Peritrochanteric fractures of the femur rank among the most severe fractures in elderly people. The Gamma Nail is one of the latest advance in the treatment of trochanteric fractures based on intramedullary nailing principles during closed procedures. This paper is made to assess the efficacy of closed intramedullary osteosynthesis with a gamma nail in the treatment of peritrochanteric fractures depending on the type of fracture and patient age.
The study was based on a total of 30 patients surgically treated for the peritrochanteric femoral. Fracture in the period between June/2012 till February/2014, including 10 males and 20 females with the mean age are 67.63. The surgical operations were performed in all cases and Gamma3 intramedullary nail was inserted in medullary cavity.
There were 28 patients (93.33%) with good reductions while there were 2 cases with mild displacement (< 8 mm) in both AP and lateral views but considered accepted. The fracture had healed in all the patients with no significant varus displacement except in 2 patients where their fracture had healed with mild (< 20) degrees varus angulations. No intraoperative complication was reported; fracture of femur mid shaft ten weeks pos top. Had occurred in 1 patient. Screw cut out had occurred also in 1 case while 3 cases sustained superficial infection. Recovery situations of all patients were valuated based on Harris scoring with an average of 87 points. There are indications and short comings in the treatment of intertrochanteric fracture with Gamma3 intramedullary nail.
The gamma nail is an excellent alternative in treatment of unstable peritrochanteric fractures.
Intramedullary, Pertrochanteric, Orthopaedic, Gamma nail
1. To assess the patients’ recovery after operative treatment of the peritrochanteric femoral fracture with gamma nail osteosynthesis.
2. To determine the clinical results and complications of treatment of peritrochanteric fracture with Gamma nail.
3. To evaluate perioperative, radiographic and clinical measures of outcome after a minimum follow-up of one year.
Trochanteric fracture is common in elderly population. Ninety percent of trochanteric fractures in the elderly patients result from a simple fall [1]. Trochanteric femoral fractures have been estimated to occur in more than 200,000 patients annually in the United States, with reported mortality rates ranging from 15% to 30% [2]. Approximately 50-60% of all trochanteric fractures are classified as unstable. This represents a great challenge to the operating surgeon, as the rate of failure for these kinds of fractures vary from 8 to 25% [3]. Treatment options include non operative treatment and operative treatment. Operative options include closed reduction and internal fixation with dynamichip screws, dynamic condylar screws and intramedullary fixation devices [4]. Since its introduction in the late 1970's, the Dynamic Hip Screw (DHS) had become a standard device for the fixation of all trochanteric fractures of the femur [5]. The Gamma nail was the first trochanteric-entry nail introduced in 1988, and was designed specifically for the treatment of unstable fractures. Gamma nail has shorter lever arm with reduction in bending stress and lower implant failure rate and makes no dissection at the fracture site. The nail occupies the medullary canal, preventing excessive sliding and medialization of the shaft even in A3 fractures [6]. The short gamma nail is a superior implant for stable and unstable trochanteric fractures in terms of operating time, surgical exposure, blood loss, and complications, especially for patients with relatively small femora [7]. It is recommended that subtrochanteric fractures and hip fractures with associated femoral shaft fractures and pathological extra capsular fracture should be treated by intramedullary fixation [8]. In patients with unstable trochanteric fractures treated with gamma nail, technical or mechanical complications seem to be related to the fracture type, operating technique, and time to weight is ring rather than the implant itself. Screw migration is attributed to fracture instability, presence of osteoporotic bones, and impaction at the fracture site [9].
