Infectious diseases can present similar to ovarian cancer and occur concomitantly with ovarian pathology. With increased worldwide travel and migration of populations, infections endemic to developing countries can emerge in the United States. We present 2 cases of infectious diseases mimicking ovarian carcinomatosis.
Two Filopina women presented with abdominal distension and had evaluations suggestive of advanced gynecologic malignancy. The first patient underwent surgery and was found to have peritoneal tuberculosis. Intra-operative pathology from the second case revealed ovarian carcinoma with schistosomal granulomas of the intestines.
Tuberculosis and schistosomiasis should be considered when treating women with gynecologic malignancies, especially those from abroad or who have spent time overseas. Correct identification of infectious etiologies allows for pharmacological intervention and can minimize unnecessary surgical procedures.
Ovarian cancer, Schistosomiasis, Peritoneal tuberculosis
Tuberculosis (TB), an infectious disease caused by the bacteria Mycobacterium tuberculosis, primarily targets the lung, but can spread to any site within the body. In 2013 the World Health Organization (WHO) estimated that there were approximately 9 million new cases of TB worldwide, and 1.5 million deaths due to the disease [1]. Over 9,000 new cases of TB were reported in 2014 in the United States.Correct diagnosis is critical as the treatment success rate approaches 86% [1,2].
Schistosomiasis is an infection caused by trematode worms. Initial symptoms are similar to a viral syndrome, then progress to inflammation with scarring of the liver, bowel and bladder. Over 200 million people are infected with schistosomiasis worldwide [3]. While the worms that carry the disease are not present in the United States, sporadic cases have appeared in non-endemic regions due to global migration [3]. The vast majority of these cases are seen after travel to sub-Saharan Africa. Travelers usually present with fever as the symptom of acute infection, but chronic infections (in travelers) are not typically clinically significant [4].
With a lifetime risk of 1 in 70, ovarian cancer is far more prevalent in the United States than either of the aforementioned infectious etiologies [5]. Presenting symptoms commonly includes bloating, abdominal distention, early satiety, and mass effect symptoms to include pain, urinary retention, and constipation. Ultrasonography is utilized to evaluate the pelvis for features that are suggestive of malignancy. Features worrisome for carcinoma include large complex adnexal masses and the presence of ascites. Elevation in cancer antigen 125 (CA 125) is also suggestive of malignancy, particularly in the postmenopausal patient. A clinical picture with a high probability of malignancy warrants surgical intervention [5].
We present a case of TB mimicking ovarian carcinomatosis and a case of ovarian cancer with concomitant intestinal schistosomiasis, both of which were discovered during ovarian cancer de bulking surgery.
A 52-year-old Filipina presented with abdominal distension. A Computed Tomography (CT) scan of the abdomen and pelvis revealed nodularity within the peritoneal cavity suggestive of diffuse peritoneal carcinomatosis (Figure 1). Cancer antigen 15-3 (CA15-3) and CA 125 were elevated. An image guided biopsy was negative for malignancy. She underwent exploratory laparotomy with intra-operative findings of diffuse peritoneal nodularity. A total abdominal hysterectomy with omentectomy and lysis of adhesions was completed. Nodules ranging from 0.1 to 0.3 centimeters (cm) were noted to widely punctuate the uterine serosal surface. Two 1 cm nodules were removed from the surface of the small bowel. The omental tissue removed was scattered with micro nodules ranging from 0.1 to 0.5 cm with confluence of nodules into larger aggregates. Frozen pathological diagnosis was performed and revealed noncaseating granulomas. Final pathology was significant for peritoneal and serosal noncaseating granulomata and no evidence of carcinoma. Acid Fast Bacilli (AFB) peritoneal and sputum cultures were positive for Mycobacterium tuberculosis.
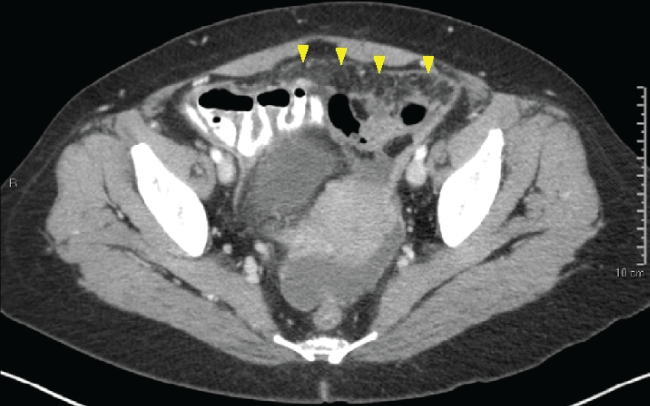 Figure 1: CT abdomen/pelvis revealing diffuse nodularity within the peritoneal cavity, suggestive of peritoneal carcinomatosis (arrowheads). View Figure 1
Figure 1: CT abdomen/pelvis revealing diffuse nodularity within the peritoneal cavity, suggestive of peritoneal carcinomatosis (arrowheads). View Figure 1
She was initiated on anti-tuberculin therapy which included Ethambutol 1200 mg and pyrazinamide 1500 mg orally daily for 2 months; Rifampin 600 mg, isoniazid 300 mg, and Vitamin B6 50 mg orally daily for 6 months. Currently, she is alive and well.
