There is controversy regarding which reconstructive technique provides the best outcome in acute rupture of the distal biceps tendon. Our study demonstrates the safety and efficacy of using a combined endobutton and tenodesis screw technique through a single anterior incision.
Over a Four year period, 25 consecutive patients underwent distal biceps reconstruction using this technique. Three patients were lost to follow-up leaving 22 patients for review. Mean follow-up was 24 months (6-51). All patients were evaluated using a questionnaire, clinical examination, x-rays, power measurements, and Oxford Elbow (OES) and Mayo scores.
There were no re-ruptures, fractures or hardware-related complications. Overall 95% of patients (21/22) were satisfied and rated their experience as excellent or good. Mean time to return to work was 100 days (0-280) and mean time requiring pain relief was 23 days (1-56). 55% returned to sport at their pre-injury level. One case developed heterotopic calcification and there were 3 cases of superficial infection. Mean OES and Mayo scores statistically improved from 18 (6-37) to 43 (24-48) and from 48 (5-95) to 95 (80-100) respectively (p < 0.00001).
We describe a safe and reliable technique that produces excellent clinical and functional outcomes and allows an early return to function, with no re-ruptures and a low complication rate.
Distal biceps, Endobutton, Biotenodesis screw, Acute rupture
The incidence of rupture of the distal biceps tendon appears to be increasing [1]. Acute rupture usually occurs in men in the fourth to sixth decade, in the dominant arm with a higher incidence in smokers [2]. It is thought to be a result of excessive eccentric tension as the arm is passively extended with force.
Patients usually describe a tearing or popping sensation felt at the front of the elbow. Clinical findings include swelling, bruising and tenderness in the antecubital fossa. A palpable gap, emptiness in the fossa and pain on palpation of the distal tendon with weakness of resisted supination are all signs suggestive of injury. Provocative tests include the biceps squeeze test and the biceps hook test; both tests have been reported to have a sensitivity and specificity of up to 100% [3,4]. It is suggested that patients lose 20-30% of their flexion strength and 40-50% of supination strength after this injury [5]. Those patients that find this loss of function unacceptable are listed for surgery after counselling of the potential risks.
If there is continued doubt as to the integrity of the tendon, ultrasound or magnetic resonance imaging (MRI) have been shown to be useful adjuncts with one study suggesting a sensitivity of 100% in the MRI reporting of full thickness distal biceps tears [6].
Numerous repair techniques have been reported [7-12] but no one specific technique has been shown to be superior to others. In our unit we employ the 'Distal Biceps Button™' (Arthrex, Inc, Naples, Florida) tension slide technique, which utilizes a titanium endobutton and a tenodesis screw implanted with a single anterior incision as described by Rios, et al. [13].
In this case series we report the clinical, radiological and functional outcomes of patients who underwent repair of an acute rupture of the distal biceps tendon.
Over a four year period (April 2009 to May 2013), 25 consecutive patients with acute ruptures of the distal biceps tendon underwent surgery using the distal biceps button tension slide technique by 3 fellowship trained shoulder and elbow surgeons. Follow up was undertaken at 2 weeks, 6 weeks, 3 months, 6 months and 1 year. Data was prospectively collected as patients underwent clinical and radiological follow up together with recording satisfaction and functional elbow outcome scores (Oxford Elbow Score - OES - and Mayo Elbow Score). Patients were reviewed by clinical examination specifically the hook test and plain radiograph to ensure appropriate deployment of the endobutton as a test of gross failure or re-rupture. Flexion power was calculated objectively with an electronic tensiometer. Supination strength was measured by comparing the injured side to the unaffected side. The patient shoulder was adducted to neutral and elbow flexed to 90 degrees while shaking hands with patients asking them to forcefully supinate with full force and then comparing to contralateral side. All patients were specifically asked when they returned to work, driving and whether they returned to full sporting activities at their pre-injury level.
Patients that had completed questionnaires, functional scores with clinical and radiological follow up were included in our study. Exclusion criteria included revision procedures or if any additional procedure had been performed to the elbow at the time of surgery. 3 patients were lost to follow up and there were no exclusions leaving 22 patients available for review. Mean follow up was 24 months (range 6-51).
