Aspergillosis is well known in a patient with perinuclear Antineutrophilic Cytoplasmic Antibody (p-ANCA)-associated vasculitis and pulmonary renal syndromes [1]. However, only a few cases have been reported in ANCA-associated patients. Akimoto, et al. reported a patient of ANCA-associated vasculitis with corticosteroid therapy who had massive recurrent hemoptysis due to pulmonary Aspergillus mycetoma [1]. A disseminated aspergillosis with invasion of the lungs, heart, and brain developed following resolution of pneumocystis pneumonia in a patient receiving long-term prednisolone therapy for Good-pasture syndrome with positive ANCA, an autoimmune disease that attacks the lungs and kidneys [2]. In China, Su, et al. found 7 of 157 patients with ANCA-associated vasculitis developed Invasive Pulmonary Aspergillosis (IPA) [3].
A 64-year-old woman with chronic kidney disease had hemoptysis for 2 days. Soon, dyspnea and O2 desaturation occurred. She was admitted to the Intensive Care Unit (ICU) on November 16, 2015. The blood urea nitrogen and creatinine were 96 and 8.9 mg/dL respectively. The immunological tests included antinuclear antibodies, 40 x; p-ANCA, 27.4 IU/mL (positive, > 5 IU/mL); Cytoplasmic ANCA, < 0.2 IU/mL and basement membrane zone antibody, < 20 x. As p-ANCA positive vasculitis with pulmonary renal syndrome was suspected, she received hemodialysis and intravenous methylprednisolone (40 mg every 6 hours). Her condition improved, so she was transferred to the ward on 30 November.
Because the renal biopsy revealed p-ANCA-associated diffuse crescentic glomerulonephritis, an intravenous low-dose cyclophosphamide (200 mg) and double filtration plasmapheresis were initiated. The patient received methylprednisolone 160 mg daily for about 3 weeks from November 16 to December 5, which was then reduced to 40 mg every 12 hours from December 6, 2015. On December 7, a nodular lesion appeared in the right upper lung field (Figure 1A), of which the chest Computed Tomography (CT) revealed abscess appearance (Figure 1B). Meanwhile, Aspergillus galactomannan antigen tests (index) were 2.6 in blood sample and > 7.18 in the bronchoalveolar lavage fluid respectively (normal, < 0.5 index), so voriconazole was added on December 16. However, as her consciousness became disturbed, brain Magnetic Resonance Imaging (MRI) revealed hemorrhagic necrotic lesions at left frontotemporal and right temporoparietal regions (Figure 1C and Figure 1D). The family did not accept biopsy for the brain lesions. The methylprednisolone was discontinued on December 26, 2015.
The follow-up chest CT showed persistent lung abscess on January 30, 2016 (Figure 1E). CT-guided lung biopsy revealed the presence of fungal hyphae, supporting the diagnosis of IPA. However, the patient experienced a short course of pulmonary hemorrhage (Figure 1F). Follow-up brain CT revealed marked resolution of the brain lesions (Figure 1G). She was then discharged with stable condition on March 5, 2016. Throughout the course, the patient had lymphocytopenia with a lymphocyte of less than 1000/μL for most of the time when the blood was tested (Figure 2).
