Primary isolated bladder lymphoma represents around 0.2% of all extranodal Non-Hodgkin-Lymphoma and less than 1% of all bladder tumours. Clinical representation may be unspecific and correct diagnosis is essential for the appropriate treatment. We expose the case of a patient with a primary B-cell bladder lymphoma with normal cystoscopy.
A 67-year-old patient presented with lower urinary tract infections, overactive bladder with urinary incontinence as well as haematuria susceptible for bladder carcinoma. Urine sediment, cytologie, abdominal- and kidney ultrasound as well as a CT scan did not lead to a conclusive diagnosis. Surprisingly, cystoscopy did not demonstrate any tumourous lesions and urine cytology revealed free of malignant cells. Cold four-quadrant cut biopsies finally did reveal the presence of a primary B-cell lymphoma. After a four weeks' antibody treatment of Rituximab (Mabthera) the patient showed subjective improvement and lower urinary tract symptoms disappeared. Clinical follow-up as well as repeat cystoscopic biopsies were undertaken every six months. After a follow-up period of nearly three years the patient is still in complete remission. Urinary tract infections and incontinence as well as OAB symptoms disappeared entirely.
Haematuria was the main clinical finding in the current case of primary bladder lymphoma. Uneventful radiologic examinations lead to the necessity of bladder biopsies without any macroscopic pathologic findings. We present the exceedingly rare case of a primary bladder lymphoma without any characteristic lesions in the bladder lumen. For this reason, cystoscopic four quadrant biopsies should be used largely. Biopsies are essential leading to the correct diagnosis and finally successful treatment. Single antibody therapy with Rituximab is an option in selected cases as the one presented and can be used as un therapeutic option.
Bladder lymphoma, Cystoscopy, Overactive bladder, Urinary tract infections, Rituximab
BMI: Body Mass Index; CHOP: Cyclophosphamide Doxorubicin Vincristine Prednisone; CT-Scan: Computerized Tomography Scan; DLBCL: Diffuse Low B-Cell Lymphomas; FISH: Fluorescence In Situ Hybridization; GI Tract: Gastrointestinal Tract; MALT: Mucosa Associated Lymphoid Tissue; NHL: Non-Hodgkin’s Lymphomal; Pet-Scan: Positron Emission Tomography Scan; R-CHOP: Rituximab Cyclophosphamide Daunorubicin Vincristine Prednisolone; TURBT: Transurethral Resection of Bladder Tumour
Primary lymphoma of the bladder is rare. It constitutes 5% of the nonurothelial tumour of the urinary tract [1] Primary isolated bladder lymphoma represents only 0.2% of all extranodal Non-Hodgkin-Lymphoma and less than 1% of all bladder tumours [2,3]. Of primary lymphomas of the bladder, mucosa associated lymphoid tissue lymphoma, or MALT, is the most prevalent histological subtype. Till today little more than 100 cases have been reported. The clinical, radiological and endoscopic representation may be unspecific which conducts to the fact that diagnostic features may not be well known by the unaccustomed practitioner. The diagnosis is exclusively histological. Furthermore, the optimal treatment of primary MALT confined to the bladder remains to be defined.
We expose the rare case of a primary B-cell bladder lymphoma (Malt-type), treated with Rituximab and a review of the appropriate literature.
We want to share this rare case with its unspecific clinical symptoms in order to alert our colleagues to the important role of biopsy in prompt diagnosis. We emphasize on the high index of suspicion required to identify such cases at an early stage, which has pronounced prognostic implications.
A 67-years-old female presented with a history of a couple of months lasting asthenia, inappetence weight loss of 5 kg in one-year, recurrent lower urinary tract infections which were commonly treated by antibiotics, lower abdominal pain, overactive bladder with urinary incontinence and a two-week lasting macroscopic haemorrhagic cystitis which did not disappear after eradication of an Escherichia coli infection. No other underlying medical conditions were known. On examination, the woman was sallow, abdominal palpation was physiologic, neither organomegaly nor lymphadenopathy could be found.
