This study aimed to investigate the effectiveness of one 80-minute lecture regarding pain neurophysiology, on the understanding of undergraduate physiotherapy students, in terms of the same topic.
78 third-year students from the Tokyo University of Technology participated in this study. An 80-minute one-off lecture regarding pain neurophysiology was delivered. Understanding of pain neurophysiology was assessed through a Japanese version of Neurophysiology of Pain Questionnaire (NPQ), immediately before, after, and one month after the lecture. Furthermore, students' subjective interest levels, difficulty levels and comprehension levels were also evaluated using Visual Analogue Scale (VAS).
NPQ scores improved significantly immediately after and one month after the intervention compared to the baseline (p < 0.01). Effect sizes in both comparisons were large (0.99 and 1.11 respectively). There was no significant difference between immediately after and one month after the intervention. There was no significant correlation between changes in NPQ and the three subjective outcomes in VAS.
The findings of this study suggest that a single 80-minute lecture might be effective to improve undergraduate physiotherapy students' understanding about pain neurophysiology. Educational staff in Japanese physiotherapy schools is encouraged to integrate modern pain science into their lectures.
Chronic pain, Pain neurophysiology, Education
Musculoskeletal pain is one of the most burdensome health-related issues in the world [1-3]. In some developed countries, musculoskeletal pain is estimated to be even more costly than other major diseases, such as stroke, ischemic heart diseases, cancer and diabetes mellitus [4]. One reason why the financial burden of musculoskeletal pain is enormous is that there is no definitive treatment for chronic or persistent pain conditions [5]. In acute pain states, pain typically correlates with pathobiological changes in peripheral tissues, whilst recent studies demonstrated that central sensitisation in spinal cord and brain might have larger role in the production of pain in chronic pain states [6-9]. This evidence questions the validity of traditional biomedical model, in which symptoms are thought to be explained by pathobiological damage to local tissues [10]. Thus, the biopsychosocial model has been broadly acknowledged in the recent literature [11].
Advice and education have been often utilised for patients with pain in clinical settings [12-14]. Traditionally, these interventions were often based on biomedical model [12,15]. However, a novel type of education informed by modern pain neurophysiology has been proposed by Butler & Moseley [10,16]. In this type of patient education, various information regarding pain neurophysiology is explained through figures and metaphors, on the basis of biopsychosocial model. Butler & Moseley suggested that reconceptualising the meaning of pain (eg. pain does not represent the level of tissue damage) can reduce the threat value of pain and actual pain level [16]. In fact, this educational approach has been proven to be effective in decreasing pain and improving the physical function in patients with chronic pain conditions [17-19]. On the other hand, some studies implied that biomedical-driven excessive imaging, treatments and patient's education can potentially reinforce patients' maladaptive thinking and behaviours, leading to iatrogenic chronic pain states [20-24].
Considering the fact that major advances have been made in the field of pain neuroscience, physiotherapists have to update their traditional biomedical attitudes towards pain disorders [25]. However, these relatively new perspectives about pain are currently not commonly appreciated by physiotherapists [26]. Thus, it is important for educators in physiotherapy schools to reconsider the current education regarding pain science [27]. One study found that three-hour lectures might be effective in the short term to improve knowledge regarding pain neurophysiology of physiotherapy graduate school students in the United States [28]. To date, however, no similar study has been replicated in Japanese physiotherapy contexts. In fact, biomedical ideas are still dominant in physiotherapy schools in Japan, and pain science is not explicitly described as a formal part of the national physiotherapy curriculum in the Japanese law [29].
The purpose of this study was to examine the short-term effects of a single 80-minute lecture on Japanese undergraduate students' understanding about pain neurophysiology.
Participants were 78 third-year undergraduate students who belonged to Department of Physical Therapy, School of Health Sciences at the Tokyo University of Technology from September to October in 2016, and participated in a series of lectures in the subject of 'manual therapy'. They had never received any formal lecture specifically regarding pain science. A written consent to participation was achieved after sufficient explanation about the purpose and methods of the study, and an assurance of privacy and confidentiality. The study was a prospective case series with pre- and post-intervention measurements, corresponding to evidence level lV in the hierarchy of National Health and Medical Research Council [30].
