We report the case of a 23-years-old female dental medicine student with contact dermatitis on her hands caused by methacrylates. Forty-eight-hour closed patch testing showed positive reactions to Ethylene glycol dimethacrylate, 1,6-Hexanediol diacrylate, 1,4-Butanediol dimethacrylate, Drometrizole. These are identified as contact allergens. They can be found in the dental materials, but also in the nail polish. It is therefore easy to be exposed to methacrylate in daily life. We measured the skin reaction during the patch test, and noticed that the temperature of the affected skin changes. The highest value was registered when the patches were applied, and the lowest - one week after the treatment.
Patch-test, Thermo-vision, Allergic contact dermatitis, Methacrylate, Professional allergens
The allergic contact dermatitis (ACT) is the most frequent manifestation of immunotoxicity in humans [1]. The disease has a strong social and economic effect [2]. ACT is a the 4th type reaction by the classification of Coombs and Gell. The allergic reactions that we observed in patch-tests, can be measured by the temperature changes of the affected skin [3,4]. The method we applied to measure the patch test reactions, is also applicable for measurement of the intensity of the allergic reaction of the affected skin [5]. However, some studies show that the local lymph nodes are also involved in the reaction [6]. Initially we assumed that our patient's symptoms are connected with the acrylic products contained in her gel nail polish. They can be found in different products like dental composites, nail polish, artificial nails, cosmetics, adhesives, prostheses, etc [7]. There is a similarity between dental and cosmetic products - they have the same kind of methacrylate [8]. In this paper we report a case of contact dermatitis caused by methacrylate contained in different kinds of source - dental materials and cosmetic products.
We report a case of 23-years-old female, student of dental medicine, who developed dermatitis on her hands approximately one month ago, when she applied a nail gel polish in Cyprus - Clarite O.P.I. The gel nail polish is a multicomponent allergen which contains. In the past there were four times of exposure to gel nail polish, but the product have been different. When she was in Cyprus, she visited a dermatologist who put the diagnosis "Allergic contact dermatitis", and advised the patient to make a patch test. Her hands developed xerotic skin, erythema, papules and itching. When she returns back to Sofia, she starts working with dental materials, mainly with Spofadental - Duracryl™ Plus. The gel nail polish and the dental materials have some common allergens - Methyl methacrylate, Bisphenol A dimethacrylate, Ethylene glycol dimethacrylate, 1,6-Hexanediol diacrylate [8]. On Figure 1 and Figure 2 we see the affected skin of the palms.
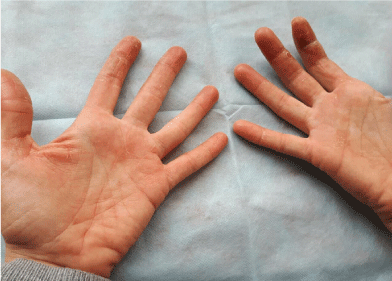 Figure 1: The palms affected by the allergic contact dermatitis.
View Figure 1
Figure 1: The palms affected by the allergic contact dermatitis.
View Figure 1
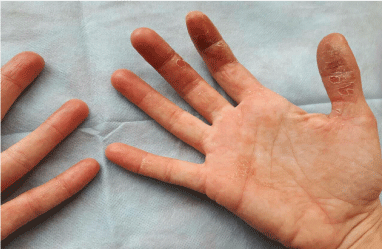 Figure 2: The palms affected by the allergic contact dermatitis.
View Figure 2
Figure 2: The palms affected by the allergic contact dermatitis.
View Figure 2
In order to identify the dermatitis cause, we carried out a patch test (on the patient's back) for the most suspicious allergens by the Chemotechnique diagnostics - Dental Screening Series DS-1000, and allergens from the Bulgarian dental allergens produced in the National centre of infectious and parasitic diseases. For patches we use IQ Ultimate™. The patch test performance and the results assessment were based on the ICDRG (International Contact Dermatitis Research Group) criteria. The results are presented in Figure 3 in Table 1.
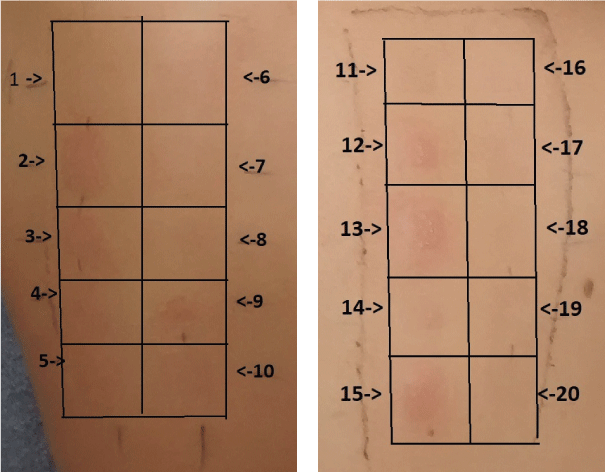 Figure 3: Pictures of the patient's back at the moment of patch test results checking. View Figure 3
Figure 3: Pictures of the patient's back at the moment of patch test results checking. View Figure 3
Table 1: Results from the Patch test. View Table 1
We have positive reactions for two of the common allergens: Ethylene glycol dimethacrylate and 1,6-Hexanediol diacrylate.
