Avascular necrosis is a known complication of systemic lupus erythematosus. We report an unusual case of avascular necrosis affecting both the lunate and triquetrum in a child with this condition. Vasculitis, synovitis and IgM anticardiolipin antibodies were probable predisposing factors. The use of arthroscopic synovial debridement improves symptoms even in the presence of carpal chondromalacia and potentially delays the need for salvage surgery.
Avascular necrosis (AVN) of the carpus typically affects the lunate (Kienbock's disease), to a lesser extent the scaphoid (Preiser disease) and rarely the capitate, hamate or triquetrum [1,2]. Although uncommon, pediatric AVN of isolated carpal bones have been published in individual case reports [3,4]. Multifocal patterns of the carpus have previously only been documented in adults and include AVN of the entire proximal row with and without hamate involvement [5]. Although often idiopathic, the common secondary causes and associated factors for carpal AVN include trauma, corticosteroid intake and anatomical variation (e.g. negative ulnar variance with Kienbock's disease). Systemic lupus erythematosus (SLE) has been associated with both AVN of the lunate and scaphoid in adults. Corticosteroid use is predominantly quoted as the leading factor attributed to the onset of AVN in SLE [6], however studies have also shown SLE to be an independent risk factor, probably secondary to synovitis and/or the presence of autoimmune related antibodies [7].
We present, to our knowledge, the first case of synchronous lunate and triquetral AVN in a child with SLE. The aetiology and management of carpal AVN in childhood SLE are also discussed based on the available literature.
A 14-year-old girl, diagnosed with SLE five years previously, presented with a two-year history of non-traumatic pain and stiffness of her right dominant wrist. She was able to write and self-care, however she was unable to partake in hand-held ball and racquet sports at school.
Although she previously had received a short course of prednisolone for associated lupus nephritis, she was medication free for over two years prior to the onset of wrist pain. Supplementary immunosuppressive treatments, including hydroxychloroquine and mycophenolate, had successfully abated any acute flare-ups. She had not reported any swelling around her wrist or any other joint inflammation for several years. Examination revealed flexion-extension of 75º/35º, radio-ulnar deviation of 10º/25º and full prono-supination. There was tenderness over the triangular fibrocartilage complex (TFCC) and radio-carpal joint dorsally, painful lunotriquetral translation test, but no effusion or palpable synovitis.
Plain radiographs, computed tomography (CT) and magnetic resonance imaging (MRI) findings revealed multifocal intra-osseous cysts and lunotriquetral AVN (Figure 1, Figure 2 and Figure 3).
 Figure 1: Focal lucencies with sclerotic margins in proximal row carpal bones.
View Figure 1
Figure 1: Focal lucencies with sclerotic margins in proximal row carpal bones.
View Figure 1
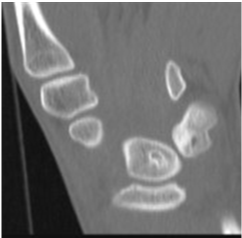 Figure 2: CT confirms lytic areas with sclerotic margins.
View Figure 2
Figure 2: CT confirms lytic areas with sclerotic margins.
View Figure 2
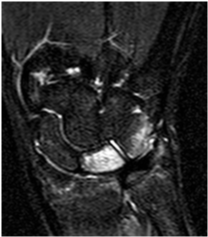 Figure 3: Coronal short tau inversion recovery (STIR) image: High signal change in lunate-triquetrum, indicating extensive marrow oedema consistent with AVN.
View Figure 3
Figure 3: Coronal short tau inversion recovery (STIR) image: High signal change in lunate-triquetrum, indicating extensive marrow oedema consistent with AVN.
View Figure 3
After conservative treatment with splinting, activity modification and oral anti-inflammatory analgesia, symptoms persisted, and a right wrist arthroscopy identified dorsal synovitis, extensive chondral detachment of the articular proximal surface of the lunate and triquetral chondromalacia (Figure 4, Figure 5 and Figure 6). A corticosteroid injection was deemed unsuitable pre-operatively with a diagnosis of AVN and no external signs of synovitis.