Between June, 2012 and February, 2014 an experimental, hospital-based study was conducted in department of orthopedic at King Fahd Armed Forces Hospital, Jeddah, Saudi Arabia based on a total of 30 patients surgically treated for the peritrochanteric femoral fracture. The pertrochanteric fractures taken for study were fresh fractures which were studied prospectively after taking due consent. Subsequently they were subjected to management by gamma nail surgery in a consecutive fashion over the above mentioned period. The study excluded patients with combination of trochanteric fractures and ipsilateral shaft fracture which were treated by long gamma nail and also those who were lost to follow-up. Patients were seen postoperatively at regular intervals of first month, third month, sixth month and then annually. All the patients were evaluated for perioperative parameters like duration of screening time (in seconds), operating time (in minutes), blood loss during surgery (in milliliters), ease of procedure; possible intra operative complications like malreduction/failure of reduction, jamming of nail, drill breakage, failed distal locking, iatrogenic fracture shaft femur, fracture displacement. Blood loss during surgery included blood loss due to fracture and operative losses. Here screening time meant the time during which a particular fracture was screened under image intensifier during surgery. In the present study the ease of operation was categorized as easy, usual and difficult. This was purely a perioperative subjective criterion and the opinion of the operating surgeons was taken into account to label a surgery as easy, usual or difficult. Postoperatively they were assessed for malunion, delayed union, osteonecrosis of head of femur, osteoarthritic changes at hip, general and local complications and any additional/revision surgery required. Also, they were assessed for date out of bed to chair, state of ambulation, ambulatory status at discharge, requirement of ambulatory assistant devices, weight-bearing status at discharge and length of hospital stay. Radiographic assessment of fracture fragment position, lag screw position, nail alignment and extent of fracture healing was made.
The target population was patients admitted in orthopedic department of orthopedic at King Fahd Armed Forces Hospital. A purposeful, non-random sample included 30 patients surgically treated for the peritrochanteric femoral fracture. Study population consisted of 10 males and 20 females with the mean age are 67.63. The surgical operations were performed in all cases and Gamma3 intramedullary nail was inserted in medullary cavity.
Harris hip score was used for pre and post operation functional assessment, Statistical Package for the Social Sciences (SPSS) program version 21 used for data entry and analysis.
Ethical approvals obtained from Ministry of Health, research ethics committee of King Fahd Armed Forces Hospital and head of orthopedic department. Also, Informed consent taken from the patients.
The mean follow up of 30 patients was 15 months (12-18) and details of these are shown in Table1. There were 10 males and 20 females. The right side was affected in 16 patients and the left side in 14 patients. The age ranged from (50-81 years) with the mean age is 67.63 years old. The mechanism of injure was fall in 25 patients and RTA in 5 patients. The patients stayed in the hospital for about (4-7 days) with the mean hospital stay are 5 days.
Table1: Data of the 30 patients with trochanteric fracture. View Table 1
There were 28 patients (93.33%) with good reductions while there were 2 cases with mild displacement (< 8 mm). In both AP and lateral views but considered accepted. The fracture had healed in all the patients with no significant varus displacement except in 2 patients where their fracture had healed with mild (< 20) degrees varus angulations. Lag screw position (Diagram 1) was central in anteroposterior and lateral views in 12 cases (40%) of cases while it was central in AP but posterior in lateral view in 9 cases (30%). Lag screw was central in AP but superior in lateral view in 2 cases (7%) of patients. Also lag screw was inferior posterior in 4 cases (13%), while it was superior and posterior in 2 cases (7%); it was inferior and anterior in 1 case (3%). There was one case reported with cut out of the lag screw through the femoral head. The Gamma nail requires short incision (4-6 cm) (Diagram 2). The blood loss ranged from (100-250 ml) with the mean blood loss was 196 ml (Diagram 3). The operative time ranged from (45-90 Min) with the mean operative time was 67.5 minutes. The average time of c-arm exposure was 2.9 minutes as it ranged from (1.5-3.5 min) (Table 2). One distal locking screw was inserted in all the patients, one of it discovered post operatively that it was outside the nail hole.
