.
The acquisition of the images was performed by GE Vivid E9 echocardiography system (GE Healthcare, Horten, Norway), using a 3.5 MHz transducer; two-dimensional standard views (parasternal long axis, apical 4, 3 and long-axis chambers) have been recorded at baseline and stress peak by triplane acquisition.
The test was defined positive in case of detection of echocardiographic biphasic response or in case of evidence of a significant amount of viable or ischemic myocardium, respectively defined as the improvement (for viability) or worsening (for ischemia) of kinesis at least of 2 or more adjacent myocardial segments.
Measurements were performed off-line using dedicated software (Echo PAC version 112.0; GE Healthcare, Milwaukee, WI), according to ASE-EACVI recommendation [7]. Morphological echo parameters, as wall thickness and left ventricular (LV) diameters, were obtained at baseline; functional echo parameters were obtained both at baseline and stress peak; all before and after PCI. Functional parameters included: LV ejection fraction (EF) by Simpson biplane method, end-diastolic (EDV) and end-systolic (EDS) volumes, wall motion score index (WMSI), indices of diastolic function (E wave, A wave, deceleration time, E/A ratio), tissue Doppler (TDI) derived parameters (E' wave, S' wave, A' wave, E/E'), global longitudinal strain (GLS) calculated by STE, and strain rate (SR, S, E, A) (Figure 1 and Figure 2).
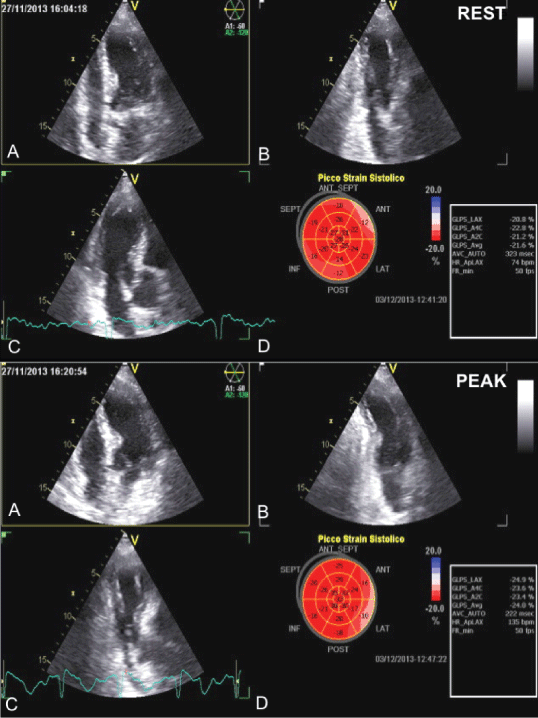 Figure 1: Triplane acquisition at baseline (upper panel) and peak (bottom panel) of stress.
Figure 1: Triplane acquisition at baseline (upper panel) and peak (bottom panel) of stress.
A) Apical 4 chamber view (A4C); B) Apical 2 chamber view (A2C); C) Apical long axis view (LAX); D) Bull's eye of global longitudinal strain (GLS).
View Figure 1
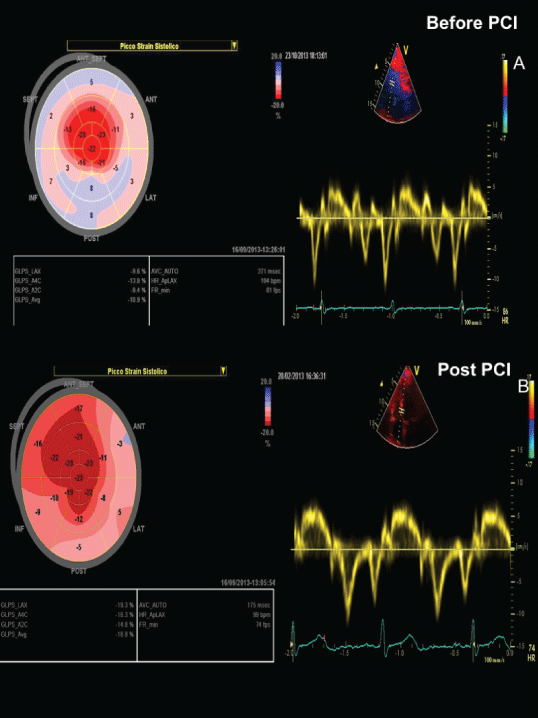 Figure 2: Global longitudinal strain and tissue velocities at mitral annulus before and after PCI (rest).
View Figure 2
Figure 2: Global longitudinal strain and tissue velocities at mitral annulus before and after PCI (rest).
View Figure 2
TDI velocity was also used to obtain systolic and diastolic longitudinal functional reserve (SLR and DLR respectively) defined by recently proposed formulas [8,9]: SLR = S' {1 - (1/S' rest)} and DLR = E' {1 - (1/E' rest)}. E' and S' values indicate the variations of these parameters between baseline and stress peak.
Values are presented as mean ± standard deviation (SD). Differences among groups were evaluated by one-way ANOVA. All p-values were considered statistically significant at less than 0.05.
The study has been performed in accordance with the ethical standard laid down in the 1964 Declaration of Helsinki and its later amendments.
The baseline clinical characteristics of patients are summarized in Table 1. The mean echocardiographic follow-up after PCI was 3.09 ± 1 month. The mean age of the patients was 58.5 ± 11.8 and among them, all (100%) were men. All patients had at least 2 or more cardiovascular risk factors including hypertension and dyslipidemia (81%); diabetes mellitus type II was present in 36% and 54% of them had previous myocardial infarction. Clinically, the majority of them had a stable angina causing, according to the Canadian classification, a mild (81%) or moderate (18%) reduction of the daily activities. All patients had previous coronary angiography, therefore CTO artery was known; CTO of left anterior descending coronary artery (LAD) was present in 18% of them, right coronary artery (RCA) in 45% and circumflex coronary artery (LCX) in 36%.
