The World Health Organization identifies health as "a state of complete physical, mental, and social wellbeing", and views spirituality (a function of the soul) as an important factor in the quality of life and wellness of individuals regardless of their religious affiliations [1].
Family medicine should validate comprehensive, holistic patient care, including spiritual health [2,3]. Muslim people believe in God or a universal spirit and frequently consider religion important [4]. Furthermost, people in crisis believe that spiritual power is important in physical and mental health [5], Habitually, Muslim people use faith and prayer for healing or to cope with illness [6,7].
Religion in Arab countries is very important for this population's belief, values, faith in destiny, and to improve coping and healing [2,6,7]. While different spiritual wellness in different communities may have altered meditation, prayer, affirmations, or specific spiritual practices that support people connected to a higher power or belief system.
Physicians require training in spiritual medicine to help patients with chronic pain [8,9], palliative care [10], dying [11], hospitalized patients, acute crises, worsening illness or persistent health disease, incurable disease, mental illness, grief, domestic violence, and broken relationships [12].
The use of spiritual practice in primary or secondary care will increase professional satisfaction and prevent burnout [13].
There are many negative correlations between improper patient's spirituality and health in many domains; physical, mental, physiological and behavioral health statuses. In the physical domain, it will aggravate hypertension, cardiac arrhythmias, chronic body ache, premenstrual syndrome, migraine and cluster headaches. While in the mental domain it will exacerbate anxiety, insomnia, depression and low self-esteem Although in the physiologic effects, it will worsen metabolism, rate of breathing, blood pressure, muscle tension, heart rate and increased brain waves. Whereas in the behavioral domain, it will increase drug abuse, alcohol consumption, smoking addiction, and increase destructive behavior [14-16].
There are many barriers for physicians to practice spiritual medicine including; lack of physician time, experience, and suspicion of the role of physician in spiritual medicine respectively (71%, 59%, 31%) [17].
Spirituality is a multifaceted, multidimensional human experience that includes religious and nonreligious. Spirituality has three components; cognitive, experiential and behavioral dimensions (Figure 1). The cognitive is the mental framework, which consists of meaning, purpose, truth beliefs and values [18-29].
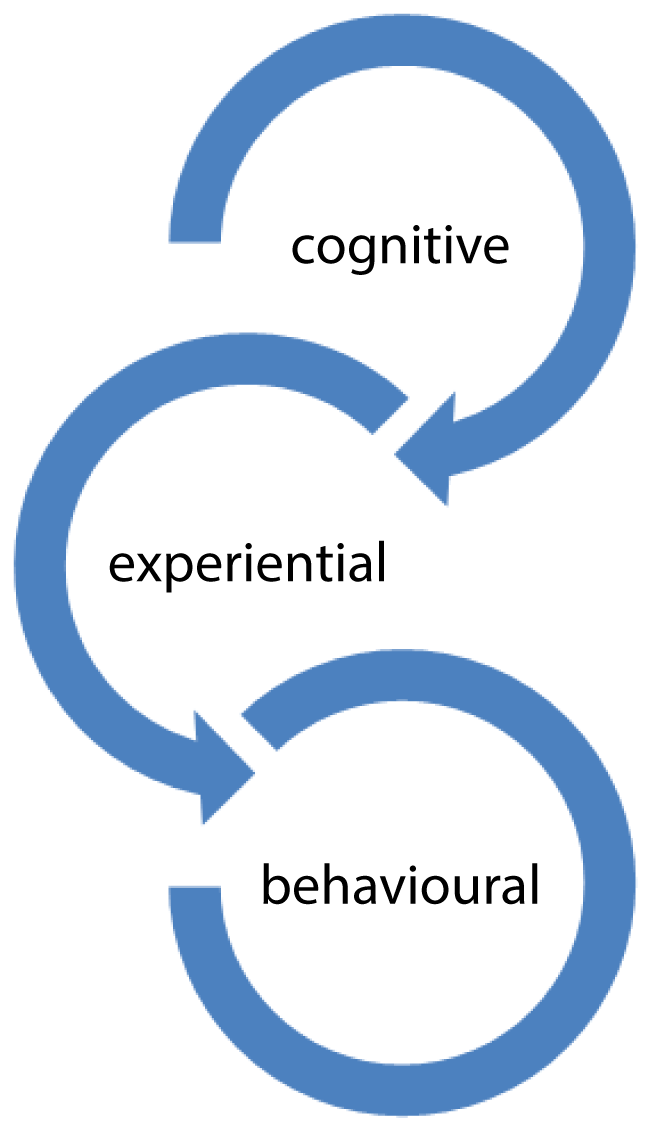 Figure 1: Multidimensional of spiritual perspectives. View Figure 1
Figure 1: Multidimensional of spiritual perspectives. View Figure 1
Experiential is the quality of an individual's inner resources which consists of hope, love, connection, inner peace, comfort, support, the ability to give and receive spiritual love, and the types of relationships [26-29].
