International Journal of Stem cell Research and Therapy
Mesenchymal Stem Cell: Considerations for Manufacturing and Clinical Trials on Cell Therapy Product
Yen-Shun Chen1*, Yi-An Chen1, Pei-Hsun Tsai1, Chih-Ping Chen2, Sheng-Wen Shaw3 and Yogi Hsuan1
1Stem Cell Research Department, Meridigen Biotech Co. Ltd., Taipei, Taiwan
2Department of Obstetrics and Gynecology, Mackay Memorial Hospital; Department of Medicine, Mackay Medical College, New Taipei City, Taiwan
3Department of Obstetrics and Gynecology, Chang-Gung Memorial Hospital, Lin-Kou Medical Center, Taoyuan, Taiwan
*Corresponding author: Yen Shun Chen, Stem Cell Research Department, Meridigen Biotech Co. Ltd., 7F, Number 68, Section 1, Neihu Road, Neihu District, Taipei City 11493, Taiwan, Tel:+886-2-26275175; Fax: +886-2-26275275; E-mail: yenlife@gmail.com
Int J Stem Cell Res Ther, IJSCRT-3-029, (Volume 3, Issue 1), Short Review; ISSN: 2469-570X
Received: February 16, 2016 | Accepted: March 28, 2016 | Published: March 31, 2016
Citation: Yen-Shun C, Yi-An C, Pei-Hsun T, Chih-Ping C, Sheng-Wen S, et al. (2016) Mesenchymal Stem Cell: Considerations for Manufacturing and Clinical Trials on Cell Therapy Product. Int J Stem Cell Res Ther 3:029. 10.23937/2469-570X/1410029
Copyright: © 2016 Yen-Shun C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Mesenchymal stem cell (MSC) have the ability to self-renew and differentiate into various cell type, and they are the most widely used cell type in stem cell therapies. Designing a new MSC drug is an intricate process, considering the versatile nature of cells and the susceptibility to manufacturing processes. As the number of MSC-based clinical trials rapidly grows over the years, there is an urgent need to develop a more stringent method to characterize MSC for quality and to enhance scrutiny on the safety and efficacy of manufactured MSC. In this review, we discuss the sources, quality, safety and characterization of new MSC-based drugs required for Investigational New Drug (IND) submission approval, as well as the relevant regulations and the outcomes of current clinical studies of MSC for cellular therapeutic product.
Keywords
Mesenchymal stem cells, Umbilical cord, Fibroblast, Chemistry manufacturing and controls, Manufacturing processes, Surface markers, Regulatory, Clinical trials, Good Manufacturing Practice, EphA2
Abbreviations
aGvHD: Acute graft-versus-host disease; Allo-: Allogeneic; ALS: Amyotrophic lateral sclerosis; AMSC: Adipose tissue-derived mesenchymal stem cells; ARDS: Acute respiratory distress syndrome; ATMPs: Advanced therapy medicinal products; Auto-: Autologous; BLA: Biologics License Application; BM: Bone marrow; BMSC: Bone marrow-derived mesenchymal stem cells; BM-MNCs: Bone marrow-derived mononuclear cells; BPD: Bronchopulmonary dysplasia; CBER: Center for Biologics Evaluation and Research; CDSCO: Central Drugs Standards Control Organization (India); CFR: Code of Federal Regulations; CFU-F assay: Colony-forming unit - fibroblast assay; CGH: Comparative Genomic Hybridization; cGMP: Current Good Manufacturing Practice; cGTP: Current good tissue practice; CJD: Creutzfeldt-Jakob disease; CMC: Chemistry, manufacturing and controls; CMV: Cytomegalovirus; EGF: Epidermal growth factor; ELISA: Enzyme-linked Immunosorbent Assay; EMA: European Medicines Agency; EphA2: Ephrin receptor A2; FC: Flow cytometry; FDA: U.S. Food and Drug Administration; FGF-2: Basic fibroblast growth factor-2; FISH: Fluorescence in situ hybridization; GLP: Good Laboratory Practice; GvHD: Graft-versus-host disease; HBV: Hepatitis B virus; HCT/Ps: Human cells, tissue, and cellular and tissue-based products; HCV: Hepatitis C virus; HGF: Hepatocyte growth factor; HiDOS: High-throughput dynamic multiple omics system; hiPS-MSC: Mesenchymal stem cells derived from human induced pluripotent stem cells; HIV-1, HIV-2: Human immunodeficiency virus types 1 and 2; HLA class I/II: Human leukocyte antigen class I/II;HLA-DR: Human leukocyte antigen - antigen D related; HTLV-1, HTLV-2: Human T-lymphotropic virus types 1 and 2; HUCMSC: Human umbilical cord-derived mesenchymal stromal cells; IND: Investigational new drug; iPSCs: Induced pluripotent cells; ISCT: International society of cell therapy; IV: Intravenous; LIF: Leukemia inhibitory factor; MFDS: Ministry of Food and Drug Safety; MNCs: Mononuclear cells; MPACs: Multipotent adult progenitor cells; MPCs: Mesenchymal progenitor cells; MS: Multiple sclerosis; MSC: Mesenchymal stem cells; N/A: Not applicable; NIH: National Institutes of Health; OA: Osteoarthritis; OBD: optimal biologic dose; Oct-4: Octamer-binding transcription factor 4; PCR: Polymerase chain reaction; PHS Act: Public Health Service Act; PL: Placenta; RNA-seq: RNA sequencing; R&D: Research and Development; SLE: Systemic lupus erythematosus; Sox-2: (Sex determining region Y)-box 2; SSEA-3, SSEA-4: Stage specific embryonic antigen types 3 and 4; Stro-1: Stromal precursor antigen 1;UC:Umbilical cord; UCB: Umbilical cord blood; WJ: Wharton’s jelly
Introduction
Cell therapy is a type of medical intervention in regenerative medicine in which sick, dying, or missing cells or tissues are replaced with healthy cells to restore or establish normal functions [1,2]. Because they have the ability to self-renew and differentiate into various cell types, stem cells are widely studied for their application in regenerative medicine. Among all types of stem cells, mesenchymal stem cells are the most commonly used in cell therapies because they are relatively easy to procure from a variety of tissues, free from ethical concerns, less likely to form teratomas, and rarely undergo spontaneous differentiation during ex vivo expansion [2-5]. Moreover, therapies using MSC are often considered safe because the transplanted cells exist only for a short time in the recipient’s body. Their paracrine effects on tissue repair, as well as the anti-inflammatory properties and homing abilities to damaged sites, have made MSC a very popular candidate for clinical study [6]. The major problem with MSC-based therapies, however, is the inconsistency in the outcome and the strength of effectiveness [7]. The characteristics of MSC from different donors or tissue sources vary greatly. Moreover, the quality of MSC is susceptible to the way they are processed, leading to different results in the risk/benefit assessment in the clinical applications of MSC. As the number of MSC-based clinical trials rapidly grows, there is an urgent need to develop a more stringent method of MSC characterization for quality control and to enhance scrutiny on the safety and efficacy of manufactured MSC. Here, we cover issues related to the quality, safety and characterization of MSC for potential therapies and discuss general regulatory frameworks for new MSC-based drug development, as well as current clinical studies involving MSC and approved MSC therapies.
Sources for Human Mesenchymal Stem Cells
Human mesenchymal stem cells can be procured from various sources, and their potency in curing different diseases depends on their source [7]. Bone marrow (BM) is the most widely recognized source of MSC, even though only 0.001%-0.01% of bone marrow cells are composed of MSC [8]. Harvesting BM from a donor is a highly invasive and painful procedure. Moreover, the number of cells harvested, differentiation potential, and maximal life span of MSC from BM decline with increasing age [9]. Therefore, alternative sources to isolate MSC from have been intensively investigated. Evidence has suggested that MSC have full therapeutic potential and are mostly located in the vascularized tissues throughout the body [10]. The alternative sources of MSC-like cells include adipose tissue, placenta, amniotic fluid [11], dental pulp [12], synovial membrane [13], peripheral blood, periodontal ligament [14], endometrium [15], umbilical cord (UC), and umbilical cord blood (UCB). Notably, human umbilical cord-derived mesenchymal stromal cells (HUCMSC) are fetus-derived stem cells collected from discarded Wharton's jelly, which can be obtained after birth without harming either them other or infant, and thus area good substitute for BMSC for the donor’s benefit. Recently, human somatic cells have been easy to reprogram into induced pluripotent cells (iPSCs), and this could be another source of MSC. The protocols for deriving mesenchymal stem cells from human induced-pluripotent stem cells (hiPS-MSC) have been proposed as a robust, efficient and safe system for therapy [16,17].