Table2: Operative and post operative data. View Table 2
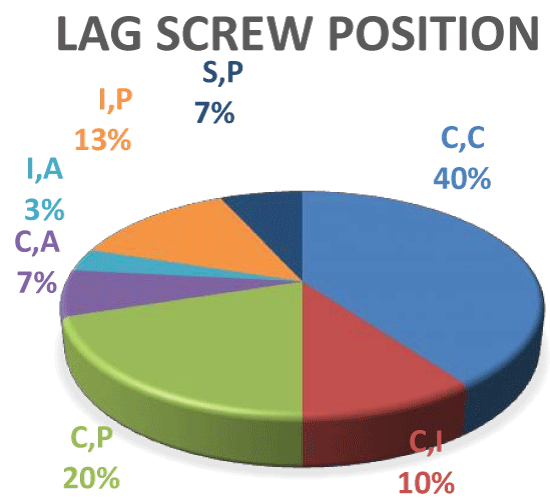 Diagram 1: Showing percentage of lag screw position. View Diagram 1
Diagram 1: Showing percentage of lag screw position. View Diagram 1
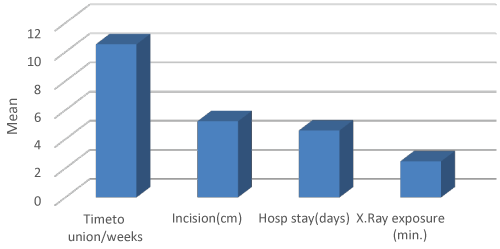 Diagram 2: Showing union time, incision, hospital stay & x-ray exposure time. View Diagram 2
Diagram 2: Showing union time, incision, hospital stay & x-ray exposure time. View Diagram 2
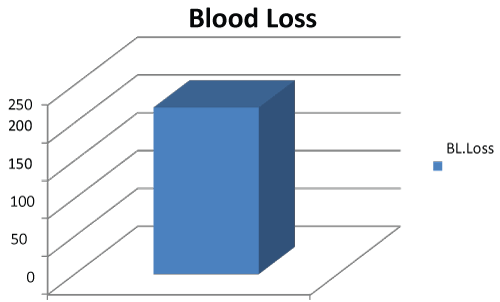 Diagram 3: Showing the average blood loss. View Diagram 3
Diagram 3: Showing the average blood loss. View Diagram 3
There were no recorded intraoperative complications like femoral shaft fractures or neurovascular injury or major bleeding in the present study. Also there was no systemic complication from the anesthesia and all patients recovered from the anesthesia. The mean hospital stay for the patients was 4.6 days (average 3-6 days) (Diagram 2).
The time to union of the fracture anged from 8 to 13 week with the mean time to union was 10.9 weeks (Diagram 2). About 2 patients were united in 13 weeks (7%), 8 patients were united in 12 weeks (24%), 11 patients were united in 11 weeks (37%), 4 patients were united in 10 weeks (13%), 1 patient was united in 9 weeks and 3 patients was united in 8 weeks (10%).
Only one patient was not united (3%) (Table 2). Union was assessed clinically by examining the patients for any local tenderness, limping, pain during range of motion or inability to bear weight over the affected extremity. Also union was assessed radiologically by appearance of callus on x-rays. 29 patients showed good and complete union (97%) while one patient only complicated by non union and screw cut out (3%).
Pain score was decreasing by time and it became very mild and non-significant at three months post operatively. The pain was compared to the pre fracture level or degree of pain that was present in some patients due to osteoarthritis and osteoporosis. There were 3 patients without any pain (10%), 20 patients with occasional, slight pain (67%) in comparing with pre fracture level of pain and 6 patients with mild pain but not affecting daily activity (20%). It is noted mainly at the mid thigh.
There was no apparent limp in 14 patients (47%) at six, twelve months while there was slight limping in 12 patients (40%) that was not present before the fracture but not affecting their daily activity. Also there was moderate limping in 3 patients (10%) in comparing to the pre fracture state. There was one patients complicated by infection and screw cut out and she was bed ridden as she could not ambulate.
17 patients used support for long distance walking (57%), while 9 patients used support for short distance walking (30%) and 3 patients did not use any support for walking (10%).
Distance walked was not affected in 9 patients (30%) and decreased mildly in the other 20 patient (67%) and they reported that it is decreased than the pre fracture distance that they can walk, while there was one non ambulating patient.
There were 22 patients who can ascend the stairs normally using railing (76%) but they said that it was the same as before the fracture, while there were 6 patients who can ascend the stairs normally without using railing (18%).
25 patients were found that they can sit comfortably in ordinary chair (85%), while only 4 patients who need high chair to set comfortably (12%).
18 patients can wear their shoes easily (60%), while 9 patients reported difficulty in wearing their shoes (30%) in contrast to the pre fracture state and the remaining 3 patient were unable to wear their shoes alone (10%).
