The SPRINT trial was a landmark study and appeared to set new aggressive goals for the treatment of hypertension. It relied upon an average of multiple blood pressure measurements taken with an automated blood pressure cuff with a noted cool-down period beforehand. Our study was designed to see if the values obtained in common office practice differed from the so called "research grade" numbers achieved in the SPRINT trial. To accomplish this, we had participants screened with a manual cuff pressure per normal clinic protocols. Their blood pressure was then assessed in a more structured method incorporating rest periods between successive measurements with an automatic cuff. The results showed that for mean-automatic--to-manual BP, a statistically significant difference was found for systolic differences (t = 3.992, df 51, p < 0.001). At the same time, neither the first-automatic-to-mean automatic BP matched pair differences were found to be statistically significant for either systolic (t = 0.167, df 51, p = 0.868) or diastolic (t = 0.235, df 51, p = 0.815) BP reading differences. We believe that applying the goals of the SPRINT trial within the context of manually obtained blood pressures will lead to discrepancies for clinicians. At the very least, a rest period with an undisturbed environment should be sought when taking blood pressures.
Hypertension, Sprint, Manual blood pressure, Automatic blood pressure, Office
Hypertension is quite an important condition in our society. Currently affecting more than one billion people per latest estimates, its prevalence becomes even more important in those greater than 60 years of age. Systolic blood pressure, in particular, becomes an important risk factor indicator for subsequent coronary events, stroke, ESRD, and heart failure. Clinical data indicates that efforts made at lowering it result in reduced risk of developing such catastrophic outcomes. Significant studies such as the recent SPRINT trial have shown that it becomes important to evaluate how aggressive blood pressure reduction needs to be in order to curtail risk of cardiovascular events [1]. This implies having an accurate reading of blood pressure in order to be successful. However, that is not always easier to come by. Previous research has shown that differences in blood pressure measurement exist between medical personnel and trained physicians with medical personnel tending to overestimate blood pressure [2]. This has implications, for example determining ASCVD risk when taking into account office blood systolic blood pressure readings. A study by Ye, et al. has previously shown that systolic blood pressure variability can lead to inaccurate CVD risk estimation and thus influence statin strategy [3]. More so, selective blood pressure techniques pertaining to rounding and selecting numbers near treatment cut offs have been shown to affect cardiovascular and all-cause mortality in prospective studies [4]. This shows the significant importance placed on obtaining precise blood pressure values. While home blood pressure measurements are a formidable option, compliance with patients can be an issue with lower levels of education and younger age predicting poor follow through [5]. Depending on the clinical setting and the population served, it may be more beneficial to stick with office blood pressure readings. The question in essence becomes whether we are better off measuring blood pressure multiple times in order to ensure accuracy. Indeed, previous research has shown that multiple reads during an office visit better predict out of office blood pressure [6]. This is something worth considering in light of the fact that clinicians often have to rely on a single blood pressure reading to determine risk stratification, treatment protocol, etc. The SPRINT trial, as mentioned before, was immediately touted as a landmark study and appeared to set new aggressive goals for the treatment of hypertension. It relied upon an average of multiple blood pressure measurements taken with an automated blood pressure cuff with a noted cool-down period beforehand. Our study is designed to see if the values obtained in common office practice differs from the so called "research grade" numbers achieved in the SPRINT trial. What we propose is a prospective study examining blood pressure as an average of three reads. We would compare this average to a first read as well as a manual blood pressure to examine any variability's. Our hypothesis is that there will be differences of at least 5 millimeters in mercury when the values are compared.
Inclusion criteria were English-speaking patients of both sexes greater than 18-years-old with a history of HTN, regardless of stage, whose blood pressure required monitoring to ensure proper follow up. Exclusion criteria was age less than 18-years-old with no history of HTN or those who decline study, cannot give informed consent, or were non-English speaking. Patients/Participants who had standing appointments with the office were enrolled. The principal investigator or academic advisor identified patients with reported history of hypertension through medical records contained in their paper charts. Patients were given a form describing the study and its intended measures with the principal investigator and academic advisor available to answer any questions. If a verbal/signed agreement was made, the process was begun as described shortly. The supervising physician/academic advisor was in charge of the clinic an involved in the care of a majority of the patients while the principal investigator was a resident managing a smaller subset of patients. All patients had their blood pressure assessed with a manual cuff by nursing staff in one room as is current clinic protocol. They were then placed in dedicated separate examination rooms with a quiet environment to avoid any distracting stimuli that could potentially cause an increase in blood pressure. Omron HEM- 907XL automated cuffs were then used to obtain three consecutive blood pressure reads performed by the supervising physician/academic advisor thereafter, usually around 5-10 minutes after. Estimated time for automated measurements after check-in was around 25 minutes although this could vary considering how busy the clinic was. The American Heart Association has published guidelines for proper technique in assessing blood pressure and this was used as standard practice. Protocol consisted of putting cuff on one arm with arm support being at heart level. The legs were uncrossed with support for the back and feet in place. No conversation were had during blood pressure measurements and all patients were asked to empty bladder before measurement. There was a 5 minute rest period before the first measurement, followed by another 5 minutes before the second measurement, and ending with another 5 minute period before the third measurement. We predicted the average time needed to complete this protocol lasted around 16-20 minutes.
