Journal of Musculoskeletal Disorders and Treatment
Outcomes of Non-operative Management of Deep Gluteal Syndrome - A Case Series of Six Patients
Ricardo Gonçalves Schröder1*, Rob Roy L Martin2, Valerie L Bobb3, Anthony Nicholas Khoury1,4, Ian James Palmer1 and Hal David Martin1
1Hip Preservation Center, Baylor Scott & White Health, Dallas, TX, USA
2Department of Physical Therapy, Duquesne University, Pittsburgh, PA, USA
3Baylor Institute for Rehabilitation - OP, Baylor Scott & White Health, Dallas, TX, USA
4Bioengineering Department, University of Texas at Arlington, Arlington, TX, USA
*Corresponding author:
Ricardo Gonçalves Schröder, Hip Preservation Center, Baylor Scott & White Health, 3900 Junius St. Suite 705, Dallas, Texas - 75246, USA, E-mail: ft.rschroder@gmail.com
J Musculoskelet Disord Treat, JMDT-2-012, (Volume 2, Issue 2), Case Series
Received: February 15, 2016: Accepted: April 25, 2016: Published: April 27, 2016
Citation: Schröder RG, Martin RRL, Bobb VL, Khoury AN, Palmer IJ, et al. (2016) Outcomes of Non-operative Management of Deep Gluteal Syndrome - A Case Series of
Six Patients. J Musculoskelet Disord Treat 2:012.
Copyright: © 2016 Schröder RG, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction:An increased understanding of posterior hip anatomy and biomechanics has led to advances in the diagnosis and management of Deep Gluteal Syndrome (DGS). Currently, there is limited information detailing the successful conservative management of DGS.
Materials and methods:The detailed history, physical examination, imaging, diagnostic testing, and physical therapy of six subjects diagnosed with deep gluteal syndrome were retrospectively analyzed and reviewed. Conservative treatment included neuropsychiatry management, intra-muscular injections through CT guidance, intra-pelvic assessment/therapy, and a home exercise program. The Visual analog scale (VAS), modified Harris Hip Score (mHHS) was utilized to measure outcomes of the non-operative treatment.
Results:Improvement was obtained in (100%) of the subjects with the combination of home exercises program, intra-muscular CT - Guided injection, physical therapy, and neuropsychiatric counseling. Average VAS scores decreased from 7.16 to 1.6, and average mHHS scores increased from 60.01 to 74. The average time in conservative therapy was 20 weeks (range: 6-36).
Conclusion:The conservative management of DGS was successful with positive outcomes achieved through a multi-professional approach accessing and treating DGS with a combination of physical, mental and social factors.
Introduction
An increased understanding of posterior hip anatomy and biomechanics has led to advances in the diagnosis and surgical management of Deep Gluteal Syndrome (DGS) [1-3]. Currently, non-operative interventions for DGS are directed to the piriformis muscle, the most known cause of DGS. Positive outcomes have been achieved through utilization of intra-muscular injections associated to physical therapy strategies such as electro-thermo, soft tissue length-tension, and movement reeducation [4-7]. DGS is a condition involved with musculoskeletal, psychological and social factors. A multiprofissional approach may be necessary to manage DGS addressing these factors.
DGS is a condition which patients frequently present with posterior hip pain associated to inability to sit for 30 minutes, radicular pain of the lower back or hip, and paresthesia's of the affected leg. The feeling of motor weakness can also present during standing activities [2,3,8,9]. Due to the anatomical variability surrounding the sciatic nerve, the etiology of the DGS can result from multiple structures such as bone, fibrous scar bands, and muscles [10-12]. DGS can coexist with and may be misinterpreted by intra-articular hip pathologies, and intra/extra-pelvic nerves entrapments, which also may acts an isolated potential causes of posterior hip pain [4,8,13]. Due to the difficult diagnosis, DGS commonly are associated to a chronic presentation with psychological and social disturbances. A comprehensive history, physical examination and imaging diagnosis are performed to precise the source of posterior hip pain, and rule out similar misinterpreted conditions [8].
