The inherited ichthyosis correspond to abnormal keratinization of genetic origin; if events skin or nails were better individualized, the mucosal was never reported.
We report different manifestations of language observed in 33 patients with the hereditary ichthyosis.
This is a retrospective study over a period of two years: From May 2012 to April 2014, addressing all patients with inherited ichthyosis Visitors to our dermatology department at the University Hospital of Tlemcen (Algeria).
33 patients were included, divided between the different forms of hereditary ichthyosis (lamellar linked to the X keratinopathique, congenital ichthyosis form erythroderma dry). 22 of 33 patients had reached: That is to say over 66% of patients. 6 Geographical languages fissural 16 languages.
If we only take into account geographical language that is to say 6, plus the appearance of geographic tongue on fissured tongue, it makes a total of 7 of 33 patients, we have frequency of 21%, this frequency is significantly higher compared to the general population is 1 to 2.5%, more than 10% in psoriasis. Their frequency was higher in the group of congenital autosomal recessive ichthyosis.
The association more scrotal tongue geographic tongue or fissured was present in 4 cases. Taking into account language fissural, 16/33 patients we have a frequency of 48%, this rate is considerable, if compared with the frequency of the fissured language in the general population (5 to 6.5%) and also with respect to its frequency in psoriasis, which is 10 to 33%.
Over the hereditary ichthyosis examination of the genital or oral mucosa should be performed systematically since the achievement of the oral mucosa, would be even more common than in psoriasis. Similar studies will compare the results and to obtain a more objective frequency, given the size of the sample because of the rarity of the condition.
Fissured tongue, Geographic tongue, Hereditary ichthyosis
Ichthyosis is hereditary abnormalities of life-long keratinization. Clinical traits, mode of transmission and histological study allow the classification of most ichthyosis evolving without particular clinical context and those accompanying other neuropsychic, ophthalmological and other disorders. Much rarer.
This is the most frequent and is transmitted on an autosomal dominant mode. It appears from the first months of life and is manifested by flaky scales on the faces of extension of the limbs and convexities in general. The face and the large folds are respected. Palms and plants have an aged skin appearance with accentuated folds. A keratosis pilaris can associate, especially on the posterior faces of the arms.
Ichthyosis worsens in winter and improves in summer. The association with manifestations of atopy is quite frequent: Eczema, asthma and rhinitis. Histologically, it is a retention ichthyosis with no granular layer.
It affects only boys, transmitting on a recessive mode related to x. There is a genetic deficiency in steroid sulphatase. Its beginning is earlier towards the second or third month of life. The scales are larger, grayish or blackish (black ichthyosis). They affect the convexity of the limbs, the trunk and the neck. There is no keratosis pilaris and the palms and plants are respected, as are the large folds.
Cryptorchidism and corneal opacities may be associated. Transmitting women can with a dry legs and obstetric complications. Histologically, it is a retention ichthyosis with the presence of a granular layer.
It is transmitted in an autosomal recessive mode. The beginning is neonatal and can be done in form baby-collodion. It is a diffuse erythema affecting the face, scalp, folds, palms and plants, covered with gray and adherent dander. An ectropion may associate with it. The affection becomes worse in the sun and heat. Currently, dry ichthyosiform erythroderma, lamellar ichthyosis where erythema and more discreet and wider dander are distinguished. Histology shows proliferation ichthyosis.
It is also rare and is transmitted on autosomal dominant mode. At birth, it is a macerated and bullous erythroderma, and then progressively appear sheets of brownish, hard and disabling hyperkeratosis. Heat promotes the appearance of erosions and there is no tendency to regression. Histology shows epidermolytic hyperkeratosis.
This congenital syndrome results in a glossy and varnished appearance of the skin which is covered by a membrane adherent as collodion. This is responsible for an ectropion, a splinter, curled ears and fixed fingers in half-flexion. It is a newborn at risk: Infection and dehydration. Desquamation begins on the second day. In two thirds of cases the evolution is towards dry erythroderma or lamellar ichthyosis and in 10% towards autosomal dominant ichthyosis.
Autosomal recessive is an autosomal dominant ichthyosis associated with neuropathy and retinitis pigmentosa. It is due to a genetic deficiency of alpha-oxidation of phytanic acid. A poor early chlorophyll diet can prevent the onset of neurological signs.
