Some reconstruction methods are used after distal gastrectomy, and an endoscopic approach for choledocholithiasis is restricted by the type of reconstruction. We investigated retrospectively the risk factors for post-surgical choledocholithiasis after distal gastrectomy.
Between January 2004 and December 2013, pathological stages I and II (UICC 7th edition) gastric cancer patients who received a distal gastrectomy in our hospital were retrospectively studied for the incidence and risk factors of post-surgical choledocholithiasis.
We studied 267 patients who were diagnosed with pathological stages I and II cancer and were reconstructed by the Billroth I method (147 patients) and by the Billroth II method (17 patients) and by the Roux-en-Y method (103 patients) between January 2004 and December 2013 in our hospital. Post-surgical choledocholithiasis occurred in 7 patients (2.62%), including 2 patients after the Billroth I method and 5 patients after the Roux-en-Y method. Based on univariate and multivariate analysis, the history of cholecystolithiasis, the incidence of elderly patients, and the Roux-en-Y reconstruction were found to be independent risk factors for choledocholithiasis after distal gastrectomy.
In this study, a past history of both cholecystolithiasis and Roux-en-Y reconstruction after distal gastrectomy for gastric cancer may be related to choledocholithiasis in elderly patients, especially those over 74 years of age.
Choledocholithiasis, Distal gastrectomy, Elderly patients, Roux-en-Y reconstruction
Gastric cancer is one of the most fatal neoplasms in the world, especially in eastern Asia [1,2]. For gastric cancer patients, surgery and endoscopic resection are the only curative treatments [3,4]. There are several reconstruction methods after distal gastrectomy, such as the Billroth I method, the Billroth II method, Roux-en-Y reconstruction, and jejunal interposition. The choice for each reconstruction method is decided by the policy of each department and surgeon based on the presence of esophageal reflux and the size of remnant stomach. Among these methods, the Roux en-Y reconstruction may affect the endoscopic treatment of the bile duct, gall bladder, and pancreas. On the other hand, the relation cholecystolithiasis and gastrectomy had been reported that Billroth II reconstruction was one of the risk factors of gallstone after gastrectomy. But there are few reports about risk factors of choledocholithiasis after gastrectomy.
So, we examined retrospectively the incidence and risk factors of choledocholithiasis among our gastrectomy cases.
Between January 2004 and December 2013, we retrospectively studied the pathological stages I and II (UICC 7th edition) cancer patients in our hospital who received a distal gastrectomy with lymphadenectomy for the incidence of choledocholithiasis. The patients with either choledocholithiasis or a past history of choledocholithiasis and synchronous cholangiocarcinoma were excluded. In our hospital, if cholecystolithiasis is detected at the pre-surgical examination, cholecystectomy and intraoperative cholangiography were performed with the gastrectomy, and a prophylactic cholecystectomy also was performed by an open laparotomy gastrectomy.
Patient information, such as age, gender, post-surgical pathological stage, cholecystolithiasis, cholecystectomy performed or not, reconstruction method, open gastrectomy or laparoscopic surgery, extent of lymph node dissection and observation period were recorded from the medical and surgical records. This study was approved by the Ethics Committee of Tonami General Hospital.
Characteristics of these patients were analyzed by chi-square test, Welch's t test and Mann-Whitney U test, as appropriate. The univariate and multivariate analysis of risk factors for post-surgical choledocholithiasis after distal gastrectomy were performed using the Kaplan-Meier method with the log-rank test and the Cox proportional hazards model, respectively. The cut off level of age was estimated from the ROC curve.
All P-values were two sided, and P-values of 0.05 or less were considered statistically significant. All statistical analyses were performed with EZR (Saitama Medical Centre, Jichi Medical University, Saitama, Japan), which is a graphical user interface for R (The R Foundation for Statistical Computing, Vienna, Austria, version 2.13.0) [5]. More precisely, it is a modified version of the R commander designed to add statistical functions frequently used in biostatistics.
Between January 2004 and December 2013, 748 patients were surgically treated for gastric cancer in our hospital. During this period, 418 patients received a distal gastrectomy and 271 patients were diagnosed as pathological stages I and II. There were 4 patients with past history of choledocholithiasis in the Roux-en-Y and Billroth I treatment groups. And there was one patient who had synchronous cholangiocarcinoma with gastric cancer in Billroth II reconstruction group. These 5 patients were excluded from this study. (Figure 1) The median follows up duration of the patients was 2158 days (57-4450). The characteristics of these patients are shown Table1. The Billroth I reconstruction was performed on 147 patients, and the Billroth II reconstruction was performed on 17 patients and the Roux-en-Y reconstruction was performed on 103 patients. Age was significantly older in Billroth II group than other groups. And pathological stage was also significantly higher in Billroth II group than other groups. And patients with D2 dissection were significantly more in the Billroth II group. There were no significant differences in other patient characteristics of three groups.