The non-operative treatment of DGS is not well documented in the literature. The complexity of DGS, involving musculoskeletal, psychological and social components may require a multi-professional understanding and treatment strategy. The main objective in this study is to demonstrate the non-operative management of DGS through a case series of six subjects by a multiple approach to treatment.
Methods
This is a retrospective study that was previously approved by the Institutional Board Review (IRB) prior to data collection and meets the HIPPA requirements of Baylor University Medical Center.
Six subjects presenting with non-discogenic posterior hip pain for three months or more were included in the present study. Exclusion criteria were positive clinical or imaging findings for lumbar pathology (physical examination, lumbar spine radiographs, lumbar spine MRI) or previous surgical treatment for posterior hip pathology.
Diagnosis
A detailed history of the complaint was documented including duration of the symptoms and the presence or absence of trauma. The physical examination including an assessment of the osseous, capsulolabral, musculotendinous, neurovascular structures, and kinematic chain of the hip joint was performed by senior author (HM) and repeated by the physical therapist [14]. The seated piriformis stretch and active piriformis test were major, providing specificity and sensitivity to confirm DGS [8]. Palpation of the gluteal structures using the ischial tuberosity as reference helped to distinguish sources of pain. From lateral to medial, the sensation of pain at the sciatic notch characterizes the piriformis muscle; pain lateral to the ischium may represents ischial-tunnel syndrome or ischiofemoral impingement; and medial to the ischium pudendal nerve entrapment [15]. MRI imaging and diagnostic injection testing and history physical examination comprised the clinical diagnosis of DGS. Any history of previous pelvic surgery and urogynecological dysfunction was identified. Pelvic Floor Manual Muscle Test (PFMMT) [16,17] was utilized to evaluate the functioning and involvement of pelvic floor muscles.
Clinical data including: age, diagnosis, relevant history, surgical history and time from injury to begin physical therapy are given in Table 1.
![]()
Table 1: Clinical and demographical data of the patients included in the study.
View Table 1
Patient Management
Computed-Tomography (CT)-guided injections containing anesthetic, steroid and anti-inflammatory solutions (Marcaine, Kenalog, Sensorcaine, Depo-Medrol) were administered at the structure under investigation (piriformis muscle, obturator internus muscle, pudendal nerve, obturator nerve). Results of injection were utilized as treatment and/or differential diagnosis.
The neuropsychological assessment consisted of: Screener and Opioid Assessment for Patients with Pain (SOAPP-R); The Pain Catastrophizing Scale; Patient Health Questionnaire Somatic, Anxiety, and Depressive Symptom Scales (PHQ - SADSS); Minnesota Multiphasic Personality Inventory (MMPI-2-RF). These questionnaires evaluate the levels of anxiety, depression, drug abuse (opioids), and pain effects on personal behavior, personality and types of psychopathologies. Treatment strategies consisted of: psychological counseling, biofeedback therapy, and occupational therapy for pain management, physical activities using tai chi, aquatic therapy and relaxation strategies.
The physical therapy approach included patient education strategies, muscle strengthening, stretching, neural mobilizations, manual therapy (soft tissue length-tension rebalancing, articular manipulations), lumbo-pelvic stabilization, muscular rebalance and proprioception training. These interventions were also directed at pelvic floor dysfunctions when appropriate.
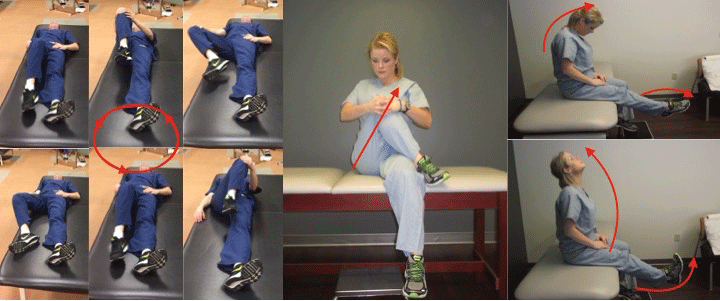
Each subject received a handout containing a home exercises program including: piriformis muscle stretch, neural mobilization (sliders) and hip joint mobilization (Figure 1).
