Magnetic resonance imaging (MRI) can reliably detect inflammation and structural changes in sacroiliac joints (SIJs) in patients with lower back pain (LBP). However, patients with LBP are usually referred for MRI of the lower back (e.g. lumbar spine LS), and imaging of the SIJs is rarely requested for these patients. The aim of this work is to use radial MRI as an additional screening technique for SIJ pathology presenting in lumbar spine patients with chronic LBP.
One hundred one (54 males/47 females) patients complaining primarily of LBP were screened using a 1.5-T MRI system. MRI scanning was performed using sagittal and axial T2-weighted sequences for the LS (12 min) and the radial T2-weighted-fat saturated sequence for the SIJs (1.20 min). Two radiologists specializing in musculoskeletal MRI individually evaluated the SIJ images for anatomical accuracy and pathology.
Almost all radial SIJ images (95%) were diagnostically acceptable for reporting; 73.3% showed LS pathology only, whereas 26.7% displayed a combination of LS and SIJ pathology. Secondary findings indicate a significant correlation with gender (p = 0.014), namely, females were more prone to SIJ disease than males.
Radial images were used to detect the presence and size of the anatomical deformity in LBP patients. Patients with detected pathology were then recommended for further follow-up and full diagnostic examination.
The sacroiliac joints (SIJs) are a significant source of chronic lower back pain (LBP). However, because the clinical signs of SIJ-related pain are similar to those observed in other structures (e.g., muscle, ligaments, and discs), SIJs are frequently not considered in the clinical diagnosis [1]. In addition, early sacroiliitis is often not visible on conventional radiographs (X-ray) or is difficult to interpret, which may lead to a long delay in establishing a diagnosis (more than eight years between the initial presentation and diagnosis) [2,3]. For most patients, back pain symptoms are nonspecific. Anatomically, the spine is the leading source (82%) of LBP; however, clinicians need to be aware of the possibility of non-spinal pain generators, such as the hips and SIJs, as they are significant sources in 25% of LBP cases [4,5].
Among the available imaging techniques, magnetic resonance imaging (MRI) plays an important role in the diagnosis of sacroiliac disorders [1]. MRI is an examination that decreases the delay between the initial presentation of symptoms and diagnosis because it can detect inflammation at early stages [6,7]. The development of MRI technology has undoubtedly exceeded expectations in the last decade and has been boosted by advances in high-field magnet and computer technology [8]. However, MRI can take a long time when multiple body regions are scanned; on average, imaging of the lumbar spine (LS) requires 20 to 45 min, depending on the region being scanned [9]. Routine sequences for SIJs will increase the scanning time by a factor of two, depending on the imaging planes and the region scanned. Orthogonal and oblique planes are the most commonly used conventional anatomical planes, and a full scan of two or three of these planes can take from 15 to 35 min [9,10].
Fortunately, the multi-planar capability of MRI is not limited to standard anatomical planes. Radial sections, which are obtained perpendicular to anatomical surfaces in a fraction of the time, provide true cross sections that differ from those provided by conventional planes [10]. Radial imaging is not a new technique; it is utilized in clinical settings (e.g., MR of cholangiopancreatography) [11]. However, for musculoskeletal (MSK) imaging, radial imaging was first introduced by Munk, Holt, Helms, & Genant [12] and Quinn, Brown, & Szumowski [13], who used this technique to examine the shoulder and knee, respectively. In addition, more recently, radial sections were used by Hitt & Van Meel [14] and Petchprapa, Dunham, Lattanzi, & Recht, [10], whose findings were consistent in terms of the benefit of using this technique in certain MSK applications.
Fundamentally, standard MRI shows anatomy through axial, coronal or sagittal planes [10,13]. Conversely, radial MRI provides a unique anatomical perspective with respect to the standard, which is especially convenient when imaging is a challenge due to the anatomical location or conjunction (Figure 1). This is important for diagnosis, as it allows for better localization of the pathology and provides different anatomical views of the anatomy. According to Vleeming, et al. [15], in the average adult, the SIJs have an auricular C- or L-shaped configuration. The SIJs lie obliquely at an angle to the sagittal plane; when standing, the S1 part of the joint is mainly vertical, and its surface runs oblique and sagittal from cranio-lateral to slightly caudo-medial [16]. The mean angle of the auricular surfaces ranges between 40º, 25º, and 10º. This variation indicates that the SIJs have an irregular shape that would need to conform to the routine slice positioning; however, in radial imaging, slice positioning is able to some extent to accommodate the shape of the SIJs.
