International Journal of Respiratory and Pulmonary Medicine
The Use of Independent Lung Ventilation for Unilateral Pulmonary Hemorrhage
Ajit A. Sarnaik*
Children's Hospital of Michigan, Detroit, MI and Wayne State University, USA
*Corresponding author: Ajit A. Sarnaik, M.D, Critical Care Medicine, Children's Hospital of Michigan, 3901 Beaubien Ave, Detroit, Michigan 48201, USA, Tel: 313 745-5629, Fax: 313 966-0105, E-mai: lasarnai@med.wayne.edu
Int J Respir Pulm Med, IJRPM-2-013, (Volume 2, Issue 1), Case Report; ISSN: 2378-3516
Received: January 07, 2015 | Accepted: February 05, 2015 | Published: February 08, 2015
Citation: Sarnaik AA (2015) The Use of Independent Lung Ventilation for Unilateral Pulmonary Hemorrhage. Int J Respir Pulm Med 2:013. 10.23937/2378-3516/1410013
Copyright: © 2015 Sarnaik AA. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Independent Lung Ventilation (ILV) has been used in the critical care setting as a rescue therapy for differential lung disease. The purpose of anatomic separation of the lungs is to prevent blood, purulent secretions, or other debris from one lung from contaminating the other lung. Physiologic separation of the lungs allows different ventilator strategies to be applied to each lung. We report the case of the successful use of ILV in a man with congenital heart disease with severe right sided pulmonary hemorrhage in which the left lung was relatively disease-free. By use of high-pressure �open-lung� strategies applied to the right lung and moderate settings on the left lung, we were able to achieve recruitment of the right lung without over-distention and injury to the left lung. ILV can be considered in the critical care setting in patients with respiratory failure involving widely differential disease between the two lungs.
Keywords
Independent lung ventilation, Acute respiratory distress syndrome, Congenital heart disease, Respiratory insufficiency, Pulmonary hemorrhage
Case Report
A 22 year old man with a history of truncus arteriosus requiring several surgeries since infancy presented with chest pain and hemoptysis. He had undergone surgery one month prior to repair an aneurysmal graft from a previous aortic valve replacement. Computed tomography showed anterior mediastinal hematoma and right pleural hemothorax. His clinical condition deteriorated, and he required intubation and mechanical ventilation.The predominant source of bleeding was his right lung. Upon cardiac catheterization, all systemic vessels to the right lung were coil embolized. Gas exchange was suboptimal despite the application of escalating peak inspiratory pressures up to 45 cm H2O and mean airway pressures up to 25 cm H2O and 100% oxygen. Results of a representative arterial blood gas were pH 7.19 PaCO2 61 mmHg, PaO2 62 mmHg, and SaO2 87% on 100% oxygen. Extracorporeal Membrane Oxygenation (ECMO) was considered, but contraindicated because of the risks of anticoagulation. Because of the differential requirement of pressure needed to recruit and ventilateeach lung, and the high airway pressure needed to tamponade the right lung, a double lumen endotracheal tube was placed in the left mainstem bronchus for Independent Lung Ventilation (ILV). The occlusive balloon was inflated in the left mainstem to anatomically separate ventilation to the lungs, and each lumen was connected to a separate ventilator. Optimal placement of the side lumen oriented towards the right mainstem was confirmed by bronchoscopy daily. The differential disease is shown in the chest x-ray on the first day of ILV (Figure 1). During the three days of ILV, the less affected left lung was ventilated with conventional mechanical ventilation with a PEEP of 10cm H2O and apeak inspiratory pressure of 35cm H2O to achieve tidal volume of approximately 25 ml. These moderately high settings applied to the less affected lung were required because of the patient's obese body habitus. The right lung was first ventilated with conventional mechanical ventilation with a PEEP of 18 cm H2O and peak inspiratory pressure of 35 cm H2O, initially achieving close to zero tidal volume.Airway pressure release ventilation with a PEEP-high of 25cm H2O and a PEEP-low of 8cm H2O was used subsequently to increase the mean airway pressure for tamponade effect. Fraction of inhaled oxygen to both lungs was 1.0. Adequate gas exchange was achieved with those settings: a representative arterial blood gas from those three days was: pH 7.27, PaCO2 49 mmHg, and PaO2 68 mmHg. After two days of high mean airway pressure, tidal volumes from the right lung increased from zero to 100ml after he was changed back to conventional mechanical ventilation. Modest evidence of recruitment and air Broncho grams are shown on the chest x-ray on the third day of ILV (Figure 2).
