Ophthalmology, Ultrasound, Melanoma, Glaucoma, Nevus
Iris nevi are a common finding on anterior segment exam with growth and conversion to melanoma a relatively rare event. A retrospective case series found that of 1611 lesions referred to a tertiary ocular oncology service, only 8% converted in 15 years [1]. Most lesions are stable, not referred to ocular oncology services, and monitored for growth in the clinic of the comprehensive ophthalmologist with slit lamp examinations and ultrasound biomicroscopy.
A 56-year-old man presented for evaluation of an iris nevus (Figure 1A). Unilateral ocular hypertension was found on outside exam requiring timolol to maintain the intraocular pressure at 19. Ultrasound biomicroscopy of the nevus demonstrated a 4 × 1 mm lesion without angle or ciliary body involvement (Figure 1B). The patient did not return for follow up and was treated for recalcitrant unilateral glaucoma during this time with a trabeculectomy and implantation of two glaucoma drainage devices.
Two years after initial presentation, the patient returned to the ocular oncology clinic (Figure 2A). Visual acuity was 20/100 in effected eye with an elevated intraocular pressure of 25. There was diffuse infiltration of the iris and ciliary body 360 degrees with a lesion height of 4 mm on ultrasound biomicroscopy (Figure 2B). Enucleation with subtotal orbitectomy performed for iridociliary melanoma with pathology confirming diagnosis (Figure 3). He is free of disease without metastases at a follow up of 2 years.
Angle involvement and elevated IOP have been shown to associate with risk for conversion to iris melanoma [1]. Elevated intraocular pressure is a risk factor for metastases [2]. Referral to ocular oncology for dynamic iris lesions, particularly before glaucoma surgery, is warranted.
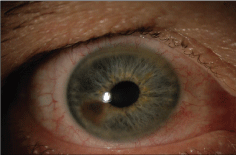
Figure 1a: Photo showing iris lesion encompassing ~2 clock hours, sparing pupillary margin and angle.
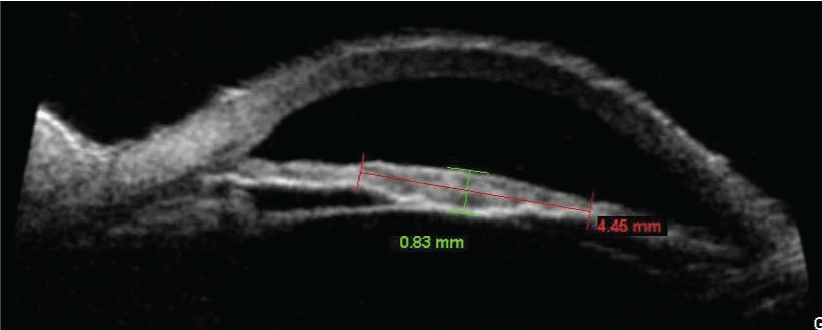
Figure 1b: Ultrasound biomicroscopy across width of initial lesion depicting flat lesion above iris not involving the ciliary body or angle.
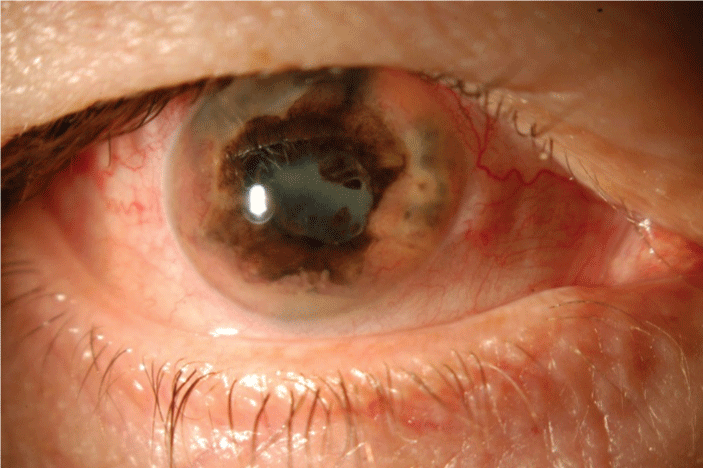
Figure 2a: Photo 2 years later showing diffuse infiltration of iris 360 degrees by the melanoma, which is both melanotic and amelanotic. Superotemporally the tumor wraps around the tube of the implant.
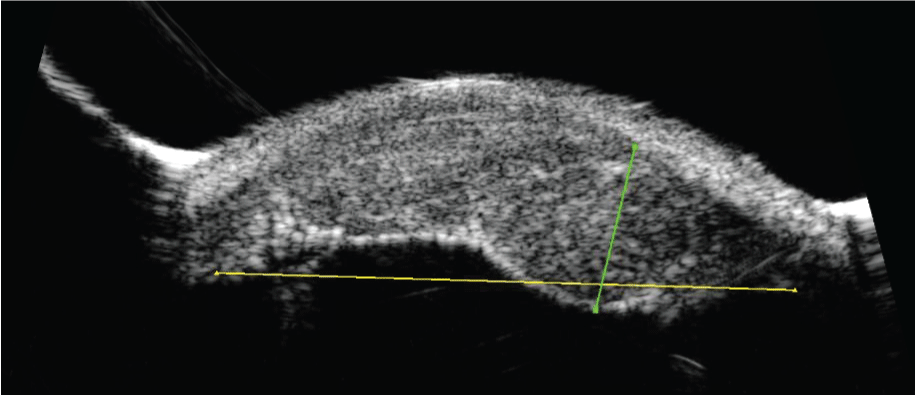
Figure 2b: Ultrasound biomicroscopy 2 years later at level of initial lesion. The lesion has invaded the angle and ciliary body. Its height has increased to encompass entire anterior chamber abutting the cornea.
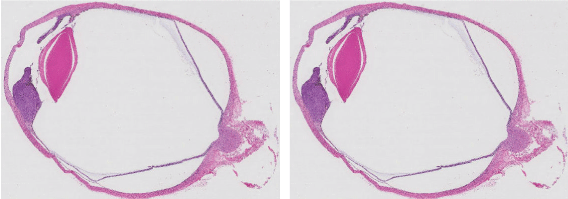
Figure 3: H&E stain of enucleated eye showing iridociliary melanoma.