Fat Soluble Vitamins (FSV) is essential for the normal growth and development of children. Many genetic and acquired conditions have the potential of interfering with FSV absorption and transport. Understanding the physiology of these conditions is imperative in providing effective treatment, including prevention of FSV deficiency. In this article, we present three case studies that illustrate the importance of FSVs. We explore recommended intake of each of the FSV as well as clinical signs of deficiency. Further discussion and research is needed to improve awareness of FSV deficiency by clinical lipidologists, the prevalence of FSV deficiency in these disorders, and effective strategies for effective treatment and prevention.
Fat-soluble vitamins, Lipidology, Lipoproteins, Metabolism
Clinical lipidologists encounter a variety of genetic and acquired conditions that alter lipid and lipoprotein metabolism. Effective treatment requires accurate diagnosis and understanding of the disease process. Dietary fat and lipoproteins play an important role in the normal absorption and transport of Fat Soluble Vitamins (FSV), which are essential for health and wellness, including normal growth and development in young children. In this article we discuss a variety of conditions and interventions which may disrupt FSV absorption and transport, resulting in well described clinical manifestations of deficiency (Figure 1).
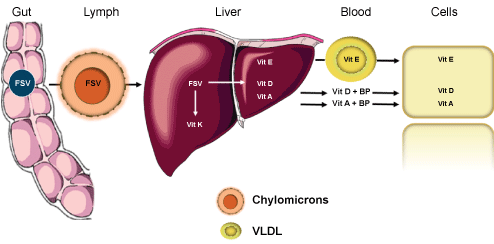 Figure 1: FSV absorption and transport. Following hydrolysis, FSV (Vitamins A, E, D and K, as well as carotenoids), are captured from mixed micelle by the apical membrane transporters, including Scavenger Receptor class B1 (SR-B1), Cluster Determinant 36 (CD36) and Niemann-Pick C1-Like1 (NPC1L1). Although incompletely understood, it is thought that proteins are involved in transport of FSV and carotenoids within the enterocyte. Non-metabolized vitamins and carotenoids are incorporated into chylomicrons and secreted into the lymph. Following transport to the liver, FSV are either metabolized, stored or transported to target cells via VLDL and binding proteins. View Figure 1
Figure 1: FSV absorption and transport. Following hydrolysis, FSV (Vitamins A, E, D and K, as well as carotenoids), are captured from mixed micelle by the apical membrane transporters, including Scavenger Receptor class B1 (SR-B1), Cluster Determinant 36 (CD36) and Niemann-Pick C1-Like1 (NPC1L1). Although incompletely understood, it is thought that proteins are involved in transport of FSV and carotenoids within the enterocyte. Non-metabolized vitamins and carotenoids are incorporated into chylomicrons and secreted into the lymph. Following transport to the liver, FSV are either metabolized, stored or transported to target cells via VLDL and binding proteins. View Figure 1
A 15-year-old boy developed progressive dementia and an abnormal gait. His birth and development were normal, except for intractable diarrhea during childhood. Xanthomas were recognized at 7 years of age; cataracts at age 10 [1]. His total plasma cholesterol, LDL cholesterol, and triglycerides were normal.
A previously healthy, developmentally normal 3-year-old boy developed Xanthomas of the extensor surfaces of the elbows and knees. His stools were very pale in color, and he had begun complaining of pruritus and abdominal discomfort, which caused a decrease in his appetite. Mild scleral icterus was noted. A fasting lipid profile revealed elevations in total cholesterol (1184 mg/dL) and Low-Density Lipoprotein Cholesterol (LDL-C, 510 mg/dL). Triglycerides were within normal limits (47 mg/dL). Liver tests were markedly abnormal [2].
A 2-month-old female was noted to have lipemic serum during a routine blood draw. Plasma triglycerides were > 2000 mg/dL, which was confirmed upon repeat testing. She was continued exclusively on breastfeeding. At 6 months of age, the child presented to an emergency department after 24 hours of refusing feedings, irritability, low-grade fever, and 2 episodes of non bilious vomiting. On physical examination, her abdomen was distended and tender to palpation. Eruptive Xanthomas were noted over the buttocks. The child's body fat distribution was normal. These 3 cases help illustrate the potential disruption in FSV absorption transport either as a consequence of the underlying disorder, medical interventions used to treat them, or both.
