Journal of Hypertension and Management
Hypertension and Anesthesia: What's New?
Pascal Colson* and Philippe Gaudard
Department of Anesthesiology and Critical Care Medicine, Heart and Lung Center, Arnaud de Villeneuve University Hospital and Montpellier School of Medicine, France
*Corresponding author:
Pascal Colson, Département d'Anesthésie Réanimation Arnaud de Villeneuve, CHRU Montpellier, 371 avenue Doyen Giraud, F-34295 Montpellier, France, E-mail: p-colson@chu-montpellier.fr
J Hypertens Manag, JHM-2-013, (Volume 2, Issue 1), Review Article; ISSN: 2474-3690
Received: April 13, 2016 | Accepted: May 13, 2016 | Published: May 16, 2016
Citation: Colson P, Gaudard P (2016) Hypertension and Anesthesia: What's New? J Hypertens Manag 2:013. 10.23937/2474-3690/1510013
Copyright: © 2016 Colson P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Hypertension is a very common disease, the first etiology of chronic cardiovascular disease in adult patients who undergo surgery. Improvement in HTA management is undeniable, but some concerns remain for the perioperative period. This article makes a short review of the state of the art regarding the anesthesia management of hypertensive patient during the perioperative period, with a special focus on anesthesia-hypertension interference.
Keywords
Hypertension, Anesthesia, Antihypertensive drugs, Cardiovascular risk
Introduction
Essential hypertension is a very common pathology, the most frequent chronic pathology of adult patients who undergo surgery, up to 13% in a recent study of a 2 million people cohort [1]. However, hypertension has disappeared from clinical risk factors in the table of contents of the 2014 ACC/AHA Perioperative Guideline [2]. This does not mean that hypertension is no longer a concern for the perioperative period, specifically for the anesthetist.
Hypertension: Pathophysiology
Pathophysiology of essential hypertension is complex, and not definitely understood in its genesis [3]. Obviously, the mechanisms involve the vascular structure and function, including an endothelial dysfunction [3]. However, essential hypertension is related to an increased vascular resistance and more than that, is characterized by an increased vasoreactivity [3] (Figure 1A). This vasoreactivity has many consequences on blood pressure regulation and blood flow to organs, which should be taken into account by the anesthetist.
.
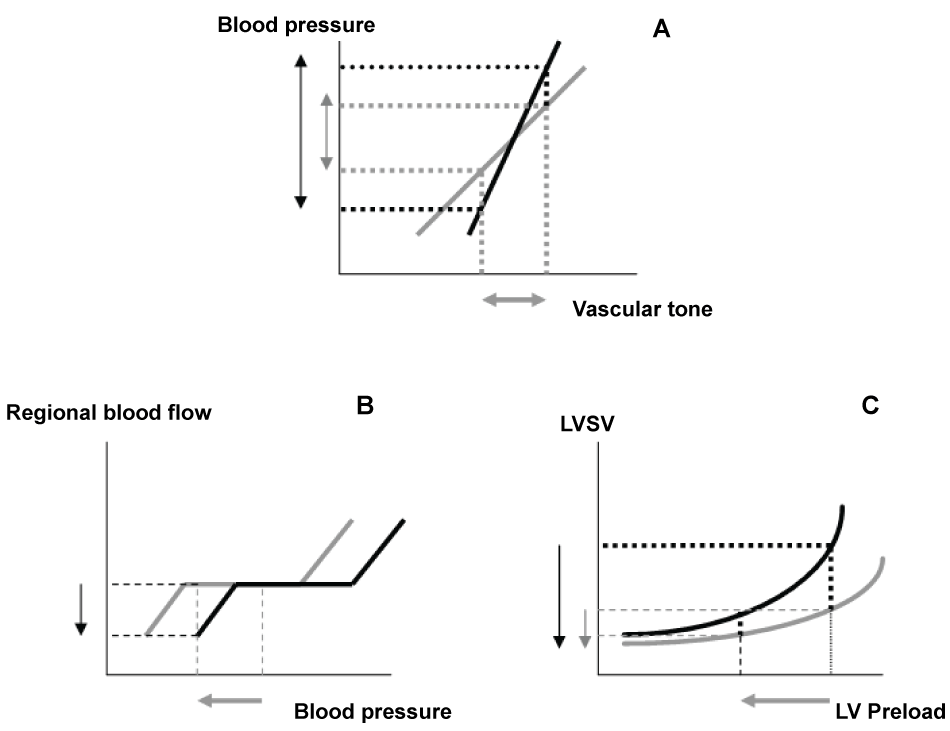
Figure 1: Pathophysiology of hypertensive patients.
