To evaluate the usefulness of ultrasonography as an evaluation tool in a Randomized Controlled Trial assessing Balneotherapy effects in Rheumatoid Arthritis.
A prospective controlled clinical trial, not blinded, randomly assigned of patients with rheumatoid arthritis accordingly to the American College of Rheumatology criteria. The Balneotherapy group received Balneotherapy's throughout 21 days in S. Jorge Spa. The main outcome was hand/wrist ultrasonography measured at the same moments in the two groups, and McNemar's tests were used to compare changes in ecographics signals, with a 5% statistical significance level. Secondary outcomes were taken at same time for HAQ-DI and DAS28. A moderated regression analysis, complemented with the Johnson-Neyman (J-N) technique was used to perform the statistical analysis.
In thermal group there was a statistically significant result (p < 0.05) regarding the evolution of synovitis only at left hand/wrist according to ultrasonography signals, between baseline and day 21, end of thermal treatment, and after 3 months. Curiously, the same statistical findings were found in the control group, but at right side. No difference was found in DAS28 at the end of Balneotherapy but almost reach significance at month 3. HAQ-DI at end of treatment and 3rd month follow-up was significantly improved in the Balneotherapy.
Pain and diminished function are hallmarks of RA patients, so any complementary contribution with no or mild side effects, as Balneotherapy, is welcome to enhance quality of life. In this study ultrasonography could detect improvement in synovitis in both RA patients groups, Balneotherapy translating both the possible effect of treatment and the natural history of RA. Both joints were the more affected at enrolment and the Balneotherapy had a slightly higher DAS28. Quality of life had a sustainable improvement with Balneotherapy. Ultrasonography is an objective, inexpensive modality to measure the response of RA small joint synovitis to Balneotherapy, provided that it is realized by a medical doctor with specific formation.
Rheumatoid arthritis, Balneotherapy, Ultrasonography, Synovitis, Vascularization, Quality of life, Randomized controlled trials
Rheumatoid arthritis (RA) [1,2] is a chronic systemic autoimmune disease characterized by persistent inflammation of synovial joints with pain, often leading to joint destruction and disability, and despite intensive research the cause of RA remains unknown [3].
New effective drug treatments in RA has resulted in less focus on non-pharmacological modalities, such as therapeutic exercise and balneotherapy [4-8]. Balneotherapy has been used for a very long time, even ante christum (AC), and is recognized as an important way to treat rheumatologic diseases, specially osteoarthritis [9,10]. It is called mineral baths or Balneotherapy, and uses different types of natural mineral water compositions like sulphur, radon, carbon dioxin, etc. Sukenik stated that the sulphur mineral water has special proprieties to rheumatologic diseases, including in the course of active inflammatory phases in RA [11,12]. In Portugal, respiratory and rheumatologic (mostly osteoarthritis) diseases are the most frequently ones treated by sulphur mineral waters which are more common and focused in the Northeast of the country. In some European countries and in USA, the use of radon is prohibited as well as controversial [13].
According to the recommendations of the "Haute Autorité de Santé" for RA published in 2007 [14] and Forestier, et al. [15], Balneotherapy appears to provide an analgesic and functional benefit to patients with stable or long-established and non-progressive RA (grade C). It is not indicated when RA is active (professional agreement) [15].
So whereas balneotherapy has a large use in non-inflammatory osteo-articular conditions its real benefits are not clearly known in RA [16]. To better understand and measure its effects a trial was conducted in order to compare Balneotherapy plus usual pharmacological treatment versus only pharmacological treatment. The aim of this study was to evaluate if Balneotherapy offers any benefit, using hand synovitis changes as the primary endpoint, evaluated by ultrasonography (US).
After approval by the ethics committee, patients were selected from the database of Unidade de Imunologia Clínica (UIC), Hospital Santo Antonio, Centro Hospitalar do Porto. Patients living at no more than 30 km away from the hospital were included in the study, in order to be able to attend the Balneotherapy and continue their ordinary daily life. An invitation letter was sent to patients to attend to a lecture on Balneotherapy in the hospital.
The inclusion criteria were: 18-years-old or more; definitive diagnosis of RA according to American College of Rheumatology (ACR) criteria; with an evolution equal or more than 1; functional status I-III (classification ACR-Steinbrocker [17]).
