Telemedicine in wound care allows the general practitioner to communicate with the specialist via telecommunications in co-managing the patients' wounds thus effectively reducing the wait for specialist, allowing patients to get treated faster. As patients with complicated wounds increased, the demand for specialist wound care advice increased. To better manage our patients with chronic wound conditions, there is a need to source out new modalities in wound care management. Though there were many studies done on telecommunications in wound care, a review was necessary as the outcomes measured varied widely with inconsistent evidence on its clinical effectiveness. The aim of this review was to evaluate whether the use of telemedicine for distant wound care advice was effective in improving wound outcomes through meta-analysis of the combined trials.
Database searches were performed in Medline, EMBASE and CINAHL. Study methodologies were assessed using Cochrane Collaboration risk-of-bias tool and JBI-MASTARI.
4 randomized controlled trials and before-and-after studies involving 274 wounds were involved in the meta-analysis and studies were of low to moderate risk of bias. The combined trial of 3 studies comprising 229 wounds evaluating wound healing rates showed significant improvement in wound healing (RR 1.50, CI 1.06 to 2.13, p = 0.02). However, there was no significant change in wound size (MD 3.86, CI 5.04 to12.75, p = 0.40).
Our review suggests that the use of telemedicine in wound care could effectively improve wound healing rate but not the change in wound size. Hence, more randomized controlled trials are still needed to prove its effectiveness in the clinical area.
Telemedicine, Wound care, Review, Patient outcomes, Wound healing rate, Wound size
The advancement in telecommunications and development in telemedicine offer promising potential for setting up tele-wound care program. Telemedicine, a provision of healthcare consultation and education using telecommunication networks to communicate information, has existed for more than 30 years [1]. In wound care, this could be done as a direct means of consultation which allows patient to receive consultation directly with the wound care specialist via telecommunications thus eliminating the need for conventional face-to-face visits. It could also be done as an indirect consultation where the general practitioner communicates with the specialist in co-managing the patients' wounds thus effectively reducing the wait for specialist, allowing patients to get treated faster. Store and forward and real-time video conferencing are the two common modalities in telemedicine in wound care.
As Singapore enters an ageing and affluent society, the number of chronic complicated wounds has risen substantially. Elderly population had grown steadily from 7.8% in 2002 to 11.7% in 2013 [2] and diabetic population had increased from 8.2% in 2004 to 11.3% in 2010 [3]. Elderly tend to have significant co-morbidity and are more likely to be on poly pharmacy which could impact wound healing [4]. Diabetic patients have poorer wound healing process due to the poorer blood circulation to wound site, proneness to infection and presence of neuropathy [4].
In our polyclinics, the number of complex wound cases have increased steadily from 46% in 2012 to 55% in 2014 and this percentage is expected to increase in the coming years, propelling the demand for specialist wound care advice. To better manage our patients with chronic wound conditions, there is a need to source out new modalities in wound care management.
Many studies were done on evaluating telemedicine in wound care as an indirect means of wound consultation however the measured outcomes varied widely in these studies with inconsistent evidence on its clinical effectiveness thus necessitating a review.
The aim of this review was to evaluate whether the use of telemedicine for distant wound care advice was effective in improving wound outcomes through meta-analysis of the combined trials.
A search was performed in the following bibliographic databases for relevant articles from inception to September 2015: CINAHL Plus with Full Text, EBSCO Medline Complete, OVID EMBASE. We developed a search strategy for CINAHL Plus with Full Text and adapted it to other databases. Key search words were “tele-wound care̵, “tele-medicine̵, “chronic wound̵, “leg ulcer̵, “wound management̵ and “wound care̵. Relevant articles were retrieved full-text and reference lists of these articles were reviewed to avoid missing any studies. A search performed in the grey literature, specifically the Open Grey data base, revealed no relevant articles. Due to limitations in time and resources, we did not perform any hand-searches of key journals. To minimize language bias, relevant articles published originally in other languages other than English were also included but these articles had to be translated to English language from the original language, either by the database or foreign language translator. A copy of the CINAHL Plus with Full Text search strategy was attached in the Table 1.
