The reconstruction of hypopharynx and larynx post ablative surgery has been always a demanding challenge. Not only the restoration of the anatomy and achieving robust wound healing, but also the complexity of function in the area for the airway and upper digestive tract not to be compromised. Moreover, the age of this group of patients and perioperative radiotherapy adds to the existing obstacles in reconstruction.
The evolution of microsurgery and free tissue transfer replacing the previous gold standard pedicled flaps revolutionized the head and neck reconstruction.
It became a necessity to elicit how far the head and neck reconstruction practice has gone around the globe and what is considered the gold standard technique for reconstruction of each of the defects encountered at the present time.
We performed a systematic review appraising the current head and neck reconstruction practice around the world aiming at concluding the gold standard methods of reconstruction of the defects in this area.
Search strategy: Medline using the PubMed interface on 1st of October 2020.
236 papers were found. Of which 66 publications in the last 10 years were shortlisted reflecting the most recent practice. 20 of these were identified addressing the reconstructive approach Figure 1.
Various reconstructive methods are reliably used in certain indications with comparable results around the globe. We present an unprecedented evidence-based universal algorithm for post ablative surgery reconstruction for the laryngeal and pharyngeal defects.
Exp larynx reconstruction, Pharynx reconstruction, Tumour, Oncology
In the field of reconstructive plastic surgery one of the most technically challenging and demanding topics following oncological resection is the hypopharynx and laryngeal reconstruction. Laryngeal and hypopharyngeal defects following ablative procedures can result in complex deficits with possible detrimental effects from a medical and a social point of view. Larynx is the second most common site of upper aerodigestive tract malignancies in which cases wide excision of the local structures is required, resulting in clinically significant defects of varying extent [1]. A variety of techniques have been utilized to provide the adequate result. Modern advances in reconstructive plastic surgery have significantly improved the options in the armamentarium of the surgeon to offer the most suitable and functional result. These include both free and local flaps. However, each form of reconstruction apart has its own advantages and disadvantages which can affect the final choice of reconstruction depending on the deficit and the patient.
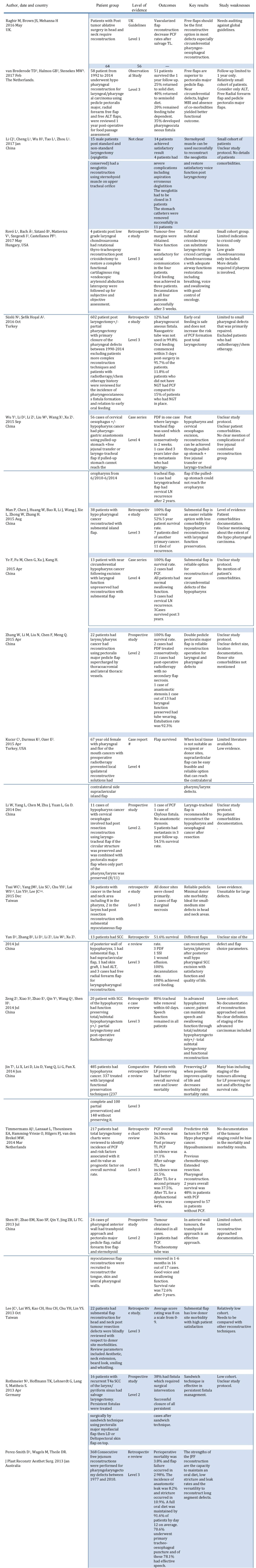 Figure 1: Relevant papers.
View Figure 1
Figure 1: Relevant papers.
View Figure 1
Small pharyngeal defects with remnant pharyngeal mucosa width of > 3.5 cm can be effectively dealt with primary closure [2-4]. The simple yet effective technique does not require microsurgical skills and can be performed in a setting of smaller and less equipped hospital [3,5]. However high rates of pharyngocutaneous fistula and stricture are associated with this type of repair. Early enteral feeding however can be initiated as show by a study by Suslu, et al. in 602 patients, in the 582 of the group early enteral feeding was initiated within 3 days of surgery with fistula rates at approximately 11% [6].
