Acute coronary syndrome, Complete left bundle branch block, Endocarditis
A 50-year old man was admitted to the emergency room due to severe dyspnea and thoracic pain with 3 hours of onset. He had no known history of cardiovascular disease, but he was recovering from drug addict. At the emergency room he was at cardiogenic shock requiring intubation and mechanical ventilation.
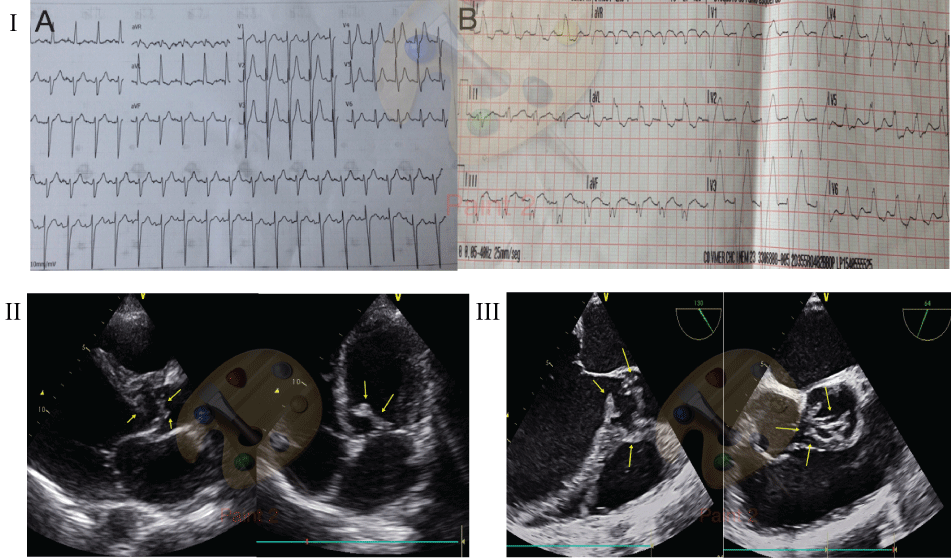
Physical exam was notable for diffuse lungs crackles. The heart sounds were normal and a grade III/VI systolic murmur was audible. The 12-lead electrocardiogram demonstrated sinus tachycardia and new complete left bundle branch block (Figure I).
The diagnosis of acute myocardial infarction with ST-segment elevation was done. The interventional cardiologist was contacted to perform primary angioplasty. The clinical cardiologist was also called, and during the waiting time for hemodynamic team he performed a transthoracic echocardiography. That showed a enlargement of left ventricle, with mild impaired function and a large mass in the ventricular side of the aortic valve, conditioning obstruction and major aortic valve insufficiency (Figure II). A transesophageal echocardiography was also perfumed and confirm the aortic valve destruction and a large paravalvular abscess involving the left sinus of Valsalva (Figure II and Figure III). Blood cultures were collected and empirical antibiotic therapy for endocarditis was initiated.
Coronary angiography was not performed due to the high risk of this procedure.
The case was discussed with the cardiac surgeon but they refused the patient and he died a few hours later.