Scalp arteriovenous fistulae, as a result of hair transplantation, are exceedingly rare, with the current literature largely limited to few single case reports. Open surgical and endovascular treatments have been described with good results. We describe a case of scalp arteriovenous fistula following hair transplantation that was successfully treated by direct puncture embolization with n-butyl cyanoacrylate glue. We also review the literature for all other published cases, in order to best characterize this rare complication in terms of presentation, involved vasculature, treatment options, and expected outcome.
Arteriovenous malformation, Fistula, Complication, Angiography, Liquid embolic material
Arteriovenous fistulae (AVF) of the scalp are relatively rare and are usually the result of traumatic injury to the superficial scalp vessels. This may occur following a variety of insults, including: Car accidents, diving accidents, penetrating injuries from assaults with sharp objects, and iatrogenic etiologies, such as temporomandibular joint arthroscopy and punch-graft hair transplantation [1]. The literature related to scalp AVF following hair transplantation is limited primarily to single case reports [2-14]. These lesions have been successfully treated with surgical ligation, excision, direct puncture embolization, and selective angiography and embolization with full resolution in 100% of cases and no reported complications to this date. Absolute alcohol, polyvinyl alcohol micro-particles, coils, acrylic glue, and Onyx material have all been reported for successful embolization of scalp AVF [5-7,10,15,16]. We present a case of scalp AVF following hair transplantation with special attention paid to the management of the lesion. We further collect and synthesize previously reported cases on scalp AVF related to hair transplant procedures, in order to provide the most complete look at this rare complication.
A middle-aged patient was referred to our center for evaluation of a left temporoparietal scalp AVF. Approximately one year after undergoing hair transplantation in 2007 the patient noticed dilated scalp vessels in the left temporal area that to his knowledge was not present prior to his hair transplantation procedure. Following an initial outside evaluation, the patient was lost to follow up and presented to us in 2015 with worsening headaches, nausea, and vomiting. Physical examination was significant for a prominent, tortuous, pulsatile vascularity present beneath the skin in the left temporoparietal area, crossing the midline and travelling towards the right parietal area with no sign of any cranial nerve deficits. Magnetic resonance imaging (MRI) demonstrated extensive scalp vascularity, without abnormal intracranial vascularity.
Selective angiography of the external and internal carotid arteries revealed a parietal scalp AVF fed by the superficial temporal arteries (STA) and occipital arteries bilaterally and draining into a single, dilated, tortuous superficial scalp vein (Figure 1A and Figure 1B). There was no connection with the intracerebral vasculature. The fistulous point was localized angiographically and the dilated, proximal draining vein was punctured directly with a 23G butterfly needle. In order to completely occlude venous outflow in a 360° fashion a standard surgical lidocaine cup was cut into a small cylinder and placed over the butterfly needle and pressure was applied circumferentially (Figure 2). N-butyl cyanoacrylate (NBCA) glue (approved by the FDA in 2000) was then injected slowly through the needle. A total of 4 cc of glue was injected with intermittent angiograms performed via a catheter positioned in the right external carotid artery. The right ECA was chosen as it allowed for better ergonomics as the embolization needle and apparatus were positioned on the left side of the patient and the fistula filled equally from both external carotid arteries. Following total occlusion of the fistula and draining vein, the butterfly needle was removed. Follow-up angiography demonstrated complete obliteration of the AVF (Figure 3). The patient's scalp appearance improved significantly, however the area where glue was injected remained as a palpable mass. There were no immediate complications and the patient was discharged home on a steroid taper. Two weeks post-embolization the patient returned complaining of left facial swelling, and follow-up imaging demonstrated the presence of a subgaleal fluid collection with no findings suggestive of abscess development or recurrence of AVF. No intervention was required as the swelling resolved rapidly and spontaneously. On two-month follow up the patient's symptoms resolved completely.
