Obstetrics and Gynaecology Cases - Reviews
Collision Tumor: Dermoid Cysts and Mucinous Cystadenoma in the Same Ovary and a Review of the Literature
Mehmet S�hha Bostanci1, Ozge Kizilkale Yildirim2, Gazi Yildirim2, Murat Bakacak3, Isin Dogan Ekinci4, Sevgi Bilgen5 and Rukset Attar2*
1Sakarya University Medical School, Obstetrics and Gynecology, Turkey
2Yeditepe University Hospital, Obstetrics and Gynecology, Turkey
3Kahramanmaras S�t�� Imam University Medical School, Obstetrics and Gynecology, Turkey
4Yeditepe University Hospital, Pathology, Turkey
5Yeditepe University Hospital, Anethesiology and Reanimation, Turkey
*Corresponding author: Rukset Attar, Yeditepe University Hospital, Obstetrics and Gynecology, Istanbul, Turkey, Tel: 0902165784832/905378401900, E-mail: ruksetattar@hotmail.com
Obstet Gynecol Cases Rev, OGCR-2-031, (Volume 2, Issue 2), Case Report; ISSN: 2377-9004
Received: September 29, 2014 | Accepted: March 29, 2015 | Published: March 31, 2015
Citation: Bostanci MS, Yildirim OK, Yildirim G, Bakacak M, Ekinci ID, et al. (2015) Collision Tumor: Dermoid Cysts and Mucinous Cystadenoma in the Same Ovary and a Review of the Literature. Obstet Gynecol Cases Rev 2:031. 10.23937/2377-9004/1410031
Copyright: © 2015 Bostanci MS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Collision tumor is defined as the coexistence of two adjacent, but histologically distinct tumors without histological admixture in the same tissue or organ. Collision tumors involving ovaries are extremely rare. The coexistence of a mucinous cystadenoma with a dermoid cyst is infrequently reported. However, the most common histological combination of collision tumor in the ovary is the coexistence of teratoma with mucinous tumors. If a dermoid cyst accompanies a multiseptated cyst and if the multiseptalcyst contains fatty foci, these two components may be associated. Recognizing the potential for the coexistence of these two neoplasms in the same ovary is essential to be able to make a correct diagnosis.
Keywords
Collision tumor, Dermoid cyst, Mucinous cystadenoma
Introduction
Dermoid cyst is a type of germ cell tumor comprising well-differentiated tissues and three germ cell layers: ectoderm, mesoderm, and endoderm, which is also known as mature cystic teratom [1]. With peak incidence in females aged 20�40�years, these tumors comprise 10�20% of all ovarian neoplasms [1]. These tumors are characterized as generally slow-growing and unilateral, with a reported bilateral incidence of 10% [2]. Multiple dermoid cysts within a single ovary are rare. Benign mucinous cystadenomas account for 80% of mucinous ovarian tumors and 20-25% of overall benign ovarian tumors [3].
A collision tumor is the coexistence of two adjacent, but histologically distinct tumors without histological admixture in the same tissue or organ. Such tumors have often been reported in various organs, but location in the ovary is rare. Some other collision tumors of the ovary have been described in literature as cystadeno carcinoma and granulosa cell tumor [4], teratoma with granulosa cell tumor [5], and serous adenocarcinoma and steroid cell tumor [6]. The juxtaposition with dermoid cysts has been reported as comprising approximately 5% of benign mucinous ovarian tumors and rare examples of proliferating mucinous tumors [7].
The case is here reported of a rare collision tumor in the ovary consisting of mucinous cystadenoma and two distinct dermoid tumors.
Case Presentation
A 27-year-old G1P1 Caucasian female presented with complaints of right-side pelvic pain and a sensation of fullness in her lower abdomen. A subsequent pelvic sonography showed a complex, right ovarian cyst of approximately 8 � 4 � 4cm in size; her carbohydrate antigen (CA) 125 level was 18.1U/mL (normal, 0�25U/mL, at our hospital) and CA 19.9 was 7.4 (normal range 0�37U/mL, at our hospital). The structure appeared cystic, anechoic with several septations and appeared to be a part of the right ovary. No pathological flow was noted and no free fluid in the Pouch of Douglas was seen. The left ovary appeared unremarkable and the uterus was noted to be within normal limits. Other abdominal organs, including the liver, pancreas, kidneys, adrenals, and GI tract, appeared normal. The patient had negative cytological findings on a vaginal/cervical smear.
