This is a case of a 55-year-old male patient that was incidentally found to have a large presacral tumor. After excision it was identified to be a smooth muscle tumor of uncertain malignant potential (STUMP). STUMPs are rare entities that have been identified most commonly in association with the genitourinary tract such as the uterus and prostate. Here we describe the first retroperitoneal STUMP with no association with the genitourinary tract and in the pre-sacral space. We discuss our surgical approach, post-operative management and surveillance.
Retroperitoneal sarcomas are rare and occur in a variety of types including smooth muscle tumors, liposarcoma, gastrointestinal stromal tumors, aggressive fibromatosis and desmoid tumors. Smooth muscle tumors are traditionally separated into leiomyomas and leiomyosarcomas. However, some retroperitoneal tumors fail to meet diagnostic criteria for either of these categories. These are termed smooth muscle tumors of uncertain malignant potential (STUMP) [1]. STUMP tumors are rare entities more common in the uterus than in the retroperitoneum. Here we present, to our knowledge the first case of a primary STUMP of the presacral space.
A 55-year-old male with a prior history significant for type 1 diabetes presented to the emergency department following a bicycle versus pedestrian collision. At initial presentation, he complained of left scapular and upper back pain. His vitals and physical examination were unremarkable. As part of his trauma evaluation, he underwent a computed tomography of the chest abdomen and pelvis that was negative for traumatic injury but uncovered a large 14 cm × 18 cm pre-sacral mass extending from L4 to S5 vertebra with associated lateral displacement of the sigmoid colon and bladder (Figure 1). A colonoscopy was performed showing no intraluminal involvement of the colon or rectum. Due to the concern for malignancy, the patient was advised to undergo surgical intervention. Since the uppermost border of the tumor was at the L4 lumbar vertebra, an abdominal approach was selected. At exploratory laparotomy a large cystic pre-sacral tumor located in the midline and extending to the left sidewall of the pelvis was found in close proximity with but not invading into the bladder, rectum, left ureter and left seminal vesicle. The mass was excised to grossly macroscopically normal margins (Figure 2).
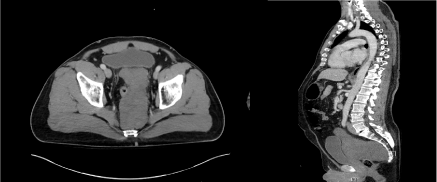 Figure 1: Axial and sagittal views of computed tomography of abdomen and pelvis with intravenous contrast demonstrating large presacral mass, displacing the rectum to the right and bladder anteriorly. View Figure 1
Figure 1: Axial and sagittal views of computed tomography of abdomen and pelvis with intravenous contrast demonstrating large presacral mass, displacing the rectum to the right and bladder anteriorly. View Figure 1
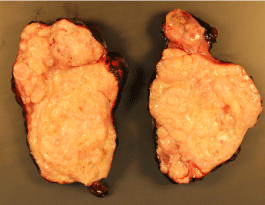 Figure 2: Gross specimen of resected pre-sacral mass. View Figure 2
Figure 2: Gross specimen of resected pre-sacral mass. View Figure 2
Post-operatively, the patient made an unremarkable recovery with discharge within four days of admission.
Final pathological evaluation was described as a large (20 cm × 8.5 cm × 5 cm) tumor which stained positive for caldesmon findings that supported smooth muscle phenotype. The tumor itself showed mild nuclear pleomorphism but low mitotic rate and low proliferative index, meaning it could not reliably be considered benign or malignant and therefore was termed smooth muscle tumor of uncertain malignant potential. The tumor had microscopically negative margins. He has remained free of recurrence during his period of follow-up with negative computed tomography scans performed every six months for the last two years.
Smooth muscle tumor of unknown potential (STUMPs) are a rare group of smooth muscle tumors that cannot be diagnosed unequivocally as benign or malignant. Put another way, STUMP is a category that likely does not reflect a true clinical entity; rather it is used when there is not enough information in the sample to exclude malignancy [2]. The diagnosis of this tumor type is made histologically using a set of criteria that include diffuse moderate-to-severe atypia, a mitotic count of at least 10 mitotic figures (MF)/10 high power fields (HPFs) and tumor cell necrosis [1]. STUMPs have an unpredictable natural history although it seems that they begin initially with a long disease-free interval and then have late recurrence of disease. STUMP tumors have predominantly been reported in cases involving the uterus, and limited reports of tumors in other sites [3,4]. As a result, the only criteria in present literature used to differentiate STUMP from leiomyosarcomas, the Bell criteria, exist in gynecological literature and do not apply to extrauterine tumors. Hence, as in our case, the diagnosis of STUMP has been made based on the histological findings of nuclear pleomorphism combined with low mitotic rate and proliferative index. In addition, the absence of tumor recurrence thus far and early metastases in our case would also serve to rule out leiomyosarcoma as a diagnosis.
While STUMPs are not necessarily malignant, neither are they absolutely benign and surgical management should balance respect for possible malignancy with minimization of patient morbidity.
As STUMP tumors are extremely rare, there are no standard protocols that have been approved as yet.
Preoperative tumor biopsy was not undertaken due to the cystic nature of the tumor on preoperative imaging, although previously has been considered an option in unresectable or aggressive looking tumors that may require preoperative chemoradiation to improve resectability. As we found in our case, there are no clear features of this tumor type that would macroscopically distinguish it from other differentials for retroperitoneal tumors. Therefore, with the potential diagnosis of retroperitoneal sarcoma in mind, it would be advisable at the time of surgery to strive for negative margins to limit recurrence. Using the literature on retroperitoneal sarcomas particularly those adjacent to hollow viscera, neurological or vascular structures, we can surmise that for now microscopically negative margins are probably acceptable [5,6].
The natural history of STUMPs is typically benign, although there are a few reports of accelerated local recurrence or distant metastasis [7]. Previous gynecological studies have found that these tumors tend to recur as either STUMPs or leiomyosarcomas [1]. In that event, repeat resection is recommended combined with adjuvant chemoradiation [1].
At present there are no universally accepted guidelines on the duration and frequency of post-resection surveillance. In keeping with guidelines for surveillance of retroperitoneal sarcomas, we have chosen a regime of six monthly computed tomography scan of the chest abdomen and pelvis with contrast every six months for three to five years and then yearly for life [5].
STUMP tumors are rare entities more common in the organs of the genitourinary tract that in the retroperitoneum. This is the first reported case of a presacral STUMP tumor under its current definition. Close clinical and radiographic follow up is advisable following resection in order to allow for early identification and treatment of local recurrence.