The differentiation potential of MSC may differ depending on from where the MSC originate [7]. For instance, researchers have proven that early fetal, placental, and amniotic sources yield abundant primitive MSC with greater multipotency and with faster and longer self-renewal than from an older adult’s bone marrow [18,19]. Moreover, cell size and gene expression of MSC differ depending on their source and expansion methods [2,20,21]. In addition, single cell RNA-Seg reveals that the transcriptional diversity of murine bone marrow-mesenchymal stem cells is associated with the osteogenic, chondrogenic, and adipogenic differentiation ability of MSC [22]. Furthermore, it has been reported that MSC from different harvesting sites have varied adipogenic properties and are susceptible to apoptosis on various levels [2,23,24]. Concerning all of these differences, the properties and qualities of MSC from a given source should be carefully evaluated when designing an MSC-based product for therapeutic use.
Characterization of MSC Quality, Safety and Potency
Mesenchymal stem cells are often isolated from a donor and expanded in laboratories before being given to a patient in cellular therapies because effective clinical treatment demands a large amount of MSC. Intravenous administration of MSC to patients often requires a dose of approximately 106/kg body weight per injection [25,26]. It is therefore important to determine the manufacturing processes of an MSC-based product, including from isolation to expansion, and methods in the early phases of drug development. Because research groups use different tissue sources, means of isolation, culture protocols, and chemistry, differences in manufacturing and controls (CMC) characterization tools, MSC quality, safety and efficacy could be expected [2,20]. We next discuss how the donor and manufacturing processes affect the quality of MSC, and what assays are required to assess the safety, potency, and characteristics of the product (Table 1 and Figure 1). Factors such as donor variance and eligibility, manufacturing processes, cryostorage and stability programs for lot-to-lot release are all important points to consider and questions to attend to in the Investigational New Drug (IND) Application for an MSC-based therapeutic product (Figure 1 and Figure 2).
.
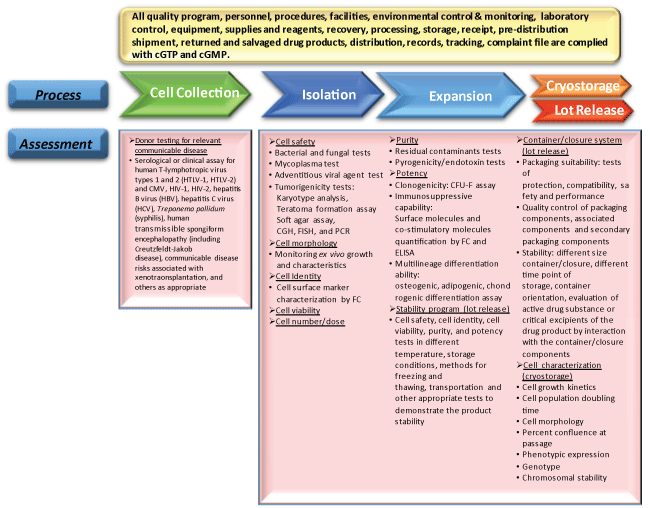
Figure 1: Suggestive assessments in cell collection and manufacturing process of MSC-based product. The flow chart represents the main steps in MSC product development from cell collection, manufacturing to cryostorage and lot release. Rectangles under the flow chart are suggestive assessments for those individual steps.
cGTP: current Good Tissue Practice; cGMP: current Good Manufacture Practice; CGH: Comparative Genomic Hybridization; FISH: Fluorescence In Situ Hybridization; FC: Flow cytometry and CFU-F: colony-forming unit-fibroblasts; ELISA: Enzyme-Linked Immunosorbent Assay
View Figure 1
.
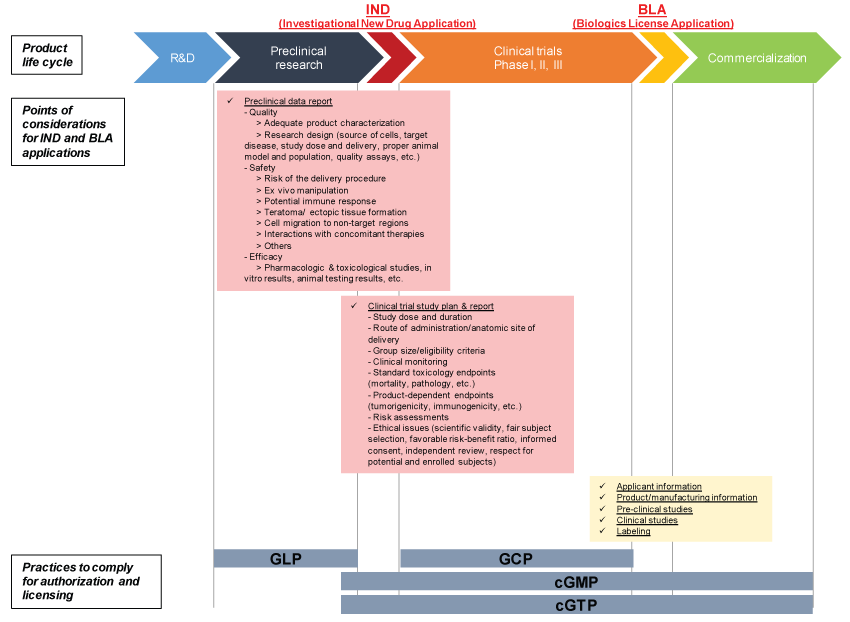
Figure 2: Points of considerations for IND and BLA applications and practices to comply in different phases of a cellular drug development. Note that the time frames for cGMP and cGTP are not clarified by the FDA but any HCT/Ps establishment that performs a manufacturing step is responsible for complying with cGTP and cGMP requirements.
R&D: research and development; GLP: Good Laboratory Practices; GCP: Good Clinical Practices; cGMP: Current Good Manufacturing practices; cGTP: Current Good Tissue Practices.
View Figure 2
Donor Eligibility and Cell Collection
To select reliable and robust cell sources for MSC in clinical applications, it is necessary to investigate how cell behavior differs between donors. In terms of the potency of isolated MSC, selecting a good donor is difficult because evaluation criteria are lacking. While the features of a donor that might affect MSC potency and normality are not fully identified yet, age may be one of the most important criteria [27,28]. Several in vitro and in vivo studies of human MSC suggest that the age of the MSC donor could be directly linked to differentiation and cloning potential of MSC [9,28] but not to their morphology or marker expressions [29]. Researchers have also reported that the level of secreted paracrine factors by MSC correlates with donors of matched age and gender, and there could be up to a 10-fold difference [7,30]. Although there are no specific regulatory requirements for donor selection, there remains a risk of procuring substandard or off-standard MSC from relatively unsuitable donors [28]. For MSC therapies in IND applications, donor screening and testing are necessary for all allogeneic cells or tissues, as required in the 21 Code of Federal Regulations (CFR) Part 1271, except those that meet the exceptions in the 21 CFR 1271.90(a). It is recommended that the donors be screened for human T-lymphotropic virus types 1 and 2 (HTLV-1, HTLV-2), cytomegalovirus (CMV), HIV-1, HIV-2, hepatitis B virus (HBV), hepatitis C virus (HCV), Treponema pallidum (syphilis), human transmissible spongiform encephalopathy (including Creutzfeldt-Jakob disease), communicable disease risks associated with xenotransplantation, and others as appropriate (Figure 1) [27].
Manufacturing
After cell collection from a donor, the manufacturing process of MSC include isolation, expansion, cryostorage, and lot release (Figure 1). In general, an establishment designed for manufacturing of MSC-based products should have a well-developed CMC strategy and comply with current good tissue practice (cGTP) and current good manufacturing practice (cGMP) requirements [31,32]. Product testing is recommended throughout the manufacturing process to evaluate the process itself and to ensure the consistency and quality of the product [27]. Regarding sterility, safety, purity, and potency of a MSC product, several assessments should be performed. To confirm the sterility and safety of the cells, bacterial and fungal testing, mycoplasma assays, and various adventitious agent testing, as appropriate, should be performed (Figure 1). For product purity tests, assays for residual contaminants (such as residual peptides, cytokines and growth factors used during manufacturing) and pyrogenicity/endotoxin testing should be conducted. As for potency tests, different assays could be used depending on the features of the product. Feasible assays include, but are not limited to, CFU-F assays for clonogenicity, flow cytometry or ELISA for surface molecules and co-stimulatory molecules quantification, and differentiation assays to evaluate the multi-lineage differentiation ability. In the final stages where the manufactured product will be cryopreserved or released, the container/closure and stability program of the final product should be carefully tested [27] (Figure 1).