Behavior perspectives are the way a person externally manifests individual spiritual beliefs and their inner spiritual state [16,30-32].
Many people find spirituality either through religion or through connection to scientific truth, arts, prayer, meditation, yoga, t'ai chi, walks in the country or listening to soothing music [16]. While different types of religious try to help answer mankind's spiritual questions, each has developed a specific set of beliefs, teachings and practices [16,32].
The patient may develop spiritual distress when individual's resources are not enough to cope with crisis demand (weak meaning, hope, love, peace, comfort, strength and connection in life). This has a detrimental effect on physical and mental health [26-29].
The physician should assess his/her personal belief, values, faith in destiny and comfort in practicing spiritual medicine. There are many history tools to assess patient's spirituality and its impending effect on the patient's health; FICA mnemonics (Table 1) [32], HOPE mnemonics (Table 2) [32], and open Invite spiritual history tools (Table 3) [32].
Table 1: FICA spiritual history tool [32]. View Table 1
Table 2: HOPE spiritual history tool [32]. View Table 2
The physician should listen attentively to patient spiritual need with empathy and provide the patient with compassionate support. The physician then will identify patient's spiritual needs and dimension of their lives. The physician should document helpful spiritual viewpoints that may be used in future crisis [31].
Table 3: The open invite spiritual history tool [32]. View Table 3
Physicians should understand different traditions and practices may affect faith in healing. Patients of Muslim population have religious practices that may influence on acute or chronic health status. Most Muslim populations fast during Ramadan from sun rise to sun set. This impacts glucose control and other biological factors. Most Muslim population eats Halal meat slaughtered in an Islamic way. Strict dietary codes need research to determine effects on health. Physicians need to know that Muslim people don't drink alcohol or may need to alter the traditional nutritional advice or receive alcohol counseling. Furthermore, Muslims believe practicing prayer which enhances spiritual health. Physicians should allow patients to identify spiritual beliefs, practices, and resources by asking: [16,32]
1. "Do you have spiritual practices? (e.g. praying, meditating, listening to music, or reading sacred text)?''.
2. "Are you part of a faith community? (e.g. home visitation program, a food pantry, or health screening program)?".
3. Physicians can reinforce positive coping behaviors and, with the patient's permission, offer to contact the patient's spiritual community to mobilize community faith resources as appropriate.
4. Physician and patient faith traditions coincide by offering faith-specific support.
Physicians that use and integrate spiritual medicine will enhance patient's trust, rapport and improve patient-doctor relationships. It will increase patient's compliance, and motivate patients to change destructive behaviors. Patients will recognize their spiritual needs and search for effective resources for healing and coping with a difficult crisis. Mostly the physician with limited medical solutions for incurable disease greatly enhances patient wellbeing and increase physician's professional pleasure and satisfaction [13,32]. There are many research which verifies the beneficial effect of multidisciplinary spiritual, compassionate care for patients. Also, support towards patient spiritual evidence based care, and it helps patients and families during malignancy stages. While many researchers proceeds patient's views of spiritual health experience [33-36].
The physician should always think about their role as a healer rather than curer. The magical skills from the spiritual arts will comfort patients by focusing on patient-centered; cooperative-partner; and the healing relationship. As physicians, we need to integrate spirituality into medical practice by "doing no harm" and preserve the patient's autonomy, freedom of thought and belief.
None.
None.
None.