Hypertension (HTN) in childhood is a serious cause of mortality and morbidity Hypertension during childhood is diagnosed more than past as a consequence of increasing awareness about childhood hypertension, measuring blood pressure by the accurate technique and childhood obesity epidemic.
Demographic profiles, treatment regimens, response to treatment and etiology of hypertension were reviewed in children diagnosed with hypertension in this study.
Retrospective cross-sectional study.
Children diagnosed with hypertension in our center between January 1, 2012 and December 31, 2013 was reviewed in this study.
The mean age of 231 patients diagnosed as hypertensive was 14.4 ± 4.5 at the time of diagnosis. One hundred seventeen patients (50.6%) were classified as having primary hypertension and 49.4% of the patients were classified as having secondary hypertension. Family history was present in 11.7% of the patients. Twenty patients with primary hypertension had family history whereas 7 patients with secondary hypertension had family history; this difference was statistically significant (p = 0.01). There were 17 hypertensive children with chronic kidney disease and 20 renal transplantation patients were found to be hypertensive. End organ damage was found in 136 patients. Ninety four patients were advised life style changes, 60 patients were treated by calcium channel blockers, 22 patients by angiotensin converting enzyme inhibitors, 19 patients by beta blockers and the rest of the patients by combined therapy. Treatment was efficient in 76.6% of the patients. Response to treatment did not differ between primary and secondary hypertension.
There was no association between end organ damage and younger age at the time of diagnosis.
Our study results highlighted the need for more detailed studies to investigate the main causes of secondary HT in younger hypertensive children and also suggested that children with a family history of HT should be monitored closely. Assessment of the end-organ damage is also of utmost importance for diagnosis, follow-up, and the evaluation of treatment options. It is also emphasized that monotherapy should be initiated in patients who are unresponsive to the dietary changes, who have secondary HT, and who exhibit end-organ damage.
Hypertension, Children, Etiology, End-organ damage
Hypertension (HT) is a major risk factor for cardiac, cerebral, and vascular diseases that develop in the later years of life, although its origins can often be traced back to childhood. Compared to the adults, the prevalence of HT is lower among children (1 to 2%). However, the incidence of primary HT has been gradually increasing due to several factors such as the routine measurement of blood pressure in the outpatient clinics, obesity resulting from the excessive consumption of foods with high calorie and fat content, increased consumption of salt, reduced physical activity, and increasing stress [1,2].
Examination of the end-organ damage is important for making a decision on treatment, predicting prognosis, and assessing the degree of HT.
The relationship between HT and development of atherosclerosis during adolescence has been demonstrated in autopsy studies [3]. Other indicators of end-organ damage include the left ventricular mass, retinopathy, and the urinary albumin excretion. Ambulatory Blood Pressure Monitoring (ABPM) is considered superior to instant blood pressure measurements in predicting the end-organ damage [4].
In the present study, the demographic characteristics, end-organ damage, treatments and treatment responses of children with HT were evaluated, and the etiology of HT was further investigated.
From January 2012 to December 2013, 231 children (112 girls, 119 boys) ranging in age from 1 years to 21 years had a diagnosis of hypertension determined at our center. Databases were collected retrospectively and the following data were retrieved from the clinical records; gender, age at diagnosis, symptoms, physical examination, laboratory measurements, echocardiographic results and the retinal examination.
Patients with HT caused by acute renal injury, as well as patients with hypertensive emergency (crisis) were excluded from the study.
This study was approved by the institutional review board and the need for individual informed consent was waived.
The blood pressures of the patients were measured using the manual auscultation method. Three measurements were made separately following a five-minute resting period, and the mean values were determined. Blood pressures values equal to or greater than the 95th percentile according to the age, sex, and height of the patient were considered as HT. The patients were classified according to the HT stages defined by the National Health and Nutrition Examination Survey (NHANES) group: pre-hypertensive: blood pressure between the 90th and 95th percentile; stage 1: blood pressure between the 95th percentile + 5 mmHg and 99th percentile; stage 2: blood pressure 5 mmHg greater than the 99th percentile [5].