Urine culture showed sterile pyuria. Urine sediment, urine cytology, a complete blood count, biochemical analyse of renal function and abdominal- and kidney ultrasound as well as a computertomographie didn't give any hint of the underlying pathology. Rigid cystoscopy showed signs of chronic infections and bleeding bladder walls (Figure 1). Only cystoscopic four quadrant biopsies could reveal the diagnosis: Histopathology features were those of a non-Hodgkin's lymphoma, compatible with an extranodal low malignant marginal zone B-cell lymphoma of mucosa-associated lymphoid tissue (MALT lymphoma, WHO classification of 2008) [1] based on chronic cystitis. Cells were positive for CD20. Laboratory evaluation including protein electrophoresis was all within normal limits.
 Figure 1: Initial Cystoscopy with signs of chronic infection and bleeding bladder walls but without any tumourous lesion. View Figure 1
Figure 1: Initial Cystoscopy with signs of chronic infection and bleeding bladder walls but without any tumourous lesion. View Figure 1
Subsequently, a PET-CT scan of the abdomen and pelvis was performed, which revealed diffusely thickened bladder walls with a moderate uptake of the bladder (Figure 2). There was no sign of paravesical fat infiltration and no pelvic or abdominal lymph node enlargement or any other anomaly. Due to the highly invasive nature of the tumour, bone marrow biopsy was performed. It showed no evidence of leukaemia or lymphoma.
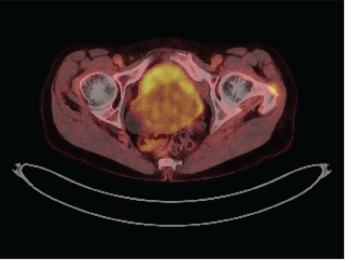 Figure 2: Pet-Scan revealed diffuse thickened, metabolic active bladder walls. View Figure 2
Figure 2: Pet-Scan revealed diffuse thickened, metabolic active bladder walls. View Figure 2
After a 4-week lasting antibody treatment once a week with Rituximab (Mabthera) 375 mg/m2 patient felt better and lower abdominal pain disappeared. Clinical controls combined with Cystoscopic biopsies and pelvic CT-scans were undertaken every 6 months for two years and later on once a year.
After a follow-up period of nearly three years our patient is still in complete remission. Haematuria, urinary tract infections and overactive bladder associated incontinence disappeared totally.
Primary lymphoma of the bladder is an exceeding rare malignancy. Its rarity and symptoms common for chronic cystitis often delay its diagnosis. Data to guide therapy is limited.
Bladder lymphoma was first described in 1985 by Eve and Chaffey [2]. Just over 100 cases have been reported since. Extranodal marginal zone lymphoma of mucosa associated lymphoid tissue type (MALT-type lymphoma) of the urinary bladder, first described in 1990, is the most common primary bladder lymphoma [2,4,5]. On histology most, cases are low-grade lymphomas [6]. B-cell bladder lymphomas are more frequently seen than T-cell ones [5]. Kempton, et al. found out that only 6 of all documented bladder lymphomas registered between 1940 to 1996 in the Mayo tissue registry are primary [4].
The rare occurrence of this neoplasm is a consequence of the fact that there are no germinal follicles or lymphoid tissue developing in the urinary bladder itself [7]. Hereby, the aetiology of such malignancies remains unknown. The MALT concept provides a mechanism by which malignant lymphomas could develop in the bladder and in other sites of the body that normally possess no lymphoid tissue, after long-standing antigenic stimulation by bacterial infection [8-10]. As such, patients often present, like the here exposed case, with symptoms of chronic cystitis [5,11-13]. This theory is supported by the fact that lymphoepithelial lesions are seen in MALT lymphoma [9-14]. However, cases in which chronic cystitis and histological inflammation are lacking have been cited [7,11,14]. The base for disease development in these cases is still unknown. Other authors have raised the possibility of a residual embryonic cloaca, from which the bladder derives, source lymphoid proliferation in adulthood [15].