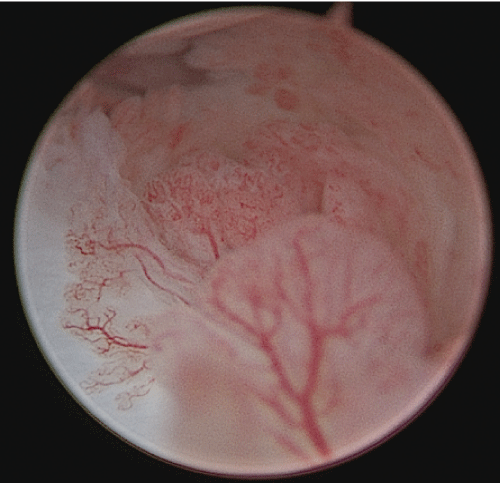 Figure 4: Right radiocarpal arthroscopy (3/4 portal): Synovitis dorsal capsule.
View Figure 4
Figure 4: Right radiocarpal arthroscopy (3/4 portal): Synovitis dorsal capsule.
View Figure 4
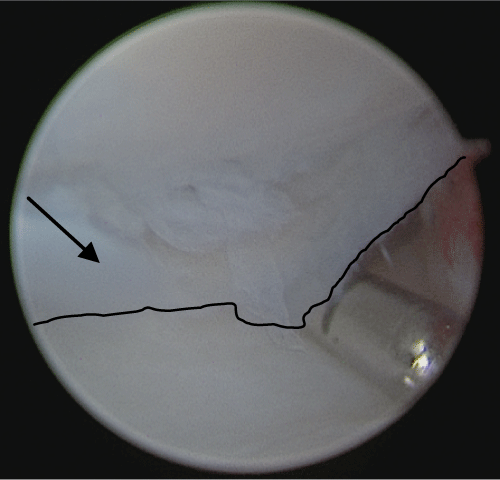 Figure 5: Right radiocarpal arthroscopy (3/4 and 6R portals): Lunate chondral flap (arrow and black line outlining flap edge) with lunate bone above and lunate fossa of distal radius below.
View Figure 5
Figure 5: Right radiocarpal arthroscopy (3/4 and 6R portals): Lunate chondral flap (arrow and black line outlining flap edge) with lunate bone above and lunate fossa of distal radius below.
View Figure 5
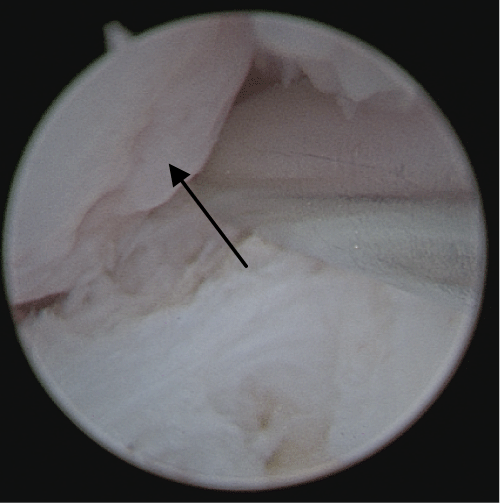 Figure 6: Right radiocarpal arthroscopy (3/4 and 6R portals): Triquetral chondromalacia (arrow).
View Figure 6
Figure 6: Right radiocarpal arthroscopy (3/4 and 6R portals): Triquetral chondromalacia (arrow).
View Figure 6
Following arthroscopic synovial debridement and removal of any loose bodies/cartilage, followed by a period of reduced loading of 6 weeks, she was pain free both at rest and loading at 3 and 6 months post-operatively. A further review was undertaken 2 years later and there was no recurrence of her symptoms. Visual analogue scale was recorded as 0 at rest and loading. Range of movement of the right wrist now measured 90º of flexion and 70º of extension, which is greater than the non-operative side of 50º extension. Radial-ulnar deviation increased to 35º/50º. Right hand grip strength using a dynamometer was 21 kg compared to 14 kg on the left. No synovitis or swelling noted. Repeat X-rays showed no collapse or fragmentation, slight sclerosis of the triquetrum with normal appearance of the lunate.
