International Journal of Surgery Research and Practice
Markedly Elevated Tumor Markers with a Benign Epidermoid Cyst of Spleen
Jane Lee*, Jingjing Sherman and L Brian Katz
Department of Surgery, Mount Sinai Hospital, New York, USA
*Corresponding author: Jane Lee, Department of Surgery, Mount Sinai Hospital, New York, NY, USA, E-mail: jane0516@gmail.com
Int J Surg Res Pract, IJSRP-3-048, (Volume 3, Issue 2), Case Report; ISSN: 2378-3397
Received: July 01, 2015 | Accepted: October 13, 2016 | Published: October 17, 2016
Citation: Lee J, Sherman J, Katz LB (2016) Markedly Elevated Tumor Markers with a Benign Epidermoid Cyst of Spleen. Int J Surg Res Pract 3:048. 10.23937/2378-3397/1410048
Copyright: © 2016 Lee J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A 25-year old female presented with left upper quadrant pain of several weeks duration. Her labs were significant for elevated tumor markers including CA 19-9, CA 125 and CEA. Computed tomography of the abdomen showed ascites, ovarian cysts and enlarged spleen with a large cystic lesion measuring approximately 9.9 × 3.2 cm. Diagnostic laparoscopy revealed an enlarged cystic spleen, ovarian cysts and no evidence of malignancy. Splenectomy was performed along with ascites cytology, peritoneal and omental biopsies. Following surgery, tumor marker levels decreased. Pathologic examination of the specimen with immunohistochemistry confirmed epidermoid cyst of the spleen.
Introduction
Serum tumor markers are used to detect various cancers and monitor response to therapy, however, they can also be elevated in various benign conditions. Cancer antigen 19-9 is mainly used to monitor response to therapy or recurrence of pancreatic cancer, gastric cancer, gallbladder cancer, cholangiocarcinoma, or adenocarcinoma of the ampulla of Vater and may be elevated in ovarian cancer. Cancer antigen 125 is mainly used as a biomarker for epithelial ovarian cancer. It is a large transmembrane glycoprotein derived from the epithelia of the fallopian tube, endometrium, and endocervix [1,2]. The level also varies slightly with the menstrual cycle [3]. Carcinoembryonic antigen is a protein found in embryonic/fetal tissue and serum levels diminish after birth. However, it can be elevated in malignancies especially mucinous cancers of the colon and ovaries. Breast, pancreas, thyroid, or lung cancers can also exhibit elevated CEA [4]. CEA can also be elevated in other conditions such as smoking, cholecystitis, cirrhosis, diverticulitis, IBD, pancretitis, and pseudomyxoma peritonei [4].
We describe a case of a young healthy female presenting with abdominal pain and elevated tumor markers with CT findings significant for ascites, ovarian cysts and enlarged spleen with a large cystic lesion. The full work up and surgical management is described in detail.
Case Report
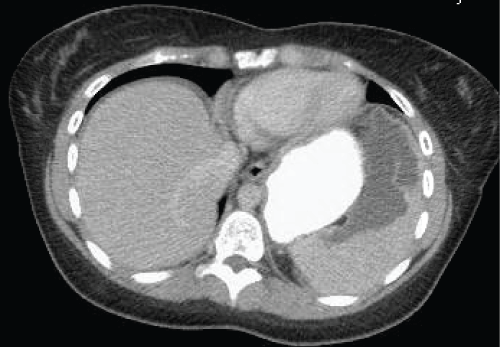
A 25-year old female presented with left upper quadrant pain of several weeks duration, which became more intense for 2 days prior to admission. Her past medical history was significant for a benign thyroid nodule, ovarian cysts, and surgical history of bilateral breast reduction. She was not taking any medications. Her abdominal exam was only significant for tenderness to palpation in the left upper quadrant. No discrete masses were palpable, and she had no signs of peritonitis. A computed tomography scan of the abdomen and pelvis was obtained, showing an enlarged spleen measuring approximately 13.0 × 5.8 × 12.4 cm, containing a large splenic cyst measuring 9.9 × 3.2 cm as shown in figure 1. Ascites fluid was also noted in the pelvis as well as bilateral ovarian cysts. Preoperative labs were remarkable for elevated tumor markers including CA 19-9 of 38221.7 U/ml (normal < 35 U/ml), CA 125 of 513 U/ml (normal < 35 U/ml), and CEA 38.7 ng/ml (normal < 3 ng/ml). Echinococcus IgG antibody titers were negative. Other lab values, including markers for ovarian pathology (inhibin A and B, AFP, beta-HCG, LDH) were within normal range.
.
Figure 1: CT scan of abdomen showing an enlarged spleen measuring approximately 13.0 × 5.8 × 12.4 cm, containing a large splenic cyst measuring 9.9 × 3.2 cm.
View Figure 1
Diagnostic laparoscopy was performed showing an enlarged spleen with a large splenic lesion, bilateral ovarian cysts and serous ascites. There was no evidence of malignancy, and all other organs appeared normal. Ascites fluid was sent for cytology, and peritoneal/omental biopsies were taken. Due to the large size of the cyst and its location near the hilum, a partial splenectomy could not be performed. Total splenectomy was then performed laparoscopically without complications. Postoperatively the patient did well and was discharged the following day. Postoperative labs showed significant decrease in tumor marker levels, CA 19-9 of 12902.5 U/ml, CA 125 of 208 U/ml, and CEA 9.8 ng/ml. She was doing well without any issues on postoperative follow-up.
