Gorlin Goltz syndrome, or Nevoid basal cell carcinoma syndrome, is known as a rare autosomal dominant hereditary disease.
Like most syndromic diseases, it is responsible for systemic damage. Nevertheless, the main and feared type of affection is dermatological lesions of basal cell carcinoma type. The genetic expression lies in the mutation of the PTCH gene, a tumor suppressor, located on the long arm of chromosome 9.
Gorlin goltz syndrome is a rare hereditary disease known essentially for the malignancy of the dermatological lesions.
The purpose of this article is to present the particularities of dermatological damage that can be source of confusion for establishing the diagnostic. We will proceed to a description of this syndrome through a case followed in department of ORL and Maxillo facial surgery of RABAT, we will proceed to a description of this syndrome.
This is a young adult of 23-years-old who suffers from dermatological lesions on the face. He has had congenital blindness since childhood, his sister and father died due to complications of undocumented dermatological lesions.
In his history, the patient benefited 1 year ago from the removal of an ulcerous lesion on the face's skin, which turned out to be benign (Figure 1 and Figure 2).
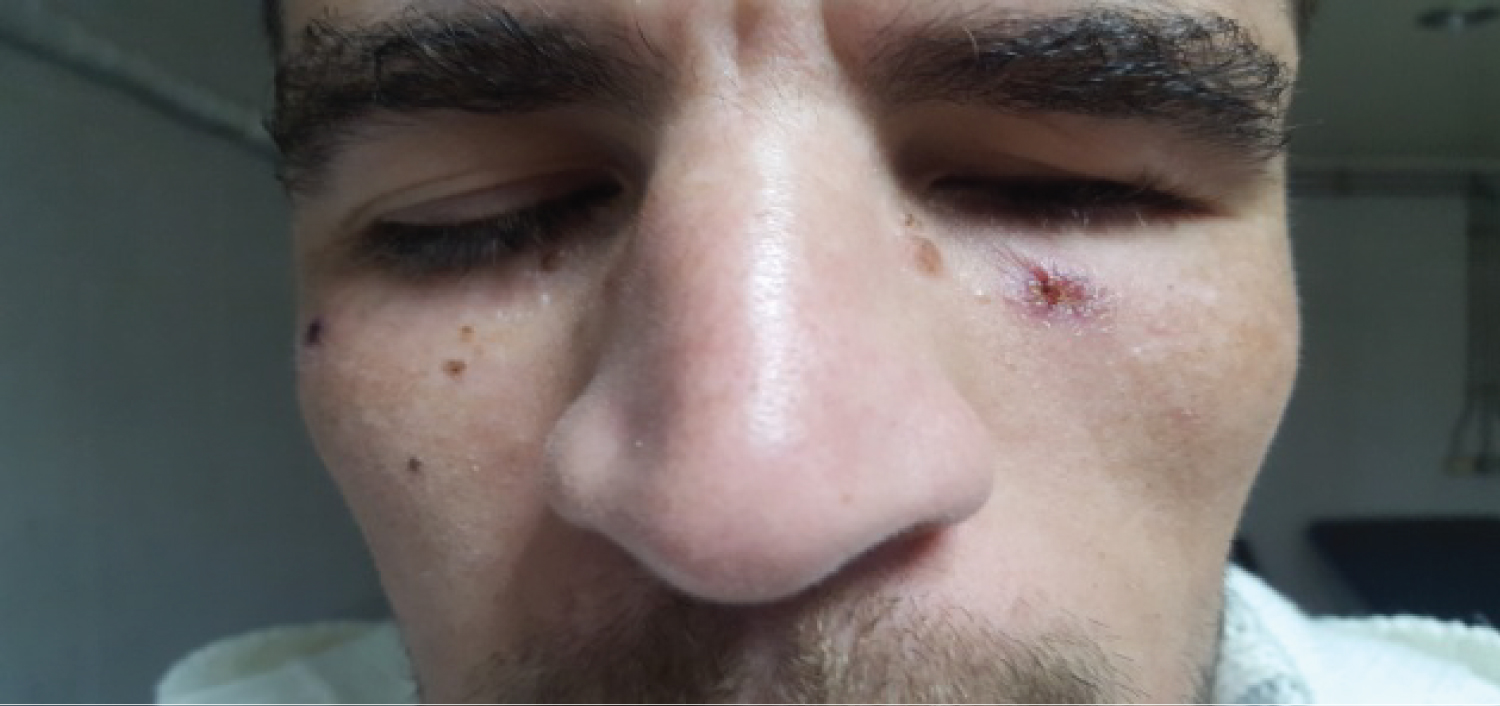 Figure 1: Infra-orbital skin ulceration.
View Figure 1
Figure 1: Infra-orbital skin ulceration.