The overall prevalence of symptomatic AVN is 9% for patients with SLE and 29% for asymptomatic AVN [8]. In children, AVN associated with SLE has been identified at several bony sites, most commonly affecting the proximal or distal femur and humerus, with a prevalence of 5.4-8.4% [9,10]. Carpal AVN with SLE has been reported in young adults affecting the lunate, but there is no published literature regarding children. Pediatric Kienbock's disease, although not common, has been reported on several occasions and affects children as young as 6-years-old [3]. Kienbock's disease in childhood with a previous diagnosis of bilateral Perthes disease has been linked to Factor V Leiden thrombophilia [11].
Multifocal AVN is well documented in children, being associated with several conditions such as leukaemia, stem-cell transplantation, sickle cell disease and haemophilia [10]. However, although multifocal carpal AVN has been identified in adults, it has never been reported in children [5]. To our knowledge, we have therefore reported the first case of combined lunate and triquetral AVN and also the first case of carpal AVN in a child secondary to SLE.
Corticosteroid usage is the leading causative factor for AVN in SLE. High dose corticosteroids, as well as maximum and cumulative doses are particularly associative. Patients with side effects from corticosteroids seem to have the highest rate of AVN. Given the low dose administered over a short period some years previously it seems less likely corticosteroids were with main causative agent in the case study. Apart from corticosteroids, cyclophosphamide is also a risk factor in SLE. However, despite 0.5% of patients taking mycophenolate mofetil develop osteonecrosis, when taking into consideration other risk factors, there appears to be no direct causative link in SLE [8]. Likewise, this is seen with azathioprine, hydrochloroquine and methotrexate. It is therefore unlikely the other immunosuppressive medications had a direct impact of causing the AVN.
As shown with this patient's CT scan, intraosseous cysts are observed in patients with SLE, however there is no evidence to suggest that the presence of intraosseous cysts leads onto AVN. Only one of 16 patients in a case series of intraosseous cysts secondary to SLE developed AVN [12]. All 16 cases were concomitantly being treated with corticosteroids and so a confounding factor when considering aetiological causes of AVN.
Studies have also shown that SLE is an independent risk factor for AVN [10], as most likely observed with this case. Vasculopathy related to active vasculitis, renal manifestations or the presence of certain antibodies has been thought to be responsible [7]. This patient had a history of renal involvement and was also positive for pANCA, dsDNA and IgG/IgM cardiolipin antibodies. Anticardiolipin antibodies, strongly associated with antiphospholipid syndrome, have been shown to increase the risk of developing AVN in patients with SLE [7]. A meta-analysis by Nevskaya confirms this as approximately double the risk compared to other autoantibodies and autoimmune markers [8]. Any patient diagnosed with SLE should be investigated for the presence of anticardiolipin antibodies and if positive should be aware of an increased risk in developing AVN.
More recently Vitamin D deficiency in childhood has been shown to be another causative association and therefore it can be difficult to isolate one single trigger when considering the aetiology of AVN in SLE [10].
It should also be noted that radiographic and MRI investigations can have limited value in certain wrist pathologies. These investigations underestimated the extent of chondromalacia in this case. It may therefore be prudent to consider arthroscopic assessment of any cartilage damage secondary to AVN as well as identifying other causes for ongoing wrist pain, e.g. synovitis.
At arthroscopy a significant amount of dorsal wrist synovitis was indeed present. This may well have been a response to the chondral delamination of the lunate or chondromalacia of the triquetrum, rather than a direct immunological response to SLE, particularly as the disease had been so quiescent for several years. However, it has been reported that there is no correlation between the extent of synovitis in the wrist and clinical signs of disease activity [13]. Arthroscopic synovectomy and debridement of loose cartilage bodies in our patient had an early and lasting effect by reducing pain and improving function despite significant chondral damage.
We therefore propose that arthroscopic debridement of synovitis secondary to SLE-induced carpal AVN may improve pain and function even in the presence of chondromalacia, and possibly delays the need for offloading or salvage procedures.
The outcome for lunate AVN in childhood has been shown to be excellent with conservative management even in the presence of collapse [3-5]. The long-term outcome of SLE-induced carpal AVN and chondromalacia is unknown, however this pediatric patient remains pain free at 2 years post-arthroscopic debridement.