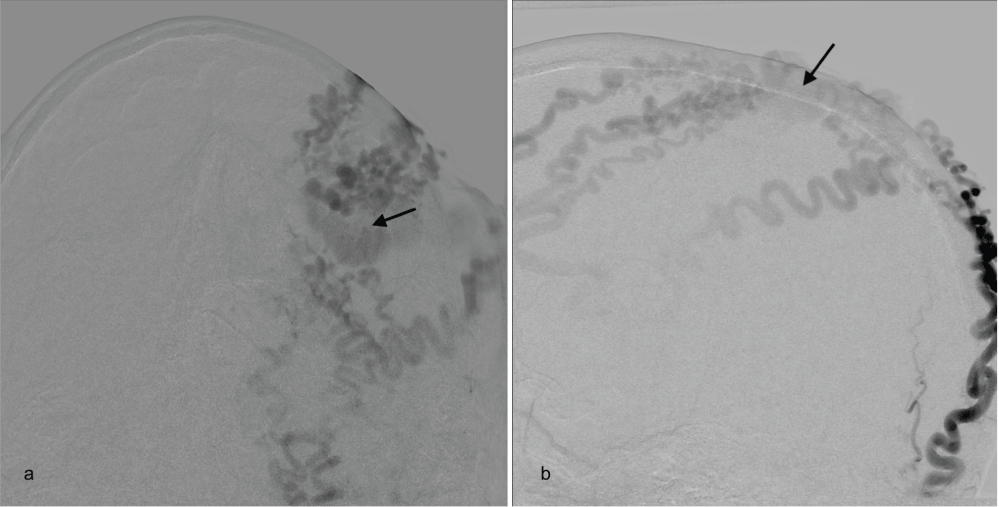 Figure 1: Submental AP (A) and lateral oblique (B) injection of left external carotid artery demonstrating the two STA branches and occipital artery connecting via a single fistulous point with the dilated draining scalp vein (arrows). View Figure 1
Figure 1: Submental AP (A) and lateral oblique (B) injection of left external carotid artery demonstrating the two STA branches and occipital artery connecting via a single fistulous point with the dilated draining scalp vein (arrows). View Figure 1
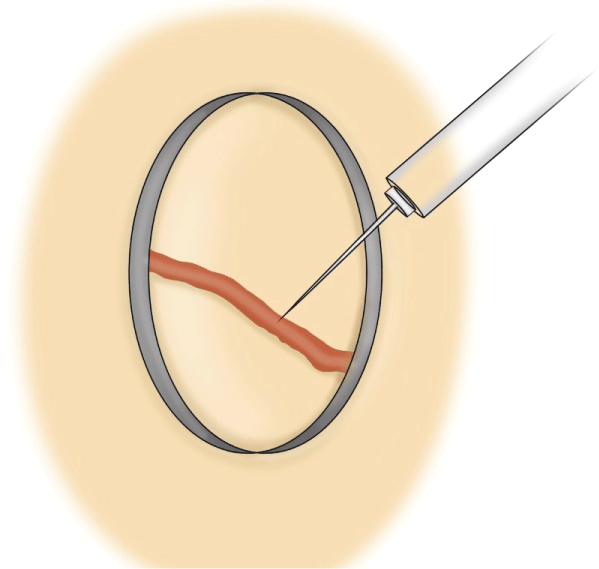 Figure 2: Direct needle puncture of fistulous point while utilizing an inverted plastic cup to apply circumferential pressure to completely occlude venous outflow, allowing for complete obliteration of the fistula with NBCA glue. View Figure 2
Figure 2: Direct needle puncture of fistulous point while utilizing an inverted plastic cup to apply circumferential pressure to completely occlude venous outflow, allowing for complete obliteration of the fistula with NBCA glue. View Figure 2
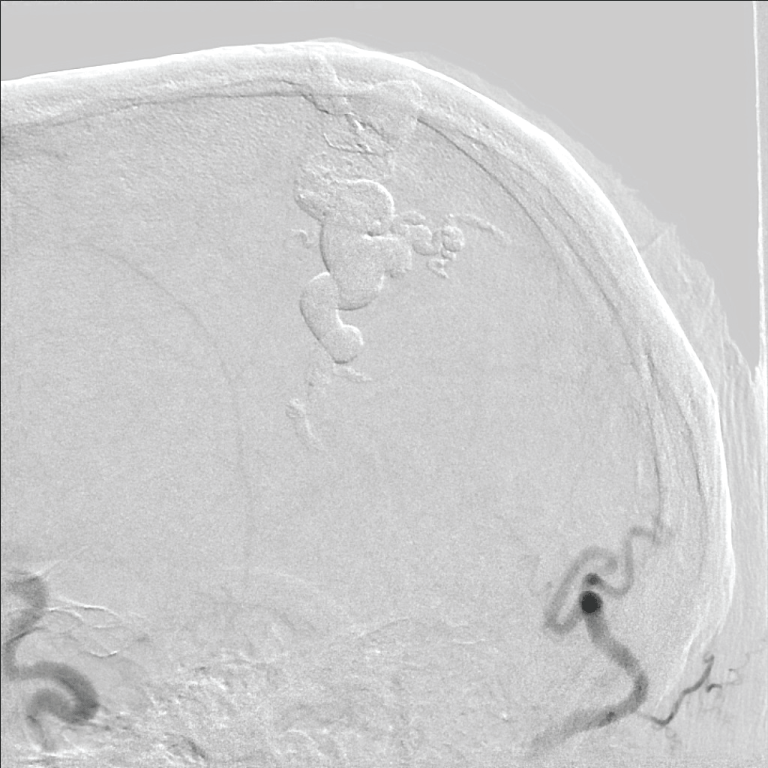 Figure 3: Lateral right external carotid artery injection that demonstrates the presence of the NBCA glue cast within the dilated scalp vein (arrow) and no residual filling via previously visualized superficial temporal and occipital arteries. View Figure 3
Figure 3: Lateral right external carotid artery injection that demonstrates the presence of the NBCA glue cast within the dilated scalp vein (arrow) and no residual filling via previously visualized superficial temporal and occipital arteries. View Figure 3
Hair transplantation procedures classically involve the resection of small patches of superficial skin containing hair follicles that are then implanted into a recipient site via an incision or punch insertion. Scalp AVF is an extremely rare complication of hair transplantation and is related to direct vascular injury incurred during the procedure due to punches, needles, and/or micro-blades. The reported literature on this complication is confined primarily to single case reports, of which they are currently 15 available in the Medline database.