Any variation in the processing methods may change the characteristics of MSC [2,20]. It has been noted that for ex vivo expansion of MSC, parameters including starting material, methods used for enrichment or separation, plating density, devices used for MSC culture, media, supplements and growth factors, as well as passage number or population doublings, are all critical to ensure both good expansion rates and maintenance of stemness of MSC [2,21]. Specifically, using a low or very low cell seeding density could maintain a high proliferation rate and multipotency of MSC [28,33]. Sequential passaging of MSC may also render the cells with progressive senescence, reduced proliferation rate, and loss of multipotency [28,34]. Therefore, in each steps of MSC manufacturing should be carefully designed, validated, and standardized to ensure a preferred and reproducible outcome [35].
Safety and Potency Assays
To evaluate the safety and potency of a manufactured MSC-based product, several assays have been established (Table 1). For safety issues, karyotype analysis, teratoma formation assay, soft agar assay, comparative genomic hybridization (CGH), FISH, and PCR are often used to roughly check for the tumorigenicity of MSC, in case they underwent malignant transformation [2,20,36]. Assays, such as endotoxin tests ([Endotoxin] < 5 EU/kg or < 0.5 EU/ml) and microbiological tests (bacteria, fungi, mycoplasma, and adventitious agents), are used to ensure the product is free of contamination. To assess the potency of manipulated MSC, aCFU-F assay can be used to quantify precursor frequencies, even though it is not a standardized protocol based on different targeting therapies. In vitro assays have been developed to quantify the expression of surface molecules, such as HLA class I/II and co-stimulatory molecules, to examine the immune-modulating responses of MSC [2]. Furthermore, previous studies have already demonstrated that infusing an MSC-conditioned medium renders therapeutic effects [2,37], indicating that MSC secrete factors (including FGF-2, HGF, EGF, and LIF) that might have beneficial effects in treating cardiovascular diseases [38] and brain injuries [39,40]. Thus, analyzing the secretome of MSC may become a decent addition topotency assays [2,21,41]. The multilineage differentiation capability is a characteristic of MSC and has been reported in many publications [7,42]. The differentiation capability to osteoblasts, chondrocytes and adipocytes is related to the efficacy of the MSC-based products and have to be evaluated by in vitro differentiation assays.
Surface Markers of MSC
To specify MSC-based products, the most common way is to perform flow cytometry to see whether MSC express representative surface markers. A number of MSC surface molecules related to their stemness and tri-lineage ability have been suggested as MSC markers. Current characterization of MSC is largely based on the minimal criteria proposed by Dominici et al. in 2006 [42]. The standard definition of MSC according to the International Society of Cell Therapy (ISCT), regardless of the origins and method of isolation, is the ability to stick to plastic, differentiate into adipogenic, osteogenic and chondrogenic lineages by means of specific culture media, and positively express CD105, CD90, and CD73 without expression of CD34, CD45, CD11 and HLA-DR surface markers [42]. Therefore, one of the general MSC drug release criteria is to examine the immunophenotypic profile, with > 95% of the population expressing positive markers (CD105, CD90, and CD73) and < 2% expressing negative markers (CD34, CD45, and so on) (Table 1). In addition to the common tri-lineage differentiation, MSC have also demonstrated the ability to differentiate into mesodermal, neuroectodermal and endodermal lineages [2,42]. Being multipotent cells of embryonic mesodermal origin, MSC have a fibroblast-like morphology and share common properties with fibroblasts, such as expression of CD105, CD73, and CD90 [43] (Table 2). MSC have a fibroblastic or perivascular nicheorigin that activate to support tissue regeneration and repair during tissue injury [44,45].
![]()
Table 1: Basic assays for MSC-based products.
View Table 1
![]()
Table 2: Comparison of MSC and fibroblast characteristics
View Table 2
Because the characteristics of MSC are similar to that of fibroblasts, it is likely that MSC cultures are contaminated with fibroblasts, which may lead to decreased purity and differentiation potential of the MSC-based products. To improve the purity of MSC cultures, it is crucial to remove fibroblast-harboring sources, such as the connective tissues during the isolation process, and develop a strategy to distinguish MSC from fibroblasts. One way to achieve this is to observe the expression of surface markers. Table 2A lists several surface markers that have been reported present or absent in MSC or fibroblasts. Some of these markers may help to identify MSC, even though the precise criteria remain unestablished. A novel MSC marker, EphA2, has been recently identified in human BMSC, human umbilical cord perivascular cells [46], and placenta/umbilical cord-derived MSC [47] with the use of quantitative discovery proteomics. Evaluation of MSC quality isolated from umbilical cords by EphA2 detection in early clinical development can save time and expenses by keeping the research direction on the right track. Another way to distinguish MSC from fibroblasts is by evaluating the stemness, colony-forming potential [48] and immunomodulation capacities of the cells because fibroblasts seem similar but are limited in these functional properties (Table 2B).
It is still unclear whether MSC from different tissue sources and processed by various methods express different markers that may indicate their clinical utilization and therapeutic outcome. Molecular profiles, especially those specifying multipotency, stemness, and lineage associated markers, demonstrate that there are significant differences in the characteristics of MSC that are derived from various tissue sources. For example, adipose-derived MSC express higher levels of CD49d, CD34, and CD54, whereas BMSC express greater levels of CD106 [7,49,50]. MSC derived from fetal tissues are also reported to be comparatively immature and expressing pluripotency markers such as SSEA-3 and 4, Oct-4, Sox-2, and Nanog [2,51]. Markers such as Stro-1 and SSEA-4 are only expressed in BMSC but not adipose-derived MSC or HUCMSC, whereas CD271 is expressed in BMSC and adipose-derived MSC but not in HUCMSC [44,52]. In short, the minimal criteria for MSC characterization are not enough to classify MSC from various tissue environments. More advanced characterization protocols are needed for the early assessment of MSC quality to improve MSC yield and differentiation potential, before considering their functionality in the later stages of clinical trials and cGMP production.
Regulatory Frameworks of MSC Therapies
When a new MSC drug is ready for clinical trials, responsible persons should apply for it to become an investigational new drug (IND) by contacting the health regulatory authority in the country where the clinical trials will take place (Figure 2). Here, we provide the general information on conditions where the current MSC-based clinical trials are approved.
In the U.S., human cells, tissue, and cellular- and tissue-based products (HCT/Ps) are regulated by the Center for Biologics Evaluation and Research (CBER), a division of the U.S. Food and Drug Administration (FDA). HCT/Ps must comply with the 21 CFR Part 1271, which addresses issues including procedures for registration and listing, donor eligibility and cGTP. Under circumstances in which the HCT/Ps are minimally manipulated, designed for homologous use only, and not combined with another article and do not have a systemic effect, HCT/Ps are regulated solely under section 361 of the PHS Act. HCT/Ps intended for non-homologous use or more than minimally manipulated are regulated as biological products and comply with IND regulations (21 CFR 312), biologics regulations (21 CFR 600) and cGMP (21 CFR 211). A cellular product such as MSC collected from umbilical cord and placenta is defined as more than minimally manipulated because the processing breaks down and eliminates the structural components that provide cushioning and support, thereby altering the original relevant characteristics of the HCT/P relating to its utility for reconstruction, repair, or replacement [53]. The FDA has published standardized deviation reporting rules and draft guidance in 2004, 2014, and 2015 respectively, regarding the scope of clinics required for HCT/Ps. In Europe, cellular products belonging to advanced therapy medicinal products (ATMPs), fall under the regulation of Directive 2001/83/EC when they have been subjected to substantial manipulation that causes a change in their biological features, physiological functions or structural properties relevant for the intended therapeutic use. Regulation (EC) No.1394/2007 has been effective since 2008, and it was "designed to ensure the free movement of advanced therapy products within Europe, to facilitate access to the EU market and to foster the competitiveness of European companies in the field, while guaranteeing the highest level of health protection for patients," as noted on the European Commission website. The main elements include a centralized marketing authorization procedure, a new and multidisciplinary expert committee within the European Medicines Agency (EMA) to assess ATMPs and follow scientific developments, technical requirements adapted to the particular characteristics of ATMPs, and special incentives for small- and medium-sized enterprises.
During IND application, the applicant should provide pre-clinical data along with a well-structured study plan for clinical trials and proof of Good Laboratory Practice (GLP), cGMP, and cGTP compliances (Figure 2). Tests needed to pass the application include those that approach the quality, safety, efficacy results (for in vitro conditions or from animal tests) and fit the regulations listed in cGTP, GLP, cGMP guidelines [31,54,55]. As for the clinical study plan, elements to disclose include drug dosage and treatment time frame, route of administration or anatomic site of delivery, patient selection criteria and group size, clinical monitoring and standard endpoints, risk assessments and others depending on the product type. These general regulatory approaches for new MSC drug IND applications are not "one-size-fits-all" due to the wide variety of cellular products and their potential therapeutic use. Applicants should consult with their regulatory authority for specific requirements [56,57].
