Aggressive Angiomyxoma (AA) is a kind of rare, low grade myofibroblastic neoplasm with high risk of local recurrence mainly for the character of locally aggressive and misdiagnosis as other soft tissue mass in the pelvis. The "laminated or swirled sign" of swirled strands of low-signal intensities in T2WI is the diagnostic sign for the layered configuration of AA. We report two cases with contrast enhanced CT and Dynamic Contrast Enhancement (DCE) MRI to show the characteristic imaging features and our findings about AA in enhanced CT and DCE MRI.
Aggressive Angiomyxoma (AA), Laminated or Swirled Sign, Magnetic Resonance Imaging (MRI), X-ray Computed Tomography (X-ray CT), Multiplanner Reformation (MPR), Diffusion Weighted Imaging (DWI), Apparent Diffusion Coefficient (ADC)
A 29-year-old woman was incidentally found a mass in her vagina. She was asymptomatic and was diagnosed as fibroma by biopsy. The CTs can show a well-limited mass with low density compared to muscle located in the left pelvic cavity (Figure 1a). After iodine contrast injection, the mass showed a progressive and heterogeneous enhancement without any layered character (Figure 1b). MRI showed a big mass extending into the obturator foramen and ischiorectal fossa, displacing the gluteus, uterus and vagina without invading (Figure 2a). The mass showed homogeneous isointensity compared to muscle on T1WI and hyteroseneous hyperintensity with some whirled strands of low signal on T2WI (Figure 2b). After Gd-DTPA injection, the mass showed a progressive enhancement and laminated strands of hyper-intensity (Figure 2c). The surgery of wide local excision was performed. Histopathology showed spindle tumor cells with no nuclear atypia scattered in the stroma of vascular and loose myxoid. The cytoplasm was positive for desmin and smooth muscle actin. The pathological result was aggressive angiomyxoma.
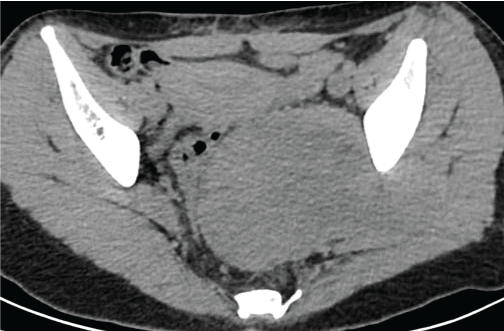 Figure 1a: CT scan showed a well-limited mass with low density compared to muscle located in the left pelvic cavity. View Figure 1a
Figure 1a: CT scan showed a well-limited mass with low density compared to muscle located in the left pelvic cavity. View Figure 1a
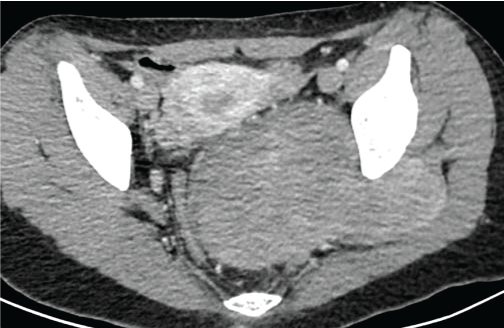 Figure 1b: After contrast injected, the mass had a progressive and heterogeneous enhancement but didn't show the classic laminated pattern or the swirl sign in the axial view. View Figure 1b
Figure 1b: After contrast injected, the mass had a progressive and heterogeneous enhancement but didn't show the classic laminated pattern or the swirl sign in the axial view. View Figure 1b
