The objective of this study was to assess whether patient instructions for the post-operative period are best remembered when given well before, just before or after surgical removal of a third molar. Also, the effect of preoperative anxiety on memory and pain was evaluated. A total of 105 patients were included. Baseline anxiety levels were assessed by a questionnaire. Next, patients were assigned to one of three groups in which the instructions for the postoperative period were given verbally before (in the consulting room), just before (in the treatment room) or after the surgical procedure (in the consulting room). The patient information consisted of 10 different items. Twenty minutes after the instructions were given, the patients were interviewed to assess the amount of instructions remembered. In addition, the level of post-operative pain was measured using a visual analogue scale (VAS).
Mean spontaneous recall score of the 'just before' group was significantly lower (2.8 ± 1.7 out of 10 items remembered) than in the 'after' group (3.7 ± 2.2 items remembered). There were no significant differences between the pain and anxiety levels. No correlation could be found between anxiety and memory score, or memory score and pain. In summary, instructions for the post-operative period are best remembered when given after the removal of a third molar.
Third molar, Memory, Instructions
In oral surgery, patients are routinely informed about their treatment and what to expect afterwards. This includes advice on wound care and pain management. The patient is supposed to remember the information given and this would contribute to a less bothersome postoperative period [1,2]. The effect of providing verbal information and instructions to the patients could lower anxiety [2,3] and postoperative pain [4-6]. However, verbal information is generally not well remembered [7], which may be especially true for oral surgery procedures as these procedures are generally considered as stressful [8-13]. Accordingly, it has been hypothesized that instructions should not be given immediately before the surgical procedure [8]. To assess if the timing of giving information to the patients has an effect on the amount the patient can recall and on postoperative pain levels, we decided to assess this further in patients referred for third molar removal. Possibly the timing of information given to the patient may be relevant and can be used to optimize our patient care regarding pain and postoperative self-care and awareness.
The inclusion criteria were an indication for the surgical removal of one lower third molar (right or left side) under local anesthesia, aged between 16 and 65 years, and no recent third removal surgery (< 6 months). The exclusion criteria were mental retardation, language barriers, recent third molar removal (< 6 months), pregnancy and the use of anxiolytic medication.
When patients were considered eligible to participate in the study, these patients were informed about the study. It was specifically stated that the study was about the patient information and assessment of postoperative pain. It was NOT mentioned that memory function was to be measured since this would trigger the patient to memorize.
The study was approved by the Medical Ethical Committee (METc).
Patients who were scheduled for third molar removal were approached by phone several days prior to the surgery. When included, patients were assigned to the three groups as follows: The first 5 consecutive patients were assigned to the standard group, receiving patient information in the treatment room. The second 5 consecutive patients were assigned to the preoperative group, receiving patient information beforehand. The third 5 consecutive patients were assigned to the postoperative group, receiving patient information afterwards. The next 5 consecutive patients were assigned back to the first group, and so forth.
Per patient the total procedure was followed-through in one session. Below the protocol per group is presented in more detail.
The patient is given local anesthesia in the operating room in the operating chair. Thereafter, the standardized 10 items patient information (Table 1) was given just before the actual treatment, i.e., just before the nurses were putting drapes onto the patient and were unpacking the surgical trays. After removal of the third molar, the patient went to the hospital pharmacist to receive pain medication and returned to be interviewed.
Table 1: Overview of the 10 items of patient information. View Table 1
Standardized patient information was given verbally in a separate consulting room several minutes before treatment. Thereafter, the patient went to the treatment room where local anesthesia was given, while the nurses were putting drapes onto the patient and were unwrapping the surgical trays. After removal of the third molar, the patient waited in the waiting room until 20 minutes were past after the start of giving information. Then the patient was interviewed in the consulting room.
The standardized patient information was given in the consulting room, after removal of the molar. The patient went to the hospital pharmacist for pain medication and back to be interviewed.
