Osteonecrosis (ON) of the hip and knee can be a source of severe morbidity for affected individuals. Although several risk factors and explanations for the pathogenesis of ON have been recognized, there exists little consensus in the literature as to the appropriate clinical management. We present three patients treated at our institution and a treatment algorithm for hip and knee osteonecrosis.
Osteonecrosis, Spontaneous Osteonecrosis of the knee, Avascular necrosis, Algorithm
ON: Osteonecrosis; THA: Total Hip Arthroplasty; TKA: Total Knee Arthroplasty; AVN: Avascular Necrosis; CSI: Corticosteroid Injection
Osteonecrosis (ON) of the hip most often occurs in the third to fifth decade of life. It has a predictable progression from asymptomatic lesion visual only on advanced imaging to eventual bone collapse requiring surgical intervention. Risk factors commonly associated with ON of the hip include trauma, excessive alcohol use, prolonged corticosteroid use and any number of diseases that can lead to ischemia of the femoral head. Even with exposure to these risk factors, however, people infrequently develop ON and even fewer become symptomatic. In a study by Lieberman, et al. looking at a cohort of liver transplant patients with extensive corticosteroid exposures only 2-3% went on to develop ON [1,2]. Overall, hip ON is a multifactorial disease process with a poorly understood genetic contribution and dose response mechanism.
The primary measurement tools used in the discussion and treatment of hip ON are the Ficat staging system and the Kerboul angle for assessing the degree of femoral head involved in a lesion. The original Ficat system was based on clinical and radiographic signs as well as scintigram and core biopsy findings [3]. Table 1 shows a simplified explanation of the Ficat system.
Table 1: Ficat and arlet classifi steinberg classification for hip osteonecrosis. View Table 1
The Ficat classification was later modified by Steinberg to be based solely on clinical symptoms and radiographic changes [4]. These changes are described briefly in Table 2.
Table 2: Steinberg classification for hip osteonecrosis. View Table 2
The combined necrotic angle, originally described by Kerboul, is an estimate of the extent of involvement of the femoral head. This was originally described as the sum of the angles of the involvement on AP and lateral radiographs, and later on MRI [5-7]. A study by Ha, et al. showed that if the combined necrotic angle was < 190, the risk of progression to femoral collapse was significantly less than an angle of > 240 [8]. Intuitively, this makes sense as one would expect lesions with greater involvement of the femoral head to have a higher rate of collapse.
Both surgical and non-surgical options exist for hip osteonecrosis. Medical treatment as a monotherapy is generally only used in early ON with pre-collapse lesions in an attempt to slow or stop disease progression and mitigate the need for surgical intervention [9-11]. One study by Wang, et al. demonstrated extracorporeal shock wave treatments to be effective as compared to core decompression with autograft when using pain and Harris hip scores as outcome measures [12]. There is limited evidence that enoxaparin and alendronate have been shown to reduce disease progression. However, enoxaparin has not been shown to work in steroid induced ON, and the data on alendronate has not been reproducible in further studies [13-15]. One of the most important things to consider is that patients who develop femoral head ON generally have had a long history of insult to that region of bone, either from steroids, alcohol, or coagulopathy. In this setting, progression of disease is expected and attempt at bone preserving interventions have worse outcomes overall [11].
Options for surgical management of hip ON can largely be classified as either femoral head sparing or femoral head replacing. Femoral head sparing techniques include any number of methods for core decompression with or without the use of grafting material. Grafting substrates can then be further divided into synthetic, allogenic and autogenic. The gold standard in grafting material is to use a vascularized autograft, typically taken from the fibula, to fill in the defect left behind by the core decompression [16,17]. This technique has been associated with improved outcomes in some patient populations, but is a technically demanding surgery. The various treatment options with the 2-year survival rate, as defined as no further intervention over that time, is shown in Table 3 [18-20].
