The UN Millennium Declaration in September 2000 was a milestone in history that marked a commitment of world leaders to a global partnership of time-bound targets for 2015 that became known as the Millennium Development Goals (MDG). MDG3 to promote gender equality and empower women included targets to eliminate gender disparities in the realms of education, employment, and government. Whereas goals such as MDG1 on poverty reduction reached its target ahead of schedule, gender gaps remain significant worldwide. One-third of countries in developing regions have not yet achieved gender parity in primary education, and as of 2015 approximately 50% of all working-age women are in the labor force compared to 77% of men [1].
The relationships between women empowerment, economic development, and favorable health outcomes are too extensive to capture in a simple causal diagram. Economists have described a "virtuous cycle" between women empowerment and development, and the need for sustained policy commitment to gender equality from both moral imperative and pragmatic need [2]. A substantial body of literature already connects women's empowerment with positive outcomes for women, families, and society. Economies grow when women work and an increase in female labor force participation results in faster economic growth [3]. The inferior social status of women in many cultures negatively impacts healthcare outcomes for women and children [4,5]. Gender based discrimination has resulted in significant female morbidity and mortality around the world and was popularized with Amartya Sen's concept of "missing women" in 1992 with estimates of greater than 100 million missing women worldwide at the time [6] and larger estimates nearly a decade later [7].
In 2008, the United Nations Development Programme (UNDP) developed a Gender Inequality Index (GII) [8], which is a composite measure of women's reproductive health, empowerment, and labor participation. An ecological study found an association between this index and neonatal, infant, and under-five mortality rates even after adjustment for confounders such as a per capita gross domestic product and immunization coverage [9]. A systematic review of 219 countries showed that for every additional year of formal education for women child mortality decreased by 9.5% [10]. Studies across multiple countries with high levels of gender discrimination showed that female autonomy and higher social status is associated with improved family planning and perinatal care utilization [11-16] and lower rates of infant and child mortality [9,11,17-19].
Families in which women have decision-making roles devote a greater share of family resources to the children [20-22]. Evidence from a panel of countries has similarly demonstrated that when women have a greater share of household income from cash transfers or through labor force participation, more family spending is for the benefit of children [23]. A Dominican Republic study found that children were significantly less stunted in female-headed vs. male-headed households [24].
The definition of female autonomy has increasingly moved towards an understanding as a multidimensional phenomenon with separate elements possessive of independent effects. As such, some discourage the use of a single index to represent autonomy and advocate for the investigation of the individual dimensions of autonomy [25]. Women's autonomy in healthcare decision-making was included in national questionnaires conducted by the Demographic and Health Surveys conducted in the 2000's in Low and Middle Income Countries (LMIC). Women living in LMIC experience significantly more gender equality than those in high income countries [9], and these same areas of the world have the most to gain in terms of economic development and women's empowerment.
Research into female healthcare decision-making autonomy is an area of growing interest due to its importance from both a human rights and healthcare outcomes perspective. Data has shown that urban and wealthier women in many LMIC tended to deliver in medical settings with the assistance of a skilled health worker [26]. However, it is unclear how socioeconomic status contributes to women's healthcare decision-making behaviors. The nature of this question is complex and likely bidirectional. Prior data has shown that women with paid employment have increased household decision-making autonomy although this relationship has not been specifically queried with regards to healthcare choices [27,28]. There are many pathways by which female healthcare autonomy could be causal or correlated with higher socioeconomic status. Women with decision-making power over their health and utilize services maybe more fit to work contributing to higher familial income. Conversely, wealth and its association with urbanicity, higher education, and distinct cultural norms among many other factors are all possible confounders in the relationship between wealth and healthcare decision-making. Nonetheless, as cash transfer programs have become popularized in the international development community as a social protection instrument, a better understanding of the relationship between wealth and female healthcare autonomy seems increasingly relevant. These interventions have demonstrated positive effects on the health and well-being of children and families [29], and possibly these effects may be partially mediated through increased female healthcare autonomy. This study aims to address if women residing in low and middle income countries who are in higher wealth quintiles have more autonomy over decisions regarding their own healthcare compared to women in lower wealth quintiles.