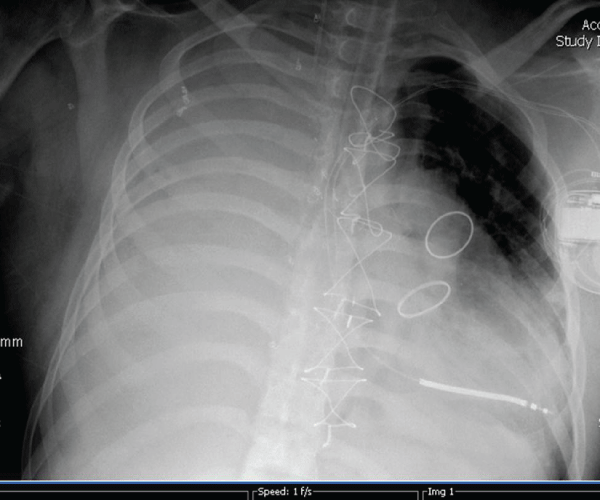
Figure 1: Differential disease is demonstrated during the first day of ILV.
There is right-sided pulmonary hemorrhage, and the left lung is relatively
free of airspace disease. The double-lumen endotracheal tube is seen in the
left bronchus. ILV is achieved with the balloon inflated in the left mainstem
bronchus and the �eye� of the proximal lumen oriented towards the right
mainstem bronchus.
View Figure 1
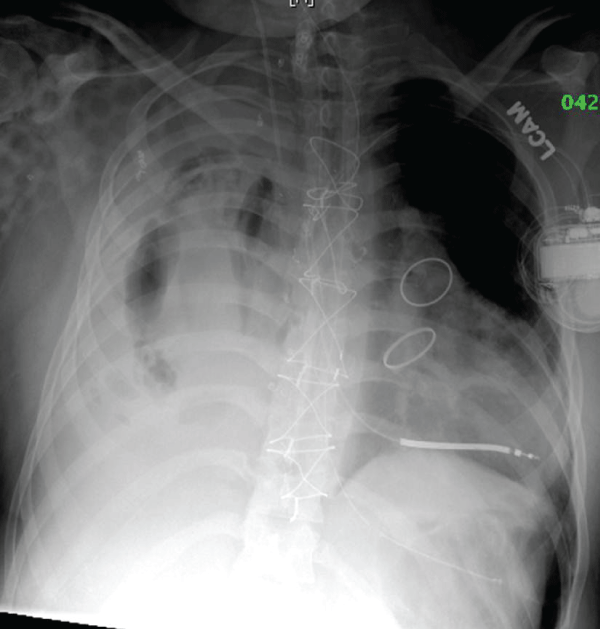
Figure 2: Modest evidence of recruitment and air bronchograms are demonstrated on the third day of ILV.
View Figure 2
Hemopneumothorax is also visible in the right lung, but it improved without evacuation four days later (Figure 3). After his right lung was recruited, he was changed back to a single lumen endotracheal tube, and managed with conventional mechanical ventilation. His respiratory status improved, but eventually developed further pulmonary hemorrhage, multiple organ failure and septic shock from coagulase negative staphylococcus infection.He eventually died of a recurrent massive pulmonary hemorrhage.