The patient was admitted for exploratory laparotomy. A right salpingo-oophorectomy was performed. Findings included a large simple-appearance right ovarian cyst occupying the entire right ovary with no normal residual ovarian stroma. An unremarkable left ovary, uterus, appendix, and liver were noted. The structure removed was diagnosed as a mucinous cystadenoma and 2 distinct mature cystic teratomas measuring totally 9 � 5 � 4.5 cm and weighing 345gm.
The cut surface showed multi loculated cysts filled with cheese-like material, hair, and mucin, with a tan smooth inner lining (resembling a mucosal surface) and focal tan shiny areas. It was noted that the fimbriae were fused. The final pelvic wash was found to be negative for malignant cells and positive for reactive mesothelium cells.
The specimen was examined by light microscopy with hematoxylin-eosin stain. Microscopic examination of the right ovary revealed three tumor types: mucinous cystadenoma corresponded to the wall of the two cysts; mature cystic teratoma produced the skin and subcutaneous tissue, including sebaceous glands and hair containing mass.
Approval for this case report was granted by the Institutional Ethics Committee and informed consent was obtained from the patient (Figures 1-3).
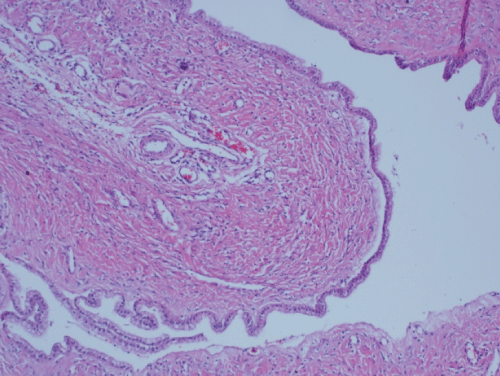
Figure 1: Mucinous cyst lined by monolayered cuboidal epithelium (H&E, x40).
View Figure 1
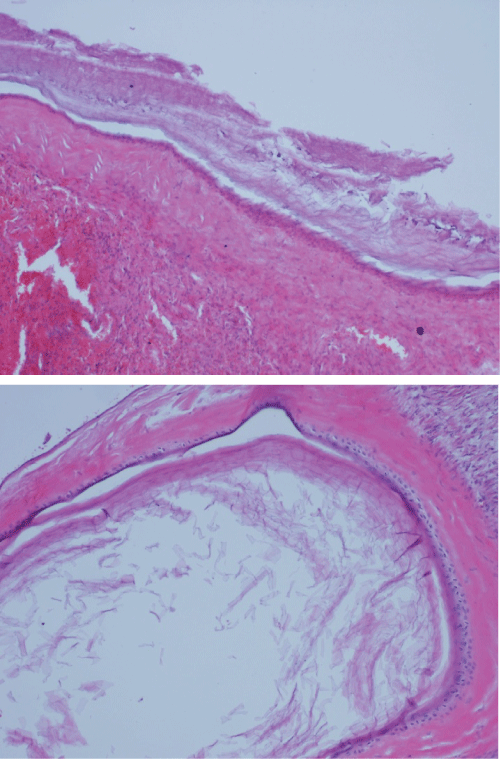
Figure 2,3: Dermoid cyst of the same ovary with squamous epithelium with keratinization (H&E, x100)
View Figure 2,3
Discussion
Ovarian neoplasms are thought to have three possible origins, surface epithelial-stromal tumors, sex cord-stromal tumors, and germ cell tumors. Germ cell tumors account for approximately 30% of primary ovarian tumors and of these 95% are mature cystic teratomas. Although mature cystic teratomas are generally unilateral, ovarian dermoid cysts may be bilateral and/or multiple in approximately 10-15% of cases. Long-term recurrence rate has also been reported [8,9]. Although rare, the possibility of additional neoplasms supervening in teratomas can be anticipated asteratomas are formed from a wide variety of ectodermal, mesodermal, and endodermal tissues. Surface epithelial-stromal tumors are classified as subgroups of serous tumors, mucinous tumors, endometrioid tumors, clear cell tumors, transitional cell tumors, and epithelial-stromal tumors. The most common mucinous tumors can be classified into 3 main categories of benign cystadenoma, borderline, and malignant. From the often large and usually cystic mucinous cystadenomas, multilocular rates have been reported as 76% and unilocular 24% [10]. Mucinous cystadenomas, which can progress to cystadeno carcinoma, are sub-divided as benign, borderline, and malignant types [11]. However, of all mucinous ovarian neoplasms, 77% to 87% are benign [10,11].
Previous reports have detailed collision tumors in several organs other than the ovary, including the esophagus, stomach, liver, lung, thyroid and kidney [12,13]. The most common histological combination of collision tumor in the ovary is the coexistence of teratoma with mucinous tumors [14,15].