Panel A: Vasoreactivity is increased in hypertensive patients (in black) when compared to normotensive patients (in grey). Small vascular tone variation induces drastic change in blood pressure in hypertensive paptient, so that blood pressure may either increase or decrease abruptly.
Panel B: Baroreflex resetting in hypertensive patient results in shifting blood flow regulation to major organs (brain, heart) to higher blood pressure levels. Therefore, a decrease in blood pressure may result in a decrease in organ blood flow in hypertensive patient, when it is maintained in normotensive patient for the same level of blood pressure.
Panel C: Left ventricle (LV) hypertrophy is an adaptation to chronic high blood pressure and LV afterload. Conversely, LV hypertrophy induces a decrease in LV relaxation and exposes the LV to steep reduction in preload even for small reduction in volemia or venous return. A fall in LV stroke volume (LVSV) may then occur with a fall in blood pressure.
View Figure 1
First the propensity to increase vascular resistance, either by chronic or repeated stimulation of arterial vasoconstriction, induces a resetting of the baroreflex to higher blood pressure levels. This resetting results in adapting blood flow regulation to organs to higher blood pressure levels [3] (Figure 1B). Therefore, hypertensive patients are able to maintain blood flow to organs when arterial blood pressure increases, thus they tolerate hypertensive crisis quite well, while they are less protected to drop in blood pressure. Indeed, the hypotension threshold that is associated with a decrease in blood flow to organs, is at a higher blood pressure level in hypertensive patients than in normotensive patients. For hypertensive patient, occurrence of hypotension, even though blood pressure does not drop to a dramatic level, is a dangerous event for brain, heart or kidney perfusions.
The second important consequence is the left ventricle (LV) hypertrophy that compensates for the wall stress imposed by high blood pressures or high LV afterload. This adaptative hypertrophy makes the LV very sensitive to a decrease in venous return and preload. Even a small reduction in venous return may induce a decrease in left ventricle stroke volume, and cardiac output [4] (Figure 1C).
Obviously, the worst clinical condition that the hypertensive patient may experience is hypotension and tachycardia. Both may add myocardial ischemia to unstable hemodynamics. LV hypertrophy, tachycardia and hypotension are a dreadful triad that is likely to induce at least endocardium ischemia, even without coronary disease.
Paradoxically, hypertensive crisis may not be considered as a such dramatic event. Hypertensive crisis may occur in many perioperative circumstances. The arterial vasoreactivity of the hypertensive patient results in increased blood pressure whenever sympathetic stimulation is triggered. Anxiety before surgery, preoperative and postoperative stress, either due to pain, hypoxia or chills are very common perioperative triggers. However, patients have adapted their cardiovascular regulation, and can face a moderate increase in blood pressure during the perioperative period without serious concern, except after vascular or cardiac surgery where tension on vascular sutures are liable to induce bleeding. Of course, sustained hypertensive crisis may cause pulmonary edema, but this complication is quite rare nowadays because anesthetist can use many handy treatments to contain blood pressure.