Table 3: Two year survival rate for surgical treatment options in hip ON. View Table 3
Rotational osteotomies also fall into the category of femoral head sparing treatment, but unlike decompression alone, are more technically demanding [20]. The goal is to offload the pre-collapse lesion through rotation of the femoral head, thus allowing continued weight bearing through an unaffected region [21,22]. Unfortunately, rotational osteotomies may create proximal femoral anatomical challenges for any subsequent arthroplasty procedure.
Total Hip Arthroplasty (THA) is the definitive treatment and the likely final pathway for most patients with femoral head osteonecrosis. Hemiarthroplasty is less often performed due the more predictable outcome and durability with THA as well as the often younger, higher demand patient who presents with this pathology. THA is also preferred over hip resurfacing due to the potential complication of femoral neck fracture or poor fixation in compromised proximal femoral bone stock. Previously, it was thought that patients with ON treated with THA had a greater inherent risk of dislocation. This risk of dislocation is more likely the result of greater demand placed on the Total Hip Arthroplasty (THA) by a younger patient population [23]. Improvement in THA materials and surgical techniques has led to improved outcomes. Recents studies have quoted 83-93% survivorship at > 15 years follow-up for patients with ON treated with THA [24-29].
All patients with radiographic and clinical evidence of osteonecrosis undergo a routine hypercoagulation screen, including blood test for Lupus anticoagulant, Cardiolipin IgG and IgM, Protein S activity, Protein C activity, Antithrombin III activity, and serum Homocysteine. This standard set of labs was developed through conjunction with our Hematology partners at the treating institution (Kaiser Permanente West LA Medical Center). These results help us determine appropriate Deep Vein Thrombosis (DVT) prophylaxis as well as seek appropriate medical consultation.
While the Ficat Staging system is the primary classification tool used in research settings, we generally determine treatment based on whether the lesion is pre-collapse or post-collapse. Our algorithm is shown in brief in Figure 1. Once a patient has progressed to post-collapse stage (we include patients with subchondral collapse (crescent sign) as post-collapse lesions), there are few if any treatments short of THA that can offer patients predictable outcomes. It is the patients who are pre-collapse and symptomatic in which we try our hardest to preserve the hip joint and delay arthroplasty. We have found that in young patients with a pre-collapse lesion, a small Kerboul angle (< 200), and a medially based lesion (closer to the fovea) have the best chance of achieving acceptable outcomes without arthroplasty. When the lateral pillar is maintained, as in medially-based focal lesions, the support of the femoral head remains adequate and there is a slower disease progression overall. In these select patients we offer core decompression in an attempt to preserve the native joint if possible. Our technique is to use a more proximal start site for core decompression, as Colwell, et al. showed that there is an increased risk of immediate postoperative fracture in cores that were taken distal to the vastus ridge [30]. We use a series of 3.2 mm Steinman pins percutaneously introduced into the femoral head to make 3 small diameter core decompression sites as originally described by Mont, et al. [31]. We augment Mont’s described procedure by over drilling the center most pin with a 4.5 mm drill and arthroscopic long-handle curette. Additionally, we have begun augmenting our core decompression with the use of concentrated iliac crest bone aspirate, which has recently been shown to significantly improve the clinical outcomes of this procedure [32]. Postoperatively, we instruct our patients to be toe touch weight-bearing for 6 weeks and 6 weeks of partial weight-bearing to allow for bone deposition and healing.
 Figure 1: Algorithm for osteonecrosis of the femoral head. View Figure 1
Figure 1: Algorithm for osteonecrosis of the femoral head. View Figure 1
Elderly patients (over age 50) who have symptomatic hip osteonecrosis, however, should be considered for THA regardless of the stage of their lesions. THA provides reliable pain relief in this population just as it does in the setting of osteonecrosis.
