Hypophosphatemia, Phosphorus, Polymorphic ventricular tachycardia, Arrhythmia
It is well known that electrolyte derangements such as hypokalemia, hypomagnesaemia, and hypocalcaemia can potentially cause dangerous arrhythmias in hospitalized patients. This can be a common concern for acute care physicians, as the occurrence of arrhythmias predisposes patients to higher morbidity, mortality, and longer length of stay. Phosphorus, however, has been less studied. It is known that hypophosphatemia can disrupt myocardial contractility and reduce cardiac function [1]. Less known, however, is its ability to trigger cardiac arrhythmia. Here we present a rare case of a young male with hypophosphatemia induced polymorphic ventricular tachycardia.
A 23-year-old male with no significant past medical history presented to the emergency department after a mechanical fall. On admission, his vital signs were stable and within normal limits. Physical exam findings included a Glasgow Coma Scale score of 15, bleeding and hearing loss in the left ear, and laceration to the left occipital area. Phosphorus was 2.3 mg/dl on admission. All other labs, including electrolytes, were normal. Imaging of the head showed small right temporal lobe hemorrhagic contusion. Transthoracic echocardiogram revealed normal left ventricular size and systolic function (ejection fraction 60-65%) with normal left ventricular diastolic filling and no abnormal findings. Electrocardiogram evidenced normal sinus rhythm.
During his stay, patient's overnight telemetry revealed intermittent, non-sustained ventricular tachycardia (Figure 1). He was asymptomatic at the time, denying any chest pain, shortness of breath, palpitations, or dizziness. Patient denied any personal or family history of heart failure or arrhythmias. Of note, he had not eaten the day prior to the event, and had remained nothing per oral (NPO) on admission. Labs were checked and found to be within normal limits, except for a critically low phosphorus level of 1.4 mg/dl. Arrhythmia continued to persist for several hours until phosphorus was replenished to 3.2 mg/dl, after which the patient no longer had any arrhythmias on telemetry (Figure 2). This patient was on telemetry for his entire hospitalization, and he was discharged several days later with a Holter monitor to evaluate for further episodes of arrhythmia, which was negative.
 Figure 1: EKG prior to phosphorus replacement. View Figure 1
Figure 1: EKG prior to phosphorus replacement. View Figure 1
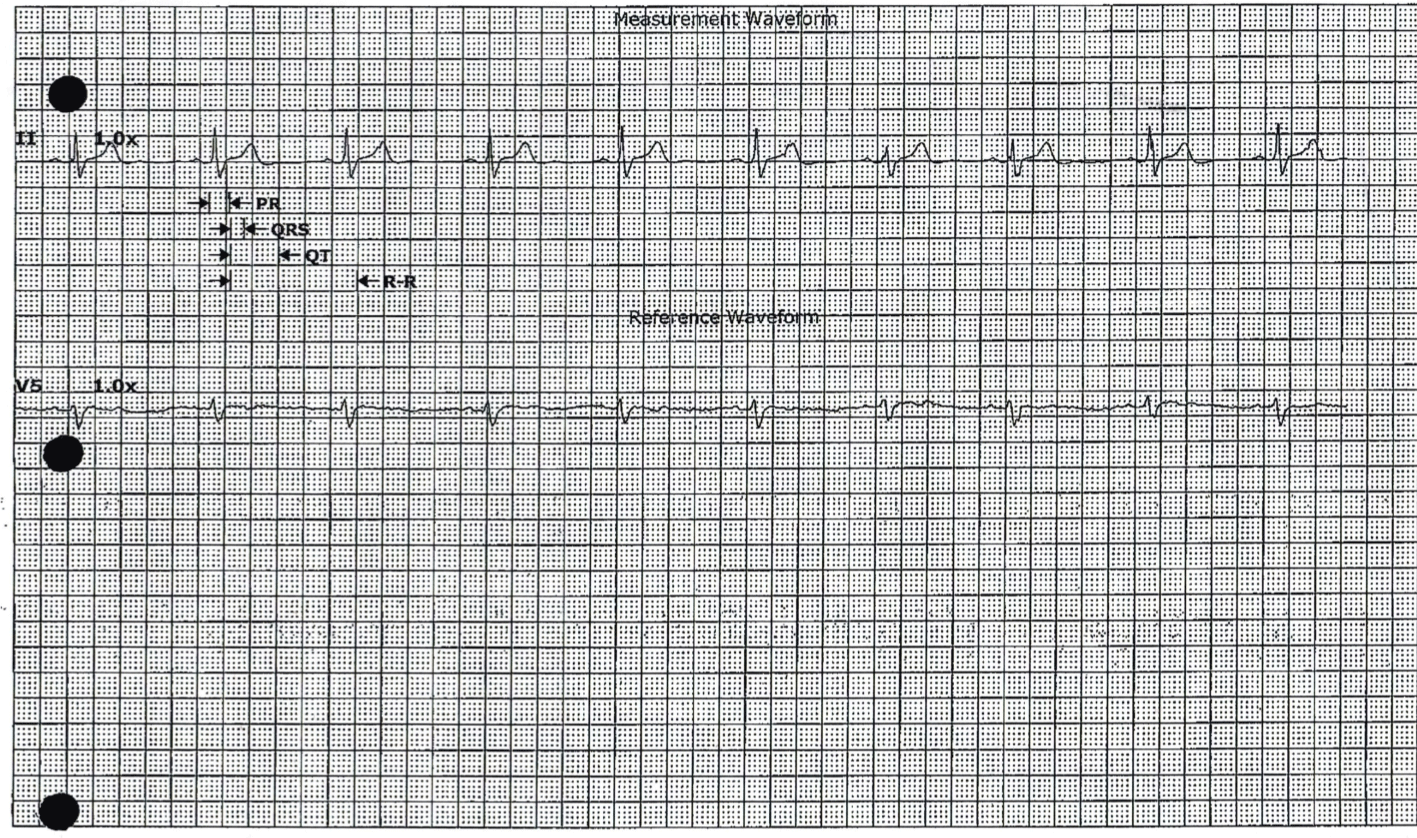 Figure 2: Telemetry strip after phosphorus replacement. View Figure 2
Figure 2: Telemetry strip after phosphorus replacement. View Figure 2
Cardiac MRI was performed after phosphorus replacement and revealed normal left ventricular function (ejection fraction of 61%) with no abnormal late gadolinium enhancement to suggest left ventricular scarring or infiltrative processes. He had no abnormal motion of the anterior free wall of the right ventricle to suggest an arrhythmogenic right ventricular dysplasia/cardiomyopathy.
Given patient's young age, genetic testing was performed with GeneDx Comprehensive Arrhythmia Panel and was found to be negative (Figure 3). This panel tested for 46 genetic variants associated with arrhythmias such as Long QT Syndrome, Catecholaminergic Polymorphic Ventricular Tachycardia, Arrhythmogenic Right Ventricular Cardiomyopathy, and Brugada Syndrome.
