True tracheal bronchus is an aberrant bronchus arising above 2-6 cm from carina, from the lateral wall of trachea and directed towards the upper lung lobe [1]. Frequently located on the right side, it can be further described as supernumerary if there is an anatomic right bronchus with normal segmental apical, anterior and posterior bronchi. It is considered displaced if it's accompanied by an absence of anatomic segmental bronchi. Tracheal bronchus can supply the entirety or part of the upper lung parenchyma [2]. Incidence described in the literature ranges from 0.1 to 1% reported in different studies. Prevalence of right tracheal bronchus has been reported as 0.1%-2% and left tracheal bronchus a prevalence of 0.3%-1% on bronchographic and bronchoscopic studies [3]. However, the incidence of 0.31% was reported via multidetector computed tomography (MDCT) analysis in a study of 9k cases. With the advent of advanced imaging techniques, its detection has become easier [4]. We described a rare presentation of tracheal bronchus in late adulthood in the form of recurrent respiratory infections.
We present a case of a 59-year-old, non-smoking, Caucasian female of Eastern European descent. She had a past medical history significant for chronic bronchiectasis and peptic ulcer disease. She was presented to our clinic with complaints of pleuritic chest pain associated with productive cough. The patient had similar symptoms in the past and was diagnosed with bronchiectasis in 2014 via a CT scan of the chest. She had undergone a bronchoscopy during that time, which was non-diagnostic. Since then, the patient's home medications included a regimen of albuterol, long-acting beta-agonist, and inhaled corticosteroids, which controlled her respiratory symptoms.
Upon examination, her vital signs were found to be stable with an O2 saturation of 97% on room air. Lung auscultation revealed diffuse rhonchi bilaterally. The rest of the physical examination was unremarkable.
Given the patient's history of chronic bronchiectasis previously controlled but now unresponsive to LABA/ICS, a CT scan of the chest with contrast was done. Compared to her previous CT scan in 2014, new peribronchial opacities were noted in the right upper lobe. Flexible bronchoscopy with bronchoalveolar lavage (BAL) was performed. Findings revealed normal vocal cords, severe erythema and inflammation of the bronchial mucosa with purulent mucous secretions and an accessory bronchus arising within 2 cm proximal to the carina on right lateral wall, at the 9 and 10 o'clock position (as shown by blue arrows in Figure 1). The opening of the bronchus was approximately 8-10 mm, and the scope was successfully introduced into the bronchus for 1 cm. Saline lavages into the bronchus returned with saline and air bubbles on multiple attempts, confirming the presence of communication between the tracheal bronchus and lung parenchyma. BAL was negative for fungal culture. AFB smear and 6-week culture, chlamydial PCR, viral culture, mycoplasma antibody, legionella direct fluorescent antibody were negative. However, the BAL gram stains and cultures grew pan-sensitive Pseudomonas Aeruginosa. The patient was started on levofloxacin.
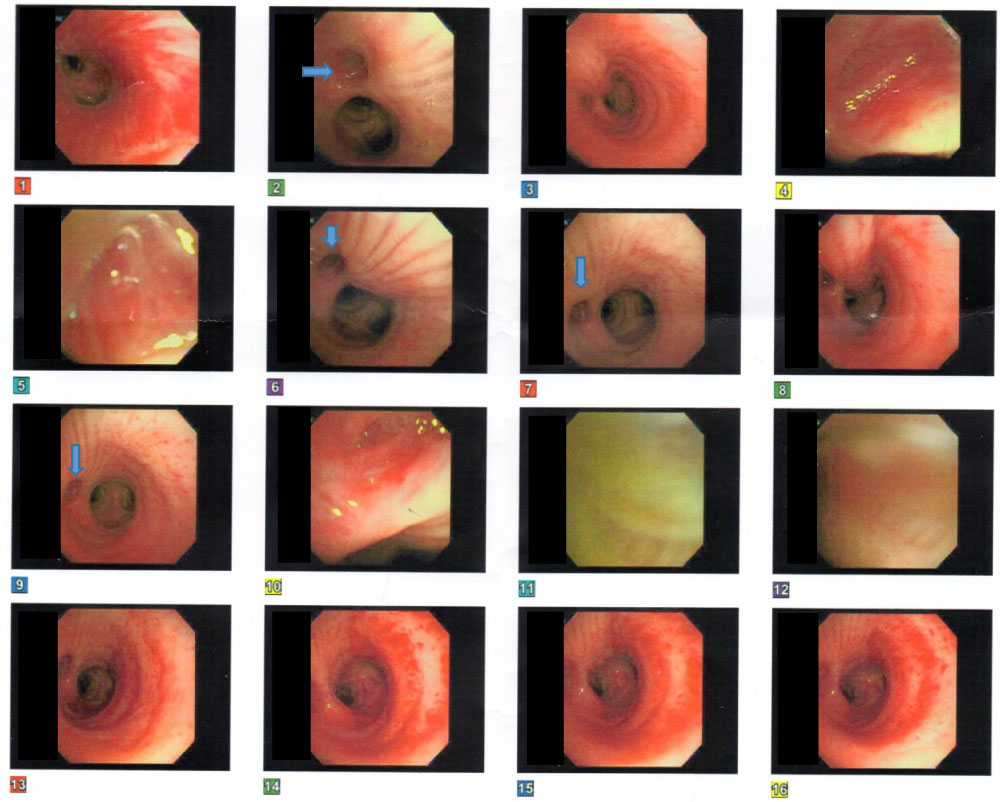 Figure 1: Arrows points towards origin of tracheal bronchus at 9, 10 O' clock positions above the carina.