MG is a 31 yo F who presented with left hip pain for over a decade. MRI and radiographs had been obtained prior to presentation to our office which showed anterior quadrant cystic changes in the femoral head consistent with AVN in the pre-collapse state. On physical exam, the patient had excellent range of motion. The patient had already tried and failed conservative measures such as oral pain control, CSI, and protected weight bearing. She elected to undergo core decompression of the affected femoral head. At one year postoperatively she has limited improvement in her pain and continues to rehabilitate Figure 1, Figure 2, Figure 3, Figure 4 and Figure 5.
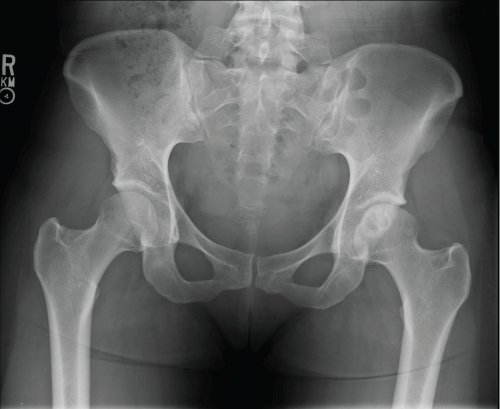 Figure 2: Preoperative AP pelvis.View Figure 2
Figure 2: Preoperative AP pelvis.View Figure 2
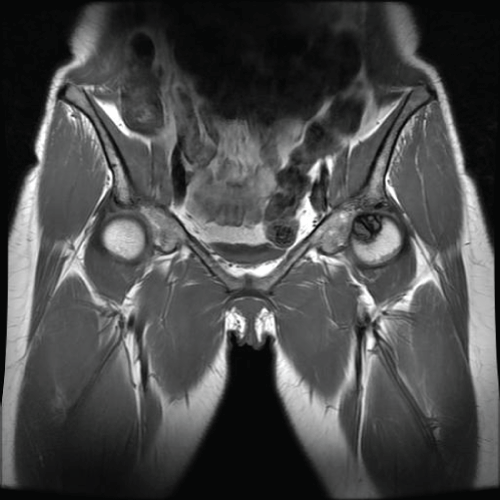 Figure 3: Preoperative coronal MRI. View Figure 3
Figure 3: Preoperative coronal MRI. View Figure 3
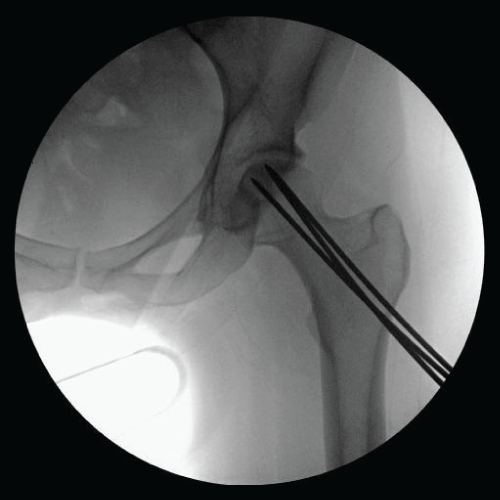 Figure 4: Intraoperative radiograph. View Figure 4
Figure 4: Intraoperative radiograph. View Figure 4
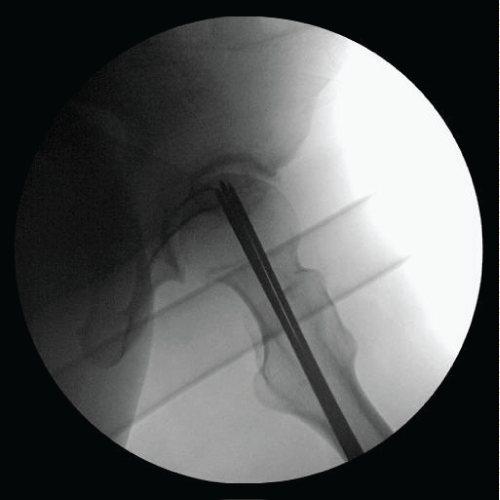 Figure 5: Intraoperative radiograph. View Figure 5
Figure 5: Intraoperative radiograph. View Figure 5
ID is an 18-year-old female, with Systemic Lupus Erythematosus (SLE) treated with long term steroids, collect and plaquenil and a history of right fibular osteosarcoma, who presented February 2015 with a one-year history of progressive activity-related bilateral hip pain. The patient described deep aching pain in the groin with radiation into the buttock and down the medial thigh on both hips. At presentation, she could no longer participate in recreational activity. She denied ever smoking and she does not use alcohol. Right hip range of motion was zero to ninety degrees of flexion, left hip range of motion was 0-100 degrees of flexion with impingement pain bilaterally. Initial Radiographs are seen in Figure 6.