When defects are larger and primary closure of pharyngeal deficit is not possible, then flap based reconstruction is indicated. One of the most commonly used flaps is the pedicled myocutaneous flaps is the pectoralis major pedicled flap. This particular flap is a safe, reliable and commonly used solution, providing a good bulk of tissue while requiring only one team approach without the need for microvascular experience in a significantly lower operative time compared to free flap reconstruction [7-9]. However, the bulkiness of the donor site [7,9,10] and the resulting poor functional outcomes compared to free flaps [11-13] both in terms of speech and swallowing are major disadvantages. Furthermore, its higher rate of stenosis and fistula compared to other means of flap reconstruction [14,15] as well as the donor site complications which can affect the range of movements of the upper extremity and the chest wall expansion [9]. The radial forearm flap offers another good alternative for pharyngeal reconstruction for such deficits. It is considered a safe, relatively simple, pliable and reliable flap with a sufficiently long pedicle [9,14,16]. The main disadvantage of the radial forearm flap is the delicate nature of the donor site which requires meticulous flap elevation and can result in post-operative complications that can have severe impact on the hand function and therefore the quality of life. Also, the colour mismatch and the hair bearing skin of the donor area can create a suboptimal aesthetic outcome [9,10,14].
In cases of more extensive defects where less than 1 cm pharyngeal mucosa remains, a more radical approach is required. Free jejunal transfer is a useful technique when the gastropharyngeal anastomosis cannot be utilised due to inability of the stomach to reach up to the pharynx [17]. The ability of replacing the hypopharyngeal defect with an already tubed flap from another part of the digestive tract has been one of its main advantages. Moreover, it has a long pedicle with adequate diameter which can support an equally long length of flap with low flap failure rates. Also the flap maintains its peristaltic activity however this is not coordinated with the remaining tissues which can cause swallowing problems. Furthermore, the commonly reported "gargly" and "moist" character of the voice [17-20]. A study of Perez, et al. [19] however showed high rates of maintained oral diet up to 90 % and effective speech results up to 78.1% in 368 patients. Another major disadvantage is the associated need for abdominal approach and the potential life threatening perioperative and post-operative donor area complications. The abdominal visceral can offer another free flap, the gastro-omental free flap [2,21]. The flap offers a significant amount of vascularised omentum to be used for coverage of the anastomosis, the dead space and the main blood vessels of the area which makes it ideal for complicated surgical sites. Just like the jejunum flap it can gap lengthy defects due to its long and reliable pedicles [21]. However, the flap has high stricture rates [14] and the flap requires a far more extensive operation which can increase the operative risks. Last but not least the flap is subject to the same intraabdominal complications as the jejunal flap.
The free fasciocutaneous flaps form another important weapon in the armamentarium of the reconstructive surgeon. Radial forearm and anterolateral thigh flap consist of the two most commonly used free flaps which are fabricated in a circumferential fashion to cover the deficit. Radial forearm as previously discussed it is considered a safe, relatively simple, pliable and reliable flap with a sufficiently long pedicle which can be tubed over a salivary bypass tube for better results. However, the rate of fistulas and stenosis are higher compared to ALT flap. Other disadvantages include poorer functional outcomes, the hair bearing skin, the colour mismatch and the donor site complications as previously mentioned. ALT flap is a very common and popular flap [10,22,23] it has become an alternative reconstructive option to the radial forearm flap regarding hypopharyngeal reconstruction. It can be used in many forms similarly to radial forearm flaps for both extended and partial deficits. As the radial forearm flap it's a reliable and safe flap with equally low perioperative mortality and flap failure rates [14,22,24]. The rates of percutaneous fistulas and stenosis are also lower than the radial forearm's. The donor site complication rates are approximately at 7% with minimal effect on the mobility of the patient. The flap can offer large skin islands which can be utilized for simultaneous resurfacing of the skin defects in the area. The distal area of donor site facilitates a two-team approach which can help shortening the operative time, as well as the constant and reliable pedicle which provides a straightforward harvesting of the flap.