18 patients were found to have node formity like flexion, abduction deformity and no leg length discrepancy (66%) while 7 patients were found complaining of mild leg length discrepancy about 1.5 cm (22%) that was treated by shoe modification and 4 patients were found to have mild flexion deformity (10%).
The range of motion (the sum of degrees of flexion, abduction, adduction, internal and external rotation) was not decreased in 5 patients (17%) as it was between (211-300 degrees) while it was found to be decreased a little in 20 patients (67%) to be between (161-210 degrees) and it was decreased in 5 patients (17%) to be between (100-160).
The final Harriships core was excellent in 7 patients (23%) as it ranged between (90-100), while it was good in 13 patients (44%) as it ranged between (80-89). It was fair in 5 patients (17%) as it ranged (70-79) and it was poor in 5 patients (16%) as it ranged less than 70 (Diagram 4).
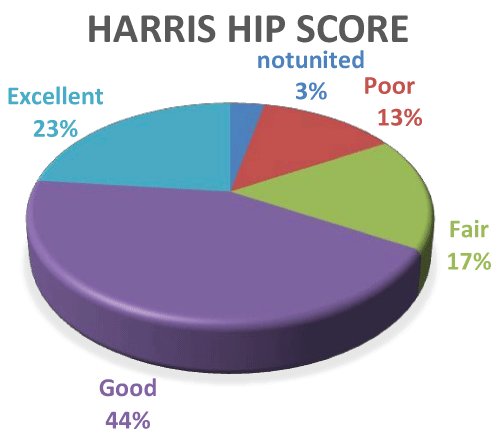 Diagram 4: Showing percentage of Harris hip score outcome. View Diagram 4
Diagram 4: Showing percentage of Harris hip score outcome. View Diagram 4
We have 5 cases with complications in our study, one case complicated by deep infection because the patient had chronic urinary tract infection and she developed septicemia and she was admitted to ICU.
This patient developed non union and screw cut out from the femoral head (Figure 1). This patient treated by nail and screw removal, serial debridement (Figure 2 and Figure 3), excision of the necrotic bone and she was given IV antibiotic according to the wound culture for 6 weeks and she was planned for bipolar hemiarthroplasty but she died before the operation (Figure 4 and Figure 5).
 Figure 1: Pre op. Intertrochanteric fracture. View Figure 1
Figure 1: Pre op. Intertrochanteric fracture. View Figure 1
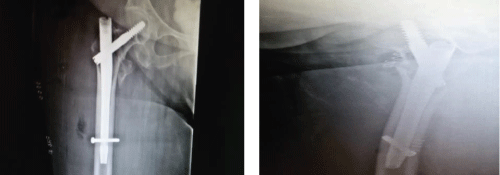 Figure 2: Direct post op. Ap & lateral views. View Figure 2
Figure 2: Direct post op. Ap & lateral views. View Figure 2
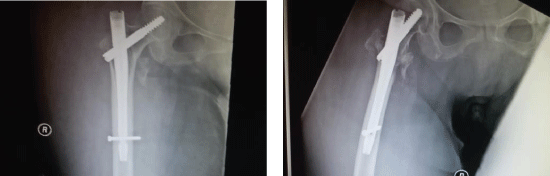 Figure 3: 2 months post op. Ap & lateral views. View Figure 3
Figure 3: 2 months post op. Ap & lateral views. View Figure 3
 Figure 4: 4 months post op. Ap & lateral views; the screw start to cut out of the head of femur. View Figure 4
Figure 4: 4 months post op. Ap & lateral views; the screw start to cut out of the head of femur. View Figure 4
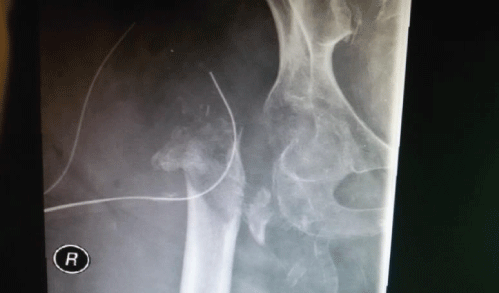 Figure 5: Post removal of the gamma nail & lag screw. View Figure 5
Figure 5: Post removal of the gamma nail & lag screw. View Figure 5
There is also one case sustained post operative femoral fracture at lower end of the prosthesis due to mechanical fall from the bed at the tenth week postoperative and treated by exchange the short gamma nail by along one with good result (Figure 6, Figure 7, Figure 8 and Figure 9).