In an 80-minute one-off lecture, some key information in patient education, such as mechanisms of nociceptive pain, peripheral neuropathic pain, central sensitisation and brain representation, a distinction between pain and nociception, and a difference between biomedical model and biopsychosocial model, were explained through 59 Power Point slides on two screens in front of the students. Lecture notes with 40 relatively important slides extracted from the 59 original slides were printed out and distributed to all students before the presentation. Lecture materials were developed in line with the guidebook of explaining pain [16]. One author (KM) prepared for the lecture material and conducted the lecture. Specific explanations about individual items in a questionnaire to assess students' understanding about pain neurophysiology were not given during the lecture [31]. Participants had no access to the presentation materials before the lecture.
A Japanese-language version of the Neurophysiology of Pain Questionnaire (NPQ) was developed by two authors and was used to evaluate students' understanding with regards to pain neurophysiology (refer to Table 1) [31]. NPQ was originally proposed as a self-administered questionnaire in 2003, and revised in 2013 (refer to Table 2) [31,32]. Although the original English version has not been validated, the Dutch version has been reported to have face validity [31,33]. Furthermore, one study reported good test-retest reliability of the original English version [31]. We obtained permission from original developers to translate this questionnaire to Japanese. Firstly, one author who had completed Masters degree in Australia and is a native Japanese-speaker performed forward translation from English to Japanese. Subsequently, another author who had achieved level 2 in Japanese-Language Proficiency Test and is a native English-speaker performed backward translation from Japanese to English. After these independent processes, these two authors discussed and produced a final Japanese version of NPQ based on consensus (Table 1). Both authors were physiotherapists and were sufficiently educated in pain biology. NPQ consisted of 12 items, each with three options (true, false and undecided). Every correct answer was worth one point, totalling a maximum score 12. A time limit for students to complete NPQ was set as three minutes. This time limit was set to ensure enough time for the lecture. Japanese NPQ assessment was performed three times in total (immediately before and after the lecture, and one month after the lecture).
Table 1: The Japanese version of NPQ. View Table 1
Table 2: The original English version of NPQ. View Table 2
A subjective questionnaire, using Visual Analogue Scale (VAS) was also administered to assess students' interest levels in the topic ("How interesting was the topic?"), the difficulty levels of NPQ ("How difficult was NPQ?") and comprehension levels regarding the lecture ("How much did you understand the lecture?") immediately after the lecture (refer to Figure 1).
 Figure 1: Subjective assessment of interest in the topic, difficulty of the lecture and comprehension regarding the lecture, using VAS. View Figure 1
Figure 1: Subjective assessment of interest in the topic, difficulty of the lecture and comprehension regarding the lecture, using VAS. View Figure 1
Values are presented as mean ± standard deviation. A statistical analysis was performed using analysis of variance, paired t-test and Bonferroni correction to determine statistically significant changes in NPQ scores. P value of less than 0.01 was used to determine statistical significance. Clinical significance of the effects was also assessed using within-group effect sizes (Cohen's d) and 95% Confidence Intervals (CI). Effect sizes were categorised as small (< 0.3), moderate (< 0.5) and large (> 0.8) based on Cohen's classification [34]. Pearson' correlation coefficient (r) was calculated to assess correlations between changes in NPQ and three subjective outcomes, including interest levels in the topic, difficulty levels of the lecture and comprehension levels regarding the lecture. Pearson's correlation coefficient was evaluated as very strong (0.8 <), moderately strong (0.6 to 0.8), fair (0.3 to 0.5) and poor (< 0.3) [35]. Statistical analysis was conducted using Microsoft Excel©2016.
Informed consents to participate in the study were obtained from 78 undergraduate physiotherapy students (29 women and 49 men). Mean age was 20.6 ± 0.7 years. All students participated in every measurement of all outcome measures and there was no drop. All participants finished NPQ in three minutes in both pre- and post-intervention assessments. The results of NPQ measurements are presented in Figure 2. The mean NPQ scores were 6.5 ± 1.7 before the lecture, 8.1 ± 1.5 after the lecture and 8.3 ± 1.4 one month after the lecture. There were significant improvements in NPQ scores immediately after and one month after the lecture, compared to the pre-intervention baseline (p < 0.01). There was no statistical difference between second and third measurements (refer to Figure 2). Within-group effect sizes were large at two comparisons (immediate effect; 0.99, 95% CI 0.74 to 1.24, one-month effect; 1.11, 95% CI 0.86 to 1.24).