The exclusion criteria were: functional status grade IV; cognitive abnormalities (for example psychoses or senile dementia); active infection; participation in other complementary treatments.
The 44 eligible patients, after a code attribution ab initio, were stratified by age to ensure a better balance between groups and randomly assigned: Immediate thermal treatment or deferred thermal treatment [18]. All patients signed an informed consent.
The hydromineral occurrence at Balneotherapy centre (S. Jorge - 30 Km from Porto), is a chloride-rich sulphur water with sodium prevailing in the cation composition.
Most patients of the thermal group departed from the hospital, at 8 am, in a special mini-bus accredited for transportation of patients and returned to Porto (around 10.30 am) from Balneotherapy centre. The trip took about 20 minutes. Some patients preferred to take their own transport. All patients maintained their usual pharmacological treatment and kept their daily life activities, namely those who had professional jobs. Every day, the same medical hydrologist was in thermal treatments throughout all the session, adjusting treatments individually, if necessary.
During 21 days, the thermal group has received alternately the following sulphur bath treatments:
One day a collective thermal pool at 34 ℃ in groups of 8 patients, per 30 minutes-oriented by the same experienced physiotherapist. The prescription of the medical hydrologist was specific for each clinical condition, namely type of exercises for different body segments (paying attention to patient's limitations but emphasizing functioning and respiratory control) followed by 10 minutes of relaxation, including different water jets, electronically controlled, focused on the most painful body areas, always maintaining a jet distributed at safety.
The following day patients had a sulphur bath (20 minutes) at 37 ℃ plus underwater jets (10 minutes) at 38 ℃ focused on to the most painful joints and finally global steam (5 minutes) at 38 ℃. The latter two treatments were also adjusted by two experienced aquatic technicians, formerly prepared to be aware of symptoms and signs of alarm. The prescription of the medical hydrologist (jet force and temperature; area of the body) was individualized to each patient characteristics and the evolution of the disease. There was no direct massage because of the subjectivity of each therapist.
The clinical evaluation was made simultaneously for the two groups (thermal and control) at day 0 (D0) baseline, day 21 (D21) end of thermal treatment and after 3 months (M3), following a pre-established protocol: Health Assessment Questionnaire - Disability Index (HAQ-DI), Visual Analog Scale (VAS) pain, fatigue, quality of life by the patient, Disease Activity Score - 28 joints (DAS28), VAS for Global Health Assessment by the same physician who had no experience on the field of Balneotherapy, joint US (the same joints, chosen by the clinician according to pain and physical examination, in the same patient by the same experienced radiologist) and laboratory tests.
Additional information was collected, regarding to the daily pharmacological treatment, as well as complications felt during the study, filled in by the patient.
All US examinations (only hands and wrists) - were performed on the same planned day of clinical examinations (D0; D21; M3) by the same radiologist (with special interest on musculoskeletal US). US examinations were performed using a Toshiba Xario equipment and a linear transducer of 5-12 Mhz. US studies of previous clinically selected joints were done using gray scale technique and color power Doppler technique. The gray scale images were obtained in the longitudinal, transversal and oblique planes. The gray scale evaluation was used to detect synovial thickening/hypertrophy and joint effusion. A simple visual semi quantitative score system was used to estimate synovial thickening (grade 0 - absence of synovial thickening, grade 1 - Mild synovial thickening, grade 2 - Moderate synovial thickening, 3 - Severe synovial thickening). Other parameters were screened and recorded with gray scale technique like synovial cysts, tenosynovitis and rheumatoid nodules. Detection and quantification of bone erosions associated with synovitis were not performed because of long time consuming and it was not contributive to the objectives of the study. Synovitis can predict structural damage in rheumatoid arthritis [19].
Color power Doppler technique studies were done in the same joints studied with gray scale technique. The color power Doppler studies were performed in the power angio mode, using standardized parameters with low velocity scale and low wall filter, adjusted to detect slow flow. Color gain was adjusted to maximize demonstration of blood flow, while avoiding noise artifacts. The transducer was gently placed on the surface of the joint to avoid compression of superficial vessels or an artifact increase in vascular resistance caused by compression. Taking into consideration the findings on previous gray scale US examination a simple visual semi quantitative score system was also used to report color power Doppler examinations (grade 0 - absence of vascularization, grade 1 - mild vascularization, grade 2 - moderate vascularization, 3 - marked vascularization).
