Genital pustular psoriasis is a rare condition characterized by well-demarcated, clear erythematous, absence of the typical scaling which is apparent on non-genital psoriasis. We describe a 30-year-old man with pustular psoriasis limited only to the glans, he was successively misdiagnosed as balanitis, Reiter's syndrome, coinfection of genital herpes and treated with itraconazole, prednisone, valaciclovir respectively, but without control. Skin biopsy was performed, and histopathological examination showed the lesions was consistent with pustular psoriasis. The skin lesions disappeared completely after one-week application of topical corticosteroid and three weeks application of 0.1% tacrolimus. 0.1% tacrolimus was applied for maintenance and there was no recurrence observed hitherto.
Misdiagnose, Psoriasis, Pustular, Genital, Glans
Psoriasis is a common and chronic skin disorder with lesions may affect nearly all parts of the skin. However, the presentation of this disease only on genital skin is rare, and pustular psoriasis occurred solely on glans is even rare. As a result of the special location, genital psoriasis may be confused with other diseases, such as balanitis, Reiter's syndrome, and sexually transmitted diseases and so on. Treatments of psoriasis are very different from other skin disorders, so correct diagnosis is extremely important.
A 30-year-old man visited our department because of erythema and scales on the glans without itching or pain for four to five days. He was initially diagnosed as balanitis and treated with oral itraconazole (Sporanox) for one week, but without control. Then laboratory investigation indicated that Human Leucocyte Antigen B27 (HLA-B27) was positive, no fungus was found in the lesions under microscope, C-Reactive Protein (CRP) and Erythrocyte Sedimentation Rate (ESR) were within normal limits. Based on the above, the patient was suspected to be suffering from Reiter's syndrome and treated with prednisone for four days, the signs of erythema and scales on the glans disappeared. However, three days after stopping prednisone, several scattered white papules and erythema reappeared on glans, with no symptom of malaise. Laboratory examination showed that type-I Herpes Simplex Virus (HSV-I) IgG was positive and HSV-I IgM was negative. The patient was then diagnosed as coinfection of genital herpes and treated with valaciclovir but without improvement. The lesions grew progressively in size, presenting numerous flat papules on an erythematous base covered with white thick scales (Figure 1A) and one flat plaque of 0.8 cm × 1.2 cm on the glans (Figure 1B). There was no oral leukoplakia or ulcer. Skin biopsy was performed, and histopathological examination showed the lesions was consistent with pustular psoriasis (Figure 2). One-week application of topical corticosteroid (Eloson) improved the lesions substantively (Figure 3A). The skin lesions disappeared completely after three weeks application of 0.1% tacrolimus (Protopic) (Figure 3B). Thereafter, 0.1% tacrolimus instead of Eloson was applied for maintenance and there was no recurrence observed hitherto.
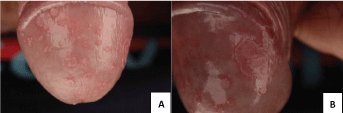 Figure 1: A) Numerous flat papules on an erythematous base covered with white thick scales; B) A flat plaque of 0.8 cm × 1.2 cm on the glans. View Figure 1
Figure 1: A) Numerous flat papules on an erythematous base covered with white thick scales; B) A flat plaque of 0.8 cm × 1.2 cm on the glans. View Figure 1
 Figure 2: Histopathological examination revealed mild hyperkeratosis and parakeratosis of epidemis, disappearance of the granular layer acanthosis and subcorneal spongiform pustules of Kogoj. Moderate density of lymphocytes were infiltrated around the vessel in the superficial dermis (HE stain). View Figure 2
Figure 2: Histopathological examination revealed mild hyperkeratosis and parakeratosis of epidemis, disappearance of the granular layer acanthosis and subcorneal spongiform pustules of Kogoj. Moderate density of lymphocytes were infiltrated around the vessel in the superficial dermis (HE stain). View Figure 2
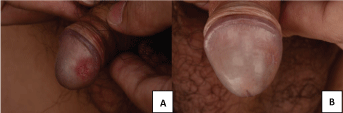 Figure 3: A) One week application of topical corticosteroid (Eloson) resulted in great improvement; B) The skin lesions disappeared completely after three weeks application of 0.1% tacrolimus (Protopic) leaving a small linear scar. View Figure 3
