Mucormycosis is an invasive infection in immunocompromised host. It can lead to a devastating rhino-orbital-cerebral involvement with detrimental consequences. This disease is mainly caused by member of the family Mucoraceae that include Rhizopus, Rhizomucor, Mucor and Lichtheimia (formerly Absdia). This infection classically affects immunocompromised patients. The most common site of this infection in immunocompromised patients related to the pattern of the associated disease. In patients with malignancy, the lungs are the more likely to be affected, while diabetic patients are more likely to have sino-orbital disease. cutaneous infection most likely associated with history of trauma [1,2]. There is no quite enough data about mucormycosis in immunocompetent but some studies showed that cutaneous infection is the most affected organ in apparently healthy patients (42.5%) followed by rhino-orbito-cerebra (38.2%) [3].
Mortality varies with the site and the type of the disease: (96%) of patients with disseminated disease, (85%) in GI mucormycosis, and (76%) in patients with pulmonary disease [1].
We rarely encounter Rhino-orbito-cerebral mucormycosis (ROCM) in apparently immunocompetent hosts. However, Multiple cases of ROCM in immunocompetent patients were reported [3]. Diabetes mellitus, malignancy and immunosuppressant agents precipitate an invasive fungal infection [4]. Our aim from this report is to expand the index of suspicion of general internists, family physicians, emergency physicians, and infectious diseases who diagnose and treat patients with sinusitis regarding the possibility of having an invasive fungal infection in otherwise healthy individual. Additionally, we are trying to highlight the possible risk factors for mucormycosis in immunocompetent.
A 32-year-old, healthy Yemeni male patient. Not smoker nor IV drug user. Medically was free. No family history of malignancy. No personal history of weight loss or loss of the appetite. No history of blood or iron transfusion. No previous history of surgical intervention. Presented with 1-month history of recurrent headache and fever. He was treated initially as a case of bacterial rhinitis by his otolaryngologist. One month later, he presented with worsening of his headache, right sided weakness, and seizure. His laboratory works up was significant for anemia and leukocytosis. Nasal discharge, blood urine and sputum turned to be negative for culture and negative acid-fast bacilli as well. At that time, Sinus Computed Tomography (CT) showed mucosal thickening that obliterates the right maxillary antral cavity with soft tissue mass that extended to the sphenoid sinus reaching up to the prepontine cistern posteriorly, with right temporal region compression laterally. Anteriorly, ethmoidal air cells were noted with an expansion to the right cavernous sinus (Figure 1 and Figure 2). Findings upon brain Magnetic Resonance Imaging (MRI) was consistent with CT findings. So, the patient went for a biopsy. Histopathology examination revealed non-caseating granuloma as in (Figure 3 and Figure 4) with broad thick-walled collapsible a septate, right-angled branching hyphae and Large irregular hyphae upon Periodic acid-Schiff staining (Figure 5) suggestive of mucormycosis.
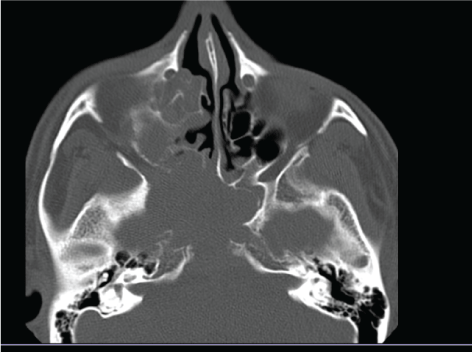 Figure 1: An axial view of the sinuses demonstrates ethmoidal air cells, a sizable soft tissue mass that involves the sphenoid sinus with wall destruction. View Figure 1
Figure 1: An axial view of the sinuses demonstrates ethmoidal air cells, a sizable soft tissue mass that involves the sphenoid sinus with wall destruction. View Figure 1
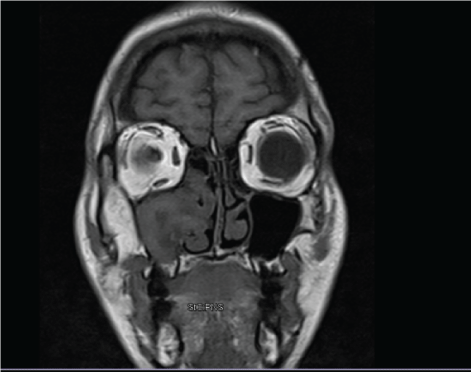 Figure 2: MRI of the sinuses shows a soft tissue mass of the right ethmoidal and axillary sinuses. View Figure 2
Figure 2: MRI of the sinuses shows a soft tissue mass of the right ethmoidal and axillary sinuses. View Figure 2
 Figure 3: Histopathological exam of the nasal discharge is consistent with non-caseating granuloma. View Figure 3
Figure 3: Histopathological exam of the nasal discharge is consistent with non-caseating granuloma. View Figure 3
 Figure 4: A slide shows broad thick-walled collapsible aseptate, right-angled branching hyphae suggestive of mucormycosis upon silver staining. View Figure 4
Figure 4: A slide shows broad thick-walled collapsible aseptate, right-angled branching hyphae suggestive of mucormycosis upon silver staining. View Figure 4
 Figure 5: Large irregular hyphae upon Periodic acid-Schiff staining. View Figure 5
Figure 5: Large irregular hyphae upon Periodic acid-Schiff staining. View Figure 5