• Case #1: Cerebrotendinous Xanthomatosis [CTX] is a rare disease characterized by the accumulation of cholesterol and cholestanol in brain and tendons. It is caused by a mutation in the sterol 27-hydroxylase gene [CYP27A1] involved in bile acid synthesis. Disruption of bile salts, such as in this case, also impairs FSV absorption. Cataracts become evident in childhood or adolescence, and xanthomata develop in the 2nd and 3rd decades of life. Significant neurologic impairment also occurs; this often includes seizures, dementia, and extra pyramidal dysfunction, typically beginning in the 3rd decade of life and progresses until death [3].
• Case #2: Although this child's clinical presentation (Xanthomas with marked elevation of total and LDL cholesterol) suggests the possibility of familial hyper cholesterolemia, his clinical, laboratory, and liver biopsy findings were consistent with familial sclerosing cholangitis [2]. The liver plays a key role in fat and FSV absorption and metabolism. It synthesizes bile salts, which facilitate emulsification of dietary fat and activate lipases, which aid in hydrolysis of fats. Inherited or acquired liver diseases can present with profound changes in the plasma concentration of lipids and lipoproteins, and malabsorption of FSV.
• Case #3: Familial Chylomicronemia Syndrome (FCS) is an autosomal recessive disorder characterized by severe hypertriglyceridemia, with triglyceride levels generally > 1000 mg/dL. Because the severe hypertriglyceridemia in FCS is the result of dietary derived chylomicrons, standard lipid lowering therapies, such as omega-3-fatty acids, niacin, and fibrates, are generally ineffective [4]. Triglycerides may be substantially lowered, however, by restricting dietary fat to < 10-15% of the total daily caloric intake [5]. If triglycerides are not lowered to goal, further dietary fat restriction may be necessary while ensuring daily essential fat intake (2-4% daily caloric intake from linoleic acid and α-linolenic acid) [6,7]. Such severe restriction of dietary fat as well as impaired long chain fat metabolism, however, may also result in FSV deficiency.
Vitamins are organic compounds necessary for normal growth and maintenance of good health. They are generally classified as being water- or fat-soluble. Important differences exist between water and fat-soluble vitamins (Table 1). Micronutrient Dietary Reference Intakes (DRIs): Recommended Dietary Allowances and Adequate Intakes, Fat Soluble Vitamins and Calcium are listed in Table 2.
Table 1: Comparison of water-versus fat-soluble vitamins. View Table 1
Table 2: Micronutrient Dietary Reference Intakes (DRIs): Recommended dietary allowances and adequate intakes, fat soluble vitamins. View Table 2
Although available as dietary supplements, in most humans, FSV are obtained from food sources. Following ingestion, FSV require bile for digestion and absorption. FSV are soluble in lipids, but not in aqueous solutions. Therefore, once absorbed FSV are incorporated into chylomicrons and transported by the lymphatic system. Vitamins A, D and E accumulate in the liver and fat tissue, and are not readily excreted. As a result, excessive intake can result in toxicity, particularly for vitamins A and D. Due to this, care should be taken to supplement only when necessary to avoid excessive intake. In contrast, vitamin K is easily excreted by the body. Dietary sources of FSV as well as signs of deficiency are included in Table 3.
Table 3: FSV sources and clinical signs of deficiency [9]. View Table 3
Table 4 lists lipid and lipoprotein disorders that potentially disrupt FSV absorption and metabolism. In addition, a variety of medications that interfere with intestinal absorption of fats (bile acid resins) or interrupt chylomicron and VLDL production and release, such as antisense apoB therapy and MTP inhibitors, may cause FSV deficiency.
Table 4: Lipid disorders and medications that disrupt fat soluble vitamin absorption/metabolism. View Table 4
Patients with disorders that disrupt FSV absorption and metabolism may benefit from routine monitoring of FSV levels with appropriate supplementation as needed for indicated deficiencies. Further research is needed on this topic to determine incidence of FSV deficiency in these conditions as well as most effective protocols for supplementation.