Clinical Trials of MSC-Based therapeutic Products
The clinical trials of IND is generally divided into three phases. Phase I trials are designed to determine the safety associated with increasing doses during cell therapy. Phase II and III trials are focused on effectiveness of the indication. When conducting these phases, ethical issues should be carefully attended to. According to the NIH’s website for clinical research ethics, points to consider include (1) contribution to social and clinical value, (2) valid and feasible approach to ensure scientific validity, (3) fair subject selection, (4) favorable risk-benefit ratio, (5) free-of-bias study, (6) informed consent, and (7) respect for potential and enrolled subjects [58]. During Phase I, safety estimation includes an investigation of the nature and frequency of potential adverse reactions related to different doses. Although the design for safety evaluation is case by case, the issues about metabolic fate, mechanism, toxicity profiles, optimal biologic dose (OBD), monitoring, and long-term follow-up should be designed. Monitoring classified as general procedures, recording of symptoms and common clinical measurements, and special procedures relevant to intended use of the drug. Long-term follow-up emphasizes subject survival and serious adverse issues, including hematologic, immunologic, neurologic, or oncologic issues. In addition to safety assessment, routes of administration, feasibility of administration and pharmacologic activity are also important topics. Phase I studies generally involve 20 to 80 subjects who are either healthy volunteers or patients. The participants in phase II and III are people who have a certain disease. Phase II and II trials involve a few hundred subjects to several thousand subjects. Phase II mainly gathers information about relationships between effectiveness and dose. This phase needs to be controlled and closely monitored. Phase III, expands in population scale and duration and is intended to collect sufficient information about effectiveness and safety to assess the overall risk-benefit relationship and provide appropriate basis for labeling.
Following the completion of clinical trials, applicants should submit a Biologics License Application (BLA) to the FDA (21CFR600-680) before launching the therapy in to the market (Figure 2). After the product has been approved for commercialization, post-marketing surveillance, which is a part of a phase IV trial, may be requested. Monitoring adverse events is the emphasis of this phase and the results will be used to update drug labeling and to reevaluate the risks of approval.
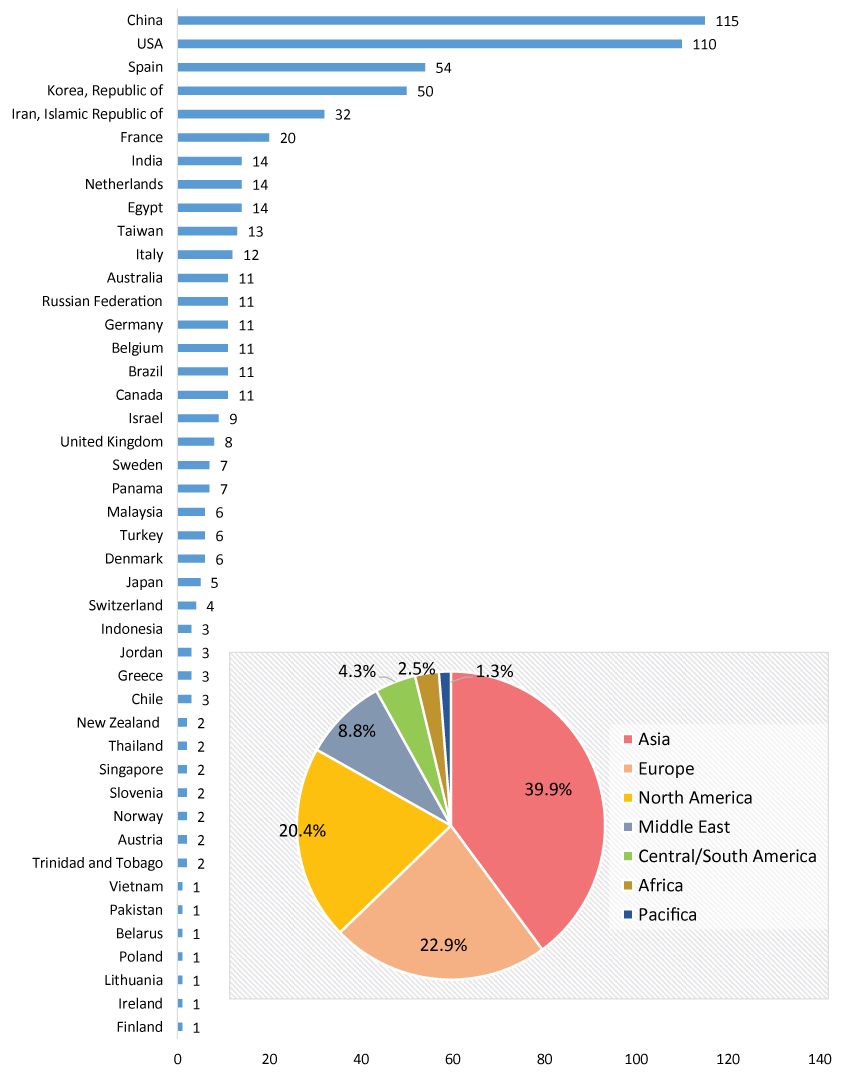
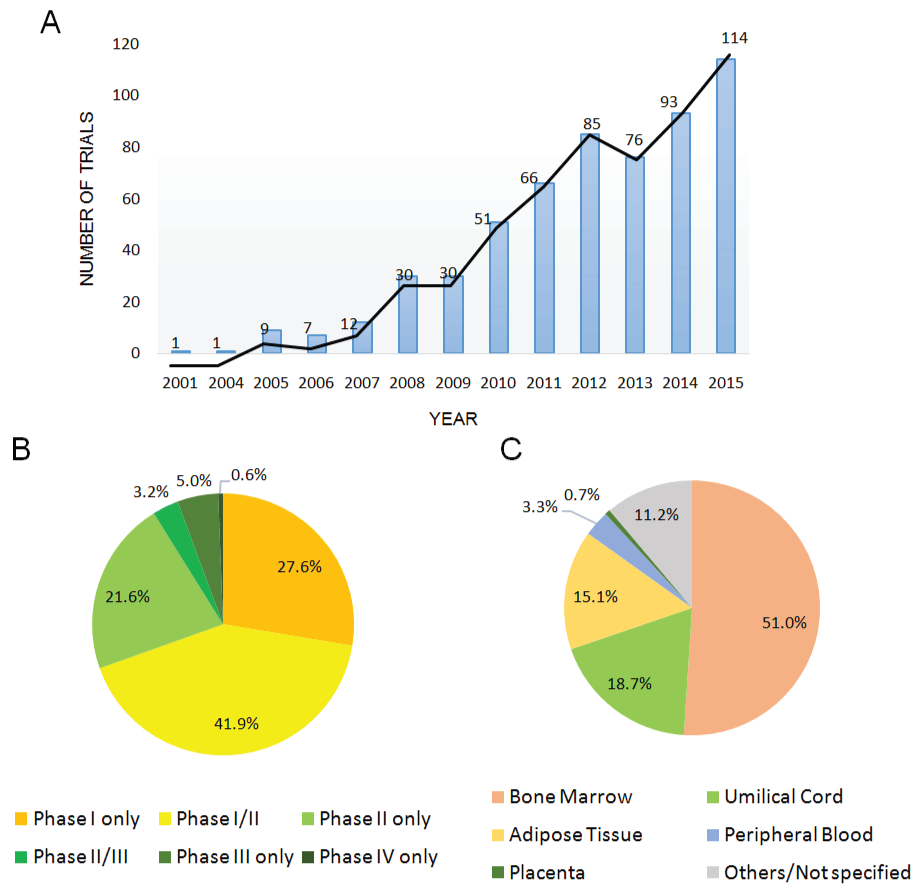
Currently, there are approximately 578 trials of MSC-based products for the investigation of their therapeutic potential (sources from the public clinical trials database http://www.clinicaltrials.gov, "Mesenchymal Stem Cell" queried on Jan. 18th, 2016). The highest activity is found in Asia (39.9%), Europe (22.9%), and North America (20.4%, mainly in the U.S.) (Figure 3). In particular, China alone conducts almost 20% of the clinical trials registered, as the Chinese government set stem cell and regenerative medicine technology as a key task in its twelfth Five-year Plan released in 2011 [59]. The nation’s government has committed funding to stem cell research at approximately 500 million dollars [59,60]. As the number of clinical trials continued to grow from 2001 to 2015 (Figure 4A), a great majority of the clinical trials are in phase I (27.6%), phase II (21.6%) or phase I/II (41.9%) trials, whereas only 5% of the trials are in phase III (Figure 4B). While there are 250 more cases to compare to several months ago, the distribution of trials by phase is similar, suggesting that most of the products are not moving forward in the clinical pipeline [6]. Over half of the trials (51%) are using MSC from the bone marrow, while umbilical cord- and adipose tissue-derived MSC are also popular, with 18.7% and 15.1% use, respectively (Figure 4C).