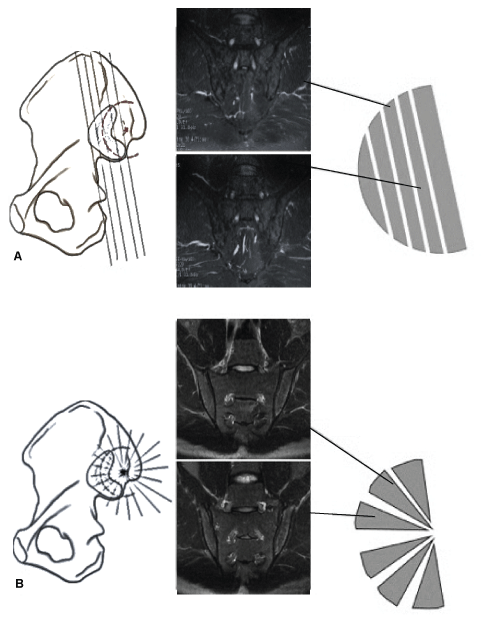 Figure 1: Comparison between the radial and routine MRI planning for image acquisition. Left panel: (A) routine slices in the coronal plan; B) radial planning of the slice circumference depends on the angle set by the operator (our study used a 6º angle). The illustration of each side of a half circle indicates the effect each positioning technique on the resulting images. For example, (A) shows images that follow a straight sequential path covering the SIJ; (B) shows the radial images of the joint in which each slice is identical to the previous slice. When the image is sliced in the coronal, sagittal, or axial plane, the size of each section and the proportions will vary. However, the mid-coronal, mid-sagittal, and mid-axial planes in the radial images (which pass through the joint at or near its center) maintain roughly comparable proportions. This aspect is important for diagnosis as it allows for better localization of pathology and provides different anatomical viewpoints of the anatomy. This figure was adapted from a published illustration [5]. View Figure 1
Figure 1: Comparison between the radial and routine MRI planning for image acquisition. Left panel: (A) routine slices in the coronal plan; B) radial planning of the slice circumference depends on the angle set by the operator (our study used a 6º angle). The illustration of each side of a half circle indicates the effect each positioning technique on the resulting images. For example, (A) shows images that follow a straight sequential path covering the SIJ; (B) shows the radial images of the joint in which each slice is identical to the previous slice. When the image is sliced in the coronal, sagittal, or axial plane, the size of each section and the proportions will vary. However, the mid-coronal, mid-sagittal, and mid-axial planes in the radial images (which pass through the joint at or near its center) maintain roughly comparable proportions. This aspect is important for diagnosis as it allows for better localization of pathology and provides different anatomical viewpoints of the anatomy. This figure was adapted from a published illustration [5]. View Figure 1
This work focused on the use of radial MR screening for SIJs in the LS of patients. The goals of this study were (1) To evaluate whether radial MRI reliably detects SIJ abnormalities, (2) To assess whether radial MRI screening is an option that benefits patients with chronic LBP due to SIJ pathology and (3) To provide patients with better prognosis that does not require unnecessary repeat MR-LS follow-up examinations.
This study was conducted in the imaging department of a general government hospital from March to June 2016. The government (i.e., Ministry of Health) and the institutional review board approved the study, and written informed consent was obtained from all patients.
In all, 101 patients, 54 males (mean age, 44.25) and 47 females (mean age, 48.10), were scanned in this study. The inclusion criteria for this study were recurrent chronic LBP and pain radiating to the hips and/or lower limbs. Patients with no clinical reason for an MRI evaluation, who had already received a LS and/or SIJ MRI from an outside institution/facility, who had generalized contraindications to MRI scanning that included but were not limited to retained metal (e.g., pacemakers, aneurysm clips, and deep brain stimulators), and who had a history of lower back or SIJ surgery were excluded. Patients who were eligible for this study were screened using a questionnaire that collected information about their physical pain and lifestyle activities, as well as a past history of pain and treatment procedures. LBP was defined for this study as the presence of at least four of the five following characteristics: Insidious onset before the age of 40 years, persistence for at least 12 weeks or longer, association with morning stiffness, improvement with exercise, and night pain [17].