Female preponderance for illness is preeminent [6,7,11-13], which is contrary to the male predominance of primary urinary bladder carcinoma [16]. MALT-lymphoma of the bladder may be more frequent in female potentially as a result of increased incidence of chronic cystitis in women. The disease typically presents in the 6th decade of life with a mean age at presentation of 64 years [4-6,12].
Our patient presented the typical most common symptoms of lymphoma of the urinary bladder: Macroscopic haematuria (present in 61% [5]) and signs of bladder irritation (dysuria, nycturia, urinary frequency, and suprapubic or abdominal pain [4,6,11,13]) combined with weight loss, fatigue and recurrent urinary tract infections.
Bladder lymphoma presents at imaging in 70% as a solitary submucosal mass and, less commonly, as multiple masses (20%) or diffuse bladder wall thickening (10%) [17]. The location is most often centred in the dome or lateral walls of the urinary bladder [17]. It usually involves the submucosa without mucosal ulceration [18]. The radiologic findings are nonspecific and do not permit to differentiate from other bladder neoplasms by imaging alone [19]. Diagnosis relies on cystoscopic biopsies, and a thorough pathologic evaluation of biopsied tissue [20].
MALT lymphomas of the bladder, in common with those at other sites, generally carry a good prognosis and have little tendency to disseminate to non-MALT lymphoid organs. Nevertheless, dissemination or to transform into higher grade DLBCL [21] is possible, implying that an early diagnosis of the MALT lymphoma is important for improved prognosis [22].
On cystoscopy, these tumours are visualized as well defined intravesicular masses typically located at the dome, retro-trigonal or the lateral walls of the bladder [20,23]. An oedematous, haemorrhagic or friable mucosa may be associated [13]. Ulcerous lesions may be present [20].
Pathological analysis should include immunohistochemical staining, FISH testing, and microscopic evaluation of the tumor grade [7,24]. The B-cell lymphoma is characterized by a proliferation of atypical monomorphic lymphoid cells. Differential diagnosis with poorly differentiated carcinoma; melanoma, Burkitt's and Hodgkin's lymphoma may be throw out using the immunohistochemical panel. FISH testing permits to detect the three main types of B cell derived Non Hodgkin's Lymphoma (NHL) with strongly associated FISH test abnormalities: Burkitt's lymphoma t (8:14) translocation of MYC gene, mantle cell lymphoma t (11:14) translocation of cyclin D1 gene, and follicular lymphoma t (14:18) translocation of BCL 2 gene. Absence of any of these translocations does not exclude diagnosis as they are not present in 100% of cases [25]. All B cell type lymphomas are CD20 positive in immunhistochemical testing [17]. Low grade lymphomas routinely test positive for CD20, CD21, and CD43 cell markers, while high grade lymphomas are correlated with CD3, CD20, and CD30 cell markers [14]. Lymphomas of the urinary bladder stain negatively with Pan-keratin, vimentin, CK20, and CK7 [17].
Once the type of bladder lymphoma has been identified, differentiation between an indolent, low grade neoplasm versus an aggressive, high grade malignancy is important in order to initiate the most appropriate treatment regimen for that patient. The average age at diagnosis of high grade lymphoma is 10 years younger than that of low grade ones [7]. Aggressive high-grade lymphoma without treatment leaves the patient with a prognosis of a matter of months [26].
Staging becomes of utmost importance. It should eliminate the presence of any other lesions to confirm the primary origin of the bladder lymphoma. It must include hole body PET-scan and bone marrow biopsy [2,27].
Common used treatment options for non gastric MALT lymphomas are:
I. Observation (based on factors such as patient age, risk factors, other underlying medical problems and tumour grade) [9].
II. Surgery (complete excision or biopsy) [28].
III. Radiation (radiation, when given alone or after an excisional biopsy, has shown excellent local control and improved overall disease-free survival) [17,29].
IV. Chemotherapy (usually used when a patient presents with systemic involvement or secondary lymphoma of the bladder) [10,30].