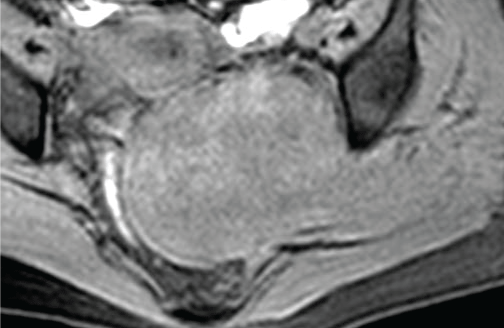 Figure 2a: In MRI, the mass extended into the obturator foramen and ischiorectal fossa,displacing the gluteus, uterus and vagina but not invading them. View Figure 2a
Figure 2a: In MRI, the mass extended into the obturator foramen and ischiorectal fossa,displacing the gluteus, uterus and vagina but not invading them. View Figure 2a
 Figure 2b: On T2WI, the mass presented some whirled strands of low signal within the lesion (black arrow). View Figure 2b
Figure 2b: On T2WI, the mass presented some whirled strands of low signal within the lesion (black arrow). View Figure 2b
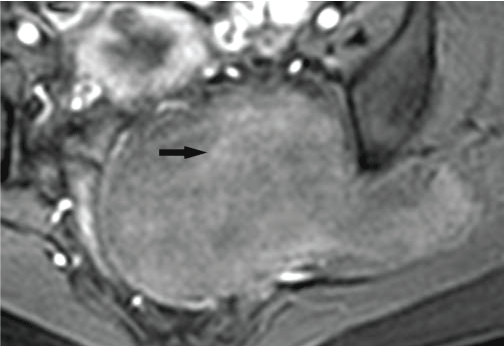 Figure 2c: After contrast injected, the mass showed a progressive enhancement and laminated strands of hyper-intensity (black arrow). View Figure 2c
Figure 2c: After contrast injected, the mass showed a progressive enhancement and laminated strands of hyper-intensity (black arrow). View Figure 2c
A 23-year-old woman was admitted for a vaginal mass for 3 years and the only symptom was frequent micturition for recent 10 days. A lobular low density mass was found in the left pelvic perineum region displacing left ovary, hystera, vagina to right (Figure 3a). The mass showed a progressive enhancement pattern on contrast enhanced CT. A fast enhancing nodule in the background of gradual enhancement was observed in this case (Figure 3b). The laminated high enhancement was noticed in the coronal view (Figure 3c). On MRI, the mass had a clear border to other tissue. The most part of the tumor was isointense and the rest was hyperintense on T1WI (Figure 4a). The T2WI showed mainly hyperintensity with swirled strands of low signal intensity in it (Figure 4b). The Dynamic Contrast Enhanced (DCE) MRI showed progressive enhancement with a fast enhancing nodule. At the same time the swirled strands with hyper-intensity on DCE MRI was noticed (Figure 5a). The DCE curve showed a wash-in both in the early enhancing nodule and the other part of the mass (Figure 5b). The tumor was isointense on DW images (b = 1000 sec/mm2) (Figure 5c). The Apparent Diffusion Coefficient (ADC) mapping showed a high value in the tumor, estimated at 2.42 × 10-3 mm2/sec (Figure 5d). The ADC value of early enhanced nodule was 2.04 × 10-3 mm2/sec compared with the muscle's 1.86 × 10-3 mm2/sec. The preoperative diagnosis was AA according to the CT and MRI. A surgery of wide local excision was performed. The mass was soft, lobular and had a complete capsule. On microscopy, the tumor cells were spindle like and spread in soft myxoidstroma with no nuclear atypia. The tumor was vascular with thickened or hyalinized vessels. On immunohistochemistry it was positive for desmin, CD 34 in different degrees and negative for SMA. And aggressive angiomyxoma was the final diagnosis.
