Phyllodestumours (PTs) of the breast are rare fibroepithelial neoplasms with risks of local recurrence and uncommon metastases [1-3]. They make up 0.3-0.5% of female breast tumours and have an incidence of about 2.1 per million [4-8]. The classification proposed by the World Health Organization for PTs into benign, borderline, and malignantis based on a combination of several histologic features [8].
We report a rare case of a giant malignant phyllodes tumor with metastases to the lung and liver that grew over a 6 years period causing significant ulceration and occasional bleeding.
Malignant phyllodes tumor, Breast, Surgical treatment
A 60-year-old woman came to the outpatient clinic of our breast center with a 6 year history of an important mass of right breast. She reported self-examination of a nodular mass of the inner quadrant of right breast (about 2 cm) 6-years before. The patient had never undertaken a clinical or radiological breast check. The mass had gradually increased by size, and in the three month period before her visit, three skin ulcerations had appeared, with exudation and occasional bleeding. The patient had no fever or anemia. The only symptoms reported were due to faulty posture linked to the weight of the tumor. The worsening symptoms (increased bleeding and exudation and appearance of foul smell) had prompted her to seek medical care.
She had family history of breast cancer (mother at the age of 85-year). Menarche was at the age of 14, one pregnancy at the age of 33 (by caesarean section), she breast-fed for 1 year, and started her menopause at the age of 50. She had followed an estrogen-progestin therapy for short periods in the past. The only significant comorbidity was found to be a GERD in combined therapy with PPI.
Laboratory data were within normal limits except for hemoglobin 10.5 g/dl (range 12-15 g/dl). Physical examination showed a large exophytic lumpy tumor of 43 × 40 cm fully occupying the right breast, with three areas of skin ulceration (about 3 × 3 cm, 8 × 7 cm and 12 × 9 cm) of the outer quadrant.
Her left breast and the rest of her clinical examination were normal. Due to pain and size of the right breast mass, the patient was unable to have a mammography performed. There were no suspicious findings in the left breast or axilla (Figure 1).
The computed tomography showed a giant breast mass with multinodular confluent aspect, inhomogeneous enhancement (due to the presence of necrotic-colliquative components) and the evidence of multiple calcifications in the most caudal portion. The mass affected the soft tissues of the breast full thickness, with infiltration of large and small ipsilateral pectoral muscles. The soft tissues of the intercostal spaces did not always show a cleavage plane with the adipose mass (Figure 2a). It revealed no axillary pathological lymph nodes and nor of the internal mammary chain. The computed tomography scans also showed multiple pulmonary micro-nodular images of non-specific meaning and a solid non-calcified nodule (5 mm) in the lateral basal segment of the left inferior lobe, suspected to be of repetitive nature. After administration of a contrast agent, the left lobe of the liver, segment II, showed an unevenly hypodense nodule (48 mm × 40 mm × 45 mm) associated to a minimum ectasia of some bile ducts in upstream of the injury, therefore suggesting the mass was suspected for metastases (Figure 2b).
It was not possible to perform a preoperative biopsy because the patient refused the procedure. She underwent a right mastectomy with partial resection of the pectoral muscles. The tumor did not appear macroscopically to be invading the chest wall. The tumor was characterized by important angiogenesis with several centimeter-sized vessels.
The wound was closed with no need of skin grafting and the total blood loss was less than 100 cc (Figure 3). The resected tumor was 41 × 32 × 22 cm and weighed 14200 gr (Figure 4) and appeared as a fleshy, multinodular confluent neo-formation with large necrotic, colliquative and calcified areas. Microscopic findings showed a malignancy spindle cell with moderate atypia and high mitotic activity (up to 28 × 10 HPF). Additional section showed a residual epithelial structure sometimes cystic and distorted without heterologous areas. The margin of the resected tumor showed a focal and partial infiltration of the muscle included into the resection. The final histopathological diagnosis was malignant phyllodes tumor.
The patient was discharged on the second postoperative day in a good condition with no wound complications.
Written informed consent was obtained from the patient for the publication of this case report and accompanying images.
The authors declare that they have no competing interests.
All authors participated in the conception and design of the study. DDG and SDA drafted the manuscript and performed the revision of the final document. GF assisted with the literature research and drafted the manuscript. RM drafted the manuscript and performer the revision of the final document. All authors read and approved the final manuscript.
The final systematic editing for language and style, together with preparation for publication, was made by Ornella Cosomati.
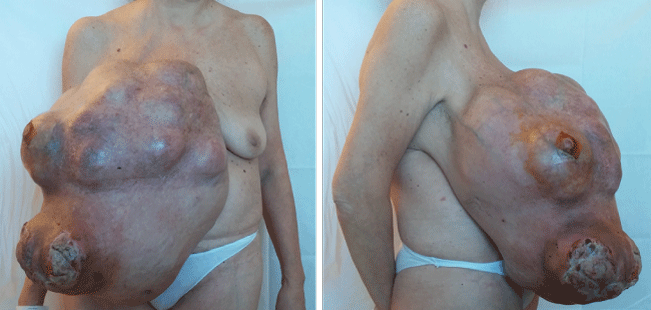
Figure 1: Pre-operative photograph shoving giant right breast mass of 43 × 40 cm with skin ulceration and severe disfigurement.

Figure 2a: The computed tomography shows a giant breast mass only partially included in the FOV due to its size.

Figure 2b: The computed tomography shows suspected liver metastases of 48 mm × 40 mm × 45 mm.

Figure 3: Final result after mastectomy.

Figure 4: The excised mass, 43 × 40 × 40 cm.