Yet, uncontrolled hypertension before surgery has justified postponing surgery, if > 180/110 mmHg [5]. Actually, the numbers of blood pressure do not matter that much [6]. Indeed, the real danger for the uncontrolled hypertensive patient is when high hypertension grades are concerned [7], which are associated with extreme hemodynamic instability during the perioperative period. These patients are more threatened by iterative uncontrolled drop in blood pressure or declines in organ blood flow during anesthesia and surgery than hypertensive treated patients.
Interestingly, hypertension is no longer considered as major risk factor in various scores used to predict cardiovascular complication or death [2]. In a large recent study on perioperative mortality, hypertension is the most frequent preoperative characteristic but does not appear in the multivariate model validated to predict mortality [1]. However, it would be naïve to consider hypertension as a problem solved for the perioperative period. Epidemiological studies have shown that many treated hypertensive patients (30 to 60%) are not well controlled by their treatment [8]. This should be reminded to anesthesiologist, any hypertensive-treated patient should be considered at risk of hemodynamic instability during anesthesia and surgery. Hypertension, not well controlled, is an indirect risk factor, able to amplify the exposition to other risk factors like coronaropathy [5]. Moreover, masked episodes of ischemia (kidney, heart, and brain), may not affect short term outcome, but may jeopardize cell capital insidiously.
Anesthesia: Consequences on Hemodynamics in Hypertensive Patient
Cardiovascular system regulation depends on three systems: the sympathetic nervous system, the renin-angiotensin system (RAS), and vasopressin, and general anesthesia interferes with both the sympathetic nervous system and the RAS [9] (Figure 2). Similarly, epidural anesthesia, beyond sympathetic blockade, suppresses renin release in response to arterial hypotension [10]. The anesthesia-induced reduction in sympathetic tone on the vascular capacitance results in a decreased effective intravascular volume, and angiotensin II may counterbalance this effect [11]. Accordingly, blood pressure may decrease markedly during general anesthesia when angiotensin II action is impeded by an angiotensin II competitive inhibitor [12]. Yet, besides RAS and the sympathetic system, endogenous vasopressin may be involved in blood pressure regulation during anesthesia through binding to receptors involved in vasoconstriction (V1a receptors) [13]. During epidural anesthesia and enalaprilat-induced inhibition of the RAS, the plasma vasopressin concentration increases significantly [14]. Vasopressin may compensate both systems blockade through a mesenteric vasoconstriction with blood flow redistribution away from the mesenteric circulation towards shorter-time-constant circulatory territories, therefore increasing venous return indirectly [13].
.
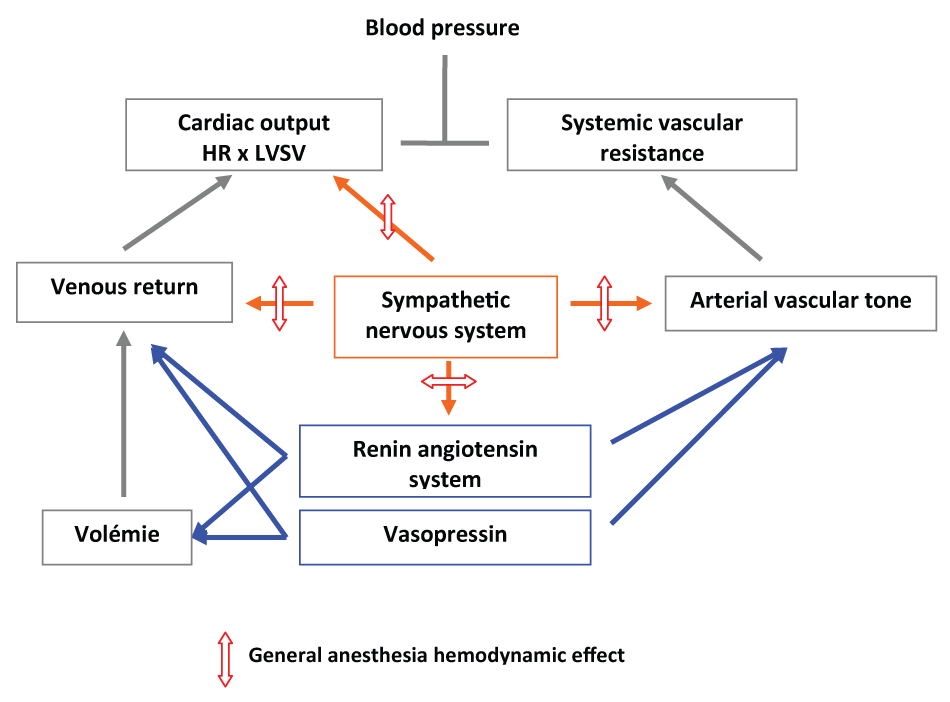
Figure 2: Consequences of anesthesia on blood pressure regulation.