It is autosomal recessive and is characterized by dry ichtyosiform congenital erythroderma, spastic para or tetraplegia, mental retardation and macular degeneration of the retina.
Dorfman syndrome-Chanarin syndrome, Conradi syndrome.
These ichthyosis are characterized by squames drawing figures: Ichthyosis linear circumflex, genodermatosis in cockade, variable erythro-keratoderma. Concerning the circumflex linear ichthyosis, its association with the Netherton syndrome is recorded in North Africa.
We are reporting different manifestations at tongue level observed in 33 hereditary ichthyosis patients.
The retrospective study lasted two years (May 2012-April 2014) and concerned all hereditary ichthyosis patients who consulted our dermatology department at University Hospital of Tlemcen (Algeria). But only patients whose oral mucosa was inspected were included in this study.
We included a total of 33 patients that had various forms of hereditary ichthyosis (lamellar, X related, keratinopathic, A dry ichthyosiform congenital erythroderma).
First, within 25 autosomal recessive congenital ichthyosis affected patients, 15 had an affected tongue:
• In the first family, 3 out of 4 children were affected from which 2 had Geographic Tongue (GT) (Figure 1)
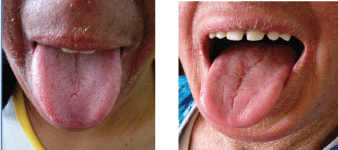 Figure 1: Appearance of lateral cracks on the geographical language of his brother.
View Figure 1
Figure 1: Appearance of lateral cracks on the geographical language of his brother.
View Figure 1
• Four others also had GT
• Nine had cracked tongues distributed in scrotal tongue and superficial (Figure 2) and deep cracks
 Figure 2: Two patients had a deep medial fissure and superficial fissures. View Figure 2
Figure 2: Two patients had a deep medial fissure and superficial fissures. View Figure 2
• Ten of them however, had a normal tongue
Then, six patients had an X related ichthyosis and every single one of them had an affected tongue from which
• Three were scrotal tongues
• One had a deep medial crack
• And two had superficial cracks
A dry ichthyosiform congenital erythroderma affected patient had a normal tongue.
A patient with keratinopathic ichthyosis had a scrotal tongue.
Some patients were controlled after that from which we found:
• An initial transformation of a GT into a scrotal tongue (Figure 3)
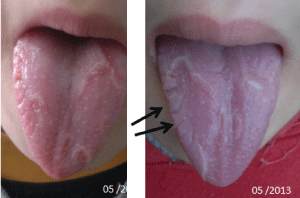 Figure 3: The examination of the 13-year-old patient with ICAR showed a beginning of transformation of her geographical language into the scrotal tongue. View Figure 3
Figure 3: The examination of the 13-year-old patient with ICAR showed a beginning of transformation of her geographical language into the scrotal tongue. View Figure 3
• Appearance of lateral cracks (beginnings of the scrotal tongue) on GT
• Appearance of GT on scrotal tongue
In the end, 22 out of the 33 patients had an affected tongue which is more than 66% of them (6 GT, 5 scrotal tongues, 6 deep medial cracks and 2 superficial cracks). If we only consider geographic tongue afflicted patients, in addition to the development of the GT over the scrotal tongue which is 7 patients in total, we get a frequency of 21% which is significantly superior to its frequency among general population (1-2, 5%) [1] and among psoriasis affected patients (10%) [2] as it was more frequent among the autosomal recessive congenital ichthyosis patients.
The association of the scrotal and geographic tongues occurred in 4 cases.
Patient genotyping will allow accurate diagnosis and phenotypic correlation. Although advances in molecular biology have led to a better understanding of genotype-phenotype correlations, genetic counseling has improved, and genomic analysis for prenatal diagnosis of individuals and families affected by an increasing number of genodermatosis has occurred. Refined, these advances have not yet been converted in terms of clinical benefit for patients [3]. Over the hereditary ichthyosis examination of the genital or oral mucosa should be performed systematically since the achievement of the oral mucosa, would be even more common than in psoriasis. Similar studies will compare the results and to obtain a more objective frequency, given the size of the sample, because of the rarity of the condition. Antenatal diagnosis is currently possible for some ichthyosis.