After the diagnoses of ROCM, we did an extensive work up to rule out underlying disease. serology testing for Human Immunodeficiency Virus was negative as well as immunoglobulin. Fasting blood sugar was 98 and HbA1C was 4.9. CT chest and abdomen were all negative for malignancy. A neurosurgical consultation was made for possible surgical debridement but the family and the patient refused the surgical choice. So, patient was treated medically. The patient was started on intravenous amphotericin B therapy 300 mg along serial kidney function monitoring. But patient developed sever chills, rigors, and sever electrolyte disturbance. Which did not respond to premedication preparation (paracetamol and diphenhydramine). So we decreased the dose of amphotericin and added voriconazole 380 mg twice daily. The repeated MRI after 3 months, there was mild regression of the sinus disease without progression. But then the patient passed away as he was not compliance to treatment due to insurance issues.
Mucormycosis is a rare infection, fatal opportunistic mycotic infection that affects the human beings. The incidence of mucormycosis is approximately 1.7 cases per 1,000,000 population per year according to recent reports from spain and California [5].
The plurality of patients developing mucormycosis reported having history of risk factors, which are summarized in Table [1]. Most important causes are organ transplantation, chronic corticosteroid treatment and hematologic malignancies [6]. It was not commonly described in patients with human immunodeficiency virus (HIV). The abnormalities in neutrophils with impaired phagocyte response and increased available serum iron are the most common two conditions in the majority of patients with mucormycosis [6]. According to this mechanism, diabetic patients was found to have impairment in phagocytes activity [1], which can well explain that disease was also described in diabetic patients.
Table 1: Risk factors for the mucormycosis infection. View Table 1
However, some healthy individuals have developed mucormycosis with no identifiable risk factors. The clinical manifestation of rhino-cerebral mucormycosis most commonly mimicking symptoms of sinusitis or periorbital cellulitis, facial pain, unilateral facial swelling, fever, and blackened necrotic eschars of the nasal mucosa and palate.
The literature review revealed about 126 articles published until 2009, from 35 countries. the total described patients were 212. The most affected place was India (44.3%) patients, followed by USA and Australia 42 (19.8%) and 12 (5.7%) patients, respectively. Just 6 (2.8%) cases have been described from Italy. In addition to a case series of 5 patients in Italy, published in 2011 [3].
Some reports showed that most of immunocompetent patients with ROCM tend to have delayed diagnosis and management. This delay, would significantly increases the risk of CNS disease. Since the mucormycosis is able to produce toxins that are able to blunt the mucosa, a previously damaged mucosa from infection, allergy, and trauma is at risk for developing ROCM in immunocompetent host [7,8]. A hypothesis of the correlation of chronically insulted mucosa and ROCM development in immunocompetent hosts needs to be tested.
Geographically, India ranked first in a recent literature review with 94 cases, followed by USA with 42 cases, and Australia with 12 cases [9]. According to literature review, we conclude possible risk factors that might play a role in ROCM. This disease has been observed more in dark color people [3]. Climatic conditions due to hot weather could give the chance to this organism to thrive. The temperature required for their growth is 28 to 30 c [10]. Air condition which can lead for dryness of mucosal epithelium. Air condition could be one of the main sources of mucormycosis as it gives this organism a great circumstance to multiply [11].
Poor nutrition may play a role by causing proteins and vitamins deficiencies which might impair the needs of the bodies to well regulate our immunity. Socioeconomic poor conditions will cause bad hygiene, recurrence of the trauma, poor education, lack of awareness and late diagnosis, are possibilities as risk factors.
Physicians in developing countries tend to underestimate the importance of reporting mucormycosis infections in immunocompetent hosts. This practice makes recent review faces multiple challenges in terms of accuracy. Thus, we aim to report this case to alarm physicians who deal with sinus infections in their daily practice.
Having a high index of suspicion for possible ROCM in patients with sinus infections. Especially, if the patient shows worsening course to initial therapies. Early diagnosis and administration of antifungal therapy along with surgical debridement is crucial element. The earlier the intervention the better the outcomes.