A 46-year-old Filipina presented with abdominal distention and a 20 cm pelvic mass at her annual gynecological visit. Radiological investigation revealed a 15 cm left ovarian cystic tumor containing mural nodules characteristic of epithelial ovarian cancer (Figure 2). Exploratory laparotomy with hysterectomy and bilateral salpingo-oophorectomy and ovarian cancer debulking procedure was performed after frozen section confirmed epithelial ovarian cancer. Miliary nodules were discovered on the serosa of the descending and rectosigmoid colon (Figure 3). Due to extensive intestinal involvement, surgical extirpation was not performed, but biopsies of the sigmoid epiploica were obtained. Pathological diagnosis showed Stage IIC poorly-differentiated serous ovarian cancer. The intestinal biopsies revealed granulomatous inflammation of the serosa consistent with a remote infection with schistosomiasis.
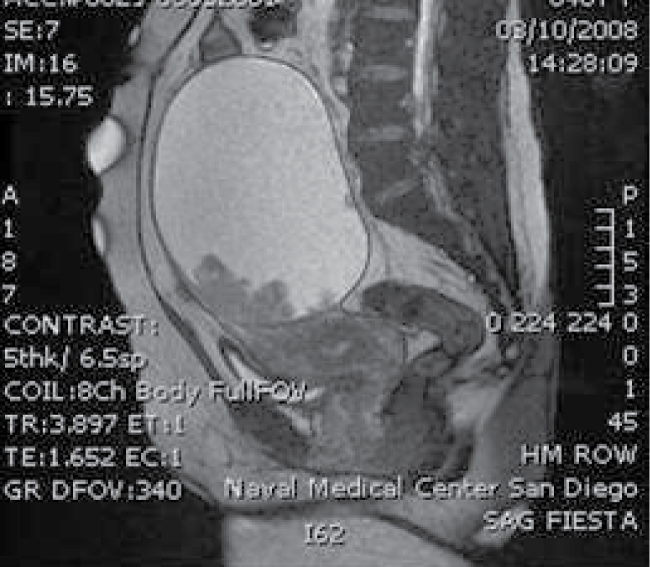 Figure 2: MRI of the abdomen/pelvis showing large left ovarian cystic mass with mural nodularities. View Figure 2
Figure 2: MRI of the abdomen/pelvis showing large left ovarian cystic mass with mural nodularities. View Figure 2
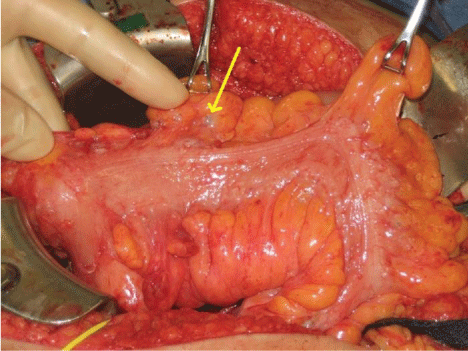 Figure 3: Miliary nodules (arrow) noted on the serosa of the large intestine. Final pathology revealing granulomatous inflammation consistent with schistosomiasis. View Figure 3
Figure 3: Miliary nodules (arrow) noted on the serosa of the large intestine. Final pathology revealing granulomatous inflammation consistent with schistosomiasis. View Figure 3
The patient was then referred to Infectious Disease, where it was determined that she was most likely infected with S. japonicum given her social history. There was no evidence of active infection based on the remote nature of her last exposure. Treatment was still recommended however as continued parasitemia could possibly lead to cirrhosis as well as other medical problems once she was subjected to chemotherapy.She was treated with praziquantel 40 mg/kg orally as a single dose.She then underwent adjuvant chemotherapy with 6 cycles of carboplatin AUC 6 and paclitaxel 175 mg/m2 every 21 days. She is currently aliveand without evidence of recurrent ovarian cancer.