In order to assess the allergic inflammation status we measured the temperature of the affected areas three times: Before the patch test; on the day when we read the result; and one week later. These measurements were performed with FLIR T620 thermo-camera with resolution 0.06 degrees and software Flir Reporter Professional software 2013. We accept for significant any temperature change for more than 0.4 degrees between first and last monitoring of identical areas of the skin. The thermovision is performed in a special room for this in the Faculty of dental medicine - Sofia. The temperature there is 22 ± 2 degrees, the humidity 40%, no movement of air with more of 1.0 meters/sec, distance between the camera and the patient from 0.3 to 2 meters, no thermal radiation open sources [9]. The temperatures we detected are summarized in Table 2. On Figure 4, Figure 5 and Figure 6 we show the thermos-vision pictures of the hands. Figure 7 and Figure 8 present a comparison between the temperatures of the different fingers and Figure 9 - the average temperatures of the three measurements.
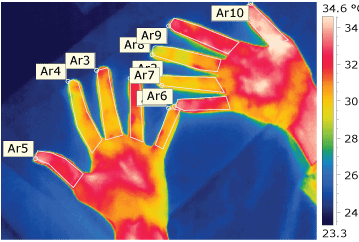 Figure 4: Thermo-vision picture of the hands before the patch test.
View Figure 4
Figure 4: Thermo-vision picture of the hands before the patch test.
View Figure 4
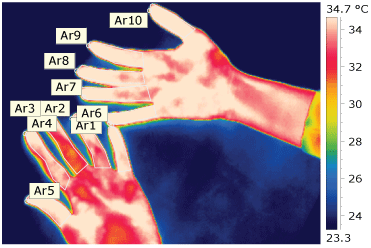 Figure 5: Thermo-vision picture of the hands in the day of the patch test reading. View Figure 5
Figure 5: Thermo-vision picture of the hands in the day of the patch test reading. View Figure 5
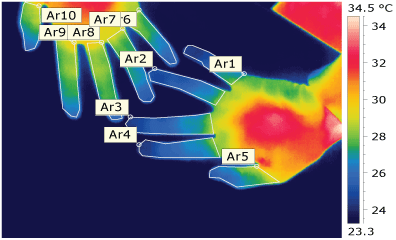 Figure 6: Thermo-vision picture one week after the beginning of the treatment. View Figure 6
Figure 6: Thermo-vision picture one week after the beginning of the treatment. View Figure 6
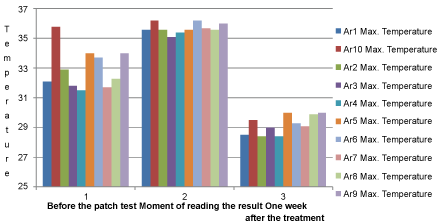 Figure 7: Maximal temperatures of the explored areas.
View Figure 7
Figure 7: Maximal temperatures of the explored areas.
View Figure 7
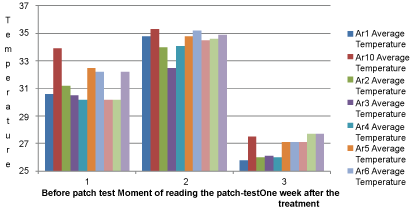 Figure 8: Average temperatures of the explored areas.
View Figure 8
Figure 8: Average temperatures of the explored areas.
View Figure 8
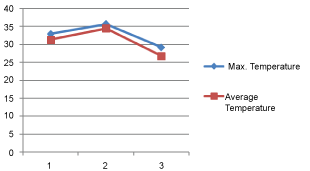 Figure 9: The change of the maximal and average temperature at the three moments of measurement.
View Figure 9
Figure 9: The change of the maximal and average temperature at the three moments of measurement.
View Figure 9
Table 2: Maximal and average temperatures of the affected areas. View Table 2
About 8 hours after the patch application, the patient called to complain from strong itching on the place of the patch, and perioral rash. Later she visited our laboratory for patch reading, and by this time the rash had disappeared.
Treatment: The patient was informed the sources of allergens, and advised to stop any contact with them. The nail polish was removed carefully, and the contact with dental materials containing methacrylate was avoided. We prescribed a topical corticosteroid cream - Elocom - 0.1% and another cream containing urea - Linola® Urea 12% (Figure 10).
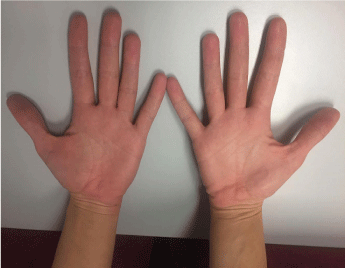 Figure 10: The palms of the patient one week after the last contact with the allergens. View Figure 10
Figure 10: The palms of the patient one week after the last contact with the allergens. View Figure 10
The patch test makes contact between the skin and allergens. Our aim was to provoke an allergic reaction, that would indicate sensibilisation of the organism. The sensibilisation to acrylic monomers is often observed in dental personal, and our patient is working with dental materials during her education [10,11]. Besides, there are cases of contact dermatitis induced by the methacrylate contained in artificial nails [12]. We also have to consider the full range of responses observed during the patch test. This includes the possibility that the results could be a result of cross reactivity or more likely a broad increase in sensitivity to all allergens as a result of compromised skin barrier condition as is a well-recognised phenomenon in dental industry [13,14].
We presume that the process has a local character. However, the impact area and borders are subject of discussion. The allergic reactions are functions of the immune system, so we can expect the whole immune system to be involved. This means that the test affects the whole organism. On the other hand, the reactions of this type is relevant to the local effects of the allergens in the place of contact. This is demonstrated by the observed skin changes.
However, we noticed increasing of the intensity of the main allergic disease - demonstrated by increase of hands temperature.
We analysed the thermovision photographs to estimate the intensity of the allergic inflammation. The temperature trend of the affected areas indicates how the disease develops. As a component of the inflammation, the rising of the temperature is a sign of exacerbation. This risk of exacerbation has to be considered every time when a patch test is performed.