.
Figure 4: (A) Trend in number of registered clinical trials of mesenchymal stem cells-based therapy in patients from 2001 to 2015; (B) Registered MSC clinical trials classified by clinical phase; (C) MSC from different sources applied in current clinical trials. All of the data collected from www.clinicaltrials.gov (Jan. 18th, 2015) with the term "mesenchymal stem cells" listed 578 trials.
View Figure 4
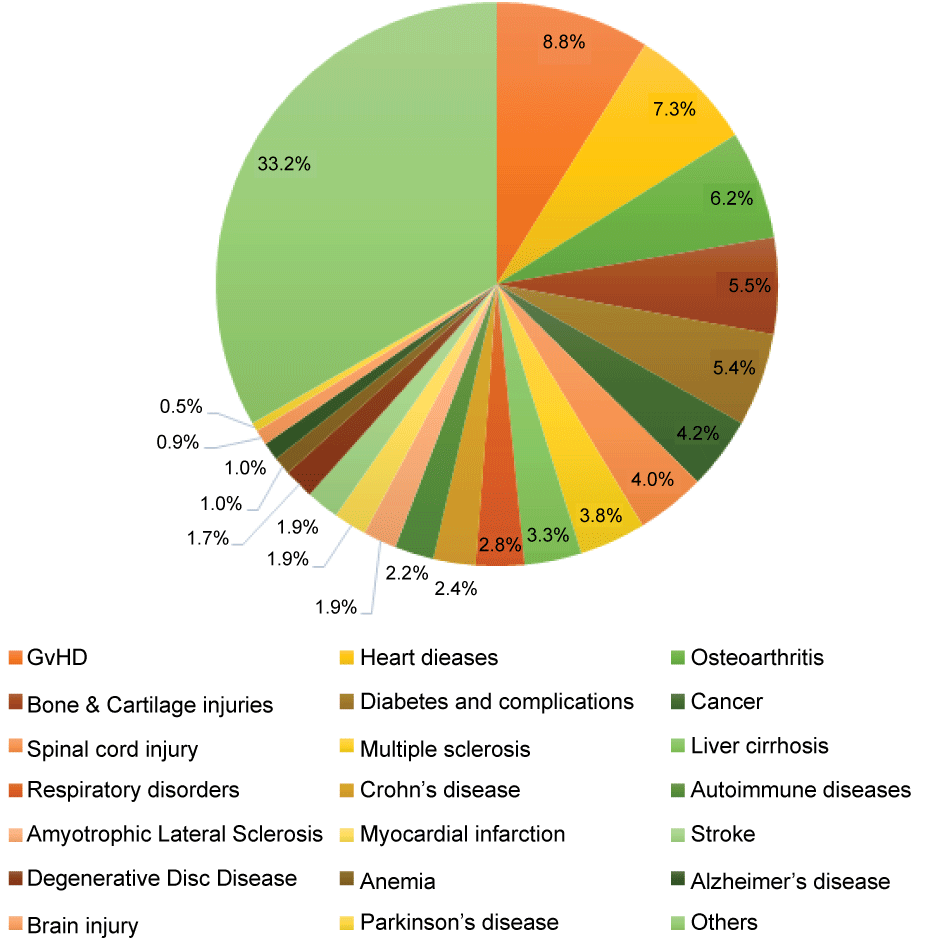
MSC has been applied clinically in treating a wide range of diseases for their multipotency, immunomodulatory properties, homing abilities, and the ability to secrete bioactive molecules assisting in the recovery and repair of damaged tissues [61]. Proposed indications include graft-versus-host diseases (GvHD, 8.8%), heart diseases (7.3%), osteoarthritis (6.2%), bone and cartilage injuries (5.5%), diabetes and its complications (5.4%), cancer (4.2%), spinal cord injury (4.0%), multiple sclerosis (3.8%), liver cirrhosis (3.3%), respiratory disorders (2.8%), Crohn’s disease (2.4%), autoimmune diseases (2.2%), and many others (Figure 5). Table 3 highlights the outcomes of some of the clinical trials reported over the past five years. These reports mostly claim the safety and feasibility of their therapy, while the efficacy of the treatment varies in different studies. This suggest that MSC therapy is at the least a safe approach to treat diseases, but its therapeutic potential requires further investigation and demonstration by researchers and clinicians.
.
Figure 5: MSC-based clinical trials categorized by indications. Data gathered from ClinicalTrials.gov. GvHD: Graft-versus-host disease.
View Figure 5
![]()
Table 3: Highlights of MSC therapy outcomes from published clinical trial reports (Jan., 2011- Mar., 2016).
View Table 3
In 2011, the MFDS in Korea approved the first MSC drug called Hearticellgram®-AMI (Pharmicell) for acute myocardial infarction treatment. Since then, eight other MSC therapeutic products were approved and released onto the market, including the well-known Prochymal® for acute GvHD treatment, which was first developed by Osiris Therapeutics and later off-loaded to Melbourne-based Mesoblast Ltd. [62]. Table 4 lists current MSC therapies available on the market and their indications.
![]()
Table 4: MSC therapeutics products on the market. (Data from 2012; sources from official websites of each company, [118,119])
View Table 4
Future Perspectives
MSC are the most commonly used stem cells in clinical applications currently. Still, there are several major hindrances to widening their use [4]. The establishment and implementation of controls for safety, quality, and efficacy of an MSC-based product remains to be the greatest challenge. More in-depth studies are necessary to determine whether certain MSC sources are more beneficial in certain diseases and if their safety and efficacy profiles are similar [7]. The high-throughput dynamic multiple omics system (HiDOS) is an advanced technique for understanding MSC behavior through the use of genomic, proteomic, cell image assays, which provide integrated big data information on MSC in each tissues niche, from fetus and adult sources, in their immune modulation, tissue repair, or self-renewal and differentiation capacities. This database will enhance our understanding of MSC in biology and help define the safety and potency among various MSC samples among variable proteins and genetic information. The enactment of standards by regulatory authorities should accelerate to meet the fast-paced development of MSC therapies and the challenges that follow. Close communication and collaboration is necessary among research teams, clinicians performing clinical trials, and industry. We believe that MSC will continue to be one of the public’s great interests and serve as an ultimate solution for a wide array of diseases.
References
-
Daley GQ, Scadden DT (2008) Prospects for stem cell-based therapy. Cell 132: 544-548.
-
Bieback K, Kinzebach S, Karagianni M (2011) Translating research into clinical scale manufacturing of mesenchymal stromal cells. Stem cells international 2010: 193519.
-
Kern S, Eichler H, Stoeve J, Klüter H, Bieback K (2006) Comparative analysis of mesenchymal stem cells from bone marrow, umbilical cord blood, or adipose tissue.Stem Cells 24: 1294-1301.
-
Wei X, Yang X, Han ZP, Qu FF, Shao L, et al. (2013) Mesenchymal stem cells: a new trend for cell therapy. Acta pharmacologica Sinica 34: 747-754.
-
Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, et al. (1999) Multilineage potential of adult human mesenchymal stem cells.Science 284: 143-147.
-
Trounson A, McDonald C (2015) Stem Cell Therapies in Clinical Trials: Progress and Challenges.Cell Stem Cell 17: 11-22.
-
Dimarino AM, Caplan AI, Bonfield TL (2013) Mesenchymal stem cells in tissue repair. Frontiers in immunology 4: 201.
-
Bieback K, Kern S, Kocaomer A, Ferlik K, Bugert P (2008) Comparing mesenchymal stromal cells from different human tissues: bone marrow, adipose tissue and umbilical cord blood. Bio-medical materials and engineering 18: S71-6.
-
Stolzing A, Jones E, McGonagle D, Scutt A (2008) Age-related changes in human bone marrow-derived mesenchymal stem cells: consequences for cell therapies.Mech Ageing Dev 129: 163-173.
-
Huang NF, Li S (2008) Mesenchymal stem cells for vascular regeneration. Regenerative medicine 3: 877-892.
-
De Coppi P, Bartsch G, Jr., Siddiqui MM, Xu T, Santos CC, et al. (2007) Isolation of amniotic stem cell lines with potential for therapy. Nature biotechnology 25: 100-106.
-
Perry BC, Zhou D, Wu X, Yang FC, Byers MA, et al. (2008) Collection, cryopreservation, and characterization of human dental pulp-derived mesenchymal stem cells for banking and clinical use. Tissue engineering Part C, Methods 14: 149-56.