Figure 3: A) One week application of topical corticosteroid (Eloson) resulted in great improvement; B) The skin lesions disappeared completely after three weeks application of 0.1% tacrolimus (Protopic) leaving a small linear scar. View Figure 3
Psoriasis is a common skin disorder, which affects around 2%-5% of the population in the world [1]. Based on the morphology of the skin lesions, psoriasis has been classified into several clinical subtypes, such as plaque psoriasis, pustular psoriasis, guttate psoriasis and erythrodermic psoriasis. Based on anatomical locations, psoriasis can be classified into different phenotypes, such as genital psoriasis, scalp psoriasis, plamoplantar psoriasis, nail psoriasis and inverse psoriasis. Pustular psoriasis has been classified into localized or generalized. Genital pustular psoriasis has been reported to be part of the generalized pustular psoriasis [2]. However, pustular psoriasis located only in the genitalia can rarely been seen [2]. Here we report a rare case that pustular psoriasis limited only to the glans.
The typical characteristics of genital psoriasis is usually less obvious than non-genital psoriasis, and genital psoriasis is often characterized as well-demarcated, clear erythematous, lacking the typical scaling which is apparent on non-genital psoriasis [3]. Genital pustular psoriasis had been described by Quan [2]. They found that the patient's glans penis and distal penile scattered numerous minute, white papules and pustules on an erythematous base [2]. Here we described a man with numerous flat papules on an erythematous base covered with white thick scales. There was no obvious pustule on the glans which is different from typical non-genital pustular psoriasis.
As a result of the special location, the diagnosis of genital psoriasis should be careful and considerable. These diseases may be confused with balanoposthitis, Reiter's syndrome, and sexually transmitted diseases and so on. Balanoposthitis is common inflammatory skin disorders, which may be caused by infection and irritant, with fungus being the most frequently diagnosed [4]. In our case, there was no obviously fungal infection. In addition to balanoposthitis, the differential diagnosis for genital pustular psoriasis includes Reiter's syndrome. Reiter's syndrome is characterized by the red, pustular, and crusting papules and plaques over the hands, feet, and with similar genital lesions [5]. However, no clear other mucosal and skin disorders were present in our patient. Based on characteristics of the skin lesions on the glans and histopathological examination, our patient was diagnosed with localized pustular psoriasis occurring atypically only on the glans penis.
The cause of pustular psoriasis is complicated and not fully understood. Infection, drugs, sunlight, and pregnancy have been reported to be associated with generalized pustular psoriasis [6-8]. Psoriasis is a chronic inflammatory disease, signaling pathways of NF-κB, IFR-γ, IL-23, IL-17 and TNF-α may be involved in [9-11]. In our case, although there was no improvement to application of valaciclovir, previous infection of HSV may be a possible factor to produce psoriasis.
Treatment for psoriasis depends on whether the lesions are localized or disseminated. First-line treatment for localized psoriasis includes mild to moderate strength topical corticosteroids [12]. However, some other reports did not suggest the application of moderate strength corticosteroids for genital psoriasis and only recommend the topical use of weak strength steroids, which may be combined with vitamin D analogues [13]. Topical tacrolimus is indicated for the treatment of psoriasis based on several double-blind and open studies, especially for genital, facial, and intertriginous psoriasis [14]. Coal-tar preparations is frequently recommended to be the second most advised topical treatment for genital psoriasis. Tar may be used individually or combined with topical steroids when weak corticosteroid is insufficient [15]. Vitamin D analogues are another possible treatment for genital psoriasis, particularly male genital skin lesions [13]. Here we used moderate strength topical corticosteroid for only a short time and the improvement was great. Moreover, in our case, tacrolimus (Protopic) was proved to be effective when applied for maintenance and result in no recurrence observed hitherto.