All procedures were carried out by specialist (Consultant) elbow surgeons. A single curvilinear incision is made in the antecubital fossa with a proximal lateral and distal midline limb (the "lazy S incision"). A modified anterior Henry approach is undertaken using the interval between pronator teres and brachioradialis muscles. Careful superficial dissection is necessary to protect the lateral antebrachial cutaneous nerve (LABCN) from inadvertent damage.
Further dissection distally reveals a series of veins (the so-called leash of Henry) and the recurrent branches of the radial artery that usually require ligation or coagulation. The bicipital tuberosity is optimally exposed with the arm in maximal supination and extension; a radial retractor is placed around the tuberosity and the footprint is debrided of any remaining tendon and a 2.7 mm bicortical guidewire is inserted 30 degrees ulnar to reduce risk to the posterior intraosseous nerve. A 7.5 mm cannulated tenodesis drill is then used to drill the near cortex only.
The end of the ruptured tendon is retrieved, debrided and whipstitched using a Fiberwire suture (Arthrex, Inc, Naples, Florida) ready for placement in the osseous tunnel. The suture ends are placed individually through the Biceps Button™, which is then passed into the tunnel using a dedicated introducer, passed beyond the far cortex and then deployed such that the button comes to lie flush against the outer cortex. The suture ends are then pulled away from the hole, forcing the tendon to be pulled into the hole (Figure 1, Figure 2 and Figure 3).
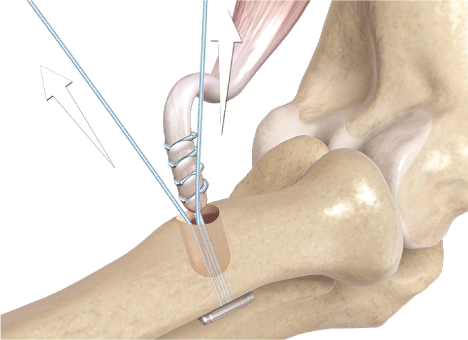 Figure 1: One limb of the suture is placed through the tendon with a mayo needle and tied.
View Figure 1
Figure 1: One limb of the suture is placed through the tendon with a mayo needle and tied.
View Figure 1
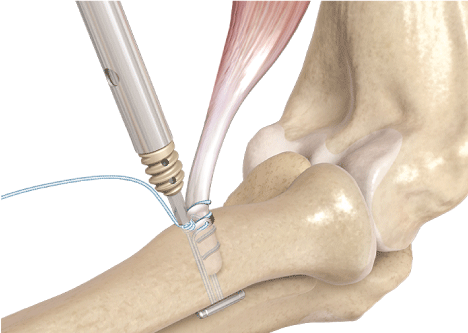 Figure 2: One limb of the suture is then placed through the tenodesis screwdriver and a 7 Ø 10 mm PEEK interference screw is then inserted into the tunnel ensuring the tendon is captured fully.
View Figure 2
Figure 2: One limb of the suture is then placed through the tenodesis screwdriver and a 7 Ø 10 mm PEEK interference screw is then inserted into the tunnel ensuring the tendon is captured fully.
View Figure 2
 Figure 3: The sutures are tied off, the wound is irrigated thoroughly and closed.
View Figure 3
Figure 3: The sutures are tied off, the wound is irrigated thoroughly and closed.
View Figure 3
Patients are placed into a sling postoperatively but are allowed to perform full active range of movement immediately without any loading of the biceps, under the supervision of a physiotherapist. A graduated strengthening and resistance programme begins at 6 weeks. Immediate mobilisation of the elbow has obvious advantages and has been reported to have no adverse effect on outcome [14].
22 patients underwent repair of an acute rupture with a mean age at presentation of 46 years (32-59). 21 were male, there were no bilateral ruptures and 13 patients injured their dominant side (59%).
All but one patient described their surgery as successful with 16/22 rating their overall experience as excellent compared with 5 good and 1 fair. The average return to work was 100 days (range 0-280 days) with the average return to driving 49 days (range 0-112 days).