Primary hypertension is defined as high BP in which secondary causes such as renovascular disease, renal failure, coarctation of aorta, pheochromocytoma, aldosteronism, or other causes of secondary hypertension or mendelian forms (monogenic) are not present.
The Body Mass Index (BMI) was calculated as weight in kilograms divided by the square of height in meters. Patients with a BMI greater than the 95th percentile according to their age and sex were defined as obese.
All patients with HT were tested for plasma renin activity, aldosterone, creatinine clearance, serum electrolytes, fasting blood glucose, lipid profile, and uric acid, and also underwent renal Doppler ultrasonography to exclude the secondary causes of HT. To evaluate end-organ damage, Complete Urinalysis (CUA) and 24-hour urine protein test were performed, and consultations were requested from the Pediatric Cardiology and Ophthalmology Departments.
Routine two-dimensional echocardiographic evaluation was performed with an ultrasound system provided with pulsed, continuous and colour Doppler (Vivid-6 GE® and HP Sonos 5500®). The left ventricular end-diastolic diameter, Ejection Fraction (EF), shortening fraction, and septal thickness were noted at the parasternal long axis view using the M-mode echocardiography. All echocardiographic evaluations were carried out according to the recommendations of the American Society of Echocardiography guideline.
Fundus examinations were made in a dark room by an ophthalmologist after dilating the patients' pupils with a cycloplegic eye drop, and by using a direct ophthalmoscope. The retinal lesions were classified according to the Keith-Wagener-Barker staging system, as defined by Keith, et al. in 1939 [6].
Statistical analysis was performed using the SPSS v21.0 software (SPSS Inc., Chicago, IL, USA). Data are described as frequencies, median with interquartile range, and means with Standard Deviation (SD), where appropriate. Normally distributed continuous variables were compared by analysis of variance techniques, while non-normally distributed continuous variables were compared using the Mann-Whitney U nonparametric method. The chi-square test, and when appropriate, Fisher's exact test, was used to test for differences in proportions. The quantitative data were analyzed using the Pearson's and Spearman's correlation analyses. A p value of < 0.05 was considered as statistically significant.
The study included 231 patients (112 females, 119 males) with a mean age of 14.46 ± 4.50 (range: 1 to 21) years. Mean body weight, height and body mass index values were 54.12 ± 18.90 kg, 139.83 ± 17.12 cm and 21.60 ± 4.94, respectively. Twenty-four patients were considered overweight (body mass index BMI > 85th percentile), while 36 patients were obese (BMI > 95th percentile).
A family history of HT was identified in 11.7% (27 cases) of the patients. Among all cases, 141 were asymptomatic, while the most common complaints on admission were headache in 42 patients, and nosebleed in 18 patients. These signs were followed by vertigo, dizziness, and tinnitus.
Secondary HT was identified in 49.4% of the patients, while 50.6% had primary HT. The frequency of secondary HT was found to be higher in younger patients (Table 1). The most common cause of secondary HT was renal parenchymal disease (56 patients) in all age groups, while aortic coarctation was observed in eight patients. Renal artery stenosis and congenital renal anomalies were identified in 4 and 24 patients, respectively. There were 17 hypertensive children with chronic kidney disease and 20 renal transplantation patients were found to be hypertensive.
Table 1: The association of age of diagnosis, family history and type of hypertension. View Table 1
The family history was present in 20 of the cases with primary HT, while only 7 patients with secondary HT had a family history, indicating a significant difference (Table 1).
Primary HT was detected in 34 of the 36 obese patients, and in 83 of the 195 non-obese patients, indicating a significant difference (Figure 1).
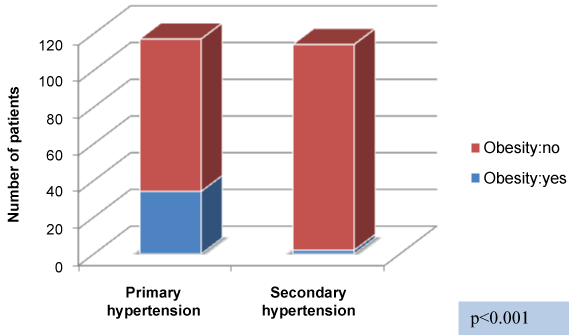 Figure 1: Association between hypertension etiology and obesity.
