Post-transplant lymphoproliferative disorders (PTLD) are frequent in organ recipients; they are most often of B lymphocyte origin; on the other hand, CD30+ t-cell PTLD remain rare; we report the observation of a case of CD30+ anaplastic large cell lymphoma in a renal transplant recipient.
CD30+ lymphoma, Anaplastic large cell lymphoma, Posttransplant lymphoproliferative disorders
The estimated prevalence of post-transplant lymphoproliferative disorders (PTLD) in organ transplant patients undergoing long-term immunosuppressive treatment is 1 to 5% but can reach 20% [1]. Primary cutaneous lymphomas are malignant lymphocytic proliferations strictly localized to the skin, without initial extracutaneous extension. In about half of the cases, it is a lymphoma of the mycosis fungoides type, or Sézary syndrome. More rarely, CD30+ lymphoproliferations are involved, including lymphomatoid papulosis and cutaneous anaplastic large-cell lymphoma [2]. The discovery of a cutaneous anaplastic lymphoma requires a complete extension workup, the main objective of which is to ascertain the primary cutaneous nature of this type of lymphoma.
We report a case of anaplastic large cell lymphoma CD30 in a renal transplant patient.
The patient was 61-years-old, with a history of diabetes, hypertension under treatment, a pigmented basal cell carcinoma of the nipple-areolar plate operated on, a renal transplant under immunosuppressive treatment for 17 years, who had multiple painless nodular lesions with telangiectasias on the forehead for 4 months (Figure 1).
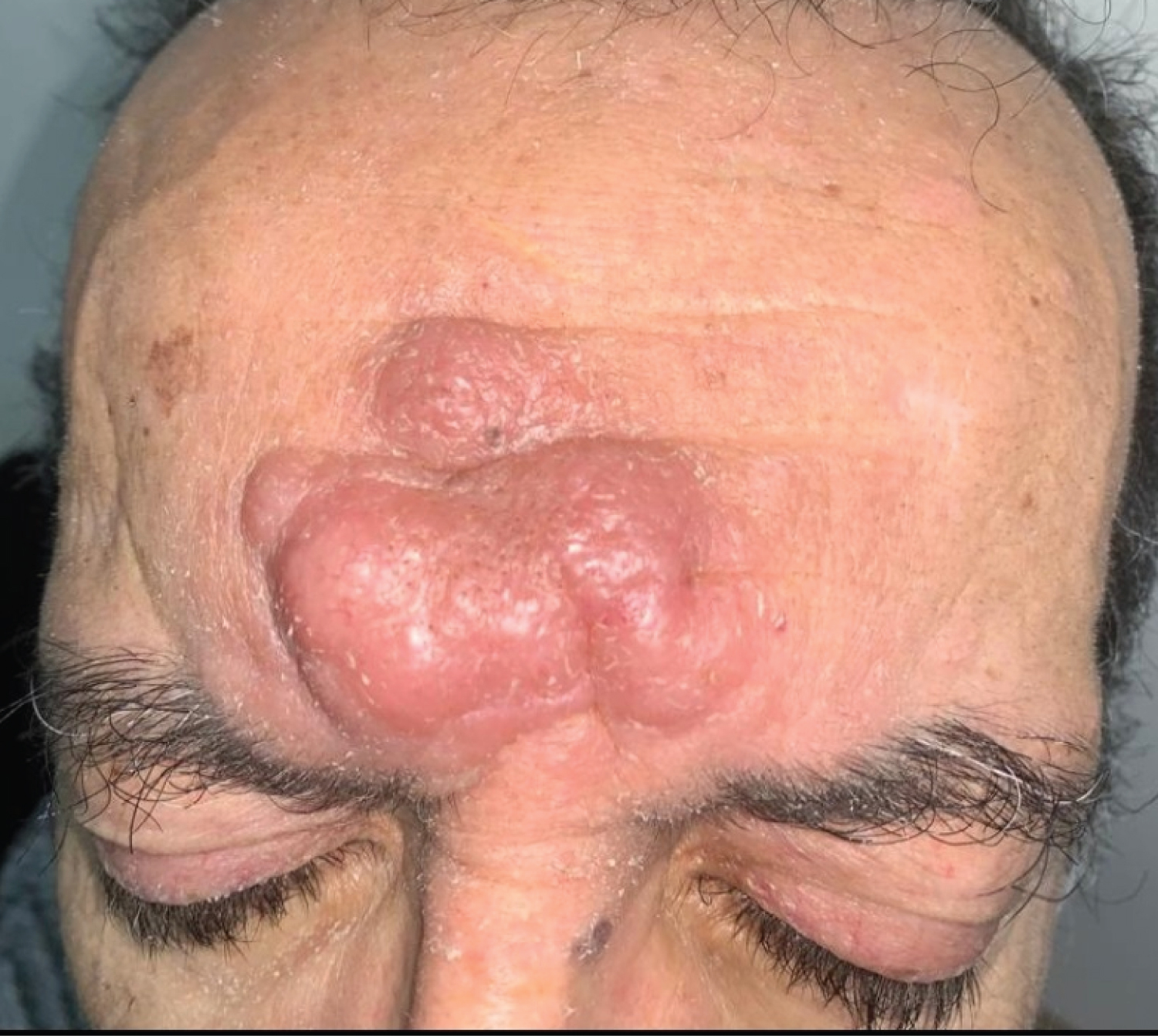 Figure 1: Erythematous, eroded, indurated nodules on the forehead.
View Figure 1
Figure 1: Erythematous, eroded, indurated nodules on the forehead.
View Figure 1
A skin biopsy was performed. Anatomopathological study showed a primary cutaneous CD30+ T lymphoproliferation, suggesting a primary cutaneous anaplastic large cell T lymphoma. Immunohistochemical analysis shows that the atypical lymphocytic infiltrate is of T phenotype (CD3+) with a broad antigenic loss (CD2-CD5-CD7-CD4-CD8-). The atypical infiltrate expresses the CD30 antigen in a homogeneous, intense and diffuse manner. The proliferation index evaluated on Ki-67/MIB1 labelling is very high, estimated at almost 100% of the tumor population. P80/ALK1 staining is negative.