Mean OES and Mayo scores statistically improved from 18 (6-37) to 43 (24-48) and from 48 (5-95) to 95 (80-100) respectively (p < 0.00001).
Two patients lacked 10° of flexion, extension and supination, one patient lacked 20° of flexion and one patient had lost 10° of supination; all other patients had a full range of movement at final follow up.
10 patients felt restricted from full sporting activity: reasons given for activity restriction included fear (7 patients), perceived weakness (6 patients) pain (5 patients) and restricted range of movement (4 patients) (Table 1).
Table 1: Supination/pronation strength. View Table 1
Mean flexion power measured in the operative arm compared with the non-operated arm revealed no difference; 15.5 kg versus 15.4 kg respectively. 8 patients subjectively demonstrated less supination power in the operated arm in comparison to the non-operated arm whereas 3 patients demonstrated increased supination power in the operated arm in comparison to the non-operated arm. There was no subjective difference in supination power in the remaining 11 patients.
One patients reported a superficial infection which was treated with a short course of antibiotics. Two patients had superficial stitch granulomas which resolved with removal. 19 patients (86%) reported symptoms of altered sensation in the lateral forearm, all of which had completely resolved within 3 months. No patients sustained a re-rupture at final review. Post-operative radiographs were obtained in 20 of the patients at final follow up which showed that one patient had developed minor heterotopic ossification but was asymptomatic.
No intra-operative or postoperative radial fractures were seen and there were no cases of implant failure or clinical re-rupture were seen at final follow up.
The incidence of acute rupture of the distal biceps tendon is increasing [2]. This may be due to increased activity levels in the middle-aged population as well as the greater demands on the biceps muscle during professional and amateur sport and other recreational activities. Distal biceps reconstruction poses a significant surgical challenge with its aim to allow immediate range of movement and return patients to work or sporting activities quickly, balanced with the requirement of providing an ideal biological and biomechanical environment to allow tendon-bone interface healing. There is no single "gold standard" fixation technique but reconstruction options have expanded recently in order to utilise more modern surgical techniques.
Historically a single extensile anterior approach was used to reinsert the avulsed tendon. Concerns over neurological complications, encouraged Boyd and Anderson to develop a 2-incision technique designed to minimize anterior exposure [15]: however, this technique introduced the potential complications of heterotopic ossification (HO) and proximal radio-ulnar synostosis [16]. The Mayo Group modified this approach by splitting the supinator and avoiding subperiosteal dissection and this led to a decrease in the rate of these specific complications [16]. Single incision techniques became more popular with the introduction of suture anchors, due to the ease of insertion and the belief that one incision caused less morbidity. Single incision surgery also lent itself to the newly introduced interference screw and cortical button techniques. There is still great debate as to whether one or 2 incision techniques have an effect on the risk of neurological injury [10,12]. However, it is now widely reported that range of movement outcomes are equivalent whether undertaken by a modified Boyd-Anderson or a single anterior incision approach [17]. Grewal, et al. [10] randomised control study (RCT) reported lower number of minor complications, most of which where LABCN neurapraxias with a two-incision technique (3/43) as compared to a single anterior approach (19/47), and only 1 case of low grade heterotrophic ossification in each arm. We suspect the rate of neurapraxia that we encountered were secondary to the use of radial sided soft tissue retraction. Interestingly, Kelly, et al. [18] described a HO rate of 5.1% with no cases of synostosis when a modified Boyd Anderson approach was exclusively used. He described a nerve paraesthesia complication rate of 5/74 (7%). In our study, where a single incision technique was exclusively used, there were no cases of synostosis and only one case of mild HO. Although there were no permanent neurological complications, our study did reveal an 86% rate of temporary LABCN injury.