.
Figure 1: Home Exercises Program. (a) Hip circumduction (sciatic nerve mobilization): Oscillatory hip/sciatic nerve mobilization utilizing the greater trochanter to mobilize the SN into the deep gluteal space. The motion comprises: 45° flexion + max abduction and external rotation followed by 90° hip flexion, 15° adduction + hip extension; (b) Deep Rotators muscle stretch: Affected leg crossed with the knee being pulled towards the contralateral shoulder, stretching sensation at the gluteal region. The duration of the stretch should not be longer than 20 seconds; (c) Neural Mobilization (neural sliders): Rhythmical motion of the superior and inferior segments. Combination of Head/trunk flexion with plantar flexion, followed by trunk/head extension with dorsal flexion.
View Figure 1
Outcomes of non-operative treatment were assessed by: modified Harris Hip Score (mHHS) [18] and Visual Analog Scale (VAS).
Results
All six subjects were female with an average age of 40.83 years (range 21-54 years). The duration of symptoms was an average of 20.16 months (range 6-60 months). Improvement was obtained in all subjects (100%) with the combination of home exercises program, intra-muscular CT - Guided injection, physical therapy, and neuropsychiatric counseling. Physical therapy and intra-pelvic evaluation/treatment were administered in 100% of the subjects. Only one subject did not receive injection as testing/treatment. Neuropsychiatric evaluation was referred for 100% of the subjects, with three subjects (50%) requiring neuropsychiatric treatment.
The average time of treatment was 20 weeks (range 6-36 weeks). Average VAS scores decreased from 7.16 (range 5-10) to 2.4 (range 0-3) and mHHS scores increased in average from 60.0 (range 36.3-93.9) to 74 (range 62.7-100) (Table 2). A table summarizing the details of physical therapy treatment, techniques and follow-up visits are given in Appendix.
![]()
Table 2: Outcomes of the non-operative treatment.
View Table 2
Discussion
The current study demonstrated a summary of a non-operative treatment strategy for DGS. The multidisciplinary approach addressed the main aspects involved with DGS utilizing a home exercise program, intramuscular injections, neuropsychological intervention, and supervised physical therapy.
Home exercises program
A group of complementary exercises utilized were designed to improve the function of the pelvic trochanteric muscles, sciatic nerve mobility, and hip range of motion. The piriformis muscle stretch was utilized to reduce contracture at the pelvic-trochanteric muscles, a mechanism that can contributes to increased gluteal pain [7]. Neural mobilizations exercises were utilized to increase the sciatic nerve range of motion and improve sensory and neural pain levels [19-21]. In case of neural tension and pain during neural mobilization exercises, the patient was instructed to release of sciatic nerve strain performing the exercise with the hip abduction [22]. Hip circumduction enhance the mobility of the sciatic nerve within the peritrochanteric space and help control muscular spasm/pain [23]. The clinicians involved in the treatment emphasized the importance of the home exercise program.
Intra-muscular CT-guided injections
Six subjects received intra-muscular CT-Guidance injection of anesthetic, steroid and anti-inflammatory solutions as a diagnostic tool and treatment. Three subjects required more than one intra-muscular injection to achieve improvement. One subject received piriformis and obturator externus muscles injections at different periods. In this case, the injection at the obturator externus muscle demonstrated better results than the piriformis muscle injection. This specific case may indicate the entrapment of the obturator nerve simulating symptoms of DGS [4,24]. One subject in the current study improved without the necessity of injections.