The MRI screening was performed using a 1.5-Tesla General Electric (GE) Optima MR450w system (GE, Shuwaikh, Kuwait). Patients were scanned in the supine position using a GEM Posterior Array coil with the necessary positioning pads placed under the knees. The MRI scanning protocol included a routine LS examination, with the additional designed radial SIJ sequence (a few additional sagittal and axial SIJ images were obtained for anatomical comparisons only). Routine LS scanning included a T1-weighted (T1-W) spin echo (SE) and a T2-W fast SE (FSE) sequence in both the axial and sagittal planes (12-min scan time), as shown in Table 1. Scanning of the SIJs involved the use of a T2-W FSE radial MRI sequence with fat suppression (FS). In this sequence, the slices were centered on the middle of the L5 vertebral body using sagittal LS images for reference, with slice 1 in the coronal oblique position and the following 14 slices rotated incrementally. The coronal oblique images were placed parallel to the length of the sacrum, along with two FS slabs: Oe positioned inferior to the region of interest, and one frontally through the bowel and anterior abdominal wall to minimize the effect of motion artifacts during breathing and internal movements. The field of view (FOV) was set at 26 cm, and the matrix was set at 288 × 224. A section thickness of 5 mm at 6º intervals was chosen because the curvature of the SIJs can vary from 2-18º (which remains debatable) between the articular surfaces of the sacrum and the ilium bones [5]. The other parameters were as follows: Repetition time (TR), 3400 ms; echo time (TE), 102 ms; flip angle 20º; scanning time, approximately 1:20 min (Table 1). Additional scanning features for improving spatial resolution, reducing scanning time and limiting artifacts included the following: Flow compensation (FC), no phase wrap (NPW), extended dynamic range (EDR), tailored radiofrequency (TRF), auto-calibrating reconstruction (ARC), and zero-interpolation filling (ZIP 512), which are further explained in the discussion.
Table 1: Summary of the sequences and technical parameters used in the present study. View Table 1
Radial MRI can be very effective diagnostically (e.g., reduced scanning time, high-resolution images); however, MRI involves several technical factors that can either enhance or worsen the diagnostic value of a sequence. When using specific scanning features of an MRI system, some features have their own specifications and limitations. For example, when using the FC, this technique will provide the advantage of intra-voxel dephasing reduction, which improves the uniformity of blood signals and reduces cerebral spinal fluid (CSF) flow effects [18]. Although saturation bands were used in the sequence to help compensate for CSF and vascular pulsation, FC can enhance T2-W images to further compensate for CSF flow and vascular motion. The drawbacks of using FC include potentially limiting the FOV or slice thickness for a given TR. This was resolved in the radial sequence as it utilizes an FOV of 26 slices with a thickness of 4 mm. Moreover, NPW, which is a scanner option that permits imaging without aliasing, was used to prevent wrapping artifacts [18]. The drawback of using this technique is that the number of excitations (NEX) is reduced to improve efficiency, which eventually reduces the signal-to-noise ratio (SNR) and the overall resolution. For further compensation to maintain a proper NEX value and improve imaging efficiency, both ARC and ZIP were added. ARC is a generalized auto-calibrating, partially parallel acquisition that reduces imaging time [18]. ZIP allows images to be obtained artificially at a higher matrix size. EDR was added to increase the dynamic range of the receiver amplifier [18]. Failure to use EDR may result in over ranging and the production of halo artifacts. Finally, a TRF option was included; TRF changes the shape of an RF pulse such that its magnitude varies with time to create a suitable slice-selective pulse [18].
All images were examined for bilateral or unilateral bone or ligament SIJ disease. Two radiologists (with five and four years of experience in MSK imaging, respectively) identified and reviewed any abnormalities within the images. For each patient, MR image sets were anonymized, and images from the same patient were read in two separate sessions at least 6 weeks apart to reduce rater bias. The radiologists independently scored the images and were blinded to patient identity and clinical, laboratory and radiological data. Radiological abnormalities were broadly categorized into structural changes and disease activity. Structural changes were evaluated at the hyaline cartilage, subchondral bone, bone marrow, ligaments and joint space. The acute or chronic nature of the disease was indicated as the presence or absence of hyper intense T2-W MRI signals. Radial MRI scans were scored according to image quality (image contrast, resolution, and artifacts). Agreement between both MRI readers with respect to activity and structural changes was analyzed by cross tabulation using both percent agreement and kappa statistics (unweighted Cohen's kappa); statistical analyses were performed using Wizard software (Mac OS X 10.10 Inc. Chicago, USA).