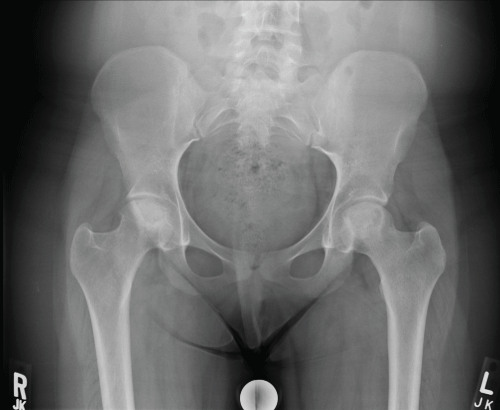 Figure 6: Preoperative AP pelvis. View Figure 6
Figure 6: Preoperative AP pelvis. View Figure 6
Given her history an MRI of the pelvis was done at that time showing bilateral femoral head osteonecrosis. Both femora had extensive involvement with collapse Figure 7 and Figure 8.
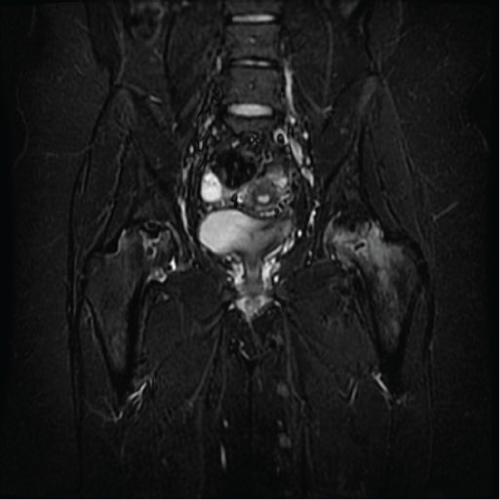 Figure 7: Preoperative coronal MRI. View Figure 7
Figure 7: Preoperative coronal MRI. View Figure 7
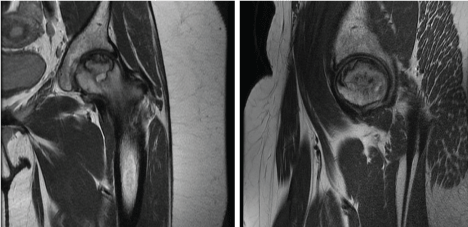 Figure 8: Preoperative coronal and sagittal MRI of left hip. View Figure 8
Figure 8: Preoperative coronal and sagittal MRI of left hip. View Figure 8
Six months following initial presentation she had stopped attending college due to hip pain and was unable to ambulate without assistive device (crutches). Repeat radiographs showed advancement to collapse on bilateral femoral heads (Figure 9). She was scheduled for staged bilateral total hip arthroplasty and she has done well postoperatively. Figure 10 is an intraoperative clinical photograph showing advanced femoral head collapse and postoperative radiograph showing bilateral THA after staged procedures (Figure 11).
