A 32-year-old man was referred to us with an abdominal mass detected by ultrasonographic examination during phyisical checkup. She had history of hepatic hemangioma for 10 years. Examination of the heart and lungs was normal, and there were no apparent enlarged lymph nodes. The tumor markers were all within normal range. Subsequently, the CT of the abdomen confirmed the presence of a well circumscribed, encapsulated mass with different shaped calcifications, which seemed to arise from the pancreas and was adherent to the pancreatic neck. The mass enhanced intensely in the arterial phase with moderate washout in the venous phase. In addition, CT revealed no other enlarged lymph nodes and involved organs (Figure 1(A-E)). At exploratory laparotmy, an encapsulated tumor measuring 6 × 7 cm was completely removed adjacent to the pancreatic neck. Pathology revealed Castleman lymphadenopathy of hyaline-vascular type (Figure 1F). The patient was discharged 7 days later without postoperative complications and is well 2 years after surgery.
Castleman's disease (CD), also known as giant lymph node hyperplasia, is an uncommon lymphoproliferative disorder firstly described in 1956. It is an unusual condition in which the primary etiology and pathogenesis, which may be reactive or neoplastic, remain unclear. Clinically, CD may be unicentric if confined to a single lymph node or multicentric when there are numerous involved nodes associated with concomitant systemic symptoms. Two main histological variants of the disease have been recognized: hyaline-vascular type and plasma-cell type. The hyaline-vascular type, usually found in unicentric CD, is characterized by small hyaline-vascular follicles and interfollicular stroma with capillary proliferation. Plasma-cell type, typical of multicentric CD, present large follicles with intervening sheets of plasma cells. Patients with the hyaline-vascular type of CD are usually asymptomatic, and the disease is found occasionally, in contrast to the patients with plasma-cell type who are often symptomatic at the time of diagnosis. Castleman's disease is most frequently described in the radiology and pathology literature as located in the mediastinum but may be found in other anatomic regions [1]. Castleman's disease most commonly manifests as a localized mass. Imaging studies may aid in the diagnosis of CD, especially in the hyaline-vascular type. CT scan generally shows well-circumscribed mass of soft tissue attenuation, with calcification including punctate, coarse, peripheral, and arborizing patterns occasionally. These calcifications combined with an intense enhancement are characteristic imaging manifestations suggestive of hyaline-vascular type, different from the other soft tumors such as extraskeletal chondrosarcoma and malignant mesenchymoma [2,3]. Therefore, parapancreatic hyaline-vascular type of CD should be considered when imaging studies show a parapancreatic mass with vessel-like enhancement and characterized calcification, even without clinical symptoms as described in our patient.
Treatment of unicentric CD is predominantly based on surgical resection, which offers the best chance for cure. Complete resection of the lesion provides cure of the disease because there are no reported cases of recurrence [4]. A better understanding of this disease would avoid unnecessary extensive surgery for a benign condition. Patients with the multicentric multicentric CD have a less favorable prognosis and require systemic treatment [5].
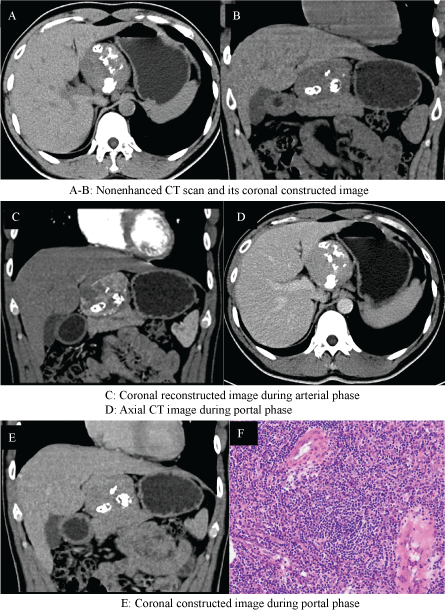
Figure 1: (A-E) CT scan shows a well-circumscribed, round, multiple-calcified mass that appears intensely enhanced in the arterial phase with moderate washout in the venous phase; (F) Histolopathological examination shows a hyperplastic lymph node with large follicles, marked vascular proliferation and hyalinization of the germinal centers.