A total of 101 patients were assessed. All patients had LS-related pathology (the most common pathologies were disc herniation and bulging). Seventy-five (73%) patients only presented with a LS abnormality (29 females and 45 males; mean age, 46 ± 14 years; range, 16-79), whereas twenty-six patients (26%) were diagnosed with a combination of LS and SIJ pathology (17 females and 9 males; mean age, 48.1 ± 14 years; range, 28-79), as shown in Table 2. Chronic changes were most frequently encountered in SIJ patients (16% of the SIJ patients). As shown in Figure 2A, some cases showed significant bilateral chronic changes (grade 3 and 4 on the right and left, respectively) in the form of irregular articular margins and dense sclerosis involving > 90% of the left iliac portion and approximately 40% of the superior right iliac segment of the SIJ.
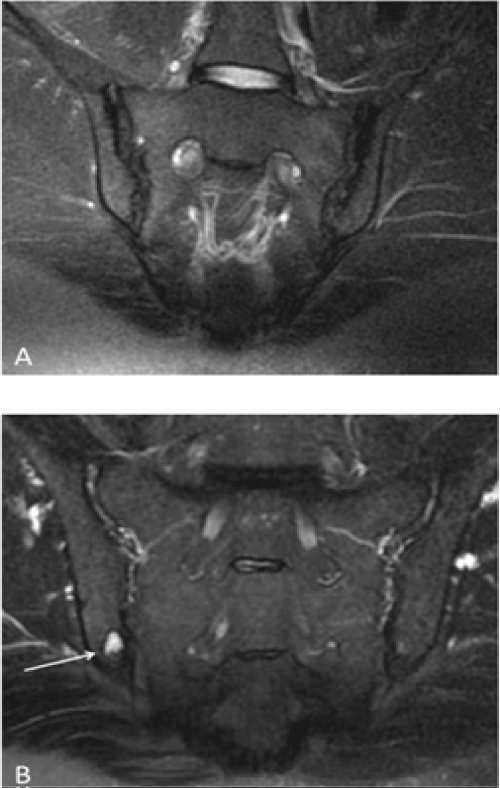 Figure 2: A) A 40-year-old female presented with LBP radiating to the left lower limb. The figure shows a radial T2-W FS image of the SIJ (the loss of signal on the left [large arrow] is greater than the loss on the right side [small arrow]) shows chronic changes in the form of irregular articular margins and dense sclerosis, which were more extensive on the left side (grade 3) than on the right (grade 2); B) A 54-year-old male presented with LBP radiating to both lower limbs; radial MRI of the SIJs revealed a focal area of sclerosis involving the inferior articular margin of the right iliac bone with well-defined erosion and active subchondral edema (arrow). View Figure 2
Figure 2: A) A 40-year-old female presented with LBP radiating to the left lower limb. The figure shows a radial T2-W FS image of the SIJ (the loss of signal on the left [large arrow] is greater than the loss on the right side [small arrow]) shows chronic changes in the form of irregular articular margins and dense sclerosis, which were more extensive on the left side (grade 3) than on the right (grade 2); B) A 54-year-old male presented with LBP radiating to both lower limbs; radial MRI of the SIJs revealed a focal area of sclerosis involving the inferior articular margin of the right iliac bone with well-defined erosion and active subchondral edema (arrow). View Figure 2
Table 2: MRI findings of all abnormalities found in the LS and SIJs. Data are shown as the percentage, 95% CI, standard deviation (SD) and (n). View Table 2
Radial MRI scans were evaluated according to signal changes within the SIJs. Normally, the SIJ space has a symmetric and homogeneous signal intensity in all sequences. An atypical signal intensity pattern of the joint space includes an intermediate signal on T1-W images and a high signal on T2-W and PD images [19]. Examples of focal, high T2-W signal changes are shown in Figure 2B and were confined to the inferior portion of the articular margin of the right iliac bone, indicating a focal area of subchondral edema and erosion. The high T2-W signal suggested active disease. Generally, most incidences of SIJ abnormalities were evident on the radial MRI scans and were depicted as abnormal signal changes within the joint and surrounding bone.
The percentage of reader agreement was calculated as 81%, and the kappa test results (presented in Table 3) show very good agreement for most SIJ abnormalities. However, the confidence interval (CI) for the kappa value showed a wide range. This range could be due to the small sample size, but some researchers [20] have calculated kappa values for small sample sizes (e.g., 5); however, the CIs for these studies are likely to be wide, resulting in "no agreement" within the CI.