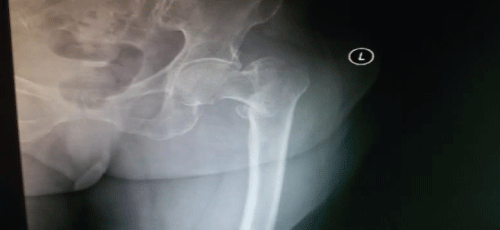 Figure 6: Pre op. X-ray. View Figure 6
Figure 6: Pre op. X-ray. View Figure 6
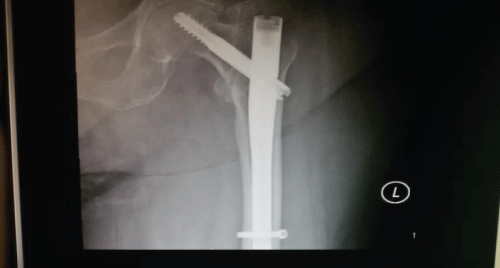 Figure 7: Direct post op. X-ray. View Figure 7
Figure 7: Direct post op. X-ray. View Figure 7
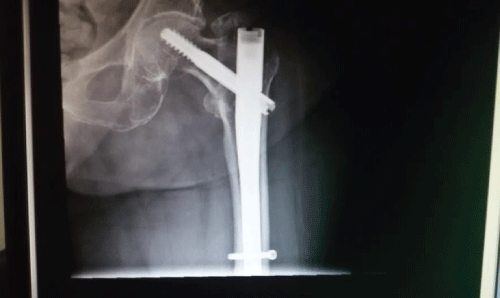 Figure 8: 6 weeks post op. View Figure 8
Figure 8: 6 weeks post op. View Figure 8
 Figure 9: Ten weeks post op. with fracture femoral shaft at the tip of the nail & reoperation using long gamma nail. View Figure 9
Figure 9: Ten weeks post op. with fracture femoral shaft at the tip of the nail & reoperation using long gamma nail. View Figure 9
Also there are more 3 cases complicated by superficial infection no treaching the prosthesis deeply and were treated by local wound debridement, irrigation, wash and dressing with adding IV antibiotic according to wound culture fort two weeks then continue with oral antibiotic for more two weeks with complete wound healing without causing any effect on the stability of fixation.
Unstable peri and subtrochanteric fractures of the proximal femur are complicated by the massive tension moments laterally and compressive forces created medially by the weight of the body, hip flexors and external rotators and by the abductor musculature, resulting often in fracture displacement, loss of fixation and implant failure [10].
The goal of any fracture fixation is to provide and maintain stable fixation while improving functional results. The available published literature on this subject has shown that these fractures may be treated by a variety of devices, including Nail Plate devices, Dynamic Hip Screw (DHS) and medullary devices, e.g. Ender’s Nail, Zickel nail, Gamma Nail devices. The compression hip screw is currently the device most commonly used to stabilize trochanteric fracture [11]. However, failure rates and complications as varus, collapse and limb shortening, cut-out through the head and neck and, rarely, lateral pulling out of the side plate were reported [12].
To decrease these complications, the Gamma Nail (GN) was developed. The design of the Gamma nail combines the advantages of the sliding lag screw and those of intramedullary fixation with decreasing the moment arm as compared with that for the compression nail-plate system. It has the advantage of closed insertion, preservation of fracture hematoma and less dissection, which is an important consideration in fracture healing [13].
The Gamma nail proved to be an adequate implant to stabilize stable and unstable peri- and subtrochanteric fractures. Calvert in his study found that GN was better for the management of complex peritrochanteric fractures with subtrochanteric extension.