V. Targeted antibody therapy (by the anti-CD20 antibody rituximab) has been used along with other modalities in systemic lymphomas [10,30,31].
VI. Antibiotics (they are usually used in presence of a known bacterial origin for chronic infections, e.g. Helicobacter Pylori in the stomach). There have been rare cases where antibiotics were used for MALT lymphomas of the bladder [5,32]. Probably the prosperity of this treatment can be explained with the lymphoma development on an underlying chronic cystitis.
No treatment recommendations based on lesion size have been published. For this reason, Simpson, et al. [7] proposed recently to use the following criteria set for other bladder tumours:
➢ TURBT has proven effective in urothelial bladder cancer that has yet to invade the musclaris propria (stage Ta, Tis, and T1).
➢ Radiation alone proved to be successful in only 66% (2 of 3) cases.
➢ As for the type of chemotherapy different regimens were successfully used treating low grade bladder lymphomas [7]; CHOP was reported by the literature to be the most frequently applied [5,15,20,28]. It has documented success in treating both low and high grade primary bladder lymphomas as either solitary treatment or combination therapy [15]. The addition of rituximab in cases of CD20 positivity should be systematic due to the therapeutic benefit provided by this monoclonal antibody in this situation [10,28,33].
As low-grade lymphomas are highly radiosensitive and the disease-free outcome is very good [6] Vempati, et al. concluded that radiotherapy is the most appropriate treatment for localized disease [34] in order to achieve organ preservation. For patients at reproductive age, the authors postulated to use maximal surgical resection with the aim to preserve fertility as radiation of the bladder may be harmful to the proximal reproductive organs [34].
Chemotherapy and rituximab are often used for secondary, recurrent, or disseminated disease [10]. In summary the treatment is not well defined [35] and the prognosis remains unknown [20,28].
The current patient presented local infiltration of the bladder. Surgical excision would have meant bladder excision and did not present an option. Local radiation would have been a possibility. Rituximab targets the CD 20 cell surface protein, present on B-cells and on most B-cell malignancies. Its various effects are: Cell lysis, antibody dependant cellular cytotoxicity and induction of apoptosis [33,36]. As a single agent therapy Rituximab has been shown effective in DLBCL treatment [37]. Finally, based on own experiences with antibody monotherapy in primary lymphoma of other organs, our oncological tumour board proposed a monotherapy with Rituximab.
This is at our knowledge the first published report of a monotherapy with Rituximab as first line single-agent therapy of a primary low-grade MALT lymphoma of the bladder.
The optimal follow-up strategy for patients with lymphoma of the bladder remains unknown [34]. Our patient was followed clinically, combined with urine cytology, rigid cystoscopy and four quadrant biopsies and pelvic scans every six months for two years and later on once a year, as it is recommended for transitional cell carcinoma. Nearly 3 years after the initial diagnosis she is still in complete remission. The prognosis is difficult to be determined given the rarity of primary NHL of the bladder. In concordance to the literature we hope and expect long term survival without remission [4,5,7,13,14].
In conclusion, primary low-grade MALT lymphoma of the bladder represents a rare malignancy with excellent prognosis if detected at an early stage [5,7,13,14,38]. For this reason, practitioners should know about this entity and its presentation. Four quadrant cystoscopic biopsy must be used without hesitation after exclusion of other underlying causes. Early diagnosis implies excellent prognosis and increased patient survival. For early stage disease, antibody treatment alone with Rituximab presents nearly no side-effect profile [10,34,37,39] and may be considered as an option for local disease treatment as an alternative to radiotherapy or excision. A second line chemotherapy or radiotherapy may be indicated in cases of locoregional recurrence. Treatment standardisation is difficult because of the few cases worldwide. Other reports of experiences with this treatment are crucial.
We thank Dr. Etienne Combaz for his support and technical assistance.
The authors declare that they have no competing of interest.
All authors have made significant contributions by making diagnosis, treatment and intellectual input in this study and writing the manuscript. All authors read and approved the final manuscript.