Also the functional results in terms of speech and swallowing are shown to be equal or even better than of other fasciocutaneous or jejunal flaps [22,25,26,27] with better quality of voice and high rates of achieving tracheoesophageal speech. The advantages make the flap also adequate for previously untreated cases as tubed flap. The main disadvantage of the flap is the bulkiness of the flap compared to other flaps, especially in cases of obesity. This necessitates a time-consuming thinning of the flap which can endanger the suprafascial vascular plexus and therefore the flap viability [10,24,28].
In cases of salvage procedures (post radiation or chemotherapy) a greater amount of soft tissue is required to allow adequate coverage of the deficit. Gastro-omental free flap is considered to be a reliable solution to this situation. The flap offers a big amount of well vascularised omentum to allow coverage of all the exposed structures with a lower rate of percutaneous fistulas compared to the jejunal flaps [21,29,30,31]. Furthermore, it is a long flap that can bridge defects up to 30 cm, it offers good plasticity of the gastric antrum and the greater omentum for simultaneous coverage of the deficit and the exposed structures which is also thinner compared to the more bulkier ALT flap and a good vessel calibre [29-32]. These advantages make it a good option for cases of an unfavourable recipient site. However, the flap necessitates a good general health in order to tolerate the required laparotomy and the surgically more complicated intraabdominal procedure. Furthermore, the possible complications from the donor site along with the perioperative mortality associated with such complications are some of its disadvantages that must be taken into consideration. The flap can be combined with skin resurfacing with an ALT flap in cases when further resurfacing is required with the disadvantage of an even more prolonged and demanding operation [29-32].
If the deficit is too long and the length of the available flaps is not sufficient to cover the deficit of a required oesophagectomy, gastric pull through can be utilized to replace the oesophagus. Its advantages include a one stage procedure which can gap extensive deficits and it requires only one anastomosis to be performed. The disadvantages are similar to gastro-omental flap and are associated with the necessary intraabdominal operation plus the morbidity and mortality of the operation. The gastric pull through combined with the use of a jejunal free flap it can be used to bridge deficits up to the oropharynx as described by Wu, et al. A similar technique is the colon transposition flap that offers the advantage of having a higher reach compared to other visceral flaps but due to the high complication rates it uses is mostly limited to cases where the gastric pull up technique is unavailable due to concurrent malignancy or previous surgery in the area.
In cases of percutaneous fistula, vascularised tissue from outside the irradiated area is recommended and can significantly reduce the rate of such complications, but at the cost of an additional procedure. Rothmeier, et al. [23] described the use of sandwich technique for managing persistent fistula cases by using multiple flaps and providing the area with a muscle layer and epithelium that act as a secure barrier and therefor reduce the chances of further fistula creation.
Last but no least the submental flap offers a good local flap alternative. It is easily harvested, pliable and reliable flap that can utilized for smaller deficits. It has a low rate of complications as showed by Lee, et al. in a retrospective analysis of 22 patients. However, the flap although pliable cannot be utilised in cases of larger deficits or in cases of previous radiotherapy [28,32,33].
Meta-analysis of the literature showed marked evolution in the hypopharynx and larynx reconstruction approaches post oncological ablative surgery. The traditional usage of pedicle regional flaps such as pectoralis major was combined with robust free flaps such as ALT and free radial forearm flap along with new evolving submental flaps enhancing the speech and swallowing function restoration and decreasing associated comorbidities such as aspiration and persistent PCF.
New evolving horizons in surgical techniques means that allotransplantation has become a possibility for complex defects providing like for like replacement of tissues and potentially aiming at normal functional outcomes, both for voice and swallowing as Grajek M, et al. showed in their pioneering First Complex Allotransplantation of Neck Organs: Larynx, Trachea, Pharynx, Esophagus, Thyroid, Parathyroid Glands, and Anterior Cervical Wall [34] [Table 1].
Table 1: Conclusion. View Table 1
The authors have no conflict of interest to declare.
No funding was obtained to produce this publication.