View Figure 1
Figure 1: Association between hypertension etiology and obesity.
View Figure 1
Of the 136 patients with end-organ damage, hypertensive retinopathy was found in 47 (20.3%), left ventricular hypertrophy in 30 (13%), and proteinuria in 59 (25.5%) (Table 2).
Table 2: End organ damage of patients with hypertension. View Table 2
Treatment options involved; life style changes for 94 patients, calcium channel blocker for 60 patients, Angiotensin-Converting Enzyme Inhibitor (ACEI) for 22 patients, beta-blocker for 19 patients, and combination therapy for remaining patients. Among all cases, 76.6% of them improved with first-line treatment. There was no significant difference in the response to treatment between primary HT and secondary HT patients (Table 3).
Table 3: Assesment of therapy in children with hypertension according to etiology. View Table 3
End-organ damage was found to be significantly more common in patients with secondary HT (Figure 2) while diagnosis at younger ages was not found to affect the end-organ damage (Table 4).
 Figure 2: Association of end-organ damage and type of hypertension.
View Figure 2
Figure 2: Association of end-organ damage and type of hypertension.
View Figure 2
Table 4: The association between end-organ damage and age of diagnosis. View Table 4
The development of end-organ damage did not differ significantly in the patients with insulin resistance or diabetes, while it was significantly higher in the patients with chronic renal failure (Table 5).
Table 5: Correlation between end-organ damage and associated diseases. View Table 5
Hypertension in childhood and the relationship of HT with high cardiovascular morbidity and mortality are serious health problems that have become more important in recent years. In a cohort study by Lo, et al. [7] on 200,000 healthy children, whose ages varied between three and seven years, 12.7% were found to have pre-HT, while 5.4% had HT. Measurements of the systemic blood pressure in this age group are of utmost importance for identifying hypertensive children, as well as children with end-organ damage secondary to HT [8]. Hypertension in childhood has been demonstrated to be an etiological factor in 50% adults with end-stage kidney failure [9]. While it is presently accepted that HT complications first emerge in childhood, it is still unknown at what frequencies and in which cases it develops. We therefore evaluated the demographic characteristics of patients with childhood HT, as well as the disease etiologies, the presence of the end-organ damage, the treatment options, and the responses to treatment.
It is often suggested that most systemic HT in children are secondary; however, the incidence of primary HT has increased in the recent years, particularly due to the increased incidence of obesity and the alterations in eating habits [10]. In a multicenter study on 351 children whose ages varied between 1 and 16, the rate of secondary HT was found to be 83% in the patients below six years of age, while this rate was 50% among all cases [11]. In the same study, the frequency of obesity was found to be lower in hypertensive patients younger than six-years-old. We similarly determined in our study that the incidence of secondary HT increases with decreasing age. Therefore, it may be concluded that a more detailed investigation is essential in the hypertensive children at younger ages.
Several studies have reported the following rates of essential HT: Lieberman, et al. 21%, Uhari, et al. 20%, Gill, et al. 2%, and Loirat, et al. 12% [12-15]. In our study, the incidence of primary HT was determined as 50.6%. This rate is not an indicator of actual incidence, since the patients included in our study were selected cases who were referred to our clinic due to HT. In addition, we suggest that the incidence of primary HT may be actually higher, as the patients with chronic renal failure and those who underwent kidney transplantation were also included in the present study.
Various studies have demonstrated that the genetic factors may play a role in the pathogenesis of HT at rates of 30% to 50% [16]. Hypertension is thought to have a multifactorial inheritance. Studies indicate that most patients with HT have a family history and HT is observed more commonly among identical twins than fraternal twins. Such findings clearly demonstrate the role of genetic factors in the pathogenesis of HT. In our study, 11.7% of the patients had a family history of HT. The ratio of family history was found to be significantly higher in patients with primary HT. Thus, the present study suggests that, given the altered eating habits in today's world, children of parents with HT need to be monitored more closely.