The utilization of intra-muscular injections combined with anesthetic, steroid solutions has become a valuable alternative for the treatment of syndromes related to excessive muscle contraction [5,25]. Fishman et al. demonstrated that 79% of patients diagnosed with piriformis syndrome improved symptoms by 50% at 10.2 months follow-up after physical therapy and injections (solution containing 1.5 mL of 2% lidocaine and 0.5 mL containing 20 mg triamcinolone acetonide) [5]. A mixed outcomes result has left the indications for intra-muscular injections as a treatment source. The necessity of multiple injections is recommended by the many clinicians literature when the relief of symptoms continues for at least three weeks [25-27]. Factors related to positive outcomes are proper patient selection, identification of etiology, anatomical variations and psychological and pathomechanic variations [28-30].
Neuropsychiatric assessment
Three subjects reported a history of depression and anxiety. One subject was referred to a neuropsychiatric evaluation after recurrence of symptoms. Common findings in this group were the chronicity of DGS and urogynecological dysfunctions, such as pain during intercourse, urinary incontinence, prolapsed uterus and endometriosis. Subjects with chronic pelvic pain commonly exhibit signs of anxiety and depression associated with the lack of definitive diagnosis, absence of local pathology, and a decreased quality of life scale [31,32]. A very few studies shows the effectiveness of an isolated neuropsychiatric treatment for chronic pelvic pain. However, cognitive therapy with a physical approach tends to produce good results in subjects diagnosed with chronic pain conditions [28,29]. Three subjects received a psychological evaluation with treatment. Out of these, two subjects obtained successful outcomes. Deep gluteal pain can affect personal and social life especially in those with chronic symptoms. Studies are needed to better understand the psychological influences of DGS and how these can be managed with psychological counseling.
Physical therapy intervention
The most common movement impairment was related to muscle weakness and poor neuromuscular control between lower extremities and the lumbopelvic segment. The physical therapy strategy utilized in this case series was designed to re-establish normal patterns of hip joint function and its biomechanical link with the lumbopelvic segment.
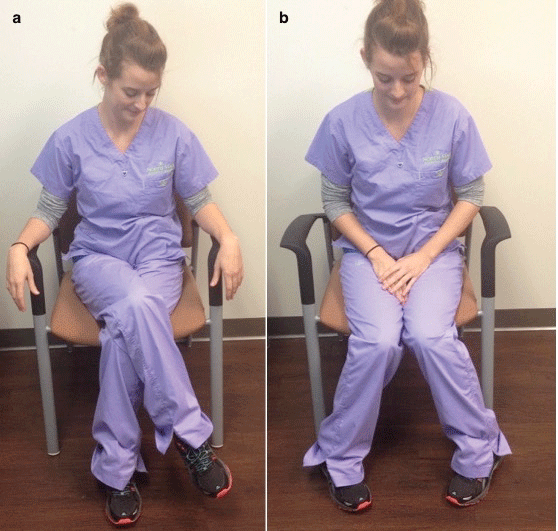
The first strategy for the physical therapist was an educational training addressing activity of daily living (ADL's). Educational training targeted the reduction of repetitive motions and avoiding repeated positions, such as the seated position with the affected side in constant internal rotation for an extended period of time (Figure 2). These positions may overstretch the external rotators of the hip joint [33,34], leading to weakness and lack of neuromuscular activation and stabilization of the lower limb during functional tasks [30]. Another complication related to these positions could be an increased strain of the sciatic nerve as recently observed in a biomechanical cadaveric study [22].
.
Figure 2: Positions that patients with DGS should avoid during ADL's. (a) Crossed legs; (b) Hips internally rotated.
View Figure 2
Myofascial therapy, muscular stretch and joint mobilizations were also utilized to decrease pain and re-establish proper muscular length and muscular activation. Neural mobilizations exercises were utilized to restore the ability of the nerve to tolerate compressive, tensile and frictional loads experienced during the normal kinematics of the hip joint [35-37]. The rehabilitation of the hip muscles and kinematic chain represents a key factor to succeed conservative management of DGS. A weakness of the gluteal muscles has been related to stiffness of the tensor fascia latae, and positioning the lower extremity in internal rotation. This mechanism may contributes to overstretching of the deep gluteal rotators [38-40]. The strengthening of the hip abductors and external rotators has produced positive outcomes in improving lower extremity balance [30,41,42]. Muscular strengthening of the hip deep external rotators, abductors and extensors was associated to proprioceptive activities in order to reestablish the correct motion of the lower extremities.