An extension workup is performed, including a biological workup, PET-CT, lumbar puncture and osteomedullary biopsy. At a multidisciplinary consultation meeting (RCP) in oncohaematology, a CHOEP-type multidrug therapy protocol (cyclophosphamide, doxorubicin, vincristine, etoposide, prednisone) was decided upon, but the patient died one month later following a severe Covid-19 infection.
Anaplastic large cell lymphoma (ALCL) is a rare and aggressive peripheral T-cell non-Hodgkin's lymphoma belonging to the group of CD30-positive lymphoproliferative syndromes [3]. (ALCL) accounts for approximately 3% of adult non-Hodgkin's lymphomas and 10-20% of childhood lymphomas. Its prevalence is unknown [4]. ALCL has recently been classified into 4 major groups by WHO: Systemic ALK+ LACL, systemic ALK- LACL, PC-LACL, and breast implant-associated LACL [5]. Systemic ALK+ LACL usually affects children and young adults. The skin involvement may appear as papulonodules or inflammatory plaques with a favorable prognosis [6]. It has a wide morphological spectrum, with the "common type", the small cell variant and the lymphohistiocytic variant being the most frequently observed. Knowledge of the existence of these variants is essential for a correct diagnosis. ALK(-) ALCL occurs in older patients, also affecting both sexes and having a poor prognosis. The etiology of the disease is unknown [7]. In the ALK-positive subtype, the ALK gene (2p23) of the anaplastic lymphoma receptor tyrosine kinase is overexpressed, due to a t (2;5)(p23;q35) translocation [8]. The immunosuppression regimen in organ transplant recipients whose goal is to avoid graft rejection, seems to play a role, as it does for B cells.... However, unlike B-cell PTLD, an association with EBV is found only in a minority of cases [9,10].
Post-transplant anaplastic large cell lymphoma (ALCL) is rather unusual, and its etiology remains uncertain. The diagnosis is based on anatomopathological and immunohistochemical examination of a skin biopsy. It is essential to carry out an extension work-up in order to look for extracutaneous damage that could be life-threatening.
This article has no funding source.
The authors have no conflict of interest to declare.