Table 1: Baseline Clinical Characteristics. View Table 1
Morphological and functional echo parameters at rest before and after PCI are summarized in Table 2 and Table 3; statistical analysis didn't show significant improvements or modifications of these parameters after revascularization.
Table 2: Echocardiographic Morphological Parameters at rest before and after PCI. View Table 2
Table 3: Echocardiographic Functional parameters at rest before and after PCI. View Table 3
Analysis of maximum heart rate achieved during stress showed improvements (P = 0.05) after PCI compared to values before, while the WMSI analysis showed no significant modifications (Table 4). There was an improvement, at peak stress after PCI, of EF (p < 0.001) and of systolic SR on 4 chambers view (p < 0.02).
Table 4: Echocardiographic functional parameters during stress before and after PCI. View Table 4
Changes (Δ), during stress, of functional echo parameters before and after PCI (Table 5): The analysis showed a trend towards improvement (9%) of EF (P = 0.15) and some parameters of diastolic function such as E wave (P = 0.1) and E' wave (P = 0.02); DLR showed significant improvement after PCI (P < 0.01). There were no significant changes for SLR, GLS and SR.
Table 5: Changes (Δ) of functional echo parameters before and after PCI. View Table 5
Many authors showed by echocardiographic studies (performed at rest) a significant improvements in terms of EF, myocardial contractility and survival from major cardiac events in patients with successfully reperfused CTO. Erdogan, et al. [10], using 3D echocardiography and STE in 118 patients at one-month follow-up from CTO recanalization, showed improvements in EF, EDV and EDS volumes, and GLS values in patients with EF > 50%. Wei-Yue, et al. [11], using 3D Real Time echocardiography, assessed EF modifications of 32 patients with and without prior myocardial infarction and successful CTO recanalization. The authors have shown significant EF improvements only in patients without previous myocardial infarction, emphasizing the importance of CTO collateral circulation in maintaining myocardial viability.
Studies with contrast echocardiography [12,13] showed significant improvements of WMSI, contractile function recovery and quantitative parameters of microvascular perfusion in the group of patients effectively reperfused.
Erdogan [10] also showed improvements of GLS values in successfully treated patients with EF > 50%, less evident in diabetics. Takimura and coll. [14] demonstrated, using 3D echocardiography, significant improvements of systolic and diastolic function after adequate CTO in 128 patients.
Our data showed non-significant increase of EF at rest and no significant WMSI variations; that's probably due the presence, in some patients, of both ischemic and viable myocardium and, considering the sample's number, we did not consider appropriate to differentiate infarction/non-infarction subgroups.
The improvements of systolic function obtained from the results of our study were less noticeable: only STE analysis of systolic strain rate, a parameter closely related to myocardial elastance [15], showed significative improvement during peak stress, before and after PCI. Despite significant increase between baseline-peak values before and after revascularization, EF showed just an improved trend, compared to global mean values. Similarly, GLS values were slightly improved, in a rate lower than the norm.
However, this phenomenon may be related to relatively short follow-up time and requirement of longer functional recovery periods but also likely to heterogeneity type of treated vessels, related to the small study sample observed.
Increased strain rate values has diagnostic accuracy in the identification of viable myocardium comparable to WMSI during dobutamine infusion [16]. Furthermore, the combined use of strain imaging associated with WMSI, significantly improves detection sensitivity of viable myocardium during dobutamine stress echo with values from 73% up to 82%. It also was shown in literature that peak systolic strain rate value greater than -0.23 sec. should be helpful to distinguish viable myocardium from non-viable with a sensitivity value of 83% and a specificity value of 84% [17].
Systolic and diastolic longitudinal reserve indices have been introduced recently as the most sensitive and early parameters to detect signs of subclinical myocardial dysfunction; they have been successfully used in groups of patients with diabetes [8], hypertrophic cardiomyopathy [18] and heart failure with preserved EF [9].
Similarly, to literature reported data, our study showed significant improvements of A wave, E' wave TDI values and a global trend of improvement in other diastolic function indexes.
Regarding longitudinal systolic and diastolic reserve indices our study showed only significant improvement of the diastolic one.
Thus, after short-term follow-up, only parameters related to diastolic function (E wave, E' wave TDI, diastolic reserve longitudinal index) improved earlier and more markedly.
CTO represent an important pathophysiological model to understand myocardial viability and ischemia; cardiac tissue perfused by chronically occluded vessel may show contractility alterations and simultaneously be partly vital and ischemic. Myocardial ischemia can induce diastolic function impairment by determining alterations of left ventricle relaxation [19]; recovery, partial or complete, of myocardial distensibility may slow the progression to heart failure, as demonstrated by several studies that support the prognostic value of diastolic abnormalities in ischemic heart disease [20].
CTO recanalization, in patients with evidence of significant amount of viable or ischemic myocardium, may offer advantages to obtain both systolic and diastolic function recovery.
Stress echocardiography is safe, inexpensive and easy to perform; it allows to study myocardial viability and ischemia in a complete, relatively easy way and with good sensitivity and specificity values; the association with new imaging techniques, such as STE for the analysis of longitudinal strain and strain rate, provides further improvements of diagnostic accuracy. Additional controls with longer follow-up periods and larger study population are needed for a more accurate analysis.
All Authors declare that they have no conflict of interest.
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent was obtained from all individual participants included in the study.