The outcomes were ultrasonography scores, HAQ-DI and DAS28, at the same moments in the two groups.
A blocked randomization stratified by age was use. For allocation of the participants to one of the two groups, a computer generated list of random numbers was used.
Given the characteristics of Sulphur water with particular smell, blinding of patients and therapists was not feasible. In respect to the care providers, they were not involved directly with the study nor with Balneotherapy modalities, however we can't assure that patients didn't comment anything during outpatient visits.
Analysis was performed by intention to treat. McNemar's tests were used to compare the proportion of individuals from the thermal and the control group that change ecographics signals (in terms of Synovitis and Hypervascularization). All patients were evaluated in moment zero and were reassessed after 3 weeks (moment 1) and 3 months (moment 2), in the follow-up. Statistical significance level was set at 5%. All the analyses were stratified by thermal and control group and performed in SPSS version 22.
The US results were allocated in four different categories according to the degree of US changes (0 - no synovial thickening; 1 - mild; 2 - moderate; 3 - severe synovial thickening). We decide to group in one simple category status 2 and 3 taking in account the number of the participants that reported such symptoms, so our final US are splitted in three categories.
The moderated regression analysis, complemented with the Johnson-Neyman (J-N) technique was used to perform the statistical analysis on HAQ-DI and DAS-28 results.
44 eligible patients accepted to participate in the trial: 22 participated in thermal group and 22 in control group between August 2011 and November 2011 [20].
Adherence to Balneotherapy was continuously assessed and a very good compliance of patients was achieved. There were only 3 cases of discontinued treatment due to reasons beyond the study.
Table 1 summarizes the baseline characteristics of the enrolled sample, including US findings. The groups were homogenous at baseline with regard to age, duration of disease, gender. All were Caucasian.
Table 1: Baseline characteristics of the study population. View Table 1
Concerning US monitoring of RA hand the following results were found (Table 2):
Table 2: Proportion of individuals that change US findings from D0 to D21 and D0 to M3. View Table 2
- Synovitis: In thermal group statistically significant results were found, regarding the evolution of synovitis between D0 and D21 and D0 and M3.
- Thermal patients improved their US signals regarding to left side joints. In what concerns to the right side, there was a tendency for improved results but not statistically significant. In control group, similar results were found, but curiously in the opposite sides: Statistically significant results were found, only regarding to the right side.
- Hyper vascularization: A similar analysis was performed regarding this variable, but no statistically power was found for this parameter in either group.
Table 3 and Figure 1 and Figure 2 show the values of the change scores of HAQ-DI and DAS-28 between each moment of evaluation and the baseline, with the respective 95% confidence interval (CI).
 Figure 1: Change scores of HAQ-DI (mean, 95% CI). View Figure 1
Figure 1: Change scores of HAQ-DI (mean, 95% CI). View Figure 1
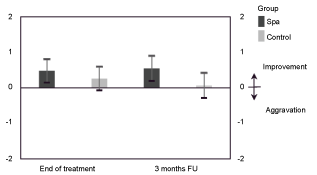 Figure 2: Change scores of DAS28 (mean, 95% CI). View Figure 2
Figure 2: Change scores of DAS28 (mean, 95% CI). View Figure 2
Table 3: Change scores on HAQ-DI and DAS-28. View Table 3
Our study has limitations, namely no blinding, impossible due to the smell associated to Sulphur waters, being recognized that is much more complex to achieve blinding in non-pharmacological trials [21,22]. The small sample size is also a limitation, although other studies regarding Balneotherapy also included low number of patients.
In 2010, Smolen, et al. highlighted the importance of synovitis detection in daily practice, and its prevention as one of the major targets of RA therapy [23]. Furthermore Dougados, et al. stated the ability of synovitis to predict structural damage in RA [19].
EULAR recommendations pointed that US may be used to detect damage at an earlier time point (especially in early RA) [24].
Whereas US allows a sensitive detection of the inflammatory soft tissue process, synovitis and tenosynovitis, it is not optimal for the detection of erosions. There is an acceptable agreement between US and Magnetic Resonance Imaging (MRI) for detection of bone erosion in patients with early RA but not conventional radiography (CR). US might be considered as a valuable tool for early detection of bone erosion especially when MRI is not available or affordable. At least in one study, US seemed to be more reliable when the disease is more active [25].
