Pertrochanteric fractures count among the most frequent fractures in elderly persons but their vascular complications are rare. We present two cases of pseudoaneurysm following internal fixation for pertrochanteric fractures in relatively young patients aged 67 and 68-years-old. The post-operative follow up was marked by the onset of a pulsatile swelling in the inner thigh. The diagnosis of pseudoaneurysm of the deep femoral artery was made by arterio-venous Doppler-ultrasound and CT-angiography. The pseudoaneurysms were managed by open surgery for the first case and by a stent for the other one. Both of them got a good outcome.
Pertrochanteric fracture, Pseudoaneurysm, Deep femoral artery, CT angiography, Doppler ultrasound
Pertrochanteric fractures count among the most frequent fractures in elderly osteoporotic persons [1]. Due to an aging population, their incidence is increasing, and they have become the main ground for emergency consultation in trauma centres in elderly patients [2].
Their treatment comprises several internal fixations means including essentially the dynamic hip screw and proximal femoral nails. Postoperative complications affect about 20% of patients, but vascular injury caused by the trauma, during surgery or during the postoperative course, rarely occurs [2]. However, it's important to know how to recognize them to avoid life-threatening situations, especially in elderly subjects [3]. Indeed, there are an increasing number of publications on this subject [1-8] but the published studies are all about case reports and there is a lack of series up to now.
We report two cases of deep femoral artery pseudoaneurysm subsequent to an internal fixation with a dynamic hip screw plate.
A 67-year-old patient presented to emergency department for a right hip trauma subsequent to a fall from his height. Physical assessment and radiographs showed a pertrochanteric fracture. The patient underwent internal fixation with a dynamic hip screw plate the next day (Figure 1). There were no surgery after-effects and the patient were discharged after two days under low molecular weight heparin and analgesic treatment. Functional rehabilitation of the right hip was set up and partial weight bearing allowed through two axillary crutches. At three months follow up, the patient presented to outpatient department for a pulsating mass located in the right Scarpa triangle. His haemodynamic state was stable, and the pedal pulse was present. The plain radiographs found out a complete bone union. For further ascertainment, an arterio-venous Doppler-ultrasound was performed and found out a pseudoaneurysm of the deep femoral artery. The diagnosis was confirmed by a CT angiography (Figure 2), then the patient underwent a pseudoaneurysm resection. One month later, the pain was totally relieved, and the patient was able to wander through a walker. After fourteen months' follow up, there wasn't a recurrence of pseudoaneurysm, and our patient recovered his whole autonomy.
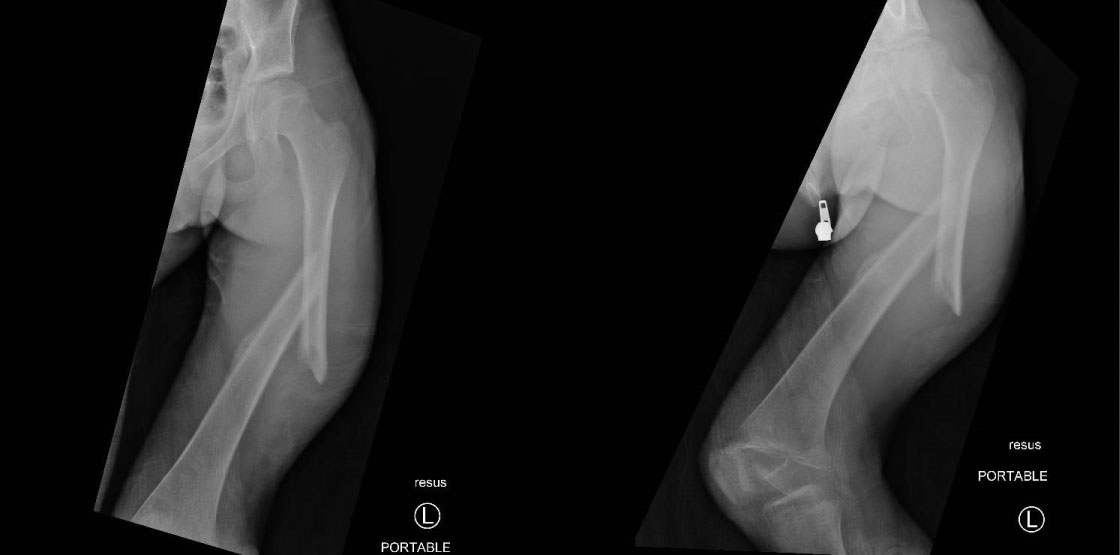 Figure 1: Pelvic X-ray showing dynamic hip screw plate used for right pertrochanteric fracture.
View Figure 1
Figure 1: Pelvic X-ray showing dynamic hip screw plate used for right pertrochanteric fracture.
View Figure 1
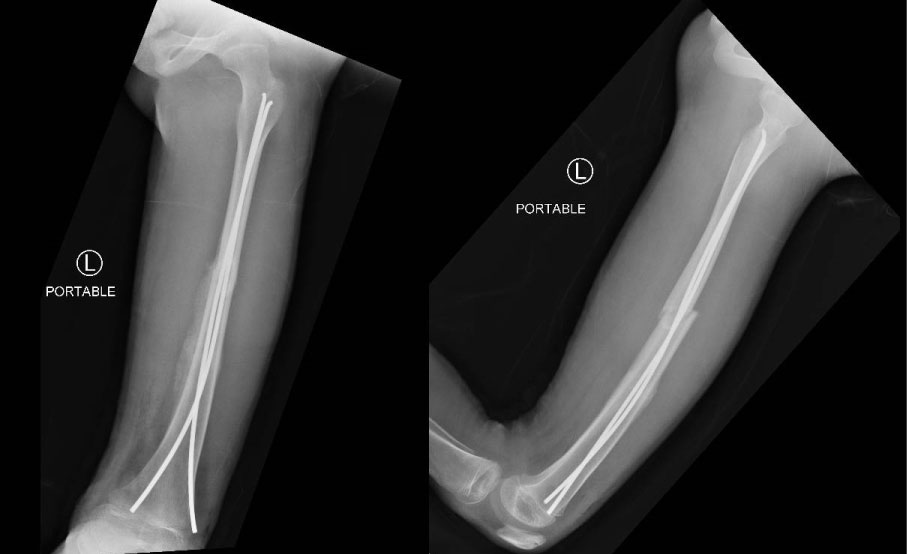 Figure 2: CT angiography showing a false aneurysm of the right deep femoral artery.