-
Harvanová D, Tóthová T, Sarišský M, Amrichová J, Rosocha J (2011) Isolation and characterization of synovial mesenchymal stem cells.Folia Biol (Praha) 57: 119-124.
-
Mrozik K, Gronthos S, Shi S, Bartold PM (2010) A method to isolate, purify, and characterize human periodontal ligament stem cells.Methods Mol Biol 666: 269-284.
-
Letouzey V, Tan KS, Deane JA, Ulrich D, Gurung S, et al. (2015) Isolation and characterisation of mesenchymal stem/stromal cells in the ovine endometrium.PLoS One 10: e0127531.
-
Chen YS, Pelekanos RA, Ellis RL, Horne R, Wolvetang EJ, Fisk NM (2012) Small molecule mesengenic induction of human induced pluripotent stem cells to generate mesenchymal stem/stromal cells. Stem cells translational medicine 1: 83-95.
-
Zou L, Luo Y, Chen M, Wang G, Ding M, et al. (2013) A simple method for deriving functional MSCs and applied for osteogenesis in 3D scaffolds.Sci Rep 3: 2243.
-
Guillot PV, Gotherstrom C, Chan J, Kurata H, Fisk NM (2007) Human first-trimester fetal MSC express pluripotency markers and grow faster and have longer telomeres than adult MSC. Stem cells 25: 646-654.
-
Wang L, Tran I, Seshareddy K, Weiss ML, Detamore MS (2009) A comparison of human bone marrow-derived mesenchymal stem cells and human umbilical cord-derived mesenchymal stromal cells for cartilage tissue engineering. Tissue engineering Part A 15: 2259-2266.
-
Bieback K, Ha VA, Hecker A, Grassl M, Kinzebach S, et al. (2010) Altered gene expression in human adipose stem cells cultured with fetal bovine serum compared to human supplements. Tissue engineering Part A 16: 3467-3484.
-
Bieback K, Hecker A, Kocaomer A, Lannert H, Schallmoser K, et al. (2009) Human alternatives to fetal bovine serum for the expansion of mesenchymal stromal cells from bone marrow. Stem cells 27: 2331-2341.
-
Freeman BT, Jung JP, Ogle BM (2015) Single-Cell RNA-Seq of Bone Marrow-Derived Mesenchymal Stem Cells Reveals Unique Profiles of Lineage Priming.PLoS One 10: e0136199.
-
Tchkonia T, Giorgadze N, Pirtskhalava T, Tchoukalova Y, Karagiannides I, et al. (2002) Fat depot origin affects adipogenesis in primary cultured and cloned human preadipocytes.Am J Physiol Regul Integr Comp Physiol 282: R1286-1296.
-
Niesler CU, Siddle K, Prins JB (1998) Human preadipocytes display a depot-specific susceptibility to apoptosis.Diabetes 47: 1365-1368.
-
Introna M, Lucchini G, Dander E, Galimberti S, Rovelli A, et al. (2014) Treatment of graft versus host disease with mesenchymal stromal cells: a phase I study on 40 adult and pediatric patients. Biol Blood Marrow Transplant 20: 375-381.
-
Zhao Q, Ren H, Han Z (2015) Mesenchymal stem cells: Immunomodulatory capability and clinical potential in immune diseases. Journal of cellular immunotherapy 1-18.
-
Department FaD (2008) Guidance for FDA Reviewers and Sponsors: Content and Review of Chemistry, Manufacturing, and Control (CMC) Information for Human Somatic Cell Therapy Investigational New Drug Applications (INDs). In: CBER.
-
Sensebé L, Gadelorge M, Fleury-Cappellesso S (2013) Production of mesenchymal stromal/stem cells according to good manufacturing practices: a review.Stem Cell Res Ther 4: 66.
-
Kennard L, Thanabalasundaram G, Tailor HD, Khan WS (2011) Advances and developments in the use of human mesenchymal stem cells - a few considerations.Open Orthop J 5: 249-252.
-
Cook MM, Futrega K, Osiecki M, Kabiri M, Kul B, et al. (2012) Micromarrows--three-dimensional coculture of hematopoietic stem cells and mesenchymal stromal cells.Tissue Eng Part C Methods 18: 319-328.
-
Administration FaD (2011) Guidance for Industry: Current Good Tissue Practice (cGTP) and Additional Requirments for Manufacturers of Human Cells, Tissues, and Cellular and Tissue-based products (HCT/Ps). In: CBER.
-
Giancola R, Bonfini T, Iacone A (2012) Cell therapy: cGMP facilities and manufacturing.Muscles Ligaments Tendons J 2: 243-247.
-
Colter DC, Sekiya I, Prockop DJ (2001) Identification of a subpopulation of rapidly self-renewing and multipotential adult stem cells in colonies of human marrow stromal cells.Proc Natl Acad Sci U S A 98: 7841-7845.
-
Banfi A, Muraglia A, Dozin B, Mastrogiacomo M, Cancedda R, et al. (2000) Proliferation kinetics and differentiation potential of ex vivo expanded human bone marrow stromal cells: Implications for their use in cell therapy. Experimental hematology 28: 707-715.
-
Rustichelli D, Castiglia S, Gunetti M, Mareschi K, Signorino E, et al. (2013) Validation of analytical methods in compliance with good manufacturing practice: a practical approach. Journal of translational medicine 11:197.
-
Tarte K, Gaillard J, Lataillade JJ, Fouillard L, Becker M, et al. (2010) Clinical-grade production of human mesenchymal stromal cells: occurrence of aneuploidy without transformation.Blood 115: 1549-1553.
-
Park KS, Kim YS, Kim JH, Choi B, Kim SH, et al. (2010) Trophic molecules derived from human mesenchymal stem cells enhance survival, function, and angiogenesis of isolated islets after transplantation.Transplantation 89: 509-517.
-
Ranganath SH, Levy O, Inamdar MS, Karp JM (2012) Harnessing the mesenchymal stem cell secretome for the treatment of cardiovascular disease.Cell Stem Cell 10: 244-258.
-
Hsieh JY, Wang HW, Chang SJ, Liao KH, Lee IH, et al. (2013) Mesenchymal stem cells from human umbilical cord express preferentially secreted factors related to neuroprotection, neurogenesis, and angiogenesis. PloS one 8: e72604.
-
Chang CP, Chio CC, Cheong CU, Chao CM, Cheng BC, et al. (2013) Hypoxic preconditioning enhances the therapeutic potential of the secretome from cultured human mesenchymal stem cells in experimental traumatic brain injury.Clin Sci (Lond) 124: 165-176.
-
Kocaoemer A, Kern S, Kluter H, Bieback K (2007) Human AB serum and thrombin-activated platelet-rich plasma are suitable alternatives to fetal calf serum for the expansion of mesenchymal stem cells from adipose tissue. Stem cells 25: 1270-1278.
-
Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini F, et al. (2006) Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy 8: 315-317.
-
Lorenz K, Sicker M, Schmelzer E, Rupf T, Salvetter J, Schulz-Siegmund M, et al. (2008) Multilineage differentiation potential of human dermal skin-derived fibroblasts. Experimental dermatology 17: 925-932.
-
Crisan M, Yap S, Casteilla L, Chen CW, Corselli M, et al. (2008) A perivascular origin for mesenchymal stem cells in multiple human organs.Cell Stem Cell 3: 301-313.
-
Feng J, Mantesso A, De Bari C, Nishiyama A, Sharpe PT (2011) Dual origin of mesenchymal stem cells contributing to organ growth and repair.Proc Natl Acad Sci U S A 108: 6503-6508.
-
Holley RJ, Tai G, Williamson AJ, Taylor S, Cain SA, et al. (2015) Comparative quantification of the surfaceome of human multipotent mesenchymal progenitor cells.Stem Cell Reports 4: 473-488.
-
Shen SP, Liu WT, Lin Y, Li YT, Chang CH, et al. (2015) EphA2 is a biomarker of hMSCs derived from human placenta and umbilical cord.Taiwan J Obstet Gynecol 54: 749-756.
-
Alt E, Yan Y, Gehmert S, Song YH, Altman A, et al. (2011) Fibroblasts share mesenchymal phenotypes with stem cells, but lack their differentiation and colony-forming potential.Biol Cell 103: 197-208.
-
Sng J, Lufkin T (2012) Emerging stem cell therapies: treatment, safety, and biology.Stem Cells Int 2012: 521343.
-
De Ugarte DA, Alfonso Z, Zuk PA, Elbarbary A, Zhu M, et al. (2003) Differential expression of stem cell mobilization-associated molecules on multi-lineage cells from adipose tissue and bone marrow.Immunol Lett 89: 267-270.
