A 51-year-old non-smoking man, refered to our pulmonary medicine clinic with a 3 years history of severe shortness of breath. His complaints has increased even more in the last 1 year. There was no history of fever, weight loss, hemoptysis and old cronic infections like tuberculosis. Physical examination appeared bibasilar crackles. The pulmonary function test showed subtle restrictive findings and there was no pathologic findings on the blood examination. Chest X-ray (Figure 1) showed, dense, numerous, bilateral diffuse micronodular opacities predominantly lower zone. Computed Tomography (CT) of the chest (Figure 2) showed symmetrical lower lobe predominant widespread nodular intra-alveolar opacities of calsific density. Also there was diffuse septal thickening (because of calcification) and diffuse ground-glass attenuation (crazy paving pattern) and subpleural multiple small cysts (black pleura sign). Transbronchial biopsy was performed, confirming the diagnosis of Pulmoner Alveolar Microlithiasis (PAM).
PAM is a very rare diffuse and chronic lung disease, characterized by the intra-alveolar accumulation of small spherical calcium phosphate bodies (microliths). It is autosomal recessive disorder and also known as Harbitz' syndrome. The etiology of PAM is mutation in the sodium cotransporter (SLC34A2) gene. Although patients usually have no symptoms and diagnosed by characteristic chest imaging findings during the early phase, this disease has a long and progressive period with deterioration of lung parencyhma. So in the late phase of disease common presentations is restrictive symptoms (dyspnea, non-productive cough, chest pain). The characteristic chest radiographic findings are numerous, diffuse, sand-like, calsific micronoduler infiltration and thin walled subpleural cysts (black pleura sign). CT scan can be benefical in diagnosis. Crazy paving patern and extensive diffusely calcifications are common and major findings on CT. Other CT findings are small subpleural and parenchymal nodules, interlobuler septal calcifications and subpleural cysts. Although the imaging can help in diagnosing of the disease, the diagnosis must confirm with histopathologycally. Currently, there is no specific medical therapy for PAM, the only effective therapy is lung trasplantation [1-4].
None.
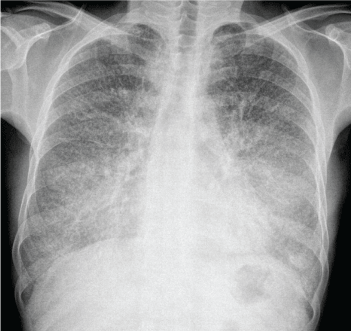
Figure 1: Chest radiogrph shows fine, diffuse, symmetric, dense micronodular (sand strom sign) especially in the basal region.
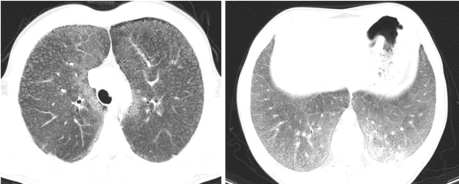
Figure 2: The chest CT shows diffuse, bilateral, lower lobe predominant micronodular calcifications along bronchovascular bundles and crazy paving pattern (ground-glass opacifity and septal thickening). Black pleura sign are also seen.