Left ventricular assist device (LVAD) placement is now commonly performed as both bridge to transplant and as destination therapy in end stage cardiomyopathy with high associated prevalence of sepsis (up to 58%) and mortality (up to 44%). Recent evidence indicates that physiologic imaging with scintigraphy is more sensitive than anatomic imaging for early diagnosis of driveline and pump infections. Additionally colonic perforation is a rare but likely underdiagnosed complication which contributes to post-placement morbidity. Here we present a case report of LVAD drive line infection associated with colonic perforation, diagnosed on 18FDG-PET/CT.
LVAD infection, Colonic perforation, PET/CT
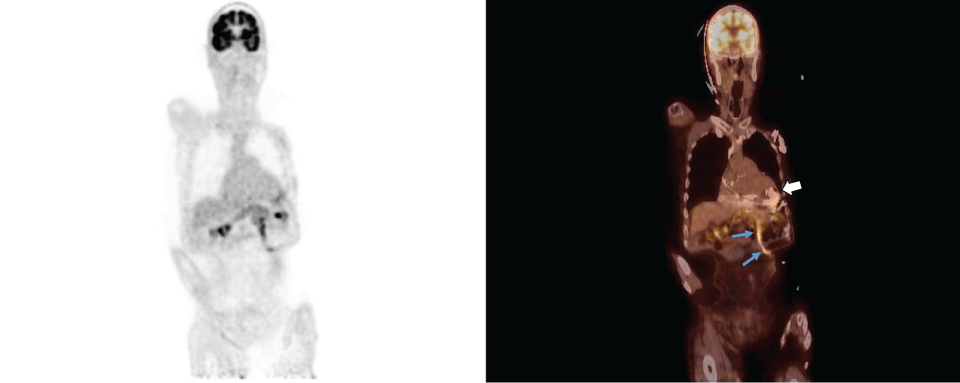
Figure 1: PET/CT demonstrating isolated drive line infection - A 79 year old with non-ischemic cardiomyopathy status post destination therapy with left ventricular assist device, presented multiple times in the year following device placement with hypotension, fever, chills, leukocytosis and abdominal pain. 2D cardiac echo and CT abdomen/pelvis with contrast were performed but no source of infection was identified. After 8 months of treatment failure with escalating intravenous antibiotics, whole body 18FDG-PET/CT demonstrated increased activity diffusely along the drive line (blue arrows). Notice the absence of FDG uptake within or surrounding the main LVAD pump (white arrow) on planar or fused images. These two findings in conjunction are consistent with isolated drive line infection of the LVAD device. There is a high prevalence of device-related infections in LVAD patients [1] with sepsis being the leading complication in this population [2] and accounting for more than twice the number of deaths compared to device failure [3]. Infection typically involves the driveline which connects the LVAD pump to its external power source and can present clinically with fever, chills, leukocytosis, erythema and purulent drainage at the exit site [4]. Less commonly, infection can extend up to the subcutaneous recess where the LVAD pump is housed leading to pump pocket infection, in which case deep tissue tenderness may also be present [5]. Anatomic imaging (CT, Ultrasound) is sensitive in identifying fluid collections, if any, associated with the infection site. However there is evidence that scintigraphy is more sensitive in identifying and localizing infection, especially early on in its course [6]. This case illustrates the utility of physiologic imaging with PET/CT to diagnose and localize LVAD drive line infection even in the setting of persistent negative anatomic imaging and associated rare complication of colonic erosion with the drive line.
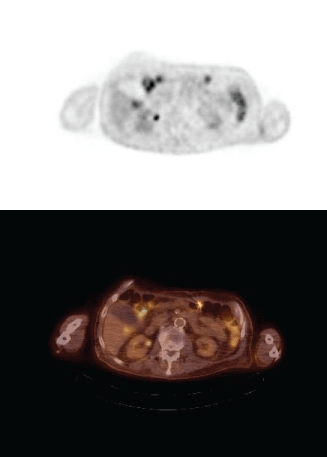
Figure 2: PET/CT demonstrating colonic erosion of the drive line - Axial images demonstrate erosion of the LVAD drive line into the superior wall of the transverse colon and asymmetrically increased activity within the adjacent segment of colon. This was subsequently confirmed during open surgical exploration of the drive line infection for which the patient received a partial colectomy. Extension of the LVAD driveline into the intestinal tract, causing erosion or perforation, is rare, with just a few isolated cases previously reported in medical literature [7-10]. In the case reported by Herman et al. [7], a similar clinical course was noted, with multiple admissions for fever, chills, hypotension and bacteremia in the context of normal anatomic imaging for a prolonged period of time. The diagnosis was made after CT chest demonstrated gas within the LVAD pocket on post-operative day 234 and colonic perforation was discovered during the emergent exploratory laparotomy that followed. This case demonstrates that scintigraphy with PET/CT can not only be utilized for diagnosis and localization of LVAD infection but can also assist in recognition of the rare but under-recognized complication of colonic erosion.