View Figure 1
Figure 1: Arrows points towards origin of tracheal bronchus at 9, 10 O' clock positions above the carina.
View Figure 1
CT chest with 3D reconstruction was ordered but due to lack of availability, high resolution computed tomography (HRCT) was performed, which showed persistent bilateral bronchiectasis. Subsequent imaging with HRCT and bronchoscopies was stable after the initiation of long-acting beta-agonists, long-acting muscarinic antagonists, inhaled corticosteroids, and antibiotics. However, the symptoms of productive cough with sputum persisted, despite therapy. The patient was referred to and is still following up with the infectious disease specialist for cyclic antibiotic treatment. The patient was referred to cardiothoracic surgery for upper lobe segmentectomy or lobectomy as definitive treatment.
Tracheal bronchus, also called "bronchus suis" is a normal finding in pig and other ruminant animals such as cattle, sheep, and giraffes [1]. True tracheal bronchus, in most cases described in the literature, was found as an incidental finding during or after intubation. Tracheal bronchus has been frequently found in children where it manifests early in the form of recurrent respiratory infections. In children, it is found as a part of multiple congenital abnormalities e.g. tracheoesophageal fistula, tracheal stenosis, Tetralogy of Fallot, VATER syndrome, and Down's syndrome [2]. Other incidental findings include squamous cell cancer, large cell cancer, tuberculosis, leiomyoma, bronchial carcinoid, and actinomycosis.
The underlying cause is usually a congenital malformation. Many theories have been proposed including selection theory, reduction theory, and migration theory.
It can be symptomatic if there is any aberrancy in venous drainage or ventilation. In that case, it can present itself as recurrent infections, wheezing, and atelectasis. Such presentation in late adulthood has been described only in a few other cases in the literature [3,4].
Our patient had recurrent infections leading to frequent hospitalization. Antibiotic treatment courses were given without any underlying known etiology. Successive CT scans showed re-demonstration of worsening right middle and upper lobe infiltrates. A careful review of CT scan chest shows tracheal bronchus at the T2-T3 level at the level of pulmonary vessels next to the main trachea (Figure 2). Bronchoscopy revealed the tracheal bronchus and confirmed its communication with the lung parenchyma.
 Figure 2: Abnormal tracheal bronchus supplying right upper lobe next to the main trachea at level T2-T3.
View Figure 2
Figure 2: Abnormal tracheal bronchus supplying right upper lobe next to the main trachea at level T2-T3.
View Figure 2
It's not clear why the patient remained asymptomatic during a major part of her life. Her current symptoms might be the result of abnormally narrowed tracheal bronchus, impairing the ventilation process. A study comparing the airflow distribution between normal lung and tracheal bronchus subjects revealed decreased aeration in comparison to the rest of the lung [5]. Further investigation is needed to reveal underlying contributing factors.
MDCT with the addition of 3D reconstruction has been the gold standard in diagnosing tracheal bronchus. The 2D and 3D feature helped significantly in identifying and differentiating intra and extra luminal pathologies in the tracheobronchial tree [6].
Adult patients who present with recurrent respiratory infections must be evaluated for rare congenital anomalies like tracheal bronchus. MDCT imaging modalities play a vital role in identification of tracheobronchial tree anomalies.
None.
All authors have equal contribution towards the preparation of this article.