Five subjects presented with low back pain. Postural dysfunction plays a critical role in the muscular activation of the lumbopelvic stabilizators, alignment and lower extremity function [43-45]. Decreasing low back pain with lumbopelvic stabilization can improved the neuromuscular control and pain associated movement syndromes of the lower extremities [46]. Postural exercises and lumbopelvic muscle strengthening were designed to improve mobility and stability of the upper body in order to allow a better central stabilization for the lower extremities motion.
All subjects diagnosed with DGS were evaluated and treated after PFMMT. Four subjects showed positive findings of pudendal nerve entrapment with signals of tenderness or weakness of the pelvic floor muscles and tensions in the sacro-spinal and sacrotuberous ligaments. Episodes of urinary incontinence, pain during intercourse, history of pelvic surgery, endometriosis and ovarian cyst were also found. One subject reported a poor outcome with pelvic floor therapy. This subject ultimately achieved a positive outcome with a piriformis injection along with physical therapy approach. Dysfunctional pelvic floor musculature may lead to the recruitment of nearby global muscles such as the deep gluteal muscles to compensate for a weak pelvic floor and abdominal musculature [16,17,47]. The piriformis and obturator muscles perform a dual function that involves the hip joint stabilization, and making up the pelvic walls as part of the parietal fascia [38]. Pelvic floor therapy was focused on muscle function, enhancing activation of hypo-active muscles and relaxing hyperactive muscles [16,47-49]. A few studies have described the pelvic floor evaluation and treatment of pelvic floor dysfunctions associated with sciatic nerve entrapment in the sub-gluteal space [50,51]. The structural integration of lumbopelvic and hip structures by eliminating compensatory patterns represents another key factor in the conservative management of DGS.
Associated factors with deep gluteal syndrome
Female subjects composed the entire population of the present study. Particular anatomical characteristics of the female pelvis may be related to hormonal changes, pregnancy, structural abnormalities such as hip dysplasia and femoral anteversion. Hip pathologies related with instability [52-55] such as: labral tears, hip dysplasia, and ligament teres injury were constantly found in this present work. The joint incongruence and abnormal motion may overload intra/extra-articular structures to provide joint stability. The neuromuscular control of the hip joint provided by the piriformis, quadratus femoris, obturator/gemelli complex, gluteus minimus and medius is not completely understood. The deep pelvitrochanteric muscles may be overload in case of hip joint instability, consequently causing symptoms of DGS.
To date the present work is the only known that addressed the multi-factorial aspects of DGS. The literature shows positive outcomes through intra-muscular injections and physical therapy, however there is a lack of discussion in the literature about the chronicity of DGS and its negative effects in the psychosocial behavior. Furthermore, the utilization of pelvic floor therapy as a treatment strategy showed an additional diagnostic and treatment approach for those presenting posterior hip pain.
The present work has several limitations. First, the lack of comparison population may make this case series study prone to bias. Second, a small sample of female subjects composed the present study. Third, the treatment flow varying between subjects generated a lack of ability to generalize and compare cause and affect of the approach presented in this study.