 Figure 1: Flow diagram for patient selection. View Figure 1
Figure 1: Flow diagram for patient selection. View Figure 1
Table 1: Characteristics of patients. View Table 1
The median duration in the incidence of choledocholithiasis after surgery was 723 days (201-2039). Four of the 7 patients were over 80-years-old at the time that the choledocholithiasis was detected. Four patients (Billroth I: two, Roux-en-Y: two) were treated with endoscopic lithotomy with 1 patient (Roux-en-Y) receiving surgical lithotomy, and 2 patients (Roux-en-Y) were observed because they had no symptoms (Table 2).
Table 2: Patients with post-surgical choledocholithiasis and subsequent treatment. View Table 2
The cut off for age calculated by the ROC curve analysis was over 74 years of age (Figure 2). The difference in the incidence of post-surgical choledocholithiasis was statistically significant in the cholecystolithiasis group for the elderly patients in the Roux-en-Y reconstruction group based on the Kalpan-Meier curve with log-lank test (Table 3, Figure 3a, Figure 3b and Figure 3c). The risk factors for post-surgical choledocholithiasis after distal gastrectomy were estimated by a cox regression analysis. A history of cholecystolithiasis (HR 21.01 p < 0.01), age (HR 15.24 p = 0.017), and Roux-en-Y reconstruction (HR 9.257 p = 0.021) were identified as the risk factors for post-surgical choledocholithiasis after distal gastrectomy (Table 4).
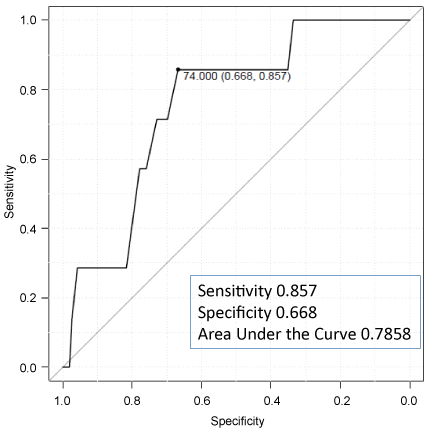 Figure 2: Estimated cut-off value (74-years-old) based on the ROC curve. View Figure 2
Figure 2: Estimated cut-off value (74-years-old) based on the ROC curve. View Figure 2
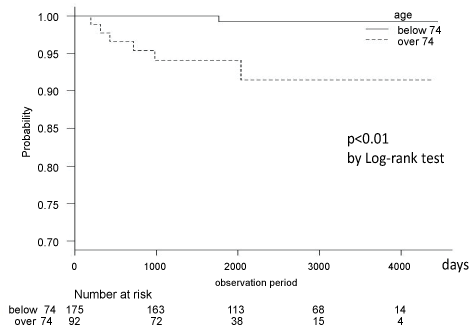 Figure 3a: Kaplan-Meier Curve for the incidence of post-surgical choledocholithiasis with over 74-years-old patients and below 74-years-old patients. View Figure 3a
Figure 3a: Kaplan-Meier Curve for the incidence of post-surgical choledocholithiasis with over 74-years-old patients and below 74-years-old patients. View Figure 3a
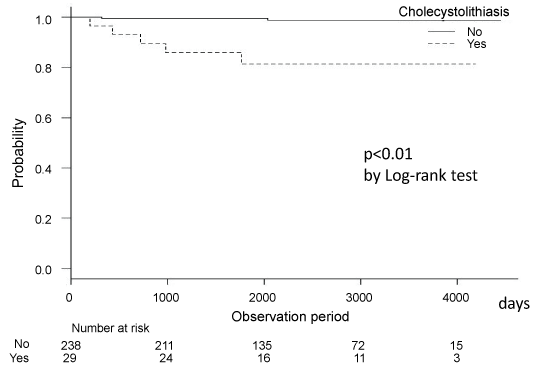 Figure 3b: Kaplan-Meier Curve for the incidence of post-surgical choledocholithiasis with the Billroth I reconstruction and the Roux-en-Y reconstruction. View Figure 3b
Figure 3b: Kaplan-Meier Curve for the incidence of post-surgical choledocholithiasis with the Billroth I reconstruction and the Roux-en-Y reconstruction. View Figure 3b
 Figure 3c: Kaplan-Meier Curve for the incidence of post-surgical choledocholithiasis in patients with and without a history of choledocholithiasis. View Figure 3c
Figure 3c: Kaplan-Meier Curve for the incidence of post-surgical choledocholithiasis in patients with and without a history of choledocholithiasis. View Figure 3c
Table 3: Patients with post-surgical choledocholithiasis and subsequent treatment. View Table 3
Table 4: Multivariate logistic regression analysis of the risk factors for post-surgical choledocholithiasis by the Cox hazard model. View Table 4
The number of elderly patients with gastric cancer is increasing [6]. In Japan, the incidence of gastric cancer in patients over 80 years of age is about 20%, and for those over 75 years of age the rate is about 35% [7]. The incidence of choledocholithiasis and cholecystolithiasis is also increasing with age [8].