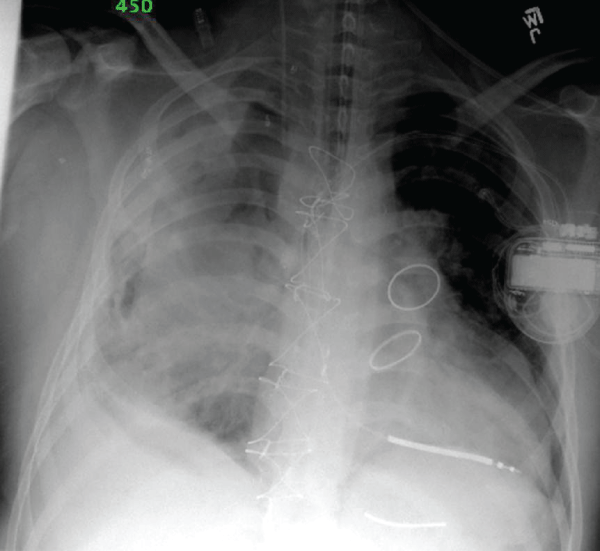
Figure 3: Further evidence of lung recruitment and partial resolution of hemopneumothorax during the seventh day of ILV.
View Figure 3
Discussion
Independent Lung Ventilation (ILV) was first described in anesthesia practice in 1931, and for the next several decades, it was mostly used for thoracic surgery procedures. In 1978, Carlon described the use of ILV in the critical care setting in cases of inhomogeneous distribution of pathologic abnormalities in the two lungs [1]. It has since been used to manage asymmetric parenchymal lung disease, pulmonary hemorrhage, single lung transplant, unilateral airway obstruction, and bronchopleural fistula [2]. In this case, ILV served the dual purposes of anatomic and physiologic separation of the lungs.
The goal of anatomically separating the two lungs is to avoid contamination of the healthy lung with blood, lavage fluid, or purulent secretions [3]. Indications for this technique in the ICU setting include massive hemoptysis [4], whole lung lavage techniques [5], and protection from interpulmonary aspiration [3]. In this patient, the balloon of the double lumen Carlens tube was inflated in the left mainstem bronchus to prevent contamination of the right lung with residual blood [6]. A definitive approach was also taken to identify and embolize the sources of bleeding by catheterization, as previously described [7]. Lung resection was considered [8], but the patient was not likely to survive the prolonged operation due to adhesions from multiple past thoracic surgeries.
Physiologic separation of the lungs allows application of different ventilator strategies to lungs with different pathophysiologic lesions. This strategy has been described in managing pulmonary contusion, single lung aspiration pneumonitis, pulmonary hemorrhage [3,9,10], complications of single lung transplants [11], and Broncho pleural fistula [12]. Two general categories of pulmonary pathophysiology are diseases of low pulmonary compliance and diseases of high airway resistance.Diseases of low compliance include ARDS, pulmonary hemorrhage, pulmonary edema, and pneumonia.These illnesses are characterized by stiff, high elastance lungs with low functional residual capacity and fast pressure equilibration across the airways.Evidence based guidelines for ARDS management include high PEEP, low tidal volume, and high rate [13]. A healthy lung subjected to these settings would lead to over-distention, decreased compliance, and increased tissue work. Over-inflation also leads to increased areas of West Zone 1 ventilation where alveolar pressure exceeds pulmonary arterial and pulmonary venous pressure, causing dead space ventilation, increased pulmonary vascular resistance, and decreased pulmonary static compliance [14]. Diseases of high airway resistance include asthma, bronchiolitis, and chronic obstructive pulmonary disease.These illnesses are characterized by dissipation of applied inflation pressure in the upper airways (low dynamic compliance), slow pressure equilibration across the airways, small airway collapse, and air trapping.Ventilator strategies for diseases of increased resistance include low rate, long expiratory time, high peak inspiratory pressure to overcome proximal airway resistance, and PEEP to prevent airway collapse [15]. A healthy lung subjected to these settings would result in over-inflation, excessive tidal volumes, and the risk of pneumothorax.
In the present case, the stiff right lung was ventilated with an �open-lung strategy� including high PEEP, low tidal volume, and high rate, as well as airway pressure release ventilation. A limitation of this case is the modest evidence that ILV helped the patient substantially improve. However, this approach may have aided lung recruitment and minimized the progression of acute lung injury. Also, the high mean airway pressure may have helped to tamponade any residual bleeding. The patient's clinical condition was grave enough to warrant consideration for ECMO, yet he improved while receiving ILV without ECMO.