 Figure 3: GeneDx Panel. View Figure 3
Figure 3: GeneDx Panel. View Figure 3
This case illustrates a patient presenting with hypophosphatemia induced non-sustained polymorphic ventricular tachycardia. Delving into the details, phosphorus is an important mineral utilized by almost every cell in the body, with changes in serum values having significant clinical repercussions in patients, especially those who are critically ill [2]. The mineral helps to regulate calcium, another mineral essential for proper cardiac functioning. In addition, phosphorus acts a buffer to help maintain normal acid-base balance, which is important since blood acidity affects heart rate [3]. Phosphorus is also found in 2,3-DPG which helps red blood cells deliver oxygen to the heart [3].
Although fairly rare in the general population, the incidence of hypophosphatemia is high in select groups of patients, such as those who are hospitalized (3.1%) or admitted to intensive care units (33.9%), and those with sepsis (65 to 80%), chronic alcoholism (2.5 to 30.4%), major trauma (75%), and chronic obstructive pulmonary disease (21.5%) [4]. Because of the involvement of phosphorus in every cell of the body, many of the symptoms of hypophosphatemia stem from intracellular phosphate depletion. Symptoms of having low phosphorus include rhabdomyolysis, thrombocytopenia, impaired diaphragmatic contractility, and metabolic encephalopathy resulting from ATP depletion.
Although not as common as seen with hypokalemia, the association between hypophosphatemia and cardiac arrhythmia has recently been made in the literature in septic patients and patients suffering acute myocardial infarction. Dating even further back to the 1970s, studies have looked into the relation of phosphorus to cardiac performance, where patients with severe hypophosphatemia had an increase in left ventricular stroke work, which improved upon return of serum phosphate to normal levels [5]. Mechanism appears to be unknown at this time, but it is postulated that the low phosphate levels may have something to do with the intracellular availability of ATP (3). Because of the importance of phosphorus in cardiac functioning, there have been several studies focused on its association with arrhythmias. In 2014, a study looked at 34 adult septic patients with hypophosphatemia. IV phosphorus replacement was associated with a significantly reduced incidence of arrhythmias (38% vs. 63%, p = 0.04), demonstrating that phosphorus replacement might be effective in reducing the rate of arrhythmias in septic patients [6].
This case occurred in a less critical patient, and as such recognition of the importance of electrolyte replacement in all hospitalized patients is a relevant concern to prevent complications such as arrhythmias.
Although it is rare, hypophosphatemia should be considered in the differential diagnosis of arrhythmia without an obvious cause. And as always, any other more common causes for arrhythmia, such as hypokalemia or hypomagnesemia, must be corrected prior to attributing the problem to hypophosphatemia.
No sources of support.
All authors contributed equally to the creation of the manuscript.