Care was taken to allow 20 minutes between the information given and the interview. The time periods were recorded by a stop-watch. No written patient information was handed out in the meantime in which the information could be read. An overview of the protocol is presented in Figure 1.
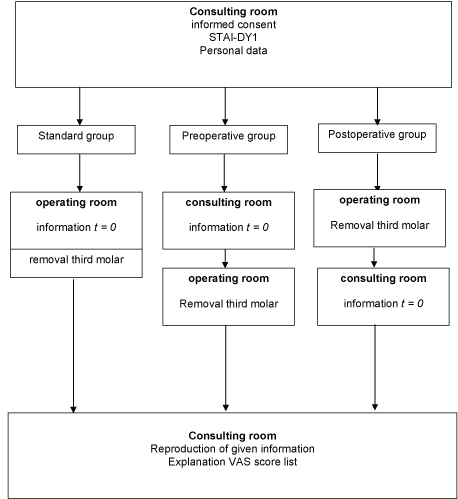 Figure 1: In the consulting room, participants are informed about the study and informed consent was obtained. The participants fill in the STAY-DY1 for determining the level of (baseline) anxiety. The patients were assigned to one of three groups.
Figure 1: In the consulting room, participants are informed about the study and informed consent was obtained. The participants fill in the STAY-DY1 for determining the level of (baseline) anxiety. The patients were assigned to one of three groups.
When in the standard group, the patient went to the treatment room where the standardised information was given and the third molar was removed.
In the preoperative group, the patient received the patient information in the consulting room, before going to the treatment room.
In the postoperative group, patient information was given after the removal of the third molar, back in the consulting room.
A time elapse of twenty minutes was taken into account for all groups between receiving information (t = 0) and the interview in the consulting room.
Afterwards instructions on use of the VAS score list were given.
View Figure 1
Prior to the surgical procedure, all patients were asked to complete the Dutch version of the State Trait Anxiety Inventory (STAI DY-1) [14]. This scale contains 40 items on a self-reported questionnaire regarding state of anxiety and is to be completed on a 4-point response scale. The 4-point rating scale for state anxiety comprised 1) Not at all, 2) Somewhat, 3) Moderately and 4) Very much anxious. The score ranging from 20-80, with a higher score correlating to greater anxiety.
The patient information consisted of a standardized list of 10 specific items (Table 1) that were all explicitly mentioned to the patient once. Care was taken not to repeat any item. Plain memory function was measured by scoring one point for each of the items remembered spontaneously, by asking what the patient 'could remember of the things said'.
In addition, 'hint' memory function was scored with standardized 'hints'. For example; when a patient could not reproduce spontaneously what to do with persistent bleeding, but could answer the question by hinting: 'what about bleeding?' a point was scored. A maximum of 10 points could thus be scored (all items remembered).
Postoperative pain was measured using a 100 mm VAS scale, ranging from 0.0 (no pain) to 10.0 (worst pain imaginable). Patients were asked to measure pain on a daily basis in a log-book until pain free. Pain scores were analyzed on day 1, 3 and 7, because in general, pain levels are mostly reduced after one week.
A difference of VAS 1.5 between the groups was considered clinical significant. A power analysis based on a standard deviation of the visual analogue scale (VAS) on pain perception of 1.4, and a difference of 1.3 between the means was used for group size assessment (data from pilot study, not shown). A power calculator for ANOVA sample size, with an effect size (F) = 0.4714, produced a sample size needed of 48. To correct for non-normal distribution, a total sample size of 90 was needed.
For the analysis both parametric and non-parametric tests were used. One-way ANOVA was used when normal distribution could be achieved. A Kolmogorov-Smirnov (K-S) test and a Shapiro-Wilk (S-W) test were used as a test for normality. The non-parametric Kruskal-Wallis test was used in non-normal distributions. Prior to each Kruskal-Wallis test, a Levene's test for equality of variances was performed to confirm homogeneity of variance between the groups for the different variables discussed. For the post hoc testing a Mann Whitney U test was used to detect significant differences between the groups individually. Before this test was performed, a Bonferroni correction was applied and therefore controlling for type I error.