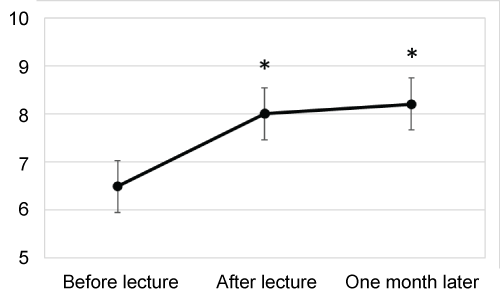 Figure 2: Changes in NPQ; *indicates significant change from before lecture with p-value less than 0.01. View Figure 2
Figure 2: Changes in NPQ; *indicates significant change from before lecture with p-value less than 0.01. View Figure 2
The results of subjective questionnaire using VAS are listed in Table 3. Mean interest score, difficulty score and comprehension score retrieved through the subjective assessment were 71.7 ± 17.0, 61.2 ± 16.9 and 60.4 ± 17.1 respectively. There was no statistically significant correlation in any combinations between those three subjective outcome measures and changes in NPQ score (refer to Table 3).
Table 3: Correlation between changes in NPQ and interest score, difficulty score and understanding score. View Table 3
This prospective case series aimed to examine the short-term effects of an 80-minute one-off lecture on undergraduate physiotherapy students' understanding with regards to pain neurophysiology. As a result, we found that their understanding improved significantly immediately after the lecture and its effect was maintained after one month. The effects sizes were large (> 0.8). These findings suggest that a single lecture can enhance undergraduate physiotherapy students' understanding about modern pain neurophysiology in the short term.
Our findings corresponded with the results of the study conducted for graduate physiotherapy students in the US [28]. One of the strength of this study is that our study showed that even 80-minute lecture can be effective (slightly shorter than the three-hour lectures delivered in the American study). Based on the positive findings of their study and our study, the current education regarding pain science for Japanese physiotherapy students should be reconsidered. As mentioned in the introduction section, some types of patient education based on biomedical models can affect patients' long-term prognosis negatively [20-24]. On the other hand, there is growing evidence suggesting the effectiveness of pain neurophysiology education based on biopsychosocial model for patients with chronic pain [17-19]. Thus, educational staff in physiotherapy schools should consider integrating pain neurophysiology education based on the current evidence into their lectures for physiotherapy students.
Although not a statistically significant correlation (p = 0.08), a poor correlation (r = 0.20) was identified between interest scores and changes in NPQ at the one-month follow-up compared to the baseline (refer to Table 3). This slight tendency might imply that the learning effects can be greater if lectures are interesting for students. During the 80-minute lecture, several students were seen napping for short periods of time. This disappointing phenomenon revealed the lack of engaging elements to stimulate students' intellectual curiosity in the lecture. The potential incompetence of the presenter and partial failure to capture students' attentions may have biased our findings.
Several limitations have to be acknowledged in our study. A first potential source of bias lies in the nature of case series. This research design is regarded as the lowest level of evidence to prove the effectiveness of therapeutic interventions due to the risk of bias [30]. Thus, the positive findings in this study must be interpreted with caution. Secondly, the long-term effects of the intervention were not clear from this study because a follow-up was only at one month after the lecture. Thirdly, it is still unknown whether educational interventions can change students' attitudes and behaviours in clinical settings. As a fourth point, this study recruited only third-year undergraduate students from the Tokyo University of Technology. It is not entirely clear whether the findings in this study can be generalised to other populations, such as different numbers of undergraduate students in other universities, clinicians and patients in painful conditions. Based on the evidence that suggests that individual patient education is more effective than group educational sessions [19,36,37], it can be speculated that the findings of this study might be applied to similar or less number of undergraduate physiotherapy students. Lastly, further study is required to ensure the reliability and the validity of the Japanese version of NPQ utilised in this study.
The results of this study imply that a single 80-minute lecture might be effective in improving students' understanding regarding pain neurophysiology. Based on the findings in this study, educational staff in Japanese physiotherapy schools is encouraged to integrate modern pain science into their lectures.
We would like to thank Professor Lorimer Moseley and Dr. Mark Catley for providing helpful advice and suggestions.
We conducted this research following an approval from an ethical committee at the Tokyo University of Technology (approval number E16HS-015).