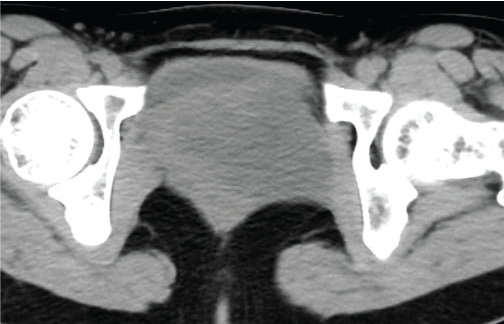 Figure 3a: The CT scan showed a lobular low density mass in the left pelvic perineum region. It displaced left ovary, hystera, vagina to right. View Figure 3a
Figure 3a: The CT scan showed a lobular low density mass in the left pelvic perineum region. It displaced left ovary, hystera, vagina to right. View Figure 3a
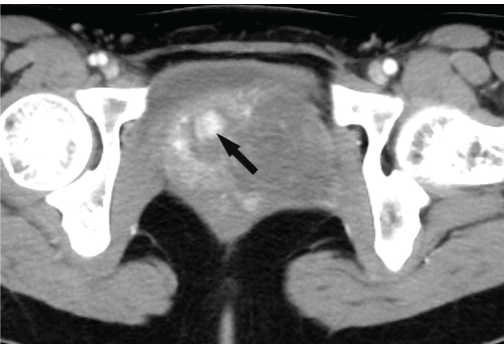 Figure 3b: The mass showed a progressive enhancement pattern on contrast enhanced CT scan. A fast enhancing nodule in the background of gradual enhancement was observed in this case (black arrow). View Figure 3b
Figure 3b: The mass showed a progressive enhancement pattern on contrast enhanced CT scan. A fast enhancing nodule in the background of gradual enhancement was observed in this case (black arrow). View Figure 3b
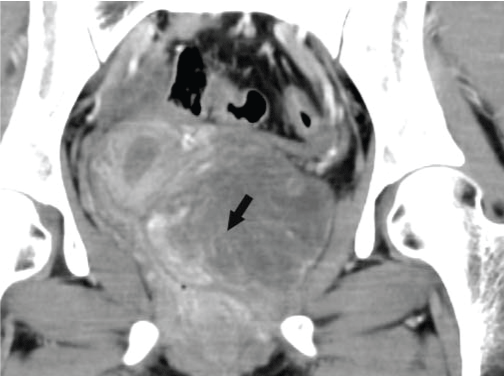 Figure 3c: We could find the laminated pattern in the coronal view (black arrow). View Figure 3c
Figure 3c: We could find the laminated pattern in the coronal view (black arrow). View Figure 3c
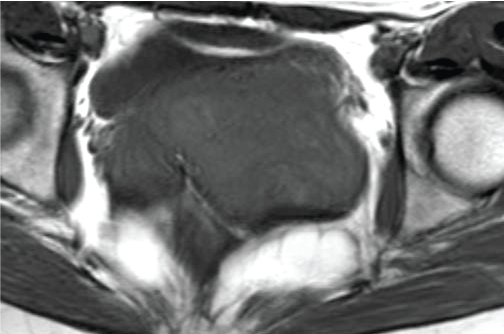 Figure 4a: On MRI, the mass had a clear border to other tissue. The most part of the tumor was isointense and the rest was hyperintense on T1WI. View Figure 4a
Figure 4a: On MRI, the mass had a clear border to other tissue. The most part of the tumor was isointense and the rest was hyperintense on T1WI. View Figure 4a
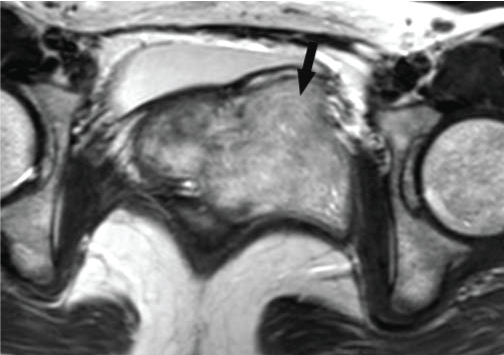 Figure 4b: The T2WI showed mainly hyperintensity with swirled strands of low signal intensity in it (black arrow). View Figure 4b
Figure 4b: The T2WI showed mainly hyperintensity with swirled strands of low signal intensity in it (black arrow). View Figure 4b
Aggressive angiomyxoma was first named by Steeper and Rosai in 1983 [1]. They used the word "aggressive" to emphasize its locally infiltrative and recurrent nature. It is a kind of mysenchymal tumor mainly located in women's pelvic and perineum during their reproductive age, usually between the second and fourth decade. The incidence rate between male and female is about 1:6 [2,3]. Though in most cases it looks like a benign tumor, there are still cases of metastasis and led to the death of the patients reported in articles [4,5]. Because of the low speed of growth and untypical symptoms, this tumor is easily misdiagnosed as Bartholin cyst, hernia or vaginal cyst [3]. The misdiagnosis may lead to the high rates of local recurrence due to incomplete excision. It even leads to unexpected hemorrhage during the surgery. So a better preoperative diagnosis of the AAM is essential for both doctors and patients.