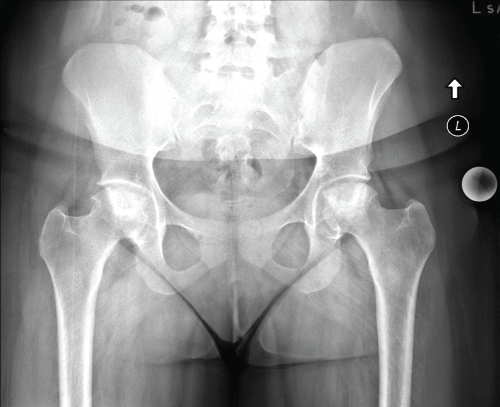 Figure 9: Repeat preoperative AP pelvis. View Figure 9
Figure 9: Repeat preoperative AP pelvis. View Figure 9
 Figure 10: Intraoperative clinical photograph of femoral head. View Figure 10
Figure 10: Intraoperative clinical photograph of femoral head. View Figure 10
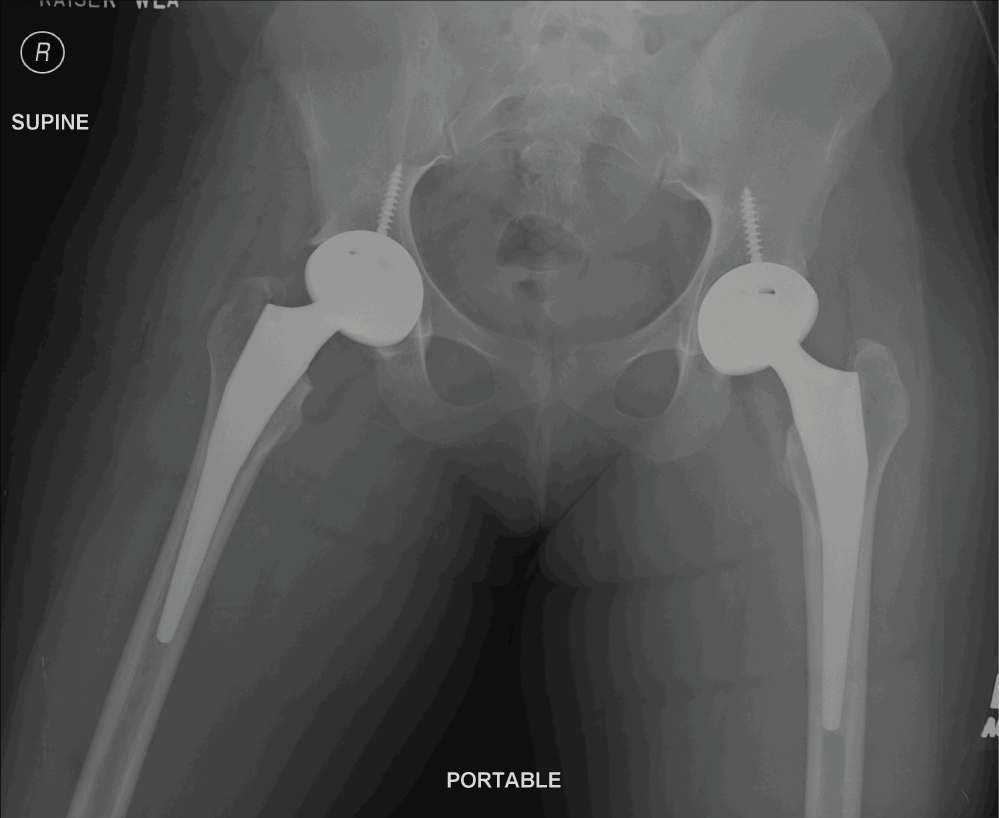 Figure 11: Postoperative AP pelvis. View Figure 11
Figure 11: Postoperative AP pelvis. View Figure 11
While we attempted a trial of conservative treatment in this patient one can see the natural course of large osteonecrotic lesions that involve the weight-bearing surface of the femoral head. These lesions have a high rate of progression to collapse and eventually require arthroplasty to alleviate their pain and improve function.