-
Parolini O, Alviano F, Bagnara GP, Bilic G, Bühring HJ, et al. (2008) Concise review: isolation and characterization of cells from human term placenta: outcome of the first international Workshop on Placenta Derived Stem Cells.Stem Cells 26: 300-311.
-
Sarugaser R, Lickorish D, Baksh D, Hosseini MM, Davies JE (2005) Human umbilical cord perivascular (HUCPV) cells: a source of mesenchymal progenitors.Stem Cells 23: 220-229.
-
Minimal Manipulation of Human Cells, Tissues, and Cellular and Tissue-Based Products -Draft Guidance for Industry and Food and Drug Administration Staff. In: Administration USDoHaHSFaD, editor.2014.
-
Administration FaD. 21 Code of Federal Regulations Part 58: Good Laboratory Practice for Non-clinical Laboratory Studies. 21.
-
Administration FaD. 21 Code of Federal Regulations Part 211: Current Good Manufacturing Practice for Finished Pharmaceuticals. 21.
-
Administration FaD. Guidance for Industry: Preclinical Assessment of Investigational Cellular and Gene Therapy Products. In: CBER, editor.2013.
-
Administration FaD. Considerations for the Design of Early-Phase Clniical Trials of Cellular and Gene Therapy Products -- Guidance for Industry. In: CBER, editor.2015.
-
(NIH) NIoH. Ethics in Clinical Research. 2015
-
Wang L, Xu XM, M. TJ (2014) Clinical Use of Mesenchymal Stem Cells and Regulatory Aspects in China. CellR4 2: e974.
-
Yuan W, Sipp D, Wang ZZ, Deng H, Pei D, et al. (2012) Stem cell science on the rise in China.Cell Stem Cell 10: 12-15.
-
Wang S, Qu X, Zhao RC (2012) Clinical applications of mesenchymal stem cells.J Hematol Oncol 5: 19.
-
Waltz E (2013) Mesoblast acquires Osiris' stem cell business. Nature biotechnology 31:1061.
-
Halfon S, Abramov N, Grinblat B, Ginis I (2011) Markers distinguishing mesenchymal stem cells from fibroblasts are downregulated with passaging.Stem Cells Dev 20: 53-66.
-
Del Pino A, Ligero G, Lopez MB, Navarro H, Carrillo JA, et al. (2015) Morphology, cell viability, karyotype, expression of surface markers and plasticity of three human primary cell line cultures before and after the cryostorage in LN2 and GN2. Cryobiology 70:1-8.
-
Brohem CA, de Carvalho CM, Radoski CL, Santi FC, Baptista MC, et al. (2013) Comparison between fibroblasts and mesenchymal stem cells derived from dermal and adipose tissue. International journal of cosmetic science 35: 448-457.
-
Cappellesso-Fleury S, Puissant-Lubrano B, Apoil PA, Titeux M, Winterton P, et al. (2010) Human fibroblasts share immunosuppressive properties with bone marrow mesenchymal stem cells. Journal of clinical immunology 30: 607-619.
-
Lupatov AY, Vdovin AS, Vakhrushev IV, Poltavtseva RA, Yarygin KN (2015) Comparative analysis of the expression of surface markers on fibroblasts and fibroblast-like cells isolated from different human tissues. Bulletin of experimental biology and medicine 158: 537-543.
-
Yamamoto K, Kishida T, Sato Y, Nishioka K, Ejima A, et al. (2015) Direct conversion of human fibroblasts into functional osteoblasts by defined factors. Proceedings of the National Academy of Sciences of the United States of America 112: 6152-6157.
-
Rosen ED, MacDougald OA (2006) Adipocyte differentiation from the inside out.Nat Rev Mol Cell Biol 7: 885-896.
-
Masuno H, Kidani T, Sekiya K, Sakayama K, Shiosaka T, et al. (2002) Bisphenol A in combination with insulin can accelerate the conversion of 3T3-L1 fibroblasts to adipocytes.J Lipid Res 43: 676-684.
-
Jeney F, Bazsó-Dombi E, Oravecz K, Szabó J, Nagy IZ (2000) Cytochemical studies on the fibroblast-preadipocyte relationships in cultured fibroblast cell lines.Acta Histochem 102: 381-389.
-
Outani H, Okada M, Yamashita A, Nakagawa K, Yoshikawa H, et al. (2013) Direct induction of chondrogenic cells from human dermal fibroblast culture by defined factors.PLoS One 8: e77365.
-
Mizuno S, Glowacki J (2005) Low oxygen tension enhances chondroinduction by demineralized bone matrix in human dermal fibroblasts in vitro.Cells Tissues Organs 180: 151-158.
-
Mazzini L, Mareschi K, Ferrero I, Miglioretti M, Stecco A, et al. (2012) Mesenchymal stromal cell transplantation in amyotrophic lateral sclerosis: a long-term safety study.Cytotherapy 14: 56-60.
-
Oh KW, Moon C, Kim HY, Oh SI, Park J, et al. (2015) Phase I trial of repeated intrathecal autologous bone marrow-derived mesenchymal stromal cells in amyotrophic lateral sclerosis. Stem cells translational medicine 4: 590-597.
-
Karamouzian S, Nematollahi-Mahani SN, Nakhaee N, Eskandary H (2012) Clinical safety and primary efficacy of bone marrow mesenchymal cell transplantation in subacute spinal cord injured patients.Clin Neurol Neurosurg 114: 935-939.
-
Mendonca MV, Larocca TF, de Freitas Souza BS, Villarreal CF, Silva LF, et al. (2014) Safety and neurological assessments after autologous transplantation of bone marrow mesenchymal stem cells in subjects with chronic spinal cord injury. Stem cell research & therapy 5:126.
-
Orozco L, Soler R, Morera C, Alberca M, Sanchez A, Garcia-Sancho J (2011) Intervertebral disc repair by autologous mesenchymal bone marrow cells: a pilot study. Transplantation 92: 822-828.
-
Mathiasen AB, Haack-Sørensen M, Jørgensen E, Kastrup J (2013) Autotransplantation of mesenchymal stromal cells from bone-marrow to heart in patients with severe stable coronary artery disease and refractory angina--final 3-year follow-up.Int J Cardiol 170: 246-251.
-
Lee JW, Lee SH, Youn YJ, Ahn MS, Kim JY, et al. (2014) A randomized, open-label, multicenter trial for the safety and efficacy of adult mesenchymal stem cells after acute myocardial infarction. Journal of Korean medical science 29: 23-31.
-
Jang YO, Kim YJ, Baik SK, Kim MY, Eom YW, et al. (2014) Histological improvement following administration of autologous bone marrow-derived mesenchymal stem cells for alcoholic cirrhosis: a pilot study. Liver international: official journal of the International Association for the Study of the Liver 34: 33-41.
-
El-Ansary M, Abdel-Aziz I, Mogawer S, Abdel-Hamid S, Hammam O, et al. (2012) Phase II trial: undifferentiated versus differentiated autologous mesenchymal stem cells transplantation in Egyptian patients with HCV induced liver cirrhosis. Stem cell reviews 8: 972-981.
-
Llufriu S, Sepulveda M, Blanco Y, Marin P, Moreno B, Berenguer J, et al. (2014) Randomized placebo-controlled phase II trial of autologous mesenchymal stem cells in multiple sclerosis. PloS one 9:e113936.
-
Connick P, Kolappan M, Crawley C, Webber DJ, Patani R, et al. (2012) Autologous mesenchymal stem cells for the treatment of secondary progressive multiple sclerosis: an open-label phase 2a proof-of-concept study. The Lancet Neurology 11:150-156.
-
Connick P, Kolappan M, Patani R, Scott MA, Crawley C, et al. (2011) The mesenchymal stem cells in multiple sclerosis (MSCIMS) trial protocol and baseline cohort characteristics: an open-label pre-test: post-test study with blinded outcome assessments. Trials 12:62.
-
Orozco L, Munar A, Soler R, Alberca M, Soler F, et al. (2013) Treatment of knee osteoarthritis with autologous mesenchymal stem cells: a pilot study.Transplantation 95: 1535-1541.
-
Reinders ME, de Fijter JW, Roelofs H, Bajema IM, de Vries DK, et al. (2013) Autologous bone marrow-derived mesenchymal stromal cells for the treatment of allograft rejection after renal transplantation: results of a phase I study. Stem cells translational medicine 2:107-111.
-
Lasala GP, Silva JA, Minguell JJ (2012) Therapeutic angiogenesis in patients with severe limb ischemia by transplantation of a combination stem cell product.J Thorac Cardiovasc Surg 144: 377-382.