Conclusion
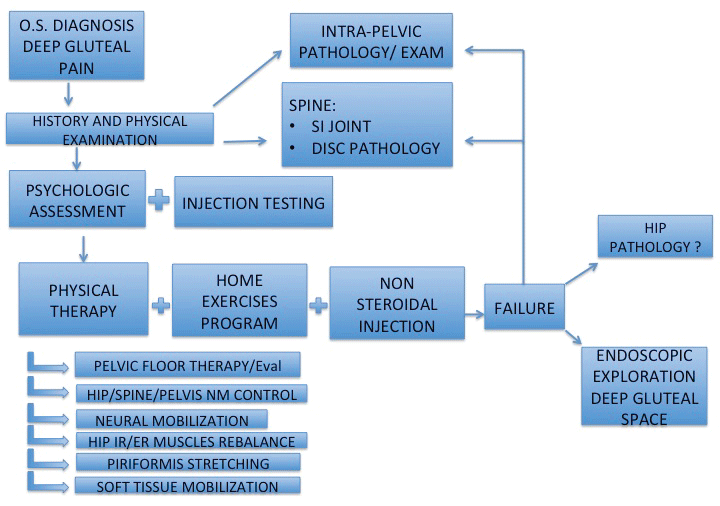
The present study demonstrated that positive outcomes were obtained through the combination of home exercises program, supervised therapeutic exercises, pelvic floor therapy, intra-muscular injection, and neuropsychiatric assessment/treatment (Figure 3). The current study establishes a commonality of rehabilitation techniques needed to further the establishment of a standardized approach to the conservative management of DGS.
References
-
Murata Y, Ogata S, Ikeda Y, Yamagata M (2009) An unusual cause of sciatic pain as a result of the dynamic motion of the obturator internus muscle. Spine J 9: e16-18.
-
Martin HD, Shears SA, Johnson JC, Smathers AM, Palmer IJ (2011) The endoscopic treatment of sciatic nerve entrapment/deep gluteal syndrome. Arthroscopy 27:172-181.
-
Byrd JWT (2005) Piriformis syndrome. Oper Tech Sports Med 13: 71-79.
-
Filler AG (2009) Diagnosis and treatment of pudendal nerve entrapment syndrome subtypes: imaging, injections, and minimal access surgery. Neurosurg Focus.
-
Fishman LM, Dombi GW, Michaelsen C, Ringel S, Rozbruch J, et al. (2002) Piriformis syndrome: diagnosis, treatment, and outcome--a 10-year study. Arch Phys Med Rehabil 83: 295-301.
-
Windisch G, Braun EM, Anderhuber F (2007) Piriformis muscle: clinical anatomy and consideration of the piriformis syndrome. Surg Radiol Anat 29: 37-45.
-
Tonley JC, Yun SM, Kochevar RJ, Dye J a, Farrokhi S, et al. (2010) Treatment of an individual with piriformis syndrome focusing on hip muscle strengthening and movement reeducation: a case report. J Orthop Sports Phys Ther 40:103-111.
-
Martin HD, Reddy M, Gómez-Hoyos J (2015) Deep gluteal syndrome. J Hip Preserv Surg 2: 99-107.
-
McCrory P, Bell S (1999) Nerve entrapment syndromes as a cause of pain in the hip, groin and buttock. Sports Med 27: 261-274.
-
Haluk M (1999) Variations of Nerves Located in Deep Gluteal Region After that , position of the nerves with the pir- iformis was studied in main 3 groups following?: The first group is includes the cases in which su- perior gluteal nerve is passed over the piriformis an. Okajimas Folia Anat 76: 273-276.
-
Orava S (1997) Hamstring syndrome. Oper Tech Sports Med 5: 143-149.
-
Yoshimoto M, Kawaguchi S, Takebayashi T, Isogai S, Kurata Y, et al. (2009) Diagnostic features of sciatica without lumbar nerve root compression. J Spinal Disord Tech 22: 328-333.
-
Possover M, Chiantera V (2007) Isolated infiltrative endometriosis of the sciatic nerve: a report of three patients. Fertil Steril 87: 417.
-
Martin HD, Palmer IJ (2013) History and physical examination of the hip: the basics. Curr Rev Musculoskelet Med 6: 219-225.
-
Gomez-Hoyos Juan, Martin Roboy, Schroder Ricardo, Palmer Ian J, Martin HD (2015) Accuracy of two clinical tests for ischiofemoral impingement in patients with posterior hip pain and endoscopically confirmed diagnosis. Arthroscopy.
-
Prather H, Dugan S, Fitzgerald C, Hunt D (2009) Review of Anatomy, Evaluation, and Treatment of Musculoskeletal Pelvic Floor Pain in Women. PM R 1: 346-358.