The four main reconstruction methods for ADBR are cortical buttons, interference screws, bone tunnels and suture anchors. Biomechanical studies have shown the cortical button to be superior in terms of highest load to failure (270N), followed by transosseous suture (210N), suture anchor (134-57N) and interference screw(105N). However, Mazzocca, et al. [19] showed in his physiological cyclical loading paper that all four options yielded similar results with low failure rates. In addition, it revealed excess movement suggesting 'pistoning' of the tendon within the tunnel and maybe impaired healing when a cortical button is used. Further studies have observed direct tendon healing to bone with interference screw fixation at 9 to 12 weeks [20-22] whereas indirect methods of fixation, such as bone anchors, tendon healing may take up to 12-26 weeks to fully mature [23,24]. Therefore, Mazzocca advocated the dual use of a cortical button and an interference screw in order to provide maximal biomechanical and biological advantage by avoiding 'pistoning' in the bone tunnel whilst encouraging early direct tendon to bone healing. However no particular technique has been proven to have clinical superiority with all four techniques reporting low and reproducible re-rupture rates.
Few studies report outcomes where both cortical button and interference screw are used as the fixation method but Cusick, et al. [9] reported a rerupture rate of 1.2% after 170 repairs using this method and Heinzelmann, et al. [11] original article had similar findings of no ruptures after 24 months in 32 repairs. Our study adds to this positive body of evidence demonstrating no re-ruptures or cases requiring revision. The age range, high levels of patient satisfaction and statistical improvements in functional scores in our study were consistent with those reported elsewhere in the literature [1].
Wang, et al. [1] reported a rerupture rate of 5.4% for all techniques in a 4-year period including 1443 patients but did not distinguish the fixation method nor approach. Olsen, et al. compared suture anchors and cortical buttons and found no re-ruptures in either cohort of a combined 37 biceps repairs [25]. Grewal, et al. [10] reported a re-rupture rate of 4.4% with the use of transosseous suture and suture anchors. Whereas Kelly, et al. [18] had only 1 rerupture out of 78 repairs over a 17-year period when using transosseous sutures.
In a recent systematic review by Kodde, et al. [12] looking at the fixation techniques in 1074 patients, with 565/1074 using suture anchors, 321 using bone tunnels, 42 using interference screws and 146 using cortical buttons showed re-rupture rates of 1.9%, 1.5%, 2.3% and 1.3% respectively.
Anatomic repair is reported to be more reliable in recreating the supination strength [26] by preserving the ulna position of the tendon footprint on the radial tuberosity and thus restoring the supination 'cam' (Figure 1). Our study only subjectively measured supination strength and thus no accurate conclusions can be drawn on this point; this is a weakness of the study.
PLLA (poly-L-Lactide) interference screws have been reported as causing significant osteolysis and tunnel expansion and could cause catastrophic failure in the form of radial cortex fracture [27]. The interference screw used in our study comprised of a different material, PEEK (poly-ether ether-ketone) and radiological review revealed no cases of osteolysis.
Single anterior incision surgery is the preferred approach for use of the cortical button. However, there is an association with posterior interosseous nerve palsy with this approach. Amin, et al.'s meta-analysis of complications from 2016 put the incidence of PIN palsy at 1.7% for anterior surgery compared to 0.2% for dual incision [28]. Cadaveric studies have suggested that the PIN can be incarcerated by the cortical button or drill with drilling at 45 degrees distally or radially, with the mean distance nearing 2 mm. This can be improved by ulna and perpendicular drill hole placement to 11 mm [29-34].
This is a small cohort of patients with ADBR undergoing fixation with this dual technique with a 12% loss to follow up rate. To our knowledge those lost to follow up have not presented to our service or to other hospitals in the region.
The combined biotenodesis screw and endobutton technique for distal biceps tendon repair is a safe and reliable technique providing excellent clinical and functional outcomes whilst allowing immediate range of movement by providing an ideal biomechanical and biological environment to allow early tendon-bone interface healing.
All authors participated in the conception and design of the study, and in interpretation of the results. PG, MB & AM prepared data from follow up. EM, PG, MB & AM participated in preparation of the manuscript. EM & PG were responsible for writing the manuscript. The illustrations have been supplied by Arthrex- who maintain the copyright.
Ethics committee approval was not required for this study. No competing interests are declared.
No conflict of interest is reported by the authors.