Table 1: Search strategy for CINAHL PLUS with full text (last run on 22.9.15). View Table 1
Primary studies with the following design characteristics were included:
(a) Population
• Participants above 18 years of age
• Participants with any type of wounds requiring wound management
(b) Intervention
• Store and forward modality between wound expert and general professional
• Real time video conferencing between wound expert and general professional
• Generating images using mobile phone then transmit image to expert via email
We excluded studies with direct patient consultation because the purpose of the review was to assess the effectiveness of using telecommunication between a professional wound expert and a general trained professional in providing distant wound care advice.
(c) Comparison
• Standard wound care management
• Face-to-face wound care management
(d) Outcomes
• Wound healing rates
• Wound condition
• Symptom control
• Patient satisfaction rates
We excluded studies with outcomes that evaluated the agreement and accuracy between face to face and remote wound assessment/management. Studies with outcomes that measured the healthcare professionals' satisfaction rates and confidence level with the use of tele-medicine were also excluded. This review was directed towards patient outcome and not a review of feasibility thus the exclusion of the above outcomes.
(e) Study design
• Randomized controlled trial
• Pilot randomized controlled trial
• Non-randomized trials
• Controlled before-after studies
• Prospective cohort studies with a comparison of treated and non-treated groups
We included studies reported in peer reviewed publications and excluded conference abstracts and posters. As this review was assessing the effectiveness of intervention, experimental studies were the best study design to answer this question but in view of the difficulty in implementing experimental trial for this topic of interest, we anticipated that many of these studies were observational study hence we included observational studies that were of higher hierarchy. We excluded studies using case control and case studies because these study designs were inappropriate to address the review question.
GLJ and ZXL independently performed searches in all three databases using the search strategy. All titles and abstracts of the identified articles were independently screened through the first literature search. Full texts of the relevant articles were then retrieved and assessed for eligibility. GLJ and ZXL independently read the articles to identify studies to be included in the review. The reference lists of the included studies were then examined to identify any potential studies that were left out. There was moderate agreement between the two reviewers (Cohen kappa = 0.448). In cases of uncertainty or discrepancies between the reviewers, a discussion was arranged to reach consensus.
A data extraction form was developed to record the relevant study characteristics and this form was piloted on at least one study in the review. Data extracted from the included studies were: study design, population characteristics, setting, intervention and control group characteristics, outcome characteristics and results. GLJ and ZXL independently filled in the data extraction form and any discrepancies between the reviewers were discussed to reach a consensus.
GLJ and ZXL independently assessed the risk of bias in the included studies. RCTs were assessed using Cochrane Collaboration risk-of-bias tool for randomized trials and studies were assessed to evaluate whether there were random sequence generator; allocation concealment; blinding of participant, personnel and outcome assessor; incomplete outcome data; and selective reporting. Non-randomized and observational studies were assessed using JBI-MASTARI and these studies were assessed to evaluate whether there was bias due to confounding; selection of participants into study; measurement of interventions; departures from intended interventions; missing data; measurement of outcomes; and selection of reported result. Any disagreements in quality assessment were resolved by discussion.
For continuous variable, the Standardized Mean Difference (SMD) with 95% confidence interval was computed whereas for dichotomous variables, the risk ratio (RR) with 95% confidence interval was computed. Chi-square test was used to test for heterogeneity across studies and p < 0.1 indicated heterogeneity. When studies showed heterogeneity, I2 would be used to measure the variability present due to heterogeneity rather than chance. I2 values of 25%, 50% and 75% were used to denote low, moderate, and high heterogeneity. Investigations would then be conducted to explain the heterogeneity. For homogenous studies, fixed effects model was used to calculate the pooled treatment effect estimates. When there is obvious heterogeneity and adequate support for heterogeneity, random effects model would be used. Meta-analysis was performed using Review Manager (RevMan 5.3) and a forest plot would be illustrated. When meta-analysis could not be performed for the combined studies, the data would be presented in a narrative form.