Table 3: Observer agreement in the evaluations of SIJ abnormalities using MRI. Cohen's kappa values are shown with their 95% CIs. View Table 3
Radial MRI scans of the SIJs were evaluated technically according to the following diagnostic image quality factors: Signal resolution, image contrast and artifacts. Approximately 95% of the images were scored as either very good (4) or excellent (5) in image quality. The radiologists could identify anatomical features of the SIJs and surrounding structures (hyaline cartilage, subchondral bone, bone marrow, ligaments and joint space). Signal and image contrast of both normal and abnormal anatomical structures were observed in most images, and a diagnosis was obtained from all images, although some images received low ratings. Lower image scores (5%) were recorded due to a low signal-to-noise ratio (SNR), blurring, and faulty fat saturation; however, these images remained diagnostically acceptable for reporting.
Secondary findings did not reveal significant correlations between SIJ pathology and age, the presence of LS pathology, or screening characteristics (i.e., weight, childbirth, job, and pain level). However, the results showed a significant correlation with gender (p = 0.014); females were more prone to SIJ pathology than males. Predictive statistical analysis was applied, revealing that males and females aged from 41 to 42 yrs. would have the highest risk for acute back pain, and the risk was higher for females (< 188) than males (< 165).
The objective of this study was to determine whether radial MRI is useful as an additional screening technique for visualizing SIJ pathology in patients with chronic LBP. The aim of this work was not to override the value of conventional MRI of the SIJ but to provide a method for screening SIJs in patients who are frequently referred for MRI LS scans and do not display an improvement after treatment. We hope that the information obtained in this study will help raise awareness among clinicians and technicians regarding the impact of subtle changes to MRI scanning routines for future patient management. To the best of our knowledge, this study is the first to evaluate SIJs using radial MRI in patients referred for lower back MRI examinations. However, the radial imaging technique has been successfully used to evaluate different anatomical regions, such as the shoulder [12], knee [13] and hip [10,14].
In general, MRI is more frequently used as a screening tool in oncology, DW or whole-body imaging. In addition, the cost-benefit relation between screening and its impact on the health of the screened subjects remains to be investigated [21]. In our study, we have suggested a different approach for the screening technique using a fast scanning protocol without adding substantially to the time or cost of the examination.
MRI is undeniably able to visualize SIJ pathology through a routine study protocol, on T2-W-SE-FS images, or after the administration of contrast during T1-weighted FS [22]. Nevertheless, these protocols are usually performed as a standalone examination or upon the specific request of the referring clinician or radiologist, as they can be time consuming (3-30 min). Our preliminary results from 101 SIJs in 25% of subjects suggest that the radial MRI technique is feasible and capable of visualizing both the normal anatomy and pathological changes without increasing the actual examination scan time (< 1:20 min).
Furthermore, the identification of the significant pain generator(s) in patients with LBP remains one of the greatest challenges for a spine specialist [4,23]. MRI can reliably detect inflammation and structural changes, but it can only do so in the region of interest being scanned, which is further controlled by the presenting symptoms and/or clinical examinations. Additionally, according to some researchers [23], not all findings on imaging studies can be identified as generators of pain. A patient can be fully diagnosed with LS abnormalities; however, over time and with age, they may develop further complications, such as in the hip or SIJs, resulting in symptoms similar to LS pathology [4]. Approximately one-sixth of patients with LBP show structural changes in at least one SI joint [24], indicating that MRI might be a useful tool that could be expanded further as a screening technique in these cases.
According to Flynn, Smith and Chaou [25], the number of lumbar MRIs in the United States is growing at an alarming rate, despite evidence that it is not accompanied by improved patient outcomes. The global point prevalence of LBP is reported to be 9.4% (95% CI 9.0 to 9.8) [26]. Based on data from a previous report [27], LBP is a growing problem among younger Kuwaitis, with a similar result to that of our study, in which age was a factor in LBP and females were more likely to have the condition than males. Additionally, MRI of the LS constitutes 30% of the routine imaging load in our hospital. Thus, when used appropriately, MRI is an important component of patient care. The clinical application of MRI should aim to reduce inappropriate or over imaging, decrease costs and time, and improve patient outcomes. As shown in the present study, the use of radial imaging for SIJ screening detected SIJ abnormalities (observed in 25% of our patients with LS pathologies), indicating the utility of this new sequence in redirecting clinician care toward using MRI as a more cost-effective screening technique. Patients that are being re-scanned for LS pathology who do not present improvements after treatment can benefit from radial MRI screening, as the findings can suggest other approaches for patient management.