Various other studies [14] found favorable results with GN in managing a greater variety of hip fractures with a less in vasive technique and with better results [15]. Other studies have reported favorable results with GN in terms of shorter operation time, less blood loss, shorter hospital stay, decreased wound infection and reduced complication rate [16]. Also, it has been observed that the rate of complications associated with GN decreases appreciably with increase in learning curve of the operating surgeons [17]. However, problems with the Old generation of Gamma nail were reported and included fracture of the nail, pain in the thigh, and intra operative and late diaphyseal femoral fractures.
Three aspects of the old implant design have been implicated: curve, stiffness and size [18]. The original Gamma nail had a mediolateral curvature of 10° that differed from the trochanter-to-diaphysis angle in an average patient. This shape of the Gamma nail is thought to cause three-point loading across the trochanteric and diaphyseal cortices. Therefore stress is concentrated mainly along the medial cortex in contact with the nail curvature and on the nail tip in contact with the lateral cortex, thus exposing the femur to intra operative and post operative fractures, even under physiologic loads [18]. Moreover, the high implant stiffness also results in a stress rising effect at the nail tip [19].
Mismatch between implant size and medullary canal diameter, particularly with in adequate reaming and forceful nail insertion (hammer), can create high hoop stresses. This can result in non-displaced fractures during nail insertion, which may propagate after weight-bearing. A new modifications of the gamma nail has been introduced with recent design features that may improve the clinical results and decrease the complication rates [20]. The newer generation Gamma3 nail has a 15.5 mm proximal diameter, 4-degree valgus inclination, and a 10.5-mm diameter lag screw. The distal locking screw is 5 mm in diameter. Available lag screw insertion angles are 120, 125 and 130 degrees with a distal nail diameter of 11 mm.
In our study, pain in the mid portion of the thigh is observed with the use of gamma nail. This is consistent with the other studies using Gamma nail [13]. The operating time in our study ranged from 45 to 90 minutes .The blood loss in our patients (196 ml in average) was less comparing to other reports [21]. The results regarding postoperative weight-bearing were also comparable to other studies [22]. Functional assessment of the operated hip joint according to the Harris scale indicates a predominance of excellent and good results in unstable peritrochanteric fractures. The average time of fracture healing in our study is 10.2 weeks while the average time of radiological exposure is 3.9 minutes and this was comparable too there studies [23].
There were no intra operative diaphyseal femoral fractures associated with the intramedullary hip screw in the present study but there is one case reported 10 weeks post operatively with femoral shaft fracture after a mechanical fall. Both intra operative and late femoral fractures were reported with the use of Gamma nail [24]. These fractures maybe caused by excessive loads around the end of the nail.
The angle of the gamma nail in the mediolateral plane is only 4 degrees with fewer forces transmitted to the end of the nail. This may explain the low incidence of late diaphyseal fractures associated with the new generation of gamma nail [20].
Osteosynthesis with gamma nail is operational procedure with extraordinary results in operations of the peritrochanteric fractures. The main advantage of this procedure includes less tissue damage and better operation outcomes. Gamma nails are theoretically more load-sharing with the medial cortex of the femoral neck than are lateral cortical constructs. Because of more medial placement of the intramedullary nail compared to the side plate of the compression hip screw, the bending moment at the nail-screw junction is lower than that at the plate-screw junction. Other potential advantages of intramedullary fixation include small erioperative exposure and possibly shorter operative time. All suggested advantages are clearly shown in this study, too. Also, because of less limb shortening, especially with the unstable and comminuted fracture, the intramedullary hip screw seems to be a promising alternative. Mid-thigh pain can be partially solved by using the locking screws only in comminuted fractures and in situations which are liable to rotation. The use of only one locking screw instead of two seems advisable for these fractures.
A reduced percentage of poor outcomes, especially in unstable peritrochanteric fractures, compared too there operative methods encourages the promotion of intramedullary gamma nail osteosynthesis. The final Harris hip score at 1 year was excellent and good in 20 patients (67%) as it ranged between (80-100), while it was fairing 5 patients (17%) as it ranged (70-79) and it was poor in 5 patients (16%) as it ranged less than 70. Thus we agree with the previous data that the gamma nail is an excellent alternative in treatment of unstable peritrochanteric fracture.