Blood pressure is a compromise between cardiac output and systemic vascular tone. Blood pressure regulation depends therefore on heart rate (HR), left ventricle stroke volume (LVSV) and vascular resistance. The sympathetic nervous system is the main regulatory system, which is blunted by anesthesia (general, or medullary). Fortunately, the backup systems, renin angotensin system and vasopressin, can compensate the sympathetic nervous system impairment.
View Figure 2
Each individual pressor system may therefore act as a compensatory mechanism whenever other systems are depressed. The RAS contribution to blood pressure support is crucial when the sympathetic nervous system is blocked by epidural or general anesthesia and when endogenous vasopressin is antagonized by a specific V1 receptor antagonist [14,15]. The greatest and most significant decrease in blood pressure during anesthesia occurs with the combination of RAS blockade and a V1 receptor antagonist [14,15].
Anesthesia: Interaction between Anesthetics and Antihypertensive Drugs
Differences among anesthetics or anesthetic management are mainly related to the effects on the sympathetic nervous system, the worst tolerated occurring with fast and/or extended sympathetic blockade. However, propofol has specific impact on vascular reactivity. Several experimental studies have shown that propofol drastically reduced vascular response to norepinephrin, angiotensin II and vasopressin. Interestingly, these effects are amplified in hypertensive subjects [16-18]. These specific effects may explain the description of the catecholamine-resistant hypotension, the so-called refractory hypotension, observed almost exclusively after anesthesia induction with propofol [19-21].
Regarding the antihypertensive treatment, after 2 decades of concern with RAS antagonist and anesthesia interference [19,22], there is less evidence that the treatment can cause adverse effects that may justify treatment withdrawing before surgery [7,22]. Indeed, refractory hypotension was thought to be related to the preoperative treatment with renin-angiotensin system antagonist but it can be related actually to the confounding effect of propofol on vessels. Therefore, chronic treatment should be given till the day of surgery when a rebond effect can occur (beta-blockers, or clonidine, though less in use) but it can be stopped the day before surgery for most treatments [5]. In this respect, except for beta-blockers and clonidine, 2013 ESH Guidelines are indeed less restrictive and quite evasive, owing to the fact that level of evidence is low (Class IIb, Level C) [5].
Anesthesia: Management of Hypertensive Patients
Before surgery, the anesthetist should know the hypertension stage of the patient. The severity of hypertension correlates directly with the magnitude of potential anesthesia changes [23,24]. Similarly, patients who are treated with several anti-hypertensive drugs should also be considered at higher risk of hemodynamic instability [25].
Besides preoperative investigation that may help to identify hypertension end-organ damages, and to classify patients according to the hypertension grade, we believe that transthoracic echocardiography may be helpful to assess LV hypertrophy, a diagnosis that may alert the anesthetic of a potential risk of LV unpriming [5].