Extra pulmonary tuberculosis is not uncommon in endemic areas [2,6]. In cases of pelvic tuberculosis, which accounts for 11-16% of extrapulmonary TB, women often deny exposure to TB and do not have respiratory symptoms [2,6,7]. Presenting complaints often include abdominal pain, abdominal swelling, weight loss, vaginal bleeding and infertility. Due to the nonspecific symptoms, women are frequently misdiagnosed. The most common misdiagnosis is ovarian cancer, but also includes pelvic inflammatory disease, tubo-ovarian abscess, ectopic pregnancy and disseminated carcinomatosis [2,6,7]. The diagnostic accuracy of commercial tests for extra pulmonary TB is highly variable and culture remains the gold standard [6,7]. Women should also be tested for sexually transmitted infections, especially the Human Immunodeficiency Virus (HIV), as concomitant infection greatly increases mortality [1]. Medical treatment of tuberculosis is largely successful, with success rates averaging 86% [1].
Radiologic imaging may be helpful in aiding diagnosis [8]. Abdominal ultrasound often reveals "septated ascites" or a "violin string" appearance of adhesions within the ascites. On hysterosalpingogram, the alteration between dilatation and constriction of the fallopian tubes due to scarring from TB gives a "lead pipe" or "beaded string" appearance and uterine synechiae may distort or even completely occlude the endometrial cavity. The peritoneum and omentum are often described as "thickened" or "nodular" on CT or Magnetic Resonance Imaging (MRI) [2,8].
Because laboratory testing and imaging often do not provide a diagnosis, many cases of pelvic tuberculosis are discovered as a result of surgical exploration, as was in the first case. This highlights the importance of intra operative frozen pathological diagnosis in order to avoid unnecessary surgery such as an extensive bowel resection. When possible, surgery should be avoided, at least until treatment has been started, in order to reduce infectious complications [7]. Surgery should be undertaken in the case of complications due to mass effect.
Although rare in the United States, schistosomiasis is quite prevalent worldwide, infecting 250 million people worldwide. It commonly affects the female lower genital tract, particularly the cervix and uterus and less commonly the fallopian tubes and ovaries. Case reports of lesions involving the upper genital tract note that it can present similarly to that of ovarian cancer, with the most common presenting complaint being lower abdominal pain. It has also been found during work-ups for ectopic pregnancy, infertility, adnexal masses, genital lesions and cervical cancer screening [3]. In the United States, there have been only 9 reported cases of female genital schistosomiasis [3]. Nevertheless, this disease should be considered in the differential diagnosis of ovarian carcinomatosis in women from endemic countries. Like tuberculosis, the presence of schistosomal infection, particularly with S. haematobium, has been positively correlated with HIV infection and women should be tested for HIV if found to have this infection [3]. All three of the major subspecies of schistosomiasis have been implicated in the development of cancer, thought to be caused by tumorigenic factors released by the parasite [9]. S. haematobium has been shown to increase the risk for squamous cell carcinoma of the bladder [10,11]. S. mansoni has been associated with hepatocellular carcinoma, while S. japonicumincreases risk for hepatocelluar carcinoma as well as colorectal carcinoma [10-12]. Interestingly, the schistosomal lesions found in our patient were located on the intestine, and based on her geographic exposures; S. japonicum was believed to be the most likely offender. The physical locations of the lesions noted intraoperatively are not suggestive of schistosomiasis as a cause of her carcinoma, but rather as an incidental finding. She went on to have a colonoscopy without evidence of carcinoma. Furthermore, cases of schistosomiasis leading to cervical dysplasia, particularly in those with HPV-positivity have been documented [10,11]. Continued research into the area of schistosomiasis and genitourinary carcinoma is warranted.
Histological confirmation intraoperatively by frozen section may prevent morbidity and unnecessary bowel surgery. Schistosomiasis is treated with pharmacologic therapy and surgical resection is not necessary to eliminate the parasitic lesions from the infected individual. Per WHO recommendations, schistosomal infections are treated with a single dose of Praziquantel 40 mg/kg. Minimizing blood loss, operative time, and major bowel surgery with the correct diagnosis may improve outcomes for these patients, especially if there is a concomitant ovarian cancer. In this case a chronic infection of intestinal schistosomiasis was discovered at the time of ovarian cancer surgery, mimicking disseminated metastatic disease to the bowel. Our patient was treated for her helminthic infection prior to chemotherapy in order to avoid any potential infectious complications as a result of her immunosuppression caused by the adjuvant carboplatin and paclitaxel. This step-wise regimen has been used successfully previously and there have not been any documented interactions between praziquantel and the before mentioned chemotherapeutic regimen [11].
In treating women with gynecologic malignancies, consideration should be given to alternative and concomitant diagnoses of infectious diseases like tuberculosis and schistosomiasis. Assessing individual risk factors and social histories can aid in a timely diagnosis, prompt pharmacologic intervention and minimize unnecessary surgical procedures. In addition, all patients with the aforementioned bacterial and parasitic infections should undergo routine HIV screening.