Various hypotheses have been suggested regarding the formation of collision tumors. The first hypothesis is that the coexistence of two primary tumors in the same tissue is due to a �chance accidental meeting�. The second hypothesis proposed is that the presence of the first tumor creates changes in the microenvironment, engendering the development of the second primary tumor or the seeding of metastatic tumor cells. The third theory proposes that each primary tumor has its origins in a common stem cell [16].
A clear diagnosis of collision tumor can be made when normal tissue intervenes between both tumors and there is no histological admixture at the interface. However, the presence of an equivocal intermediate transitional zone between the tumors may make it more difficult to differentiate between a collision tumor and a true mixed tumor [5,12]. The histological combination of teratoma and mucinous tumors is the most common form of collision tumours in the ovary [14].
The histogenesis of ovarian mucinous cystadenoma has not yet been fully clarified. There has been the suggestion of surface epithelial metaplasia origin or a teratomatous origin. Ultrastructure studies and mucin histochemical studies have supported the surface epithelial metaplasia theory [17,18]. The frequent co-existence of mature cystic teratoma and mucinous cystadenoma is the basis for the teratoma theory.
In a study by Vang et al. ovarian mucinous tumors associated with mature cystic teratomas were seen to exhibit morphological and immunophenotypic diversity [19]. Throughout the morphological spectrum, which ranges from cystadenomatous to carcinomatous, tumors of the surface epithelial-stromal type which resemble typical primary ovarian mucinous tumors may be seen and also lower intestinal tract type tumors of the kind usually encountered as secondary or metastatic tumors in the ovary [19].
Ovarian mucinous tumors, secondary or metastatic from a lower intestinal tract tumor are more often seen. Diagnosis is usually straightforward when such cases exhibit other characteristic features of metastatic disease (bilateral ovarian tumor, nodularity with surface involvement extra ovarian tumor, morphologically similar primary tumor elsewhere) [20].
Another study published in abstract form reported molecular findings (significant allelic imbalance for microsatellite markers, indicating homozygosity rather than heterozygosity for chromosomal polymorphisms) in some ovarian mucinous cystadenomas associated with mature cystic teratomas, which were consistent with a germ cell origin [21].
Although not all mucinous tumors are of germ-cell origin, mucinous elements in dermoid cysts may be of teratomatous origin as they are more likely to be intestinal rather than Mullerian in differentiation [22]. These coexisting ovarian tumors were reported by Kin et al. as rare collision tumors, the definition of which is a tumor with 2 adjacent but histologically distinct tumors with no histological admixture at the interface [14]. However, as there is some histopathological correlation between teratomas and mucinous tumors, coexistence may not be incidental.
In a study by Fuji et al. homozygous genetic patterns similar to those of the teratomatous components were shown in mucinous tumors arising together with mature cystic teratomas, and it was suggested that these mucinous tumors developed from pre-existing mature cystic teratomas [23].Evidence of a clonal relationship could be provided by additional molecular analyses demonstrating shared genetic changes in the mucinous tumor and adjacent conventional teratomatous elements to support the theory of a teratomatous origin for these mucinous tumors.
Okada et al. demonstrated that where the dermoid cyst accompanies a multiseptated cyst and if the multiseptated cyst contains fatty foci, there may be an association between these 2 components [24]. It was also stated that the recognition of the potential for coexistence of these 2 neoplasms in the same ovary is essential to be able to make a correct diagnosis [24].
Conclusion
In conclusion, to the best of our knowledge this is the first reported case of two mature cystic teratomas coexisting with mucinous cystadenoma in the same ovary. Collision tumors involving ovaries are extremely rare entities and coexistence of tumors with varying histogenesis may be diagnosed. During the intraoperative assessment of a dermoid cyst with unusual imaging findings, the intraoperative diagnosis cannot depend solely on macroscopy. The surgeon should establish good perioperative communication with the pathologists and if possible there should be intraoperative consultation with specialized gynaecology pathologists.
References
-
Kim MJ, Kim NY, Lee DY, Yoon BK, Choi D (2011) Clinical characteristics of ovarian teratoma: age-focused retrospective analysis of 580 cases. Am J Obstet Gynecol 205: 32.
-
Caspi B, Appelman Z, Rabinerson D, Zalel Y, Tulandi T, et al. (1997) The growth pattern of ovarian dermoid cysts: a prospective study in premenopausal and postmenopausal women. Fertil Steril 68: 501-505.
-
Brown J, Frumovitz M (2014) Mucinous tumors of the ovary: current thoughts on diagnosis and management. Curr Oncol Rep 16: 389.