Anesthesia induction should be induced by titration in case of severe hypertension grade or preoperative uncontrolled blood pressure. Propofol which is known to interfere with vasoreactivity may increase the risk of hypotension, but it can be minimized by slow induction. Blood pressure monitoring is mandatory, but most of the time, intermittent measurement through an automated-cuff is enough. Continuous measurement through an arterial line should be considered in case of emergency surgery in a patient with high-grade uncontrolled hypertension, if not justified by the surgery itself. Nevertheless, the real danger is lowering too much blood pressure, and then exposing organs to ischemia. It would be more adapted to measure perfusion/ischemia of various organs, but this remains difficult in clinical practice beyond myocardial ischemia with automated analysis of ST segment. Cerebral near-infrared spectroscopy, which can monitor the oxygen content of cerebral tissue, is an attractive noninvasive monitoring of cerebral microcirculation [26]. However, so far, clinical studies have failed to show that interventions to correct cerebral desaturation improve neurological outcomes in high risk surgery like cardiac surgery [27].
However, episodes of hypotension are brief and easily treated in most cases [25,28] by the administration of fluid IV and short term vasopressors. Sympathetic agonists such as phenylephrine and ephedrine are effective in most cases [25,28]. Vasopressin agonist, like terlipressin, has been used as alternative to catecholamine. Terlipressin seems easy to use, as a single shoot injection, but it is a pro-drug converted into lysine vasopressin for many hours, a kinetic not adapted to treat short episode of hypotension. Terlipressin is as effective as norepinephrin to restore blood pressure but at the expense of an increase in blood lactate levels that reflects anaerobic condition in the bowels [29].
Similarly, IV treatments are available to control blood pressure rises. Most of the time, the challenge is not to treat an hypertensive emergency but rather to avoid a high blood pressure, which may facilitate bleeding in the surgical field. During surgery, anesthesia induces a sympathetic blockade, and general anesthetics like sevoflurane, are quite effective to reduce blood pressure increase. From time to times, it is necessary to add an antihypertensive treatment, but not so frequently. The immediate postoperative period may be a critical time, where sympathetic drive increases during arousal from anesthesia. Besides pain control, shivering prevention, it may be useful to use IV treatment to titrate blood pressure control. Among several drugs, 3 are very easy to use through titration: nicardipine, urapidil and esmolol. The 2 first are vasodilators that counteract rather specifically the increase in vascular resistance associated with hypertension. Old vasodilators like nitroprusside or nitroglycerin, which have undesirable effects on preload or heart rate, can be put on the shelf. Nicardipine, a dihydropyridine derivative calcium channel blocker with high vascular selectivity, is more an "anti-vasoconstrictor" than a vasodilator, provided it is used with low bolus doses (0.5 mg) [30]. A more recent short acting dihydropyridine, clivedipine, has similar pharmacological activity, but with shorter pharmacocinetics [31]. Urapidil combines selective post synaptic α1- adrenergic antagonist activity with central antagonism of serotonin receptors, which gives it a potent vasodilator effect. However, urapidil combines reduction of both pre- and afterload, a distinctive characteristic from the dihydropyridine derivatives [31]. Esmolol, is a β-blocking agent, which decreases blood pressure by a reduction in cardiac output (through a reduction in both contractility and heart rate). Its pharmacokinetic advantages, like being rapidly metabolized by plasma esterases, therefore easily titrated and discontinued if poorly tolerated, do not justify its use as first line treatment for blood pressure rise without tachycardia.
The chronic hypertensive treatment should be resumed as soon as possible. It is particularly true when it is part of the multidrug regimen given to prevent cardiovascular risk [5,32]. The perioperative period, which is associated with hemodynamic instability, inflammation and thrombosis risk, increases the risk of cardiovascular events in patients already exposed to this risk by a chronic pathology. It has been recommended for years that Beta-blockers should be continued during the perioperative period [2] and this applies more recently for statins too [33]. Interestingly, ACE inhibitor shares some pharmacological properties with statin, the pleiotrophic effects, that may be useful during the perioperative period. Resuming as soon as possible chronic treatment with angiotensin receptor antagonist reduced postoperative mortality in a large cohort of patients [34]. Actually, there are fewer reasons to justify withdrawing the treatment before surgery than reasons to resume the renin-angiotensin system antagonist treatment as soon as possible after surgery.