-
Heldman AW, DiFede DL, Fishman JE, Zambrano JP, Trachtenberg BH, et al. (2014) Transendocardial mesenchymal stem cells and mononuclear bone marrow cells for ischemic cardiomyopathy: the TAC-HFT randomized trial.JAMA 311: 62-73.
-
Hare JM, Fishman JE, Gerstenblith G, DiFede Velazquez DL, Zambrano JP, et al. (2012) Comparison of allogeneic vs autologous bone marrowâ€"derived mesenchymal stem cells delivered by transendocardial injection in patients with ischemic cardiomyopathy: the POSEIDON randomized trial.JAMA 308: 2369-2379.
-
Cho YB, Park KJ, Yoon SN, Song KH, Kim do S, et al. (2015) Long-term results of adipose-derived stem cell therapy for the treatment of Crohn's fistula.Stem Cells Transl Med 4: 532-537.
-
Tzouvelekis A, Paspaliaris V, Koliakos G, Ntolios P, Bouros E, Oikonomou A, et al. (2013) A prospective, non-randomized, no placebo-controlled, phase Ib clinical trial to study the safety of the adipose derived stromal cells-stromal vascular fraction in idiopathic pulmonary fibrosis. Journal of translational medicine 11:171.
-
Jo CH, Lee YG, Shin WH, Kim H, Chai JW, et al. (2014) Intra-articular injection of mesenchymal stem cells for the treatment of osteoarthritis of the knee: a proof-of-concept clinical trial.Stem Cells 32: 1254-1266.
-
Herreros MD, Garcia-Arranz M, Guadalajara H, De-La-Quintana P, Garcia-Olmo D, et al. (2012) Autologous expanded adipose-derived stem cells for the treatment of complex cryptoglandular perianal fistulas: a phase III randomized clinical trial (FATT 1: fistula Advanced Therapy Trial 1) and long-term evaluation. Dis Colon Rectum 55: 762-772.
-
Oh SK, Choi KH, Yoo JY, Kim DY, Kim SJ, et al. (2016) A Phase III Clinical Trial Showing Limited Efficacy of Autologous Mesenchymal Stem Cell Therapy for Spinal Cord Injury.Neurosurgery 78: 436-447.
-
Liang J, Zhang H, Hua B, Wang H, Lu L, et al. (2010) Allogenic mesenchymal stem cells transplantation in refractory systemic lupus erythematosus: a pilot clinical study.Ann Rheum Dis 69: 1423-1429.
-
Woodworth TG, Furst DE (2014) Safety and feasibility of umbilical cord mesenchymal stem cells in treatment-refractory systemic lupus erythematosus nephritis: time for a double-blind placebo-controlled trial to determine efficacy. Arthritis research & therapy16:113.
-
Wilson JG, Liu KD, Zhuo H, Caballero L, McMillan M, et al. (2015) Mesenchymal stem (stromal) cells for treatment of ARDS: a phase 1 clinical trial.Lancet Respir Med 3: 24-32.
-
Gupta PK, Chullikana A, Parakh R, Desai S, Das A, et al. (2013) A double blind randomized placebo controlled phase I/II study assessing the safety and efficacy of allogeneic bone marrow derived mesenchymal stem cell in critical limb ischemia. Journal of translational medicine11:143.
-
Vega A, Martín-Ferrero MA, Del Canto F, Alberca M, García V, et al. (2015) Treatment of Knee Osteoarthritis With Allogeneic Bone Marrow Mesenchymal Stem Cells: A Randomized Controlled Trial.Transplantation 99: 1681-1690.
-
Sanchez-Guijo F, Caballero-Velazquez T, Lopez-Villar O, Redondo A, Parody R, et al. (2014) Sequential third-party mesenchymal stromal cell therapy for refractory acute graft-versus-host disease. Biol Blood Marrow Transplant 20:1580-1585.
-
Kuzmina LA, Petinati NA, Parovichnikova EN, Lubimova LS, Gribanova EO, et al. (2012) Multipotent Mesenchymal Stromal Cells for the Prophylaxis of Acute Graft-versus-Host Disease-A Phase II Study.Stem Cells Int 2012: 968213.
-
Muroi K, Miyamura K, Okada M, Yamashita T, Murata M, et al. (2016) Bone marrow-derived mesenchymal stem cells (JR-031) for steroid-refractory grade III or IV acute graft-versus-host disease: a phase II/III study.Int J Hematol 103: 243-250.
-
Wang D, Li J, Zhang Y, Zhang M, Chen J, et al. (2014) Umbilical cord mesenchymal stem cell transplantation in active and refractory systemic lupus erythematosus: a multicenter clinical study. Arthritis research & therapy16:R79.
-
Chang YS, Ahn SY, Yoo HS, Sung SI, Choi SJ, et al. (2014) Mesenchymal stem cells for bronchopulmonary dysplasia: phase 1 dose-escalation clinical trial.J Pediatr 164: 966-972.
-
Yang SS, Kim NR, Park KB, Do YS, Roh K, et al. (2013) A phase I study of human cord blood-derived mesenchymal stem cell therapy in patients with peripheral arterial occlusive disease. International journal of stem cells 6:37-44.
-
Lv YT, Zhang Y, Liu M, Qiuwaxi JN, Ashwood P, et al. (2013) Transplantation of human cord blood mononuclear cells and umbilical cord-derived mesenchymal stem cells in autism.J Transl Med 11: 196.
-
Chambers DC, Enever D, Ilic N, Sparks L, Whitelaw K, et al. (2014) A phase 1b study of placenta-derived mesenchymal stromal cells in patients with idiopathic pulmonary fibrosis.Respirology 19: 1013-1018.
-
Lublin FD, Bowen JD, Huddlestone J, Kremenchutzky M, Carpenter A, et al. (2014) Human placenta-derived cells (PDA-001) for the treatment of adults with multiple sclerosis: a randomized, placebo-controlled, multiple-dose study. Multiple sclerosis and related disorders 3: 696-704.
-
Perin EC, Borow KM, Silva GV, DeMaria AN, Marroquin OC, et al. (2015) A Phase II Dose-Escalation Study of Allogeneic Mesenchymal Precursor Cells in Patients With Ischemic or Nonischemic Heart Failure.Circ Res 117: 576-584.
-
Maziarz RT, Devos T, Bachier CR, Goldstein SC, Leis JF, et al. (2015) Single and multiple dose MultiStem (multipotent adult progenitor cell) therapy prophylaxis of acute graft-versus-host disease in myeloablative allogeneic hematopoietic cell transplantation: a phase 1 trial. Biol Blood Marrow Transplant 21:720-728.
-
Forbes GM, Sturm MJ, Leong RW, Sparrow MP, Segarajasingam D, et al. (2014) A phase 2 study of allogeneic mesenchymal stromal cells for luminal Crohn's disease refractory to biologic therapy. Clin Gastroenterol Hepatol 12: 64-71.
-
Pérez-Simon JA, López-Villar O, Andreu EJ, Rifón J, Muntion S, et al. (2011) Mesenchymal stem cells expanded in vitro with human serum for the treatment of acute and chronic graft-versus-host disease: results of a phase I/II clinical trial.Haematologica 96: 1072-1076.
-
Prasad VK, Lucas KG, Kleiner GI, Talano JA, Jacobsohn D, et al. (2011) Efficacy and safety of ex vivo cultured adult human mesenchymal stem cells (Prochymal) in pediatric patients with severe refractory acute graft-versus-host disease in a compassionate use study. Biology of blood and marrow transplantation :journal of the American Society for Blood and Marrow Transplantation17: 534-541.
-
de la Portilla F, Alba F, Garcia-Olmo D, Herrerias JM, Gonzalez FX, et al. (2013) Expanded allogeneic adipose-derived stem cells (eASCs) for the treatment of complex perianal fistula in Crohn's disease: results from a multicenter phase I/IIa clinical trial. International journal of colorectal disease 28: 313-323.
-
Liu X, Zheng P, Wang X, Dai G, Cheng H, Zhang Z, et al. (2014) A preliminary evaluation of efficacy and safety of Wharton's jelly mesenchymal stem cell transplantation in patients with type 2 diabetes mellitus. Stem cell research & therapy 5:57.
-
Powell RJ, Marston WA, Berceli SA, Guzman R, Henry TD, Longcore AT, et al. (2012) Cellular therapy with Ixmyelocel-T to treat critical limb ischemia: the randomized, double-blind, placebo-controlled RESTORE-CLI trial. Molecular therapy : the journal of the American Society of Gene Therapy 20:1280-1286.
-
Lee S, Kwon T, Chung EK, Lee JW (2014) The market trend analysis and prospects of scaffolds for stem cells.Biomater Res 18: 11.
-
Bersenev A (2012) Stem Cell Therapeutic Products on the Market. Regenmed Digest.