Radial imaging can be subjected to the same common artifacts (e.g., motion, flow, and wrap) that occur in routine scans. It is also exposed to the sequence-specific "cross-talk" artifact, which appears as a hypointense bar-shaped area overlying the superior and/or inferior aspect of the sacrum and iliac bones. This artifact can be explained as follows: All radial imaging planes go through the center of the joint, partially exciting the area of intersection by each selective RF pulse. After the first image is obtained, each successive image includes spins that have already been partially saturated, which affects the contrast in the center of the FOV and results in the appearance of an area of low signal intensity known as a cross-talk artifact [10,16,28]. The width of a cross-talk artifact is related to the space between sections; the closer the sections are, the broader the artifact. We have found that obtaining sections at 6º intervals while increasing the FOV to 26 allowed the cross-talk artifact to be present out of the region of interest. We also recommend that in clinical practice, an advanced MRI specialist with knowledge of system specifications and artifact minimization should plan the radial MRI sequence. Furthermore, regarding the comparisons between routine/conventional SIJ MRI and the radial sequence, we have collected several images in conjunction with the radial scans for demonstrative reasons only, as the intention of this work was not to replace the routine protocols but to screen for pathology as an additional sequence within the LS protocol (Figure 3). A comparison of both sets of images for the 101 patients would have been advantageous; however, time is an issue, and we were not able to perform this comparison in the present study.
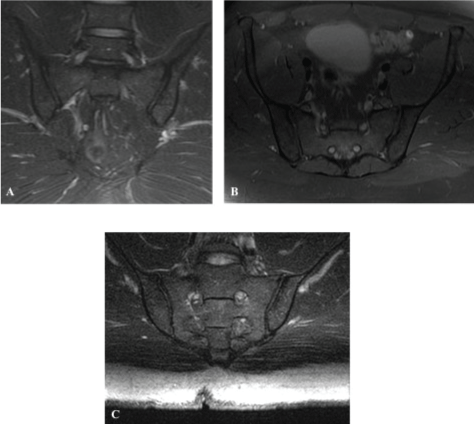 Figure 3: A) Conventional coronal; (B) Axial PD W images and (C) Radial MRI T2-W FS images of the SIJ. These images are used for comparison between routine/conventional SIJ MRI and the radial sequence and were used for demonstrative purposes only, as the intention of this work was not to replace the routine protocols but to screen for pathology as an additional sequence within the LS protocol. View Figure 3
Figure 3: A) Conventional coronal; (B) Axial PD W images and (C) Radial MRI T2-W FS images of the SIJ. These images are used for comparison between routine/conventional SIJ MRI and the radial sequence and were used for demonstrative purposes only, as the intention of this work was not to replace the routine protocols but to screen for pathology as an additional sequence within the LS protocol. View Figure 3
The proposed protocol demonstrated the feasibility of attaining multi-planar radial MRI of the SIJs using currently available commercial scanners within a 1.20-minute scan, which provided sufficient anatomical coverage and valuable diagnostic information. This protocol has the potential for rapid and reliable screening for the presence and size of anatomical deformities and the activity of disease afflicting the SIJs. The findings of this study do not negate the importance of conventional, routine SIJ scans; however, radial MRI represents a useful tool for assessing SIJ pathology as an additional screening technique for the LS of patients with chronic LBP. Although this study included conclusions obtained from 101 patients, we recommend that further screens should be performed in a different regional hospital with a larger cohort of patients to explore the diversity of this sequence in additional patients using different MRI scanners.
I thank Mr. Sam Thekkel and Mr. Akmal Ismail for their assistance.
This work did not receive funding from any agency in the public, commercial, or not-for-profit sectors.
The authors have no conflicts of interest to declare.
1. Guarantor of integrity of the entire study, Dr. M. AlMulla
2. Study concepts and design, Dr. M. AlMulla & Dr. V. Babu
3. Literature research, Dr. M. AlMulla
4. Clinical studies, Dr. M. AlMulla, Dr. V. Babu, & Mr. A. Abdullah
5. Experimental studies/data analysis, Dr. M. AlMulla, Dr. V. Babu & Dr. W. Mohammed
6. Statistical analysis, Dr. M. AlMulla, & Dr. V. Babu
7. Manuscript preparation, Dr. M. AlMulla, Dr. V. Babu, & Mr. A. Abdullah
8. Manuscript editing, Dr. M. AlMulla, & American journal Experts AJE.