Endoscopic resection for gastric cancer using endoscopic mucosal resection (EMR) and endoscopic submucosal dissection (ESD) is increasing due to the early detection of gastric cancer with endoscopy and newly developed techniques for endoscopic resection [3,9]. Gastrectomy with regional lymph node dissection is still the conventional treatment. Some reconstructions following distal gastrectomy are used, such as the Billroth I method, Billroth II method, Roux-en-Y method, and jejunal interposition. The Billroth I method is a physiological and simple reconstruction and does not require surgery to the biliary tract. The Roux-en-Y reconstruction is safer for the anastomosis and advantageous for reflux esophagitis, but it is time consuming because of the anastomosis at two sites and the difficulty in reaching the biliary tract by endoscopy. The Billroth II method has been performed less than these two methods because of the risk of occurrence of remnant gastric cancer [10]. The Billroth II method is performed on a limited number of patients for specific reasons, such as very advanced stage cancers and advanced age of the patients. The Billroth I and Roux-en-Y methods are frequently used after distal gastrectomy in Japan. As time passes, the main reconstruction method after distal gastrectomy in our hospital has been changing from the Billroth I method to the Roux-en-Y method. There are now more patients with choledocholithiasis reconstructed by the Roux-en-Y method following distal gastrectomy. One of the reasons for this change is that cholechocholithiasis is increasing along with the aging population.
The relation between reconstruction type and cholecystolithiasis has been reported in several studies [11,12]. In these reports, Billroth II reconstruction is risk factor of cholecystolithiasis after gastrectomy. The mechanisms of lithogenesis are change of cholecystokinin secretion and bacterial flora of duodenum due to exclusion of the duodenum during reconstruction [13,14]. Roux-en-Y reconstruction is also non-physiological reconstruction such as Billroth II reconstruction in terms of the tract of food. But there have been few reports on the reconstruction method and the occurrence of choledocholithiasis so far, and this was revealed in this study.
The extent of lymph node dissection with transection of the hepatic branch of the vagus nerve promotes the occurrence of cholecystolithiasis after gastrectomy [15]. In this study, there are more D2 dissections in the Billroth II group than that in the Billroth I and Roux-en-Y group. But there were no patients with post-operative choledocholithiasis only in the Billroth II group. And there were 2 patients with post-surgical choledocholithiasis in the D2 group and 5 patients in the D1+ group. There were not statistically significant differences between post-surgical choledocholithiasis and the extent of lymph node dissection.
Prophylactic cholecystectomy is not recommended in the Japanese guideline of gastric cancer treatment [16]. But in our hospital, we routinely perform prophylactic cholecystectomy with open and laparoscopic gastrectomy and cholecystectomy for cholecystolithiasis. The presence of choledocholithiasis is checked during surgery with direct cholangiography in the cholecystectomy cases.
The influence of cholecystectomy on choledocholithiasis is not clear. The patients with cholecystolithiasis detected at the pre-surgical examination tend to develop choledocholithiasis in this study.
Another problem is that it is difficult to perform an endoscopic lithotomy of the common bile duct after reconstruction by the Roux-en-Y method [17]. Some reports describe the treatment of choledocholithiasis by a balloon type enteroscopy after the Roux-en-Y reconstruction [18-20], but this procedure is not yet performed widely. The same issue occurs with bariatric surgery. There is the opinion that if cholecystolithiasis exists, cholecystectomy during gastric bypass should be performed and if cholecystolithiasis develops after the surgery, a cholecystectomy should also be performed [21].
There are some limitations in this study. This study is a retrospective, single site, small-scale study. And selection bias of reconstruction method exists, and characteristics of patients of each group in this study were not matched. Therefore, the number of patients in the Billroth II group was much smaller than in the other groups, and it is possible that accurate evaluation could not be made in Billroth II patients. Thus, a multicenter and larger scale study is needed to further investigate this problem.
We found that Roux-en-Y reconstruction following distal gastrectomy for gastric cancer may cause choledocholithiasis in elderly patients. Other types of reconstruction may be preferable for elderly gastric cancer patients.
Y. A., M.S. and N.O., designed the study and completed the major part of this manuscript. Y. A., M.S., S H, H.S., K Y, M.K., K I, and K.K. were all responsible for operations and treatments. All authors read and approved this final manuscript.
Ethics Committee of our institute was obtained.
The authors have no conflict of interest to disclose.