Osteonecrosis (ON) of the knee can be largely divided into two categories; secondary ON and Spontaneous Osteonecrosis of the Knee (SONK). Secondary ON can be thought of similar to our understanding of osteonecrosis of the hip with etiologies that impart ischemic insult, direct cellular damage, or altered differentiation of stem cells to the affected area resulting in increased intraosseous pressure [33]. We use the term spontaneous osteonecrosis of the knee when there exists no history to place the patient at an otherwise increased risk. Spontaneous osteonecrosis of the knee has also been described as a subchondral insufficiency fracture. While postarthroscopic osteonecrosis of the knee has been described as a third distinct category, some authors believe it is the trauma from the surgical procedure itself results in secondary osteonecrosis of the knee while others have hypothesized that it is lasting effects of the arthroscopic procedure resulting in a subchondral insufficiency fracture [34,35].
Risk factors for secondary osteonecrosis include trauma, chemotherapy, myeloproliferative disease, radiation, alcohol, coagulation abnormalities, corticosteroid use, and smoking [36]. Approximately 90% of cases of secondary osteonecrosis have either alcohol abuse or corticosteroid use as an associated risk factor, however, secondary osteonecrosis is likely due to multiple risk factors working in concert as only a small percentage of patients with these risk factors go on to develop clinically significant osteonecrosis [37].
Spontaneous Osteonecrosis of the Knee (SONK) most often affects the medial femoral condyle in elderly patients [38]. They often present with an episode of acute pain to the affected region of the knee. MRI analysis has found a 9.4% prevalence of SONK in persons aged > 65 years [39]. Reddy, et al. discuss a “watershed area” that exists in the blood supply to the medial femoral condyle which could predispose at risk individuals to osteonecrosis [40]. Another theory for SONK is that these areas may represent insufficiency fractures as they often occur in elderly women with osteopenic bone [41].
Radiographic studies should begin with a standard X-ray series of the involved joint. However, standard radiographs can dramatically underestimate the involvement of the affected joint. Therefore, if osteonecrosis is suspected and radiographs are normal there should be a low threshold to obtain an MRI. MRI will show early evidence of osteonecrosis with typical features such as serpentine lesions and bone marrow edema.
Mont, et al. describe an adapted Ficat staging system for Osteonecrosis of the Knee based on radiographs (Figure 12) [36].
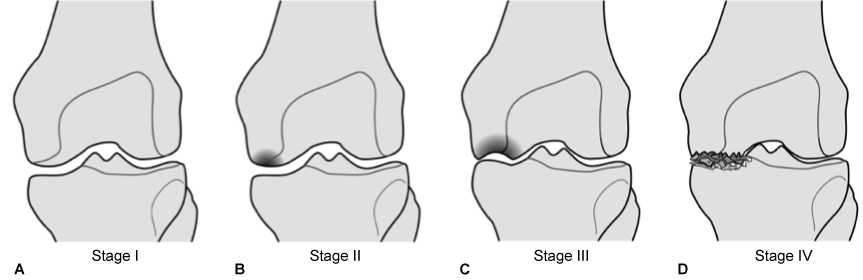 Figure 12: An adapted ficat staging system for osteonecrosis of the knee based on radiographs. View Figure 12
Figure 12: An adapted ficat staging system for osteonecrosis of the knee based on radiographs. View Figure 12
In stage I there is no radiographic evidence of osteonecrosis. In stage II there is evidence of sclerosis surrounding the involved lesion. Stage III shows the progression to subchondral collapse and Stage IV shows collapse of the involved condyle. While precise staging is important in research our clinical decision is largely based on patient symptoms, extent of the lesions, and whether or the not patient is pre-collapse or post-collapse.