-
Laycock J, Jerwood D (2001) Pelvic Floor Muscle Assessment: The PERFECT Scheme. Physiotherapy. 87: 631-642.
-
Byrd JW, Jones KS (2000) Prospective analysis of hip arthroscopy with 2-year follow-up. Arthroscopy 16: 578-587.
-
Shacklock M (2005) Improving application of neurodynamic (neural tension) testing and treatments: a message to researchers and clinicians. Man Ther 10: 175-179.
-
McHugh MP, Johnson CD, Morrison RH (2012) The role of neural tension in hamstring flexibility. Scand J Med Sci Sports 22: 164-169.
-
Ellis RF, Hing W a, McNair PJ (2012) Comparison of longitudinal sciatic nerve movement with different mobilization exercises: an in vivo study utilizing ultrasound imaging. J Orthop Sports Phys Ther 42: 667-675.
-
Khoury A, Schroder R, Gomez-Hoyos J, Reddy M, Palmer IJ, et al. (2015) The Effects of Hip Abduction on Sciatic Nerve Biomechanics during Terminal Hip Flexion. ISHA - International Meeting, Cambridge UK.
-
Sluka KA, Skyba DA, Radhakrishnan R, Leeper BJ, Wright A (2006) Joint mobilization reduces hyperalgesia associated with chronic muscle and joint inflammation in rats. J Pain 7: 602-607.
-
Cox JM, Bakkum BW (2005) Possible generators of retrotrochanteric gluteal and thigh pain: the gemelli-obturator internus complex. J Manipulative Physiol Ther 28: 534-538.
-
Ozisik PA, Toru M, Denk CC, Taskiran OO, Gundogmus B (2014) CT-guided piriformis muscle injection for the treatment of piriformis syndrome. Turk Neurosurg 24: 471-477.
-
Jeong HS, Lee GY, Lee EG, Joe EG, Lee JW, et al. (2015) Long-term assessment of clinical outcomes of ultrasound-guided steroid injections in patients with piriformis syndrome. Ultrasonography 34: 206-210.
-
Michel F, Decavel P, Toussirot E, Tatu L, Aleton E, et al. (2013) Piriformis muscle syndrome: diagnostic criteria and treatment of a monocentric series of 250 patients. Ann Phys Rehabil Med 56: 371-383.
-
Howard F (2003) Chronic Pelvic Pain. Obstet Gynecol 101: 594-611.
-
Weijenborg PT, Greeven A, Dekker FW, Peters AA, Ter Kuile MM (2007) Clinical course of chronic pelvic pain in women. Pain 132 Suppl 1: S117-123.
-
Ambegaonkar JP, Mettinger LM, Caswell SV, Burtt A, Cortes N (2014) Relationships between core endurance, hip strength, and balance in collegiate female athletes. Int J Sports Phys Ther 9: 604-616.
-
Fall M, Baranowski AP, Elneil S, Engeler D, Hughes J, et al. (2010) Guidelines - Pelvic Pain EAU Guidelines on Chronic Pelvic Pain. Eur Urol 57: 35-48.
-
Savidge CJ, Slade P (1997) Psychological aspects of chronic pelvic pain. J Psychosom Res 42: 433-444.
-
Vaarbakken K, Steen H, Samuelsen G, Dahl HA, Leergaard TB, et al. (2014) Lengths of the external hip rotators in mobilized cadavers indicate the quadriceps coxa as a primary abductor and extensor of the flexed hip. Clin Biomech (Bristol, Avon) 29: 794-802.
-
Gudena R, Alzahrani A, Railton P, Powell J, Ganz R (2015) The anatomy and function of the obturator externus. Hip Int 25: 424-427.
-
Beneciuk JM, Bishop MD, George SZ (2009) Effects of upper extremity neural mobilization on thermal pain sensitivity: a sham-controlled study in asymptomatic participants. J Orthop Sports Phys Ther 39: 428-438.
-
Bertolini GRF, Silva TS, Trindade DL, Carvalho AR (2009) Neural mobilization and static stretching in an experimental sciatica model - an experimental study. Rev Bras Fisioter 13: 2-7.