This study is a comparative cross-sectional analysis of de-identified data from the Demographic and Health Surveys (DHS). We requested permission to use these publicly available datasets from The DHS Program. The six sub-Saharan African countries included in this analysis were countries that had the lowest human development indices in addition to having available datasets at the time of analysis. The Human Development Index (HDI) is a summary measurement on key dimensions of human development including life expectancy, knowledge, and standard of living [30]. The HDI ranks 188 countries with higher numerical rankings reflecting lower index scores and human development (Norway is number one, Niger is number 188). The countries with available datasets and the highest HDI rankings (lowest index scores) included the following DHS surveys: Democratic Republic of Congo 2013 (ranking 176), Mozambique 2003 (180), Sierra Leone 2013 (181), Guinea 2012 (182), Burkina Faso 2010 (183), and Burundi 2010 (184). These countries have both high gender inequality as well as low economic development. The discrepancies in the years of the surveys reflect variation in when the surveys were conducted and which questionnaire modules were included that year, as female healthcare decision-making sections are not included in every DHS round.
The DHS data sets are nationally representative surveys of women aged 15-49. Details regarding individual surveys are described in the final reports [31-36], but they use a multistage cluster design and were weighted to be nationally representative. Country-level sample sizes included Mozambique (n = 7,382), Burkina Faso (n = 13,797), Burundi (n = 5,124), Democratic Republic of Congo (n = 12,400), Guinea (n = 6,733), and Sierra Leone (n = 9,991). Wealth was measured in five distinct wealth quintiles: poorest, poorer, middle, richer, and richest. Each household was assigned a score for possession of assets from a standard list of easy-to-observe assets such as televisions, bicycles, type of flooring, etc. Asset scores were weighted and then were standardized in relation to normal distribution to define breakpoints for the five different quintiles. The construction of wealth quintiles has been described in prior literature [37].
Health care autonomy was measured using the DHS question: Who has the final say in health care decisions? Women had the following response options: respondent only, respondent and husband jointly, husband only, or someone else. Notably, there was significant missingness within the datasets which limits the analysis regarding this question. Missingness is reported as follows: Mozambique 0.2%, Burkina Faso 19%, Burundi 44%, Democratic Republic of Congo 34%, Guinea 26%, and Sierra Leone 36%. To assess the impact of wealth quintile on female healthcare autonomy for each country we calculated the relative risk ratio of a respondent versus her husband having the sole final say on her healthcare decisions between the richest and poorest wealth quintiles via a multivariate multinomial logistic regression model. We first tested bivariate associations of demographic factors identified in existing conceptual frameworks [38,39] for statistically significant relationships to female healthcare autonomy. Education, age, and number of living children were all found to have significant associations (p < 0.05) and prior literature has also supported their relationship with women's empowerment [40-42]. These factors were thus included as adjustment variables in the multivariate analysis. Another variable included was opinion on whether wife-beating is justified if a woman goes out without telling her husband. Given the high prevalence of domestic violence in these countries, this could be a major barrier to healthcare autonomy if a woman cannot leave her home out of fear. Unadjusted model results were also compared to the adjusted model.
Additional sensitivity analyses were performed to evaluate if joint (husband and respondent) decision-making was affected by wealth quintile. Accordingly, the relative risk ratio of a joint decision-making versus the husband alone determining health care decisions was calculated between the richest and poorest wealth quintiles. Effect modification between wealth and the adjustment variables was investigated in serial models and inclusion of these predictors were determined by Wald tests significant at a p-value of 0.05. Data was analyzed using STATA Version 13.1 (Stata Corporation, College Station, TX). Using sample weights that adjusted for differences in probability of selection from survey design, characteristics from each country were described and the weighted distribution of the variables were assessed. Furthermore, all variance estimations were adjusted for complex survey design within the analyses.