Management of knee osteonecrosis broadly consists of conservative management versus operative intervention. Operative treatment consists of arthroplasty or joint preserving procedures. Medical therapy is largely derived from hip literature and lacks compelling evidence for its use in the setting of knee osteonecrosis. More recently and specific to the knee, six patients predisposed to clot formation with early stage osteonecrosis treated with enoxaparin had no collapse in short term follow-up [42]. In another study, iloprost (PGI2), a vasoactive prostaglandin analogue, proved to be an effective medical therapy for pre-collapse lesions in a study that included analysis of multiple joints with osteonecrosis (hip, knee, and ankle). The authors of this study strongly advocate for surgical intervention in post-collapse lesions [43]. While evidence for medical therapy in the setting of osteonecrosis of the knee is promising, more is needed for its application in clinical practice.
Nonoperative treatment has a high clinical failure rate [44]. It is generally agreed upon that the management of late stage osteonecrosis that has progressed to debilitating arthritis should be definitively treated with joint replacement. Non-arthroplasty procedures such as osteochondral allograft, autologous chondrocyte implantation, core decompression, and offloading procedures such as high-tibial osteotomy have all been proposed as reasonable treatment options but clinical evidence is lacking [38]. Of these options, small core decompression has shown the most promising results. Marulanda, et al. showed a 92% success rate and avoiding TKR in 97% of patients at 3 years for SONK [45]. However, to our knowledge no randomized trials are currently available for joint preserving procedures.
While prior studies had demonstrated less than optimal results with total knee arthroplasty relative to their non-osteonecrotic counterparts, more recent studies have shown success rates as high as 97% for total knee arthroplasty in the setting of osteonecrosis. Similarly, results of unicompartmental knee arthroplasty for SONK has improved, with excellent results being achieved in properly selected patients. The use of cement for fixation and femoral and tibial stems to bypass the osteonecrotic lesions is likely responsible for the improved results [46,47].
Once again, all patients presenting with osteonecrosis of the knee undergo a routine hypercoagulation screen (see Our Algorithm for Osteonecrosis of the Hip). Our first distinction in clinical decision making is the size and involvement of the lesion. For small lesions, such as those isolated to the medial femoral condyle often seen in SONK, we offer a trial period of protected weightbearing (approximately three months) with symptomatic pain control with NSAIDs and corticosteroid injections. After three months, if the patient fails to improve we consider small core decompression for patients less than 50 years of age and we offer either UKA or TKA to older patients. We offer UKA to patients with symptomatic unicompartmental osteonecrosis with minimal bone involvement (less than 8 mm depth of lesion and good rim bone for implant stability) without evidence of multicompartmental arthritis. The indications and contraindications for UKA are similar to those for osteoarthritis. Preoperative advanced imaging is required to ensure that all implants have adequate non-osteonecrotic bone stock to ensure fixation. Patients who have small focal lesions of osteonecrosis in the setting of diffuse osteoarthritis should bypass UKA and proceed to TKA.
For patients who present with diffuse osteonecrosis, we have found little efficacy in treatments short of TKA. In patients who present pre-collapse one can consider protected weightbearing and pain control. There is little role for core decompression in diffuse osteonecrosis. It is more likely that a patient seeking treatment for painful, diffuse osteonecrosis has already progressed to a collapsed stage and requires arthroplasty. We advocate the use of cement and stemmed prosthesis in order to achieve adequate fixation as well as transfer the forces away from the osteonecrotic bone and towards more healthy bone (Figure 13).
 Figure 13: Algorithm for osteonecrosis of the knee. View Figure 13
Figure 13: Algorithm for osteonecrosis of the knee. View Figure 13
SS is a 60-year-old Female, with no significant past medical history, who presented to our facility with a long-standing history of bilateral knee pain (R > L), however six months prior to presentation she had an acute episode of overnight bilateral knee pain which was so severe that she sought treatment in the emergency room. She denied trauma to either of her knees. She has history of corticosteroid injections into her knee and low back as well a short course of corticosteroid uses for her low back pain. Her physical exam, including her bilateral knee exam was unremarkable. She described the pain as primarily on the anterior aspect of both her knees. Initial radiographs were unremarkable (Figure 14). An MRI was ordered of her bilateral knees which revealed extensive osteonecrosis of bilateral distal femurs and proximal tibias (Figure 15). She received a diagnosis of spontaneous osteonecrosis of the knee and desired staged bilateral Total Knee Replacement (TKR) surgery. She underwent Right TKR initially, followed by Left TKR. Intraoperative photographs can be seen in Figure 16. Postoperatively her pain has markedly improved with unlimited ambulation. Her right knee ROM is 0-135 degrees and her left knee ROM is 0-125 (Figure 17).