2019 records were identified through the database searches. After screening through the abstract and title, only 118 articles were viewed as relevant. Of these, 52 articles were excluded because of duplicates and the inability to retrieve for full-text. 66 full-text articles were retrieved for detailed examination and of these, 60 articles were excluded because they did not fit the eligibility criteria (Table 2). 6 articles were evaluated for methodological quality and one study was excluded as the intervention deviated from the aim of this review. In total, 5 articles were considered for the systematic review but only 4 articles were included in the meta-analysis (Table 3, Prisma flowchart).
Table 2. Table for exclusion of studies for not meeting eligibility criteria. View Table 2
Table 3.Prisma flowchart. View Table 3
Table 4 provides a table describing the characteristics of the 5 included studies. There were three randomized controlled trial, one cluster controlled trial and one before and after study. In the cluster controlled trial, randomization was not done due to ethical issues. Altogether, these trials evaluated the wound outcomes in 300 patients involving 375 wounds and this was excluding subjects in Group B in one of the studies because these subjects were neither considered to be in the interventional group nor the control group [5]. Due to inadequate data in one study, only 207 patients involving 282 wounds were considered for meta-analysis [6]. However out of the 282 wounds, 8 were not included in the meta-analysis as patients either died, lost to follow up or withdrew from the study resulting in only 274 wounds analyzed. These studies took place in Austria, Australia, UK, USA and Denmark. Wounds that were included in these studies were non-healing wounds, stasis wounds, leg ulcers, foot ulcers and pressure ulcers.
Table 4. Characteristics of included studies. View Table 4
The interventions in these studies involved having the home care nurses sending digital images electronically to the remote wound care experts weekly or every 2 weeks. The home care nurses would then act upon the instructions of the wound care experts to manage the patients' wounds. In the control group, the home care nurses solely managed the patients' wound and would refer the patients to the wound care experts only when they assessed that it was necessary.
Healing rate was much better in the interventional group in 3 out of the 4 studies. In 2 studies, wound improved or completely healed in 70% of patients in the interventional group while only 18%-45% of the wounds were improved or completely healed in the control group [7,8]. The interventional group had wounds healed 11.7% faster than the control group [4]. In the before and after study, 71% of the wounds improved after 3 months of intervention [9]. These results were in contrast with one study where 88% of the wounds in the control group improved or healed and this was 3% more than in the interventional group [5]. The interventional group also took 16 days slower to heal than the control group [5].
Only 2 studies evaluated the amount of change in wound size. In the before and after study, there was a decrease of average 3.92 cm2 in wound size 3 months after the intervention [9]. In another study, the change in wound size in the interventional group was 3.57 cm2 more than that of the control group but it was not known whether the wound size was increased or decreased in the interventional group [5].
Risks of bias in these studies were low to moderate. Randomization was done in 3 of these studies however randomization procedure was not thoroughly explained except for one study where the authors described that computer program was used to generate random sequence. Though authors did not explain how performance and detection bias was avoided, the authors mentioned that double blinding was not possible due to nature of interventions. In the controlled trial where randomization was not done, the author gave sufficient explanation and to avoid bias brought by non-randomization, several important covariates were adjusted in the results. Authors took precautions to avoid protocol deviations and control contamination and when these unfortunately occurred, the involved participants were withdrawn from the study. No bias or confounding factors were detected in the before and after study.