Sample demographic characteristics by country are presented in (Table 1). The mean age for all women in the study was 28.4 years. The average number of children was three and the average highest education level was grade 3.7. The mean age, number of children, and highest educational level attained did not vary significantly between countries. Large differences were observed in the opinion on whether wife-beating was justified for going out without permission. Less than a third (29.6%) of women in Burkina Faso thought that it was justified compared to the majority of women in Guinea (82.9%).
Table 1: Sample demographic characteristics by country. View Table 1
There were also significant variations in the distribution of healthcare decision-making between countries as demonstrated in (Figure 1). In Mozambique 43% of women reported that they made their healthcare decisions independently and 23% of women answered that their husbands alone made these decisions. Conversely, among Guinean women surveyed 7.4% made decisions alone, and 65% reported that their husbands alone made healthcare decisions for them. Mozambique was also unique in that 21% of women reported that "someone else" made their healthcare decisions, a proportion that was < 1% in all of the other countries surveyed, and likely represents an elder household figure or parent-in-law.
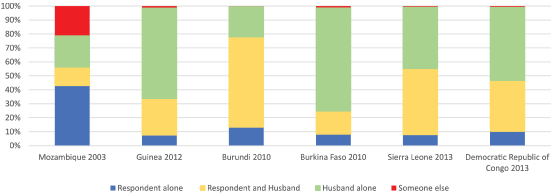 Figure 1: Healthcare decision-making distribution. View Figure 1
Figure 1: Healthcare decision-making distribution. View Figure 1
Differences in female and husband only decision-making between the richest and poorest wealth quintiles using predictions from the adjusted model and centered covariates are depicted in (Figure 2). A general trend of increased respondent only decision-making concomitant with decreased husband only decision-making between the richest and poorest quintiles was observed. Despite the suggestion of greater autonomy with greater wealth, the most prominent finding remained that respondent alone decision-making was overall low with gains of < 10% between the richest and poorest quintiles in all countries. Conversely the largest decrease in husband-only decision-making was seen in Burkina Faso between the richest and poorest quintile, and this also only reflected a ~12.5% decrease. (Table 2) presents the unadjusted and adjusted Relative Risk Ratios (RRR) and 95% Confidence Intervals (CI) of respondent-only versus husband-only decision-making between the richest and poorest quintiles in the six countries. Prior to adjustment for age, education, number of children, and opinion on wife-beating, all countries except for Sierra Leone demonstrated a statistically significant greater likelihood of autonomy for women in the richest wealth quintile in comparison to the poorest (Relative Risk Ratios, RRR, 1.17-2.03). However, after adjustment only Mozambique and Guinea continued to have significant relationships between autonomous decision-making and wealth quintile. Figure 3compares the relative risk ratios between countries in unadjusted and adjusted models.
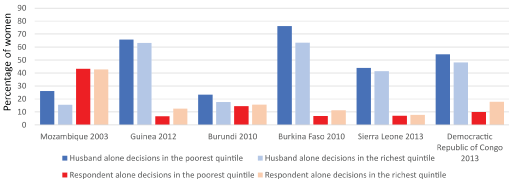 Figure 2: How female healthcare decisions were made in households in the richest and poorest quintiles. View Figure 2
Figure 2: How female healthcare decisions were made in households in the richest and poorest quintiles. View Figure 2
 Figure 3: Relative risk ratio by countries. View Figure 3
Figure 3: Relative risk ratio by countries. View Figure 3
Joint couple (husband and respondent) in comparison to husband-only decision-making relative risk ratios between the richest and poorest were statistically significant in the unadjusted analyses of Burkina Faso (RRR 1.97) and Burundi (RRR 1.42) only. These associations disappeared after covariate adjustment and are depicted in (Table 2). However, shared decision-making was overall common in many countries as demonstrated in (Figure 1). Guinea and Burkina Faso were the only countries where the majority of households reported husband-only decision-making.