Conclusion
Hypertensive patients remain a concern for the anesthetist. First because it is the first etiology of chronic cardiovascular disease in adult patients who undergo surgery. Second, in spite of improvement in HTA management, many of these patients have not fully controlled hypertension when they present at the surgery. However, a good understanding of the pathophysiology, less concerns about the possible risk of interference between anesthesia and chronic treatment, the security of anesthesia drugs or antihypertensive IV treatments make the anesthetist well prepared to treat acute hemodynamic compromise in hypertensive patient during the perioperative period.
References
-
Le Manach Y, Collins G, Rodseth R, Le Bihan-Benjamin C, Biccard B, et al. (2016) Preoperative Score to Predict Postoperative Mortality (POSPOM): Derivation and Validation. Anesthesiology 124: 570-579.
-
Fleisher LA, Fleischmann KE, Auerbach AD, Barnason SA, Beckman JA, et al. (2014) 2014 ACC/AHA Guideline on Perioperative Cardiovascular Evaluation and Management of Patients Undergoing Noncardiac Surgery. Circulation 130: e278-e333.
-
Oparil S, Zaman MA, Calhoun DA (2003) Pathogenesis of hypertension. Ann Intern Med 139: 761-776.
-
Colson P, Ryckwaert F, Coriat P (1999) Renin angiotensin system antagonists and anesthesia. Anesth Analg 89: 1143-1155.
-
(2013) 2013 ESH/ESC Guidelines for the management of arterial hypertension. The Task Force for the management ofarterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC), J Hypert 31: 1281-1357.
-
Casadei B, Abuzeid H (2005) Is there a strong rationale for deferring elective surgery in patients with poorly controlled hypertension? J Hypertens 23: 19-22.
-
(2014) 2014 ESC/ESA Guidelines on non-cardiac surgery: cardiovascular assessment and management. The Joint Task Force on non-cardiac surgery: cardiovascular assessment and management of the European Society of Cardiology (ESC) and the European Society of Anaesthesiology (ESA), European Heart Journal 35: 2383-2431.
-
Calhoun DA, Jones D, Textor S, Goff DC, Murphy TP, et al. (2008) Resistant Hypertension: Diagnosis, Evaluation, and Treatment. Circulation 117: e510-e526.
-
Matsukawa K, Ninomiya I, Nishiura N (1993) Effects of anesthesia on cardiac and renal sympathetic nerve activities and plasma catecholamines. Am J Physiol 265: R792-797.
-
Hopf HB, Schlaghecke R, Peters J (1994) Sympathetic neural blockade by epidural anesthesia suppresses renin release in response to arterial hypotension. Anesthesiology 80: 992-999.
-
Ecoffey C, Edouard A, Pruszczynski W, Taly E, Samii K (1985) Effects of epidural anesthesia on catecholamines, renin activity, and vasopressin changes induced by tilt in elderly men. Anesthesiology 62: 294-297.
-
Pettinger WA (1978) Anesthetics and the renin--angiotensin--aldosterone axis. Anesthesiology 48: 393-396.
-
Treschan TA, Peters J (2006) The vasopressin system: physiology and clinical strategies. Anesthesiology 105: 599-612.
-
Carp H, Vadhera R, Jayaram A, Garvey D (1994) Endogenous vasopressin and renin-angiotensin systems support blood pressure after epidural block in humans. Anesthesiology 80: 1000-1007.
-
Ullman JE, Hjelmqvist H, Rundgren M, Leksell LG (1992) Hemodynamic effects of vasopressin antagonism and angiotensin I converting enzyme inhibition during halothane anesthesia in sheep. Acta Anaesthesiol Scand 36: 132-137.