Correlations were studied with a Pearson- or a Spearman correlation test, to determine any influence of level of education, age and preoperative anxiety on (recall) memory as well as between (recall) memory and pain. In addition, the influence of the method of surgery, duration of surgery and preoperative anxiety levels on postoperative pain were investigated to detect possible associations.
A total of 130 patients were asked to participate of which 105 were willing to do so (Figure 2). All patients complied with the study protocol. Surgical removal of the third molars was uneventful and could be accomplished within 20 minutes.
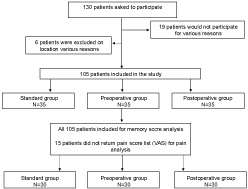 Figure 2: A total of 130 patients were asked to participate. 19 patients would or could not participate for various reasons; no time (n = 2), not interested (n = 3), too scared (n = 1), language barrier (n = 2), prior surgery (n = 5), no show (n = 6). On location another 6 participants were withdrawn; too scared (n = 1), unable to return Vas list (n = 1), mental retardation (n = 1), no third molar removal necessary (n = 2), unable to take analgesics (n = 1), for the memory analysis 105 patients were included and assigned to one of three groups. For the pain analysis 90 patients were included.
Figure 2: A total of 130 patients were asked to participate. 19 patients would or could not participate for various reasons; no time (n = 2), not interested (n = 3), too scared (n = 1), language barrier (n = 2), prior surgery (n = 5), no show (n = 6). On location another 6 participants were withdrawn; too scared (n = 1), unable to return Vas list (n = 1), mental retardation (n = 1), no third molar removal necessary (n = 2), unable to take analgesics (n = 1), for the memory analysis 105 patients were included and assigned to one of three groups. For the pain analysis 90 patients were included.
The groups remained the same, except for those patients who did not comply with instructions on returning the pain score lists.
View Figure 2
For the analysis of the memory function, 105 patients were included and for the pain analysis 90 patients because 15 patients did not return the VAS score lists.
Demographic data including level of education, anxiety and mean elapsed time between verbal information and interview, is displayed in Table 2.
Table 2: Demographic data, education level, anxiety and mean elapsed time between the groups. View Table 2
The mean time elapsing between receiving instructions interviewing was 21 ± 1.5 (SD) minutes. There were no significant differences between the groups.
Memory function was measured as the number of items that were spontaneously remembered, and those with a hint (Figure 3 and Table 3). The results for the spontaneous memory function were 2.8 ± 1.9 items for the standard group, 3.1 ± 1.9 items for the preoperative group and 3.7 ± 2.2 items for the postoperative group. There was a significant difference between the standard group and the postoperative group (p < 0.05).
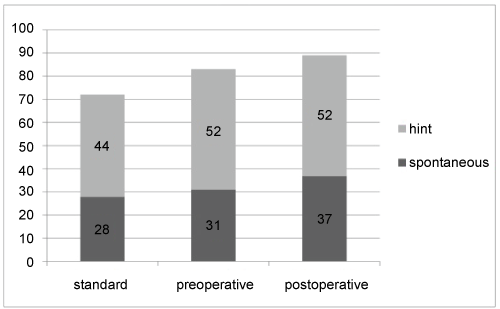 Figure 3: Memory scores in the three groups. The scores are distinguished between a spontaneous score and a score with a hint. An item remembered either spontaneous or with a hint, was awarded with 10 points.
View Figure 3
Figure 3: Memory scores in the three groups. The scores are distinguished between a spontaneous score and a score with a hint. An item remembered either spontaneous or with a hint, was awarded with 10 points.