-
Ozbey C, Erdogan G, Pestereli HE, Simsek T, Karaveli S (2005) Serous papillary adenocarcinoma and adult granulosa cell tumor in the same ovary. An unusual case. APMIS 113: 713-715.
-
Dgani R, Rozenman D, Lifschitz-Mercer B (1993) Granulosa cell tumor arising in an ovary with mature cystic teratoma. Int J Gynaecol Obstet 41: 287-289.
-
Nirenberg A, Ost�r AG, Quinn MA (1992) Collision tumor: serous adenocarcinoma and steroid cell tumor of the ovary. Pathology 24: 60-62.
-
Ueda G, Fujita M, Ogawa H, Sawada M, Inoue M, et al. (1993) Adenocarcinoma in a benign cystic teratoma of the ovary: report of a case with a long survival period. Gynecol Oncol 48: 259-263.
-
Pepe F, Panella M, Pepe G, Panella P, Pennisi F, et al. (1986) Dermoid cysts of the ovary. Eur J Gynaecol Oncol 7: 186-191.
-
Al-Fozan H, Glassman J, Caspi B, Appelman Z, Tulandi T (2003) Lateral distribution of ovarian dermoid cyst. J Am Assoc Gynecol Laparosc 10: 489-490.
-
Tavassoli FA, Devilee P (2003) World Health Organization classification of tumours. Pathology and genetics of tumour of the breast and female genital organs. Lyon: IARC Press: 163-171
-
Mittal S, Gupta N, Sharma AK, Dadhwal V (2008) Laparoscopic management of a large recurrent benign mucinous cystadenoma of the ovary. Arch Gynecol Obstet 277: 379-380.
-
Matias-Guiu X, Caixas A, Costa I, Cabezas R, Prat J (1994) Compound medullary-papillary carcinoma of the thyroid: true mixed versus collision tumour [corrected]. Histopathology 25: 183-185.
-
Goteri G, Ranaldi R, Rezai B, Baccarini MG, Bearzi I (1997) Synchronous mucosa-associated lymphoid tissue lymphoma and adenocarcinoma of the stomach. Am J Surg Pathol 21: 505-509.
-
Kim SH, Kim YJ, Park BK, Cho JY, Kim BH, et al. (1999) Collision tumors of the ovary associated with teratoma: clues to the correct preoperative diagnosis. J Comput Assist Tomogr 23: 929-933.
-
Tang P, Soukkary S, Kahn E (2003) Mature cystic teratoma of the ovary associated with complete colonic wall and mucinous cystadenoma. Ann Clin Lab Sci 33: 465-470.
-
Brandwein-Gensler M, Urken M, Wang B (2004) Collision tumor of the thyroid: a case report of metastatic liposarcoma plus papillary thyroid carcinoma. Head Neck 26: 637-641.
-
Fenoglio CM, Ferenczy A, Richart RM (1975) Mucinous tumors of the ovary. Ultrastructural studies of mucinous cystadenomas with histogenetic considerations. Cancer 36: 1709-1722.
-
Nomura K (1995) Mucin histochemistry of ovarian mucinous cystadenomas expressing gastrointestinal characteristics. Pathol Int 45: 430-435.
-
Vang R, Gown AM, Zhao C, Barry TS, Isacson C, et al (2007) Ovarian mucinous tumors associated with mature cystic teratomas: morphologic and immunohistochemical analysis identifies a subset of potential teratomatous origin that shares features of lower gastrointestinal tract mucinous tumors more commonly encountered as secondary tumors in the ovary. Am J Surg Pathol 31: 854-869.
-
Vang R, Ronnett BM (2006) A practical approach to mucinous tumors involving the ovary: distinction of primary from metastatic tumors and prediction of site of origin for metastases of uncertain origin. Pathol Case Rev 11: 18-30.
-
Magi-Galluzi C, O�Connell JT, Neffen F (2001) Are mucinous cystadenomas of the ovary derived from germ cells? A genetic analysis. Mod Pathol 14: 140A.
-
Russel P, Farnsworth A (19987) In: Russel P, Farnsworth A, eds. Surgical Pathology of the Ovaries (2nd edn) New York: Churchill Livingstone: 273-298.
-
Fujii K, Yamashita Y, Yamamoto T, Takahashi K, Hashimoto K, et al. (2014) Ovarian mucinous tumors arising from mature cystic teratomas--a molecular genetic approach for understanding the cellular origin. Hum Pathol 45: 717-724.
-
Okada S, Ohaki Y, Ogura J, Ishihara M, Kawamura T, et al. (2004) Computed tomography and magnetic resonance imaging findings in cases of dermoid cyst coexisting with surface epithelial tumors in the same ovary. J Comput Assist Tomogr 28: 169-173.





