Intraocular foreign bodies are a major cause of ocular trauma and blindness. Young adults, especially men, are the most likely victims, as a result of industrial or agricultural injuries. The management of orbital foreign bodies remains a serious diagnostic problem, despite development of diagnostic imaging techniques. Ophthalmic examination, including visual acuity assessment, is necessary before and after surgical intervention. With computed tomography accurate foreign body localization is possible.
Eye, Orbital injury, Imaging, Critical care medicine, Maxillofacial Surgery
Penetrated injuries are most difficult injuries of the eye. Intraocular Foreign Body (IOFB) may lodge in any of the structures it encounters, from anterior chamber to the retina and choroid. The management of IOFB remains a serious diagnostic problem, despite development of diagnostic imaging techniques. Here we present a case came to the observation to describe the outlines of our supervision.
A 35-year-old man suffered an injury to his right eye. He presented to an emergency department with the presence of a penetrating injury and an intraocular metallic foreign body. The patient was working as a lawnmower and employing a mechanical device to cut the lawn had hooked a piece of iron remained hidden in the tall grass. At a first clinical examination the clinical condition of the subject appeared discrete. Patient intensely anxious. We proceeded to a clinical and instrumental evaluation (fundus oculi) and with imaging (computed tomography, CT) (Figure 1: Panel A, Panel B). We found good eye pressure at the digital pressure. At the intraoperative examination, the chamber was formed and round and center-shaped optical papilla. Fortunately there was a minimal involvement of intraocular structures with no significative retinal damage. Visual acuity was difficult to evaluate pre-operably but did not seem to be greatly reduced or there were signs of retinal detachment due to massive inflammatory edema. We appreciated a Berlin's edema with temporal choroidal rupture and the presence of a hematoma in the retinal domain from six o'clock to eleven o'clock. The metallic body, though penetrating deep, had not caused vascular injuries. Then proceeded to the cautious removal of the metal body after preservation of the eyeball. Successful operation, When the mydriatic drug was instilled, the pupil dilated regularly.
IOFB is an important cause of poor vision in the young population. Initial management should consist in analyzing the history of the patient (including working anamnesis) and the circumstances of trauma [1]. The ocular examination must be complete (the fundus examination is to explore the macula and papilla) and after a systemic antibiotic treatment has been prescribed the patient is evaluated with a CT scan. Defining surrounding bone and vascular structures by CT is important for surgical removal, so, for the detection of the penetrating foreign body and to evaluate the adjacent structures, we performed a three-dimensional (3D) computer-assisted detection [2,3]. The pre-operative CT scan provides a detailed analysis of the metallic intraorbital trajectory in the orbital cavity. Timely diagnosed ruptures of the posterior segment of eye before the development of traumatic cataract (late complication of IOFB), adequate therapeutic procedures prevent serious complications of IOFB penetrated eye injury such as retinal detachment and permanent reduction of visual acuity [4,5]. Anyway, The CT imaging findings most predictive of an open globe injury were change in globe contour and vitreous hemorrhage. Clinical exam or surgical exploration remains the most important component in evaluating for the examination of ocular globe, with CT imaging as an important adjunct (specially in the presence of clinically evident ocular penetration).
None.
The authors state that they have no conflicts of interest.
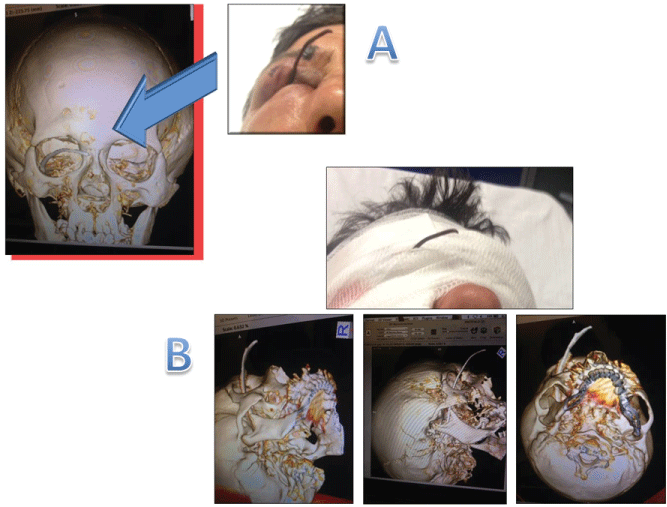
Figure 1: Panel A Three-dimensional computed tomography. We find a metal wire that protrudes outside for about 5 cm and penetrates into the entry point into the right orbital cavity; Panel B Three-dimensional computed tomography images showing the penetration of the metal wire inside the orbital cavity and its relationships with bones, intracranial and vascular structures.