Table 2: Unadjusted and adjusted relative risk ratios between richest and poorest quintiles. View Table 2
The determinants of female healthcare decision-making in low and middle income countries are multi factorial and complex. To our knowledge, this is the only study that assesses female healthcare autonomy by wealth quintile in sub-Saharan Africa. Other studies have assessed composite measures of women empowerment in African countries that frequently include female healthcare autonomy, but it is worthwhile to look specifically at this factor as it is a key determinant in healthcare quality and outcomes. Additionally, in an era where unconditional cash transfers are becoming a popular mechanism of poverty reduction and foreign aid, it is useful to consider how wealth may be associated with health-seeking behaviors.
These surveys demonstrated that among the sub-Saharan countries with the lowest UN Human Development Index scores, there was great variability in women's healthcare decision-making. Although there is some evidence of a positive correlation between wealth quintile and female healthcare autonomy the link is not strong and country specific. Rather, the most consistent finding was that respondent-only decision-making was low among most countries outside of Mozambique and generally less than 20% of households. Mozambique was also unique in that 20% of respondents described "someone else" making healthcare decisions for them highlighting different cultural norms among nations. Studies in Bangladesh have reported that attitudes of in-laws and other family members have resulted in delays in mothers seeking postnatal care [43,44]. In particular, the role of purdah or the social and religious practice of female seclusion has been implicated as a barrier to healthcare in which a non-husband influence affects decisions. Women have reported feeling ashamed when being attended by a male health worker in many low and middle income countries [45-47].
Perhaps the most substantial finding of this analysis was the loss of correlative statistical significance between wealth and autonomy in many countries when controlling for the adjusted covariates of age, education, number of children, and opinion on wife-beating. Furthermore, between the richest and poorest wealth quintiles estimates of respondent-only and husband-only decision-making did not change significantly in absolute percentage values although they did generally follow a trend of increased autonomy with increased wealth. Prior literature has demonstrated a strong association for age and number of children with increased autonomy and influence [48-50]. Accordingly, when controlling for these factors it is not surprising that the correlation between wealth and autonomy was weakened and in many instances no longer significant. Age and number of children may well likely be more important than wealth for female healthcare autonomy. There are also many considerations such as religious affiliation, ethnicity, and cultural beliefs among others that could not be assessed in this study and have also been shown to affect healthcare decision-making [51-53].
As such, these findings contribute to existing literature by demonstrating empirical evidence of a weakly positive correlation between wealth status and women's healthcare empowerment. There remain many more questions to be investigated however. While paid employment is known to increase household autonomy it is unknown if these gains are also reflected in healthcare autonomy specifically, and if women in higher wealth quintiles also experience greater autonomy even without being independently employed. The non-financial barriers for women in low and middle income countries may in fact pose more significant impediments to accessing healthcare and are both harder to measure and intervene upon. Qualitative studies also are still lacking in this area and needed to further elucidate the complex interplay of socio cultural and economic factors contributing to health seeking behaviors [51].
There are several limitations within this study. Most importantly this is a retrospective cross-sectional analysis and the relationship between wealth quintile and female healthcare autonomy is blurred by multiple confounders. It is not possible to assess a true counterfactual as in a randomized control trial. There may be distinct socioeconomic behavioral differences between families in lower versus higher wealth quintiles that affect female healthcare autonomy that have not been controlled for. Additionally, many of the countries had significant missingness that limit interpretation of data even with multiple imputation methods. Lastly, although presumably women are answering truthfully about decision-making patterns in their families, there are no existing validation studies to assess actual versus reported health-seeking behaviors in these women that these authors were able to find.
Despite significant limitations, this study offers some insight into the complex relationship between women's empowerment, healthcare access, and economic status. Given that gender equality, economic development, and improved healthcare represent core values of the millennium development goals, further research into this complex nexus is warranted to help develop future strategies that can benefit all three key components.
We are grateful to the DHS staff and teams that carried out and conducted these survey analyses in these countries and have made the data publicly available.
Data collection was performed by the DHS staff which received training in ethics and confidentiality. Our team requested access to de-identified publicly available data for purposes of analysis and women's health research and followed DHS protocols.