-
Kornberg C, Lew P (1989) The effect of stretching neural structures on grade one hamstring injuries. J Orthop Sports Phys Ther 10: 481-487.
-
Neumann DA (2010) Kinesiology of the hip: a focus on muscular actions. J Orthop Sports Phys Ther 40: 82-94.
-
Willcox EL, Burden AM (2013) The influence of varying hip angle and pelvis position on muscle recruitment patterns of the hip abductor muscles during the clam exercise. J Orthop Sports Phys Ther 43: 325–331.
-
Berry JW, Lee TS, Foley HD, Lewis CL (2015) Resisted Side Stepping: The Effect of Posture on Hip Abductor Muscle Activation. J Orthop Sports Phys Ther 45: 675-682.
-
Van der Heijden RA, Lankhorst NE, VAN Linschoten R, Bierma-Zeinstra SM, Marienke VAN Middelkoop M (2016) Exercise for treating patellofemoral pain syndrome: an abridged version of Cochrane systematic review. Eur J Phys Rehabil Med 52: 110-133.
-
Santos TR, Oliveira BA, Ocarino JM, Holt KG, Fonseca ST (2015) Effectiveness of hip muscle strengthening in patellofemoral pain syndrome patients: a systematic review. Braz J Phys Ther 19: 167-176.
-
O'Sullivan P (2005) Diagnosis and classification of chronic low back pain disorders: maladaptive movement and motor control impairments as underlying mechanism. Man Ther 10: 242-255.
-
Ekstrom RA, Donatelli RA, Carp KC (2007) Electromyographic analysis of core trunk, hip, and thigh muscles during 9 rehabilitation exercises. J Orthop Sports Phys Ther 37: 754-762.
-
Haugstad GK, Haugstad TS, Kirste UM, Leganger S, Wojniusz S, et al. (2006) Posture, movement patterns, and body awareness in women with chronic pelvic pain. J Psychosom Res 61: 637-644.
-
Key J, Clift A, Condie F, Harley C (2008) A model of movement dysfunction provides a classification system guiding diagnosis and therapeutic care in spinal pain and related musculoskeletal syndromes: A paradigm shift-Part 2. J Bodyw Mov Ther 12: 105-120.
-
Spitznagle TM, Robinson CM (2014) Myofascial pelvic pain. Obstet Gynecol Clin North Am 41: 409-432.
-
Fitz Gerald MP, Kotarinos R (2003) Rehabilitation of the short pelvic floor. I: Background and patient evaluation. Int Urogynecol J Pelvic Floor Dysfunct 14: 261-268.
-
FitzGerald MP, Kotarinos R (2003) Rehabilitation of the short pelvic floor. II: Treatment of the patient with the short pelvic floor. Int Urogynecol J Pelvic Floor Dysfunct 14: 269-275.
-
Barton PM (1991) Piriformis syndrome: a rational approach to management. Pain 47: 345-352.
-
Wyant GM (1979) Chronic pain syndromes and their treatment. III. The piriformis syndrome. Can Anaesth Soc J 26: 305-308.
-
Jacobsen S, Sonne-Holm S, Søballe K, Gebuhr P, Lund B (2005) Hip dysplasia and osteoarthrosis: a survey of 4151 subjects from the Osteoarthrosis Substudy of the Copenhagen City Heart Study. Acta Orthop 76: 149-158.
-
Boykin RE, Anz AW, Bushnell BD, Kocher MS, Stubbs AJ, et al. (2011) Hip instability. J Am Acad Orthop Surg 19: 340-349.
-
Henak CR, Ellis BJ, Harris MD, Anderson AE, Peters CL, et al. (2011) Role of the acetabular labrum in load support across the hip joint. J Biomech 44: 2201-2206.
-
Martin HD, Hatem MA, Kivlan BR, Martin RL (2014) Function of the ligamentum teres in limiting hip rotation: a cadaveric study. Arthroscopy 30: 1085-1091.