 Figure 5a: The dynamic contrast enhanced MRI showed progressive enhancement with a fast enhancing nodule (black arrow). We could see the characteristic swirled strands with hyper-intensity on DCE MRI (thin black arrow). View Figure 5a
Figure 5a: The dynamic contrast enhanced MRI showed progressive enhancement with a fast enhancing nodule (black arrow). We could see the characteristic swirled strands with hyper-intensity on DCE MRI (thin black arrow). View Figure 5a
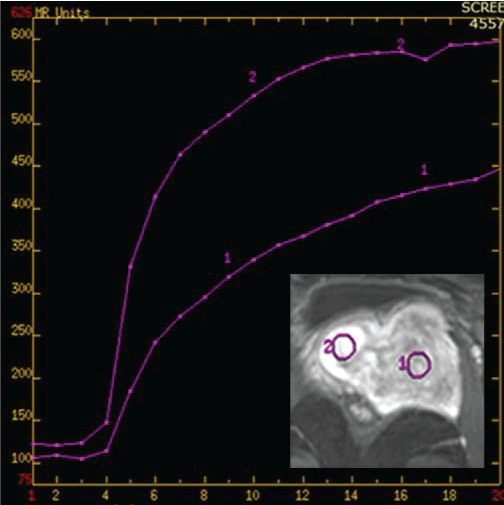 Figure 5b: The tumor's DCE curve showed a progressive enhancement model without plateau or washout both in the early enhancing nodule and the other part of the mass. View Figure 5b
Figure 5b: The tumor's DCE curve showed a progressive enhancement model without plateau or washout both in the early enhancing nodule and the other part of the mass. View Figure 5b
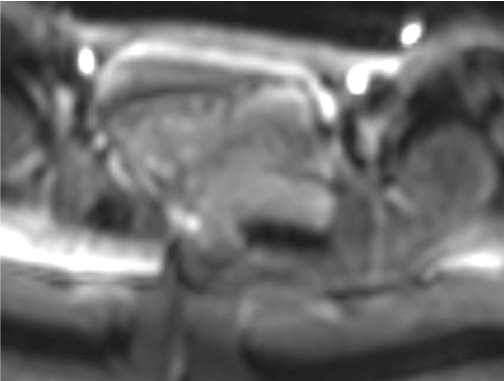 Figure 5c: The tumor was isointense on DW images (b = 1000 sec/mm2). View Figure 5c
Figure 5c: The tumor was isointense on DW images (b = 1000 sec/mm2). View Figure 5c
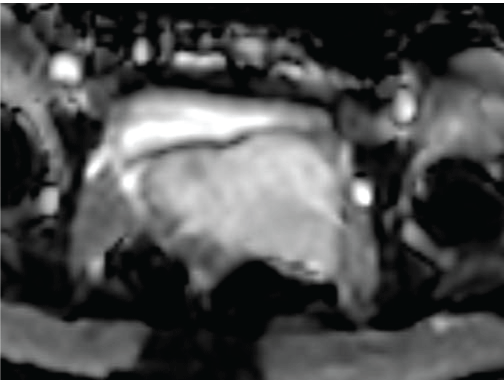 Figure 5d: The apparent diffusion coefficient (ADC) mapping showed a high value in the tumor, estimated at 2.42 × 10-3 mm2/sec. View Figure 5d
Figure 5d: The apparent diffusion coefficient (ADC) mapping showed a high value in the tumor, estimated at 2.42 × 10-3 mm2/sec. View Figure 5d
In 1986, the first report of the CT findings of the AAM was published. From then on, more and more researches have been done trying to use the noninvasive way to give a better preoperative diagnosis of this tumor. Usually, the AA presents as a mass with partial clear boarder mainly displacing other organs. It also has some finger-like structures extending into the fat or soft tissue around it in some cases [6]. On CT scan, the AA gives an appearance as a hypo-or isoattenuating mass compared to the muscle. When the intravenous contrast injected, the mass will have a heterogeneous and progressive enhancement. It is reported only about 44% to 50% cases can show the swirled sign in the contrast-enhanced CT [3,7]. But we find the MPR CT images may be a better way to show more details of the "laminated and swirled" enhancement pattern in our cases. So MPR CT tools should be paid more attention for a better detection of AA.