-
Boillot A, Laurant P, Berthelot A, Barale F (1999) Effects of propofol on vascular reactivity in isolated aortae from normotensive and spontaneously hypertensive rats. Br J Anaesth 83: 622-629.
-
Samain E, Bouillier H, Marty J, Safar M, Dagher G (2000) The effect of propofol on angiotensin II-induced Ca(2+) mobilization in aortic smooth muscle cells from normotensive and hypertensive rats. Anesth Analg 90: 546-552.
-
Park SY, Jung I, Kwon SC (2011) Mechanism of vasodilation by propofol in the rabbit renal artery. Anesth Pain Med 6: 336-341.
-
Eyraud D, Mouren S, Teugels K, Bertrand M, Coriat P (1998) Treating anesthesiainduced hypotension by angiotensin II in patients chronically treated with angiotensin-converting enzyme inhibitors. Anesth Analg 86: 259-265.
-
Brabant SM, Eyraud D, Bertrand M, Coriat P (1999) Refractory hypotension after induction of anesthesia in a patient chronically treated with angiotensin receptor antagonists. Anesth Analg 89: 887-888.
-
Brabant SM, Bertrand M, Eyraud D, darmon PL, Coriat P (1999) The Hemodynamic Effects of Anesthetic Induction in Vascular Surgical Patients Chronically Treated with Angiotensin II Receptor Antagonists. Anesth Analg 88: 1388-1392.
-
Sear JW (2014) Perioperative renin-angiotensin blockade: to continue or discontinue, that is the question! Anesth Analg 118: 909-911.
-
Dagnino J, Prys-Roberts C (1984) Studies of anaesthesia in relation to hypertension. VI: Cardiovascular responses to extradural blockade of treated and untreated hypertensive patients. Br J Anaesth 56: 1065-1073.
-
Folkow B (1982) Physiological aspects of primary hypertension. Physiol Rev 62: 347-504.
-
Colson P, Saussine M, Seguin JR, Cuchet D, Chaptal PA, et al. (1992) Hemodynamic effects of anesthesia in patients chronically treated with angiotensinconverting enzyme inhibitors. Anesth Analg 74: 805-808.
-
Murkin JM, Arango M (2009) Near-infrared spectroscopy as an index of brain and tissue oxygenation. Br J Anaesth 103 Suppl 1: i3-13.
-
Bevan PJ (2015) Should Cerebral Near-infrared Spectroscopy be Standard of Care in Adult Cardiac Surgery? Heart Lung Circ 24: 544-550.
-
Coriat P, Richer C, Douraki T, Gomez C, Hendricks K, et al. (1994) Influence of chronic angiotensin-converting enzyme inhibition on anesthetic induction. Anesthesiology 81: 299-307.
-
Morelli A, Tritapepe L, Rocco M, Conti G, Orecchioni A, et al. (2005) Terlipressin versus norepinephrine to counteract anesthesia-induced hypotension in patients treated with renin-angiotensin system inhibitors: effects on systemic and regional hemodynamics. Anesthesiology 102: 12-19.
-
Curran MP, Robinson DM, Keating GM (2006) Intravenous nicardipine: its use in the short-term treatment of hypertension and various other indications. Drugs 66: 1755-1782.
-
Salgado DR, Silva E, Vincent JL (2013) Control of hypertension in the critically ill: a pathophysiological approach. Ann Intensive Care 3: 17.
-
Wald NJ, Law MR (2003) A strategy to reduce cardiovascular disease by more than 80%. BMJ 326: 1419.
-
de Waal BA, Buise MP, van Zundert AA (2015) Perioperative statin therapy in patients at high risk for cardiovascular morbidity undergoing surgery: a review. Br J Anaesth 114: 44-52.
-
Lee SM, Takemoto S, Wallace AW (2015) Association between Withholding Angiotensin Receptor Blockers in the Early Postoperative Period and 30-day Mortality. Anesthesiology 123: 288-230.