View Figure 1
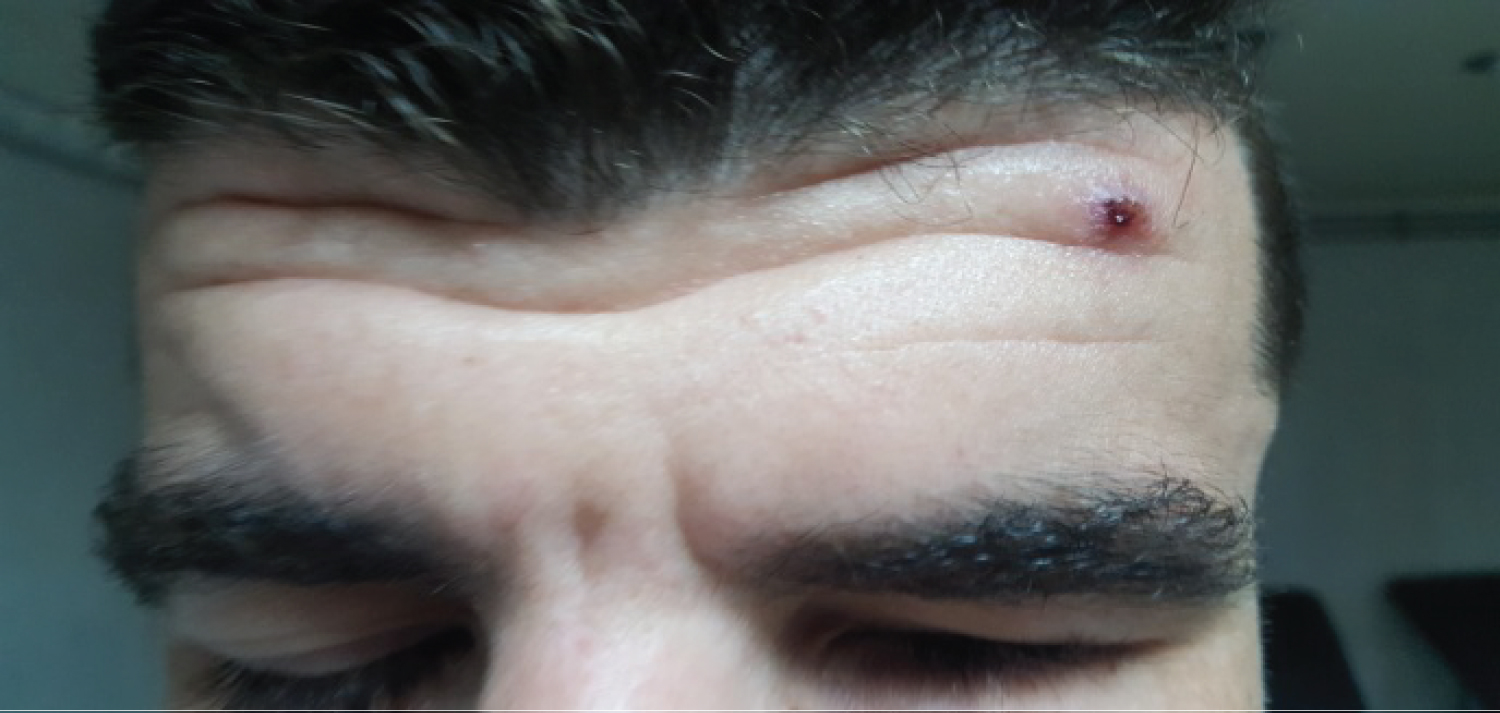 Figure 2: Frontal skin ulceration.
View Figure 2
Figure 2: Frontal skin ulceration.
View Figure 2
One month ago, the patient was hospitalized in the emergency room due to cellulitis of dental origin. The CT scan of the face revealed the presence of mandibular cysts (Figure 3).