Evaluation of pannus and the extent of vascularization within the joints of RA patients by high-resolution US might be helpful in the assessment of disease activity, and thus influence therapeutic strategies [26].
Carlo Orzincolo, et al. suggested in 1998 that conventional radiography remains the standard imaging technique for joint studies in the patients with suspected RA. US is recommended to diagnose soft tissue involvement (joint effusion). CT is very useful for showing abnormal processes in complex joints (sacroiliac and temporomandibular joints and craniocervical junction) which are difficult to depict completely with conventional radiography. MRI applications include the assessment of disease activity; in particular, this technique may be the only tool differentiating synovial fluid and inflammatory pannus [27].
Erosions represent a late stage in the disease process. One of the earliest detectable changes in patients with rheumatoid arthritis is proliferation of the synovium - the rheumatoid pannus. Both US and MRI are sensitive for the detection of synovitis, and both are superior to CR [28].
Owing to the better axial and lateral resolution of US, even minor bone surface abnormalities may be depicted. Thus destructive and/or reparative/hypertrophic changes on the bone surface may be seen before they are apparent on plain X-rays or even magnetic resonance imaging.
US has a very powerful role in rheumatologic clinical practice and it is becoming the most frequently used imaging technique in evaluating patients with arthritis [29]. Furthermore, US is the least expensive of the imaging procedures [30].
The "real time" capability of US allows dynamic assessment of joint and tendon movements, which can often aid the detection of structural abnormalities. Advantages of US include its non-invasiveness, portability, relative inexpensiveness, lack of ionizing radiation, and its ability be repeated as often as necessary, making it particularly useful for the monitoring of treatment. As US is the most operator dependent imaging modality, the experience and expertise of the examiner will determine the value of the diagnostic information obtained [31]. That's why, in our study, the same radiologist physician dedicated to the muscle-skeletal field made all the evaluations (baseline and monitoring).
The results we found in this study regarding US findings are puzzling. All patients of this study had right hand preference but we found different rheumatoid involvement between right and left hands in the thermal and control groups. That could be explained by different activities, asymmetrical rheumatoid lesions evolution, asymmetric severity of the disease; etc.
Regarding activity of disease according to DAS28 with erythrocyte sedimentation rate (ESR) or C-reactive protein (CRP) [32] we observed a non-significant improvement in thermal group, but it must be emphasized, however, that the patients of this group had a mean of disease activity at baseline worse than the control group and that at month 3 the difference between groups almost reach significance.
Finally, we found significant statistical differences in quality of life, as evaluated by the HAQ-DI, in both moments of evaluation, more pronounced in month 3. We must stress that the patient lived in the real world, not in the Spa hotel facilities, so we highlight the findings at month 3, long time after the Balneotherapy.
The comments of our patients raised the possibility that these quality of life evaluations by a rigid questionnaire didn't correspond entirely to their major worries. The same concerns were found in some papers focusing about standardized or individualized measures [33,34].
Patients with rheumatoid arthritis have much to say about their own experiences along the evolution of their disease. We only stratified the patients by age, but many other variables like gender, duration of disease, functional status, medication, can still interfere in the evolution of the disease conducting to different functional limitations [35] and to different coping of the disease.
Patients didn't report any complications during the study, namely infectious diseases.
In patients with RA, where pain (physical and psychological) predominates, every gain is benefit, contributing to enhance quality of life. That's what Balneotherapy seems to have done to the patients in this study, translated by the well-being felt by the same patient along the time of the study, according to the self-reports of health-related behaviors.
More studies in RA, namely multicentre randomized controlled trials (RCT), with the same methodology, including subjective and objectives parameters of evaluation, should be carried out to validate non-drug interventions that are considered to have only marginal benefit.
Moreover, US is a cheap modality to measure the response of RA small joint synovitis to Balneotherapy, provided that it is performed by the same radiologist specialist on muscle-skeletal US.
The authors have no conflicts of interest to declare.
The study was conducted with the approval of the local Ethics Committee of Centro Hospitalar do Porto.
Thanks, all health professionals and patients who helped to transform the design study into a real one.
This research was funded by Unidade de Imunologia Clínica.