Because of the high resolution of soft tissue, MRI has become a very important examination for the AA preoperative diagnosis. On T1W images, the tumor is hypo- or isointensity compared to muscle and on T2W images, it is usually a hyperintense lesion, mainly because of the loose myxoidstroma and the abundant water content. The most characteristic feature of the tumor is the laminated or swirled pattern on T2WI and enhanced T1WI mainly because of the inherent vascularity in the stroma [3,8]. On DCE MRI, the tumor presents a progressive enhancement without a plateau or washout. Owing to the ability to provide valuable qualitative and quantitative features of the tumor, DWI has been a hot topic in oncology. There are some articles reported the DWI of AA showed a high value of tumor ADC measurement more than 2 × 10-3 mm2/sec [7,8] as in our second case. The S Brunelle, et al. observed DWI showed heterogeneous high signal intensity both on b0 and b1000 images [8]. However in our second case, we only observed high signal intensity on b0 images. On the b1000 images the tumor was hypointense. It seems that we need more cases to reveal the feature of AA on DWI. Another important finding is that we observed a nodule with fast enhancement in both contrasts enhanced CT and dynamic contrast enhanced MRI in our second case. Though it is not a common feature of AA, we hope it will not stop the radiologist from making a diagnosis of aggressive angiomyxoma.
Pathology is the gold standard for diagnosis of the aggressive angiomyxoma. Macroscopically the tumor is usually a large multilobular or polypoid mass and partially or completely encapsulated with a smooth surface. The cut surface can be soft, gelatinous to rubbery and white to grey in color. Hemorrhage and congestion are also observed in some cases. Histologically the mesenchymal lesion consists of spindled and stellate cells spreaded in a myxoid and collagen background, which is vascular with thickened or hyalinized vessels. It has a benign character lacking of mitoses and nuclear atypia. The AAM tumor cells are positive for desmin, muscle-specific actin, CD34, vimentin, smooth muscle actin in different degrees. Estrogen and progesterone receptors are also detected in some cases. Mainly because of the benign characters, the recurrent tumor has similar features with the primary one [1,9,10].
The surgery of wide local excision is the mainly option in the measurements [7,8]. The rate of local recurrence of AA is different from reports but shows a decrease pattern in recent years. To decrease the rate of local recurrence, preoperative angiographic embolization, preoperative external beam irradiation and intraoperative electron beam radiotherapy have been applied [11]. In the patients show estrogen and progesterone receptor positivity, hormonal manipulation is also an important measurement before or after the surgery [9]. In the patients with relapsing AAM, it was reported that radiotherapy is effective [12].
For a better surgical planning, the imaging character of aggressive angiomyxoma should be aware for the radiologist. "Swirled sign" on MRI is characteristic diagnostic sign for aggressive angiomyxoma, and the laminated pattern on enhanced CT or MRI may also lead to AA as a primary differential consideration. The multi-planner reformation of enhanced CT may help the detection. The DCE MRI of AA shows a progressive enhancement model and may have some early enhancing area in the mass.