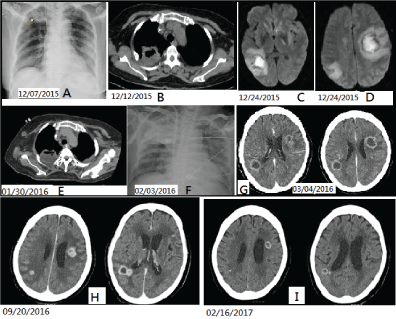 Figure 1: Chest X-ray film shows a nodular lesion in Right Upper Lung (RUL) field (A, arrow), which was suggestive of abscess formation by chest CT imaging; B) Brain MRI shows multiple hemorrhagic necrotic mass lesions, involving right temporoparietal and left frontotemporal regions; C,D) Follow-up chest CT scan shows persistent RUL lung abscess; E) Post-biopsy CXR shows consolidation over RUL; F) Indicating pulmonary hemorrhage clinically. Follow-up brain CT scans in post-voriconazole treatment; G,H) Subsequent posaconazole therapy (I) Show significant resolution of brain lesions, favoring cerebral aspergillosis. View Figure 1
Figure 1: Chest X-ray film shows a nodular lesion in Right Upper Lung (RUL) field (A, arrow), which was suggestive of abscess formation by chest CT imaging; B) Brain MRI shows multiple hemorrhagic necrotic mass lesions, involving right temporoparietal and left frontotemporal regions; C,D) Follow-up chest CT scan shows persistent RUL lung abscess; E) Post-biopsy CXR shows consolidation over RUL; F) Indicating pulmonary hemorrhage clinically. Follow-up brain CT scans in post-voriconazole treatment; G,H) Subsequent posaconazole therapy (I) Show significant resolution of brain lesions, favoring cerebral aspergillosis. View Figure 1
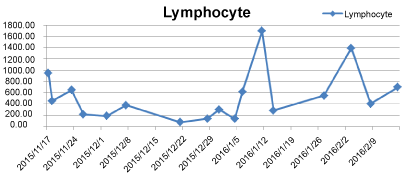 Figure 2: Throughout the course of first hospitalization, the patient had prolonged lymphocytopenia with a lymphocyte of less than 1,000/μL for most of the time when the blood was tested. View Figure 2
Figure 2: Throughout the course of first hospitalization, the patient had prolonged lymphocytopenia with a lymphocyte of less than 1,000/μL for most of the time when the blood was tested. View Figure 2
The patient was readmitted to the hospital due to a seizure attack on August 22, 2016. During this episode, she underwent navigator-assisted brain biopsies for left frontal and right parietal brain lesions, which reveal chronic inflammation without identifying tumor growth or fungal elements. She was then maintained on oral voriconazole therapy until September 20, when CT image did not show further resolution (Figure 1H). The antifungal therapy was changed to oral posaconazole (600 mg per day) for 5 months, which achieved significant reduction of the brain lesions in the CT image on February 16, 2017 (Figure 1I). A blood Aspergillus antigen index became 0.12. The patient remained stable at the follow-up visit on July 4, 2017.
IPA is a well-known complication of immunosuppressive treatment for ANCA-associated vasculitis. The prolonged lymphocytopenia and ICU stay as well as corticosteroid and cytotoxic therapy might be the risk factors for systemic aspergillosis in our patient with p-ANCA vasculitis. Lymphocytopenia with depressed T-cell function may result in increased susceptibility to IPA [4]. The role of high-dose corticosteroid treatment should be taken into consideration as a risk factor for IPA, especially in critically ill patients and those with chronic obstructive pulmonary disease [5]. Cytotoxic chemotherapy has been regarded as a classical risk factor for invasive aspergillosis [6]; nonetheless, our patient only received one dose of intravenous cyclophosphamide (200 mg), so its significance was difficult to discern.
Since serious and opportunistic infections due to immunosuppressive agents and vasculitis are well known, improved recognition, diagnosis, and prevention of these infections have become important safety issues in these patients [7]. For example, less aggressive treatment without immunosuppressants for vasculitis might achieve clinical effectiveness and avoid opportunistic infections. Angiogenesis inhibitor but not an immunosuppressive agent could be a potential tool for the treatment of vasculitis [8,9].
Cerebral aspergillosis occurs primarily in patients with severe immunodeficiency, but can happen in a previously healthy or influenza-affected patient [10,11]. Cerebral aspergillosis accounts for 5-10% of all intracranial fungal pathology and may require anti-fungal therapy for 12-18 months [10]. Our case had experienced confirmed IPA and probably cerebral aspergillosis over a 15-month observation period with antifungal therapy (Table 1). Aspergillus galactomannan antigen assay might help early diagnosis and initiation of antifungal therapy. Posaconazole achieves successful salvage after prolonged voriconazole therapy [12].
Table 1: Clinical courseand antifungal progression of our case. View Table 1
In conclusion, diagnosis of invasive aspergillosis is challenging and treatment remains difficult. The gold standard diagnosis is made by specific histopathology. The mortality rates are still high, so early therapy is mandatory.
We declare no conflict of interest and financial support regarding this letter.
The above study has been granted exemption from review by the Institutional Review Board of Chi-Mei Medical Center (IRB Serial No. 10503-E03).