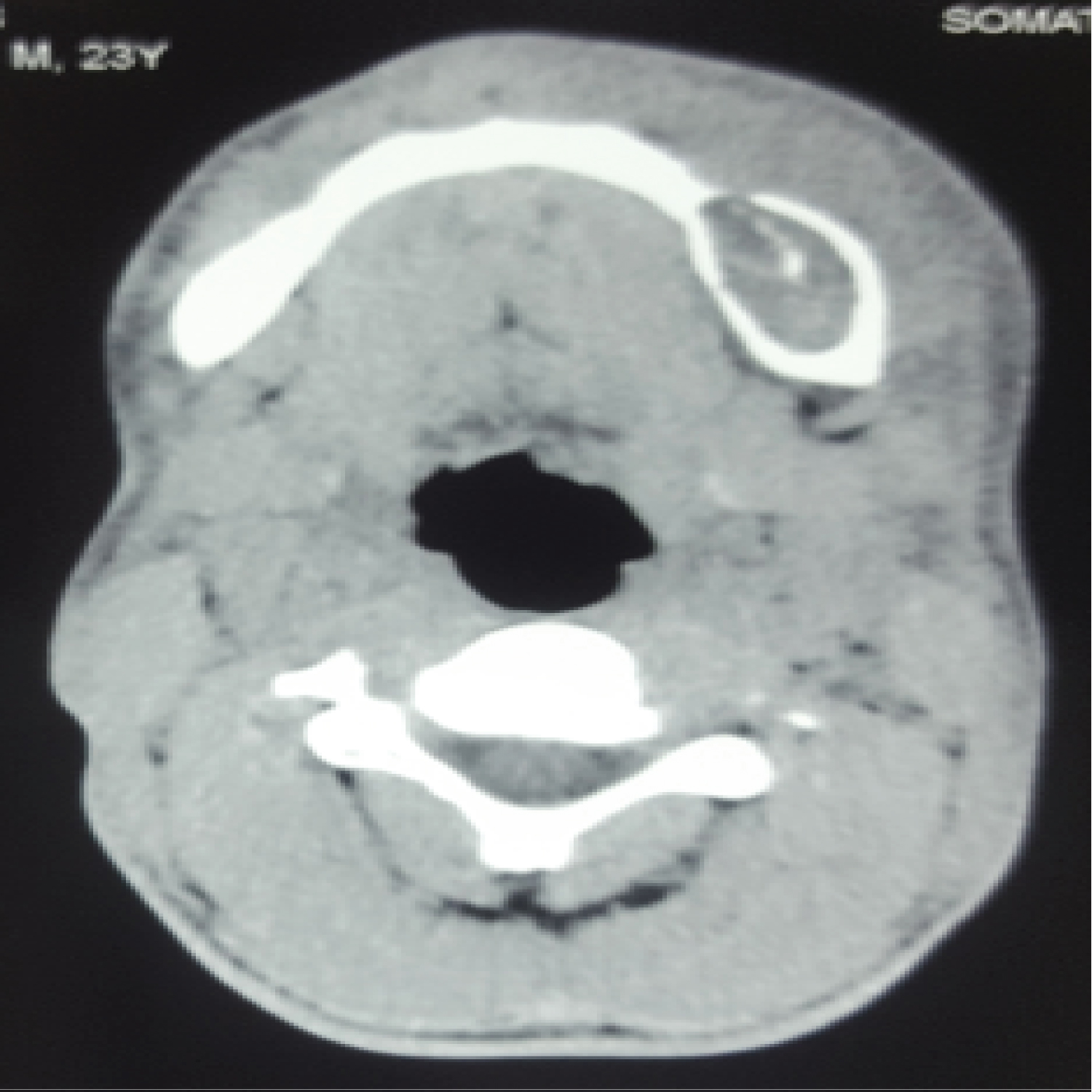 Figure 3: Mandibular cyst discovered in ct-scan for cellulitis.
View Figure 3
Figure 3: Mandibular cyst discovered in ct-scan for cellulitis.
View Figure 3
A genetic study had been done, also based on family history and clinical signs, which turned to be in favor of Gorlin Goltz syndrome.
The patient is currently still being followed in our department in collaboration with a team of dermatologists.
The severity of genetic diseases is usually based on the number and especially the quality of the genes involved. The clinical manifestations are often variable, but some have a higher frequency than others depending on the type of the syndrome. In basal cell nevomatosis, or Gorlin Goltz syndrome, it is mainly dermatological damage that is most often found. As indicated in the name of the disease, it refers to nevi and basal cell carcinomas. Several other lesions have been described in the context of Gorlin Goltz Syndrome.
As observed in the case of our patient, we note the presence of ophthalmologic lesions and mandibular cysts in association with the above-mentioned dermatologic lesions.
Cutaneous nevi with basal cell carcinoma represent major criteria of the syndrome; these lesions present an important evolutionary and degenerative power [1], it is the reason for a close follow-up of these patients.
Several other dermatological lesions are found such as Palmoplantar keratoderma, epidermoid cysts, molluscum pendulum, café au lait spots, milia and areas of hyperpilosity [1].
In the ocular manifestations we find both benign anomalies such as refractive disorders, strabismus, or more serious lesions such as microphthalmia, glaucoma and tumors.
Our patient has congenital blindness of the left eye in association with a homolateral ptosis related to a neurological disorder.
Several other abnormalities were described including neurological and osteoarticular manifestations. The diagnostic criteria were defined by Kimonis by diagnosing Gorlin Goltz syndrome if two major criteria are met or one major and two minor criteria [2]. The major criteria are mainly dermatological lesions, mandibular keratocysts, osteoarticular lesions and family history. The minor criteria are represented by less frequent anomalies such as ovarian fibroids, medulloblastoma and other neurological and skeletal anomalies.
Basal cell nevomatosis is mostly diagnosed following genetic study revealing the mutation of the PTCH gene, which is a tumor suppressor gene found in the long arm of chromosome 9 [3].