View Figure 2
Figure 2: CT angiography showing a false aneurysm of the right deep femoral artery.
View Figure 2
A 68-year-old diabetic woman presented to emergency department after a fall from her height. Imaging findings have shown a complex inter-trochanteric fracture (Figure 3). The patient underwent closed reduction and internal fixation by means of a dynamic hip screw plate (Figure 4). The fracture evolved to great trochanter non-union making the patient bedridden. This non-union was managed with decortication and band wiring (Figure 5).
 Figure 3: Pelvic X-ray showing a left pertrochanteric fracture.
View Figure 3
Figure 3: Pelvic X-ray showing a left pertrochanteric fracture.
View Figure 3
 Figure 4: Pelvic X-ray showing dynamic hip screw plate used for left pertrochanteric fracture.
View Figure 4
Figure 4: Pelvic X-ray showing dynamic hip screw plate used for left pertrochanteric fracture.
View Figure 4
 Figure 5: Pelvic X-ray showing band wiring for greater trochanter non-union.
View Figure 5
Figure 5: Pelvic X-ray showing band wiring for greater trochanter non-union.
View Figure 5
After surgery, the patient complained of a pulsating swelling located in the inner side of the thigh. Doppler-ultrasound hasn't shown any vascular abnormalities. The CT angiography revealed the existence of a pseudoaneurysm developing from the deep femoral artery (Figure 6). The patient was then referred to the vascular surgeons and got a stent. The greater trochanter achieved union after six months. After one year follow up there were neither a recurrence of pseudo-aneurysm nor other vascular complications. Our patient recovered full hip range of motion and were able to walk normally after 7 months.
 Figure 6: CT angiography showing a false aneurysm of the left deep femoral artery.
View Figure 6
Figure 6: CT angiography showing a false aneurysm of the left deep femoral artery.
View Figure 6
Pertrochanteric fractures count among the most frequent fractures in the elderly [1].
Vascular complications of these kind of fractures are extremely rare and accounts for 0.08% to 0.2%. Even if the deep femoral artery is mostly affected, in some rare cases the superficial femoral artery could be involved [3,5-8]. Duparc divided these vascular lesions into haemorrhagic ones due to sharp objects and thrombotic forms subsequent to blunt instruments [9]. Pseudoaneurysms are one of these complications [10].
These lesions are usually caused by drilling, screw insertion, sometimes to the incorrect positioning of the guide wire in nailing but can also occur because of by the fracture in itself [3].
Several mechanisms have been incriminated in their genesis:
• The irritation of the arterial wall by a pointed instrument (pin, screw, drill, retractor...) is the most reported mechanism in the literature. It's usually a technical error when positioning a too long screw or when a counter-bend or a pin slip.
• Close contact between the small, poorly synthesized trochanter and the artery may also be irritating.
• Exaggerated tractions of a curarized patient may result in the rupture of an atheroma plaque or under adventitious rupture, which will later be responsible of the artery wall embrittlement.
• Deep infections can also cause this type of complication.
• An initial post-traumatic rupture of the arterial wall cannot be ruled out.
In fact, in our second case the postoperative X-rays showed that the pins used to treat the greater trochanter non-union were too long and could puncture the deep femoral artery. This hypothesis is the most credible especially because the screws had adequate length but a drill slipping or a punch by the sharp edges of the displaced lesser trochanter cannot be discarded.
These lesions could happen at the fracture time, during reduction, internal fixation or even during rehabilitation with the mobilisation of the limb [3].
Many pseudoaneurysms are undiagnosed because they are spontaneously obliterated [10]. Some authors pinpointed the position of the distal fragment of the femur in adduction and internal rotation as a factor favouring the onset of such lesions [5].
The delayed diagnosis of this complication can be explained on the one hand by the deep localization of the artery and on the other hand by the fact that pain, anaemia and hematoma may be ascribed to the surgical procedure [1,3]. Indeed, our patients presented thigh pain and swelling several weeks before the appearance of the pulsatile mass. This could suggest that there is rather a slow increasing of the pseudoaneurysm than an acute onset.
Clinically it can present as a pulsatile mass gradually increasing in size [10]. In fact, Moreover, it can simulate a deep venous thrombosis of the lower limb when the hematoma breaks and compresses the veins. Arteriovenous Doppler ultrasonography and CT-angiography represent the key examinations in this type of pathology [3]. The therapeutic options are numerous from ultrasound guided thrombin injection, coil embolization, vascular surgery and sometimes abstention, each having good results in the literature [3].
Pseudoaneurysm of the femoral artery represents a rare complication of pertrochanteric fracture surgical fixation. Its clinical presentation must be well known by physicians. Indeed, a pulsating swelling of the thigh must raise suspicions of pseudoaneurysm and explore it further using ultrasound Doppler and CT angiography. Its treatment is easy and should be applied as soon as it is discovered to prevent life-threatening issues.
The authors declare that they have no conflict of interest.
Patients are consenting for the publication of this manuscript, including images.