Study data from 52 hypertensive adult patients was ultimately analyzed. A total of 24 (46.2%) of the total sample were women. All enrolled patients had a mean age was 56.83 years (SD 11.749) years and ranged from 22 to 77 years. Participants' average manual systolic BP reading was 129.38 mmHg (SD 21.914) and diastolic 79.02 mmHg (SD12.046). Conversely, Participants' average automatic systolic BP reading was 126.38 mmHg (SD 24.9190) and diastolic 81.15 mmHg (SD 14.829). The average difference in patients' manual-to-mean automatic systolic BP reading was 4.96 mmHg (SD 10.550) and diastolic - 1.04 mmHg (SD 8.122). The average difference in patients' initial-automatic-to mean-automatic systolic BP reading was 1.15 mmHg (SD 6.918) and diastolic 0.87 mmHg (SD 6.046) (Figure 1).
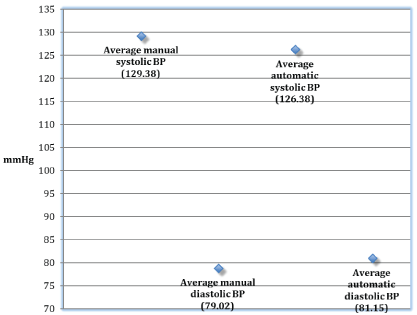 Figure 1: The average readings for both manual vs. automatic modalities with comparisons of systolic and diastolic pressures. All values listed in mmHg.
View Figure 1
Figure 1: The average readings for both manual vs. automatic modalities with comparisons of systolic and diastolic pressures. All values listed in mmHg.
View Figure 1
Using a series of both initial and controlled (i.e., controlling for both gender and age group), a series of two-tailed matched pair T-test comparison of means and repeated measure one-way Analyses of Variance (ANOVA) procedures were conducted with selected study measures. No significant differences were found when stratifying BP readings data by either gender (significant p values ranging between 0.379 and 0.076) or age group (significant p values ranging between 0.275 and 0.677).
In terms of mean-automatic--to-manual BP differences, a statistically significant difference was found for systolic differences (t = 3.992, df 51, p < 0.001) but not for diastolic differences (t = 0.281, df 51, p = 0.780). Of key interest, neither the first-automatic-to-mean automatic BP matched pair differences were found to be statistically significant for either systolic (t = 0.167, df 51, p = 0.868) or diastolic (t = 0.235, df 51, p = 0.815) BP reading differences.
Similar results were found when comparing first automatic-to mean automatic BP differences whether treating differences in continuous (ANOVA) and {0,1} dichotomous (logistic regression) terms with and without potential age group and gender factors included.
Upon implementing series of non-parametric Wilcoxon signed-rank tests for smaller two related matched and repeated measures samples, all systolic-to systolic comparisons were not statistically significant observing a coefficient alpha of 0.05. As follows, manual systolic (Mean 129.38 (SD 21.91) to first automatic systolic (Mean 126.12 (SD 22.25): t = 1.736, df 51, p = 0.089. Manual systolic (Mean 129.38 (SD 21.91) to second automatic systolic (Mean 127.92 (SD 23.77): t = 0.745, df 51, p = 0.460. Manual systolic (Mean 129.38 (SD 21.91) to third automatic systolic (Mean 126.79 (SD 22.17): t = 1.398, df 51, p = 0.168.
Diastolic-to-diastolic comparisons were not statistically significant as well save the second automatic comparison measures. As follows, manual diastolic (Mean 79.02 (SD 12.05) to first automatic diastolic (Mean 80.96 (SD 15.17): t = -1.600, df 51, p = 0.116. Manual diastolic (Mean 79.02 (SD 12.05) to second automatic diastolic (Mean 82.69 (SD 17.64): t = 2.198, df 51, p=0.033. Manual diastolic (Mean 79.02 (SD 12.05) to third automatic diastolic (Mean 79.71 (SD 15.28): t = -0.570, df 51, p = 0.571.