Every year 225,000 hair transplant procedures are performed worldwide [17]. In a single institution review of 533 cases of hair transplant procedures Salanitri, et al. reported a 4.7% risk of all complications [17] interestingly, no scalp AVFs were reported. In general, the complications of hair transplantation are often minimal or transient and may include pain, pruritis, scalp edema, hypoesthesia, hematoma development, and of greater concern, scalp necrosis, and osteomyelitis [18,19]. It is important to note that as the techniques of surgical hair restoration therapy have evolved, there has been a sharp decline in the incidence of complications [20]. In fact, scalp AVF following hair transplantation has only been described in cases where the classic punch-graft technique was utilized [3,4,6-14].
The etiology of AVF following punch-graft hair transplantation likely owes to direct traumatic injury of the superficial vasculature during the procedure. Mini-micro-grafting and other newer methods of hair transplantation, including follicular unit transplantation, result in far less scalp trauma, and thereby a much-decreased risk of complications that likely include scalp AVF [20].
Table 1 outlines the characteristics of each case report of scalp AVF following hair transplantation since first reported in 1970 [12].
Table 1: Demographics, AVF characteristics, treatment, and outcomes for 16 patients with scalp AVFs due to Hair Transplantation. View Table 1
Patients' age ranged between 26 and 64 years. The time from hair transplantation to presentation for treatment evaluation ranged anywhere from approximately one month after the procedure to 15 years following transplantation. Similarly, the time from transplant to onset of initial symptoms could be as early as three weeks or up to several years after the procedure. Patients' chief complaints often included a swollen, pulsatile scalp mass, headaches, and/or pulsatile tinnitus. Physical findings commonly include dilated scalp veins, with a murmur or thrill upon auscultation and palpation [4]. Definitive diagnosis is made via angiography with the majority of lesions originating from branches of the STA, often bilaterally, and draining into one or more dilated superficial scalp veins.
As endovascular techniques and materials have evolved over the years, there has been a clear progression in the management strategy of these lesions toward embolization and away from surgery (Table 1). Current endovascular options offer the benefit of a minimally invasive approach that allows for simultaneous diagnosis and treatment. Complete obliteration of these lesions requires that the fistulous point be the primary target for embolization. This point may be accessed transarterially or directly through the scalp under fluoroscopic guidance in order to deliver the embolization material. In cases where tortuosity of the feeding vessels limit access to the fistulous point, direct puncture embolization is a safe and effective alternative [5,10]. We opted for this route and used an inverted plastic cup to apply circumferential pressure to the scalp in order to impede both arterial inflow and venous drainage while the AVF was slowly filled with NBCA glue. A similar method was previously described by Mathis, et al. in 1994 [10]. Regardless of the method chosen, all surgical and endovascular interventions have resulted in a 100% resolution rate, with no recurrences reported. One important limitation to our reported case and likely the majority of other reports is that it is hard to know for certain whether these AVF's were not present prior to the hair transplantation procedure. This is however unlikely given the presenting symptoms and, in some cases, physical deformity.
Hair transplantation procedures, while generally carrying a very low risk profile, may occasionally lead to scalp arteriovenous fistulae. Both open surgical and endovascular interventions are generally safe and successful in the definitive treatment of these lesions. Special attention to the anatomy of the fistula should be given when deciding on the optimal treatment strategy. Post-intervention appearance should also be a consideration, as surgical intervention will leave a scar and glue embolization leaves a subcutaneous mass.
None.