This systematic review showed that use of telemedicine for expert wound care advice was significant in improving wound healing rates for patients with non-healing, chronic wounds or ulcers but not significant in the change in wound size. 4 out of the 5 studies had positive results and the combined trial of 3 studies comprising 229 wounds showed significant improvement in wound healing (RR 1.50, CI 1.06 to 2.13, p = 0.02) (Forest plot 1).Wound healing was measured by the number of wounds healed at the end of the study. Fixed effect model was used in the analysis as the combined trials showed homogeneity among studies as p > 0.1 (p = 0.12), though there was moderate heterogeneity as I2 = 54%. Moderate heterogeneity was the result of one trial slightly different from the other 2 trials [5,7,8] and the authors explained that though randomization was done but by chance, the interventional group had patients with wounds significantly larger than the control group. The removal of that trial from the analysis showed that the combined trials of the 2 studies comprising 116 wounds had moderately low heterogeneity I2 = 43% with fixed effect model showing significant improvement in wound healing (RR 1.80, CI 1.23 to 2.63, p = 0.002) (Forest plot 2). The combined trial of 2 studies that evaluated change in wound size showed no significant change in the wound size (MD 3.86, CI 5.04 to 12.75, p = 0.40) (Forest plot 3) [9]. Fixed effect model was used as there was no differences between the studies (I2 = 0%, p = 0.98).
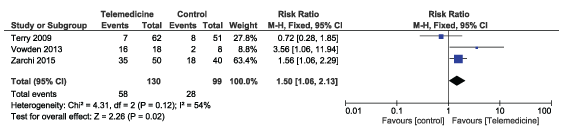 Forest Plot 1: Wound healing rate in the combined trial of 3 studies. View Forest Plot 1
Forest Plot 1: Wound healing rate in the combined trial of 3 studies. View Forest Plot 1
 Forest Plot 2: Wound healing rate in the 2 studies after removal of a slightly different study. View Forest Plot 2
Forest Plot 2: Wound healing rate in the 2 studies after removal of a slightly different study. View Forest Plot 2
 Forest Plot 3: Change in wound size (cm2). View Forest Plot 3
Forest Plot 3: Change in wound size (cm2). View Forest Plot 3
A weakness in this systematic review was due to the mix of study designs used in the meta-analysis. However, this paper provided insights on how telemedicine helped in improving wound healing rates. More randomized trials are still needed to evaluate the effectiveness of telemedicine in wound care. However, understandably, there are a lot of limitations in implementing such trials since telemedicine as an intervention costs a lot in the equipment and requires lots of resources in staff training. Hence, most randomized controlled trials were done in small scale. Study protocol should ensure appropriate randomization and measures should be taken to prevent bias so that good quality randomized controlled trial could be combined together to achieve a more significant outcome.
There were many trials evaluating feasibility of telemedicine in wound care however limited in evaluating patient and clinical outcomes. These trials had shown that there was good agreement between wound images sent via telecommunications and seeing the wound in person hence the next step of advancing research in the area of telemedicine in wound care would be evaluating on patient and clinical outcomes.
Telemedicine in wound care could be implemented in areas where there were limited access to wound care specialist. In conventional face to face consults, patients either have to wait for their appointment to see wound care specialist or the wound care specialist has to make a trip to see the patient for those with mobility difficulties. Both of which, resulted in long waiting time to get advice from the wound care specialist. In our clinical area, telemedicine would prove to be useful in gaining faster advice from wound care specialist. The community or homecare nurse could communicate with the wound care nurse specialist to get her recommendations in managing patients' wounds. Two surveys done in 2010 found that 93% to 100% of general practitioners agreed that telemedicine wound care consult was a useful tool in their practice and were satisfied with the telemedicine consult service [10,11]. An observational study found that 98.2% of patients were satisfied with the care using telemedicine [12].
Telemedicine in wound care allowed the patient to gain faster wound care advice from the specialist and this logically would translate into faster wound healing rate. The result of this systematic review had proven that telemedicine in wound care indeed improved wound healing rate. However, whether it helped in reducing the wound size in a given period remained inconclusive hence more randomized controlled trial should be done in evaluating clinical outcomes to prove its effectiveness in the clinical settings.
As we move towards delivering quality healthcare, patient-centered care, involving patients in decision making and working alongside with them, becomes important. Thus, future research should not just focus on the clinical aspect of the intervention but also incorporate patient outcomes such as patient satisfaction or patients perceptions' of using telemedicine in wound care in the study.
Special thanks to the Department of Nursing, NHGP Singapore for the tremendous support given in completing this systematic review.