There is only one known previous report on the use of ILV to treat pulmonary hemorrhage from a complication of congenital heart disease. In 2014, Murkute et al. reported an 8 year old with palliated congenital heart disease who developed bleeding from the endotracheal tube and infiltrates on radiography [16]. ILV was used to apply pressure controlled ventilation to the affected lung and volume control ventilation to the healthier lung. Although infiltrates were present, the affected lung was open.Our case carried a higher level of severity, indicated by total radiographic opacification and complete anatomic de-recruitment of the affected lung.
ILV is a potential therapy to physiologically separate the lungs in patients with differential ventilatory requirements in each lung, or to anatomically separate the lungs to prevent contamination of the healthier lung with blood, pus, or lavage fluid. Because of the relative rarity of these indications, the benefit of this therapy will not likely be proven in a randomized trial. Therefore, careful patient selection and consideration of alternatives is essential.
Acknowledgments
Ajit A. Sarnaik, MD prepared analysis of the case, literature search, and prepared and revised the manuscript. There are no financial or non-financial disclosures, nor any conflicts of interest.
References
-
Carlon GC, Ray C Jr, Klein R, Goldiner PL, Miodownik S (1978) Criteria for selective positive end-expiratory pressure and independent synchronized ventilation of each lung. Chest 74: 501-507.
-
Anantham D, Jagadesan R, Tiew PE (2005) Clinical review: Independent lung ventilation in critical care. Crit Care 9: 594-600.
-
Ost D, Corbridge T (1996) Independent lung ventilation. Clin Chest Med 17: 591-601.
-
Shivaram U, Finch P, Nowak P (1987) Plastic endobronchial tubes in the management of life-threatening hemoptysis. Chest 92: 1108-1110.
-
Smith GB, Hirsch NP, Ehrenwerth J (1986) Placement of double-lumen endobronchial tubes. Correlation between clinical impressions and bronchoscopic findings. Br J Anaesth 58: 1317-1320.
-
CARLENS E (1949) A new flexible double-lumen catheter for bronchospirometry. J Thorac Surg 18: 742-746.
-
Shigemura N, Wan IY, Yu SC, Wong RH, Hsin MK, et al. (2009) Multidisciplinary management of life-threatening massive hemoptysis: a 10-year experience. Ann Thorac Surg 87: 849-853.
-
Andrejak C, Parrot A, Bazelly B, Ancel PY, Djibre M, et al. (2009) Surgical lung resection for severe hemoptysis. Ann Thorac Surg 88: 1556-1565.
-
Wendt M, Hachenberg T, Winde G, Lawin P (1989) Differential ventilation with low-flow CPAP and CPPV in the treatment of unilateral chest trauma. Intensive Care Med 15: 209-211.
-
Cinnella G, Dambrosio M, Brienza N, Giuliani R, Bruno F, et al. (2001) Independent lung ventilation in patients with unilateral pulmonary contusion. Monitoring with compliance and EtCO(2). Intensive Care Med 27: 1860-1867.
-
Gavazzeni V, Iapichino G, Mascheroni D, Langer M, Bordone G, et al. (1993) Prolonged independent lung respiratory treatment after single lung transplantation in pulmonary emphysema. Chest 103: 96-100.
-
Baumann MH, Sahn SA (1990) Medical management and therapy of bronchopleural fistulas in the mechanically ventilated patient. Chest 97: 721-728.
-
(2000) Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. The Acute Respiratory Distress Syndrome Network. N Engl J Med 342: 1301-1308.
-
West JB, Dollery CT, Naimark A (1964) Distribution of Blood Flow in Isolated Lung; Relation to Vascular and Alveolar Pressures. J Appl Physiol 19: 713-724
-
Sarnaik AP, Daphtary KM, Meert KL, Lieh-Lai MW, Heidemann SM (2004) Pressure-controlled ventilation in children with severe status asthmaticus. Pediatr Crit Care Med 5: 133-138.
-
Murkute A, Angadi U, Jain P, Sharique T, Hegde R (2014)Paediatric pulmonary haemorrhage: Independent lung ventilation as effective strategy in management. Indian J Crit Care Med 18:694-696.