One of the remarkable aspects of this case was the diffuse extent of our patient’s osteonecrotic lesion given her relatively benign appearing x-rays. Moreover, the collapse that can be seen of her right femoral trochlear region cannot be appreciated on either the plain radiographic films or the preoperative MRI. One can assume that the severe pain that led to ER eval could have been her lesion collapsing. As one can see we used a stemmed femoral prosthesis to bypass the osteonecrotic lesion on the right knee and stemmed femoral AND tibial prosthesis to bypass the larger osteonecrotic lesion on the left side.
 Figure 14: Preoperative radiographs of a 60 F with acute onset of bilateral knee pain. View Figure 14
Figure 14: Preoperative radiographs of a 60 F with acute onset of bilateral knee pain. View Figure 14
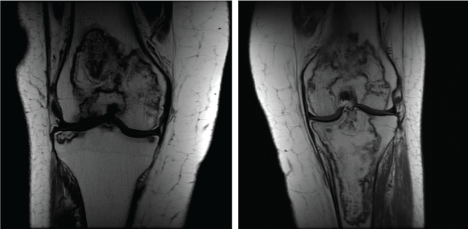 Figure 15: Right knee, left knee showing large areas of serpentine lesions in bilateral medial and lateral femoral condyles as well as the proximal tibia. View Figure 15
Figure 15: Right knee, left knee showing large areas of serpentine lesions in bilateral medial and lateral femoral condyles as well as the proximal tibia. View Figure 15
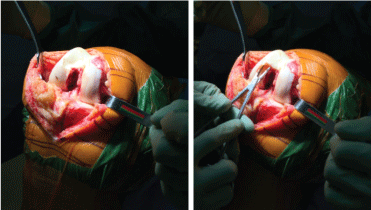 Figure 16: Intraoperative photographs of the right knee showing complete articular collapse of the femoral trochlea. View Figure 16
Figure 16: Intraoperative photographs of the right knee showing complete articular collapse of the femoral trochlea. View Figure 16
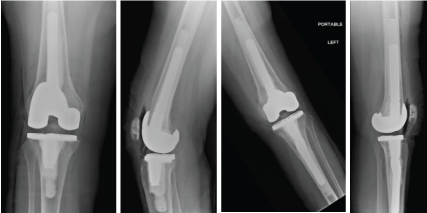 Figure 17: AP and lateral postoperative radiographs. Note that stemmed prosthesis we used in the R femur and Left Femur/Tibia in order to bypass all osteonecrotic lesions. Cement was also used for fixation in both knees. View Figure 17
Figure 17: AP and lateral postoperative radiographs. Note that stemmed prosthesis we used in the R femur and Left Femur/Tibia in order to bypass all osteonecrotic lesions. Cement was also used for fixation in both knees. View Figure 17
Osteonecrosis of the hip and knee present challenging cases for the orthopaedic surgeon. While many non-arthroplasty interventions have been described in the literature we have found little role for them in clinical practice. Core decompression may be used in small, pre-collapse areas of osteonecrosis especially if the involved bone has minimal involvement of the weight bearing surface. Arthroplasty has proven to be an excellent option for patients with osteonecrosis and debilitating pain and function. While special attention must be paid to these patients as they generally present younger than patients with degenerative arthritis and the native bone stock may be severely compromised, we have found that one can achieve excellent results with arthroplasty in the setting of osteonecrosis.