Schistosomiasis is a parasitic illness caused by blood flukes known as schistosomes. Infection is caused by freshwater exposure in endemic areas (Africa, Middle East, South America, Caribbean, East Asia). Little damage is caused by the flukes themselves, but rather by the eggs which lead to a TH-2 mediated immune response leading to granuloma formation and scarring. Intestinal schistosomiasis generally causes abdominal pain, poor appetite, diarrhea, and bloody stools [1,2].
Here we report a case of a 38-year-old Puerto Rican female with HIV who presented with intestinal schistosomiasis causing rectovaginal fistula. This mimicked Crohn's disease with multiple ulcerations throughout the rectosigmoid and schistosoma eggs on histologic pathology.
The patient is a 38-year-old Puerto Rican female who presented to the hospital with nausea, vomiting, and bloody diarrhea for 6 months. She was found to have multiple complications related to her advanced HIV disease (CD4 count 19) including central nervous system toxoplasmosis, deep venous thrombosis, and pulmonary embolism.
Physical examination revealed left lower quadrant abdominal tenderness and a 1 cm friable mass 2 cm from the anal verge on rectal examination. CT scan revealed wall thickening of the terminal ileum consistent with Crohn's disease and findings suggestive of rectovaginal fistula (Figure 1).
 Figure 1: Fistulization at the iliopectineal line extending into the vagina (arrow). View Figure 1
Figure 1: Fistulization at the iliopectineal line extending into the vagina (arrow). View Figure 1
Colonoscopy was performed confirming a 1-2 cm rectovaginal fistula and grossly inflamed mucosa with aphthous ulcerations and the patient was given a diagnosis of Crohn's disease. She eventually became septic and was taken for a diverting loop ileostomy. Biopsies taken during this procedure revealed Schistosoma eggs within the muscularis mucosa of the rectum (Figure 2) and the Infectious Disease service was consulted and subsequently started the patient on a course of praziquantel. The patient eventually showed improvement from her fistula with antiparasitic medications in conjunction with advancement flaps and fistula plug placement.
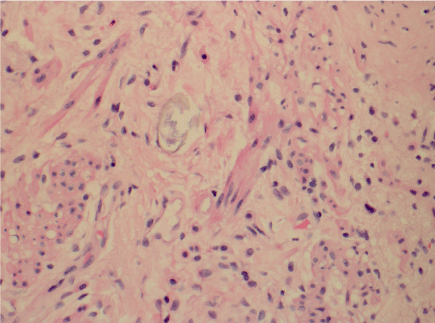 Figure 2: Rectal mucosa with refractile ovoid structures compatible with Schistosoma eggs within muscularis mucosa. View Figure 2
Figure 2: Rectal mucosa with refractile ovoid structures compatible with Schistosoma eggs within muscularis mucosa. View Figure 2
Schistosomiasis is a parasitic disease cause by blood flukes called schistosomes. Schistosomiasis can cause significant disease and usually affects individuals living in endemic areas with recurrent exposure but can also cause disease with brief exposure. While rare in North America, the World Health Organization considers schistosomiasis to be second only to malaria in socioeconomic impact of parasitic diseases worldwide [3,4]. Schistosomes have a complex life cycle with snails as an intermediate host and humans as their definitive host. The flukes infect humans by penetrating their skin after contact in fresh water. They then migrate through blood and lymphatics to the heart and lungs and eventually reach the liver where they mature to adults. Adult flukes can then migrate to various organs depending on species, including the intestines and bladder from which they are shed. Endemic areas include Africa, the Arabian Peninsula, East Asia, Puerto Rico, and areas of the Nile Valley. Infection is rare in the United States because it lacks the snail intermediate host and infections found within the US come from immigration and travelers [1].
While adult worms do little damage to the host, schistosomal eggs cause a TH-2 mediated immune response leading to significant inflammation and granuloma formation. This can lead to numerous chronic compilations including intestinal, hepatic, pulmonary, neurologic, and urinary disease.
Intestinal schistosomiasis typically is due to S. mansoni infection and presents with abdominal pain, poor appetite, and diarrhea and can lead to intestinal polyps, ulceration, strictures, and obstruction [4]. Schistosomiasis resembling inflammatory bowel disease was first reported by Mynors in 1954 who suggested that schistosomal disease could be the cause for all "regional ileitis" [5].
A rectovaginal fistula is an abnormal connection between the vagina and rectum. While the majority of rectovaginal fistulas are the result of obstetric trauma, other common causes include complex hysterectomies, radiation, and inflammatory bowel disease [6]. Simple fistulas can be repaired with excision of the fistula tract and primary repair of the rectum and vagina. Other treatment options include advancement rectal flap and fistula plugs. Advancement flap repair is accomplished by creating a flap of rectal mucosa, submucosa, and internal sphincter fibers which is then used to cover a cored-out fistula tract. An alternate surgical approach is a perineal proctectomy followed by layered closure. Other repair options include the use of bioabsorbable plugs to occlude the tract.
Crohn's disease (CD) is a chronic intestinal disease that is diagnosed clinically. It can occur at any point of the gastrointestinal tract, but the most common site is the terminal ileum. The most common feature of CD is chronic diarrhea; other symptoms include abdominal pain, fatigue, anemia or vitamin deficiencies, and anorectal disease including fistulas. Perianal fistulizing CD occurs in up to 25% of patients and can indicate a more severe clinical course. Other subtypes of CD include structuring and penetrating [7].
Multiple cases have been reported of schistosomiasis presenting with intestinal fistulizing disease suggestive of Crohn's disease [8-10] but this represents the first case seen in the US.
Chronic schistosomiasis commonly affects the sigmoid colon and rectum and usually presents with abdominal pain, diarrhea, bleeding, or ulcerations. Given its location of infection, it can also lead to anal fistulas, fissures, or abscesses. While rare in the United States, this disease process must be included in the differential diagnosis for anal and rectal fistulas especially amongst those from or who have traveled to endemic areas. It is important to obtain tissue biopsies so that the diagnosis can be confirmed by the presence of ova.