As HT in children is generally asymptomatic, the guidelines recommend that each child should be annually monitored for blood pressure beginning from the three years of age. In our study, 61% of patients did not have any complaints on admission, with HT being incidentally detected during routine examination. Therefore, we recommend that measurement of blood pressure in children should be properly performed during each examination, even if there are no complaints.
It has been demonstrated that nearly 40% of the children with pre-HT and HT suffer from impaired left ventricular anatomy [17]. In our study, the incidence of left ventricular hypertrophy was found to be 12.9% and the cardiac influence was higher in secondary HT cases. The higher rate of cardiac influence in secondary HT can be attributed to the patients with chronic renal failure among these cases, as it has been shown that patients with chronic renal failure have higher cardiac influence, independently of HT.
In the US, HT is the second leading cause of end-stage kidney failure in adults. Several studies have demonstrated that the levels of urine microalbumin are higher in children with primary HT compared to the normal population [18]. Microalbuminuria, which is strongly associated with cardiovascular disease and early mortality, is considered as an indicator of extensive endothelial damage [19]. In our study, proteinuria was also assessed and found in 25.5% all patients; it was also noted that proteinuria was significantly higher among secondary HT patients than primary HT patients. A limitation of this study is the missing data of microalbuminuria.
Except those with chronic renal failure, the kidney functions of all other patients were normal.
Opthalmic assessment and detection of hypertensive retinopathy is essential for the evaluation of end-organ involvement. In the study of Conkar, et al. frequency of hypertensive retinopathy is found as 35.3% whereas Williams, et al. mentioned it as 18% [20,21]. We found hypertensive retinopathy in 47 patients (20.3%).
One of the most important and unexpected finding of this study was that end-organ damage was not associated with the age of the children.
Medical treatment is recommended for children with persistent HT who are unresponsive to life style changes. The main goal is to maintain blood pressure at a level below the 90th percentile according to the age and sex of the patient. A decrease in body weight, accompanied by proper dietary treatment and increased physical activity, has been reported to reduce blood pressure in obese children. Pharmacological treatment must be administered to patients who are unresponsive to dietary changes and who have end-organ damage [22-24]. The study of Yoon, et al. showed that the most commonly used group of drugs in patients between the ages of 12 and 18 years was ACEIs, and that combination therapy is administered to nearly one-fourth of the patients [25]. In the same study, diuretics were found to be the second mostly administered as monotherapy drugs in adolescents. In our study, pharmacological treatment was not initiated in 94 patients and 84 (89.3%) of these patients improved with life style changes alone. Hypertension was brought under control by a calcium channel blocker monotherapy for the remaining 10 patients. A higher rate of response to life style changes was observed among the HT patients compared to other studies. This was attributed to the frequent monitoring of the patients, which contributed patient compliance. In the study of Bouissou, et al. they monitored 25 children with secondary HT between the ages of 1.5 and 18 years for an average period of 14.8 months [26]. They reported that the blood pressure of nearly all of these children could be effectively managed with a single medication, with a second drug being necessary in only 13% of them. Similarly, we administered combination therapy to only 15.5% of the patients in our study.
In conclusion, the incidence of primary HT has been gradually increasing due to the present-day changes in eating habits. Our study results highlighted the need for more detailed studies to investigate the main causes of secondary HT in younger hypertensive children, and also suggested that children with a family history of HT should be monitored closely. As HT is commonly asymptomatic in children, blood pressure should be measured at each visit, even if there are no complaints. Assessment of the end-organ damage is also of utmost importance for diagnosis, follow-up, and the evaluation of treatment options. Blood pressure can be managed by life style changes and follow-up visits scheduled at short intervals. It is emphasized that pharmacological treatment in the form of a monotherapy should be initiated in patients who are unresponsive to the dietary changes, who have secondary HT, and who exhibit end-organ damage.
This research received no specific grant from any funding agency, commercial, or not-for-profit sectors.
None.
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national guidelines.