This study looked at 52 participants with a history of hypertension that requires monitoring and compared manual blood pressures normally attained in clinic with a rigid automatic blood pressure protocol used in the SPRINT trial. There was indeed a significant difference found between manual and mean systolic automatic blood pressures and not for diastolic pressures. There were no significant differences between first automatic and mean automatic blood pressures for both systolic and diastolic. In interpreting these findings, systolic blood pressures are generally considered more clinically significant compared to diastolic as is evident in most of the literature. The outcome of a lower mean systolic pressure via automatic cuff that takes into account a rest period before measurement compared to a manual pressure via routine clinical practice was in line with previous findings [7,8]. The proximity of values between the two measurements was also evident for both systolic and diastolic. However, this study was limited by the sample size of the subjects that may have not let us reach a one minus beta level of statistical power. The effect of a few atypical measurements is more amplified and can lead to significantly larger standard deviations than what may actually exist. The notion would be to test on a perhaps larger sample in future studies in order derive more firm conclusions. The study did not keep baseline data pertaining to active or history of previous medical conditions. Thus, participants in this study may not necessarily fit the population cohort of the SPRINT trial which included those with clinical/subclinical CVD and CKD with eGFR of 20-59 ml/min/1.732 and excluded those with diabetes, history of stroke, polycystic kidney disease, or heart failure. Not to mention the differing age criteria between our study and the SPRINT trial, which specifically focused on those greater than 50 years of age. Thus any extended statistical comparison with the SPRINT trial numbers would not be plausible. Patients' smoking status, cholesterol levels, classes of antihypertensive currently on were also not recorded. Any history of white coat hypertension that could presumably inflate values was not noted as well. It is possible such factors as well as extraneous reasons may have acted as confounding variables. The question of the sample size ensuring external validity is something worth noting considering the amount of participants and possibly being influenced by geographical location of the office practice. Our eligibility requirements were kept minimal-we did not exclude participants due to various stages of hypertension or comorbidities. There were not potential participants deferred due to language barriers. Only one participant's data had to be discarded due to the automatic blood pressure cuff malfunctioning. The requirement of age was given since the clinic does not treat the pediatric population. As such, an attempt at precluding sampling bias was achieved to the best of our efforts. This study relied on a well-established protocol from a national multi-center study, the SPRINT trial, and offered a direct comparison with manual sphygmomanometer measurements. It utilized equipment, whether the manual or automatic cuff, which was consistently used on all participants, ensuring no deviations in blood pressure could be attributed to manufacturer differences. The Omron HEM-907XL has been validated in the ONTARGET and ACCORD trials in addition to SPRINT. The protocol in itself proved feasible in a busy practical clinical setting albeit a time-consuming process particularly with investigators involved in clinical duty.
The question clinicians often have to consider is who must we look out for that could be disposed to hypertension issues? Studies have shown that uncontrolled hypertension is more common among the poor, diabetics, older women, those over age of 60, and non-Hispanic blacks. Also highlighted is the decreased awareness in those who are uninsured, with fewer exposure to healthcare utilization, and reporting fewer health risk factors [9,10]. Clinicians being more attentive of their own clinic demographics places importance on those that otherwise may be overlooked. Yet, an encouraging trend per recent database analysis has shown the prevalence of hypertension remaining static overall with increasing compliant rates [11]. Linking office-measured blood pressure with ambulatory values is worth discussing with the SPRINT ambulatory ancillary study offering some insight. Clinic systolic blood pressures measured in similar protocol as the SPRINT trial were lower compared to the mean 24 hour and daytime systolic blood pressure, both in the standard therapy arm vs. intensive therapy arm [12]. Comparative studies have found automated office blood pressures to relate more closely with ambulatory daytime blood pressures than with manual pressures which are typically higher than both [7,8]. A landmark study in 2011 also pointed out the automated route aligned with the awake systolic ambulatory pressure had a stronger correlation with left ventricular mass index, a measure of end organ injury than its counterpart [13]. Whether or not a relationship exists with the results of this study remains to be seen, yet it does highlight an interesting point. This is something from a clinical perspective provider could consider when perhaps evaluating the aggressiveness of their antihypertensive regimen.