Pathology
Specimen consisted of splenic tissue and cyst wall tissue (measuring 13 × 13 × 4.5 cm in aggregate) weighing 294 g. Pathology examination of the specimen confirmed epidermoid cyst of the spleen. Immunohistochemical stains showed cyst lining cells to be positive for CEA. Ascites fluid cytology was negative for malignant cells. Peritoneal and omental biopsies showed reactive histiocytic/mesothelial hyperplasia, negative for malignancy.
Discussion
We described a case of symptomatic non parasitic large splenic cyst presenting with elevated tumor markers and treated with laparoscopic splenectomy. Few cases of splenic cysts presenting with elevated tumor markers have been described in the literature. Takagi, et al. reported a 36 year old female with enlarged spleen discovered on routine physical exam [5]. CA 19-9 was 244 and she underwent an exploratory laparotomy revealing a splenic cyst 8 cm in diameter with necrosis and bleeding. Pathology showed splenic epidermoid cyst with staining positive for CA 19-9. Hoshino, et al. presented a 33-year-old female with abdominal pain with CA 19-9 of 3,347, and CT findings of a 10 cm splenic cyst [6]. Laparoscopic splenectomy was performed and pathological examination showed a benign true epidermal cyst of the spleen with positive immunohistochemical staining for CA 19-9. Yigitbasi, et al. described a similar case of a 30-year-old woman with splenic cyst and elevated CA 19-9 of 268 [7]. Patient underwent a splenectomy and the serum CA 19-9 level decreased to normal within 6 weeks.
Splenic lesions are becoming more commonly diagnosed with enhancements in current imaging technology. Asymptomatic splenic cysts may be incidentally found on imaging. Symptomatic splenic cysts are not very common, and occur mostly when the cyst is infected, ruptured, or enlarged causing mass effects. Patients may present with left upper quadrant pain, referred pain to the left shoulder, early satiety, and/or nausea/vomiting.
Splenic cysts can be classified into parasitic and nonparasitic cysts. Parasitic cysts are mostly hydatid cysts caused by Echinococcus, and account for approximately 5% of all splenic cysts in the U.S [8]. These cysts are treated by surgical resection as well as medications such as albendazole and mebendazole. Nonparasitic cysts are classified into primary/true cysts or secondary/pseudocysts by the presence or absence of cell lining. Epidermoid cysts account for approximately 90% of all primary cysts. 8 Majority of pseudocysts are post-traumatic cysts accounting for 70-80% of nonparasitic cysts [8].
Treatment depends on the size of the cyst as well as symptoms. Asymptomatic cysts < 5 cm can be observed. However, splenic cysts > 5 cm in diameter have greater risk of rupture and surgery should be considered [8]. Size of the cyst, location in relation to the hilum as well as within the parenchyma can all be contributing factors in deciding on the type of surgery, which can involve marsupialization for simple, superficial cysts, and laparoscopic or open partial or total splenectomy for multiple or large splenic cysts. Splenic tissue preservation is a desirable goal and may be pursued in cases where at least 25% of the spleen can be salvaged for proper function [8].
In cases such as ours with a young female presenting with elevated tumor markers and splenic cyst, the diagnosis of epidermoid cyst of the spleen should be considered high on the differential and immunohistochemical staining can be performed on the specimen to confirm the diagnosis. The tumor markers are expected to decrease and return to normal after splenectomy.
References
-
Jacobs I, Bast RC Jr (1989) The CA 125 tumour-associated antigen: a review of the literature. Hum Reprod 4: 1-12.
-
Dorigo O, Berek JS (2011) Personalizing CA 125 levels for ovarian cancer screening. Cancer Prev Res (Phila) 4: 1356-1359.
-
Grover S, Koh, H, Weideman P, Quinn MA (1992) The effect of the menstrual cycle on serum CA125 levels: a population study. Am J Obstet Gynecol 167: 1379-1381.
-
Menon U, Jacobs I (2000) Tumor markers. In: Hoskins W, Perez C, Young R, Principles and Practice of Gynecologic Oncology, Lippincott Williams & Wilkins, Philadelphia 165.
-
Takagi K, Takayama T, Moriguchi M, Hasegawa H, Niide O, et al. (2014) Gastrointestinal: case of accidentally discovered splenic epidermoid cyst with serum CA19-9 elevation. J Gastroenterol Hepatol 29: 231.
-
Hoshino A, Nakamura Y, Suzuki H, Mizutani S, Chihara N, et al. (2013) Giant epidermoid cyst of the spleen with elevated CA 19-9 production managed laparoscopically: report of a case. J Nippon Med Sch 80: 470-474.
-
Yigitbasi R, Karabicak I, Aydogan F, Erturk S, Bican O, et al. (2006) Benign splenic epithelial cyst accompanied by elevated CA 19-9 level: a case report. Mt Sinai J Med 73: 871-873.
-
Nguyen HT, Marohn MR (2011) Cysts, Tumors, and abscesses of the spleen. In: Current Surgical Therapy, Cameron JL, Cameron AM (10th edn), Elsevier Saunders, Philadelphia. 480-485.