A study examining participants from the NHANES '99-'08 database evaluated how often those with a single measurement as is usual for clinic visits were reclassified to a different BP category when multiple measurements and their averages were taken. The findings showed less than 10 percent being reclassified from normal to pre-hypertensive. Even more so, 8-23.6 percent were reclassified from pre-hypertensive to normal and 18.2-33.5 with stage 1 and 2 hypertension being reclassified to lower BP categories [14]. Possible explanations for this may relate to user sensitivity as mentioned earlier. It also brings up the issue of white coat hypertension that could play a role in influencing our manual blood pressure measurements. An important point about white coat hypertension is it not necessarily being consistent across a wide spectrum-evidence lends to its variable nature with prevalence being higher in older females and minimal in others [15]. There is variability between patients but also within patients, thus attempting to quantify its effects may not necessarily be practical [16,17]. On the other hand, automated office devices are effective at reducing white coat influences [18]. An important question is whether clinicians may be satisfied with marginal errors in blood pressure for the sake of convenience-perhaps patients with normal blood pressure may not need repeated measures but those in the pre-hypertensive range and above could benefit from closer scrutiny given clinicians stick with the manually-obtained route. This also brings up another point, which is what happens when clinicians are dealing with patients whose blood pressure is perhaps reduced far too much. A point of contention with the SPRINT trial has been that aggressive lowering i.e. less than 120 mmHg is fraught with cardiovascular complications. A cross sectional study examining 24, 537 albeit Caucasian participants found that those with SBP lesser than 120 mmHg had higher rates of MACE and all-cause mortality at statistically significant levels [19]. The population cohort was not completely in line with SPRINT trial criteria, however, this does underlie a concern for the medical community and future guideline implications. For the office, clinicians would have to evaluate how comfortable they are in regard to therapy goals and compliance.
An interesting note was the erratic variability in blood pressure measurements across automatic blood pressures in some particular individuals. This is intriguing given the circumstances as to how the blood pressure is measured would not necessarily allow for fluctuations-a short period of time between measurements with no interruptions, a confined space with distractions kept to a minimal, same technique per guidelines for consecutive measurements. The reason as to why this happened is interesting. Beat-to-beat blood pressure variability is a known phenomenon. It has been postulated to be caused by a variety of factors-the interplay of the baroreceptor reflex, the renin-angiotensin system (RAS), release of nitric oxide from the endothelium, and the vascular response related to the elasticity of the arteries. This is not withstanding the emotional factors as well as rheological influences [20-22]. All individual factors differ considerably in their response rate, and as such at any given time one may be more than influential than others. This could explain the shifts in blood pressures noticed in a subset of participants.
Furthermore, the visit-to-visit blood pressure variability draws some interesting findings. When we explore the literature, we find that in the third NHANES database that included more than 30,000 participants, variation in systolic blood pressure occurred across multiple visits in individuals with a mean standard deviation of around 7.7 mm Hg [23]. Similarly, the Women's Health Initiative that looked at data from 58,00 participants, systolic blood pressure varied to a standard deviation of almost 11 across multiple visits [24]. Interestingly enough, a meta-analysis 77,299 patients found that visit-to-visit systolic blood pressure variation, independent of age or a mean systolic blood pressure, was a strong predictor of cardiovascular and all-cause mortality. In particular, a 1 mm Hg SD increase saw a 10% higher risk cardiovascular mortality, 2% higher risk of stroke, and a 3% higher risk of all-cause mortality [21]. This means for those participants with noted blood pressure variability with the automatic cuff, it may be worth seeing if the changes continue from visit-to-visit. If so, these individuals need to be monitored more closely and individual risk factors modified to reduce their risk of potential catastrophic events in their lifetime.
Addressing our limitations and predictive power of this study, the results convey an understanding that systolic blood pressure differences exist across two distinct modalities. The SPRINT trial offered evidence for a stricter governance of blood pressure goals that has universally been met with praise. However, clinicians need to realize these goals assume one has standardized the blood pressure measurement approach in a protocol driven way. Applying the goals of the trial within the context of manually obtained, no-rest measurements will not lead to accurate results, and if our data outcomes are to be believed, would tend to overshoot these goals. We believe in a procedural approach akin to the SPRINT trial to evaluate blood pressure. However, we realize the outpatient setting, whether time or resource constraints, may not always allow this. Yet at the very least, clinicians could take into account the importance of a rest period and quiet, undisturbed environment.
Dr. Bill Corser of Michigan State University for data analysis and insight.