View Figure 3
Table 3: Number of items of the patient information remembered (out of 10 presented). View Table 3
The results of the hint reproductions were 4.4 ± 1.4 items for the standard group, 5.2 ± 1.5 items for the preoperative and 5.2 ± 2.1 items for the postoperative group (not significant). For the total score (spontaneous + hint score) however, there was a significant difference between the standard group and the pre- and postoperative group, as the standard group remembered 7.2 items as compared to the 8.3 items for the preoperative and 8.9 items for the postoperative group (p < 0.001) (Kruskal-Wallis). There was a moderate positive correlation (+0.30 to +0.39) between the level of education and the memory score.
The mean level of anxiety of the groups was 41.8 ± 10.4. There were no significant differences between the groups regarding mean level of anxiety. There was no significant correlation between the preoperative anxiety and the memory score or the memory score and postoperative pain.
Pain results are presented as VAS scores on day 1, 3 and 7, duration of pain (days) and mean level of pain (Table 4). The mean level of pain is defined as the sum of all pain scores divided by the number of days patients report having pain. The only significant difference between the groups was a lower pain duration in the preoperative group (6.4 ± 4.3 days), as compared to the postoperative group (9.7 ± 5.3 days).
Table 4: Pain as VAS-scores (mean ± SD) in 90 patients who returned the VAS list. View Table 4
There was a significant, but weak, positive correlation between memory score and pain on day 1 which also proved to significantly predict pain on day 1, i.e. the more patients remember, the more pain experienced on day 1. This effect accounted for only 3% of the total pain.
This study indicates that patient instructions concerning third molar removal are best remembered when given after the surgical procedure. In accordance with this, we found a significant lower memory score in the group that received information in the treatment room just before surgery. This difference in memory may be, at least in part, due to impairment of memory during stress [15]. Stress and anxiety before dental procedures gradually climbs towards the procedure and reaches a peak minutes before and declines immediately afterwards [9]. Another study conducted at our clinic confirmed that this is also the case in surgical removal of third molars [13].
Another possible explanation why the standard group had the lowest memory imprinting may be distraction. In the operating room, distracting movements and noises (nurses unpacking surgical sets, movement of the operating chair) may impair adequate attention to what is said, therefore impairing memory imprinting.
Our study indicated that only an average of 3.2 out of the 10 items can be reproduced by the patient afterwards. To optimize information imprinting, a combination of verbal and written instructions is advocated [16].
A somewhat surprising finding was a positive correlation between recall memory score and pain on day 1. This means that the more patients remember, the more pain they experience. This opposes the finding of others [4,5,17], stating that information may lower the pain levels. An explanation may be that the information provided in this study was not targeted at coping or education regarding the pain to be experienced, but was more practical, for instance regarding wound care or what to do when a bleeding occurs. Also, some studies even implicate that preparatory information can sensitize a patient to experience more pain [3,18]. A significant difference between the groups was detected regarding pain duration with the lowest pain duration in the standard group. Perhaps the aforementioned 'sensitisation' effect plays a role i.e. patients are more aware of possible postoperative negative sequels, are triggered to experience more pain. Correlation assessments did not reveal any significant variable associated with this finding.
Strong points of our study are the group homogeneity and the similar periods between the information given and the interview. This counters the effect of difference in educational level, age, and time elapsed between the information provided and the interview on memory imprinting. Also, the use of a standardized list of information was chosen to make sure everything was explicitly mentioned.
To make the study address the 'reality' of daily practice, care was taken NOT to inform the patient that an interview was to be taken; it was only mentioned that the study was about information and pain.
A limitation of our study was that anxiety levels were not measured just before and after surgery, so that fluctuations in anxiety, and possible effects on memory imprinting, could not be assessed. Also, all patients did receive written information about their treatment after the interview (patient-folder). Although folders are only read in about 36% [17] when a patient reads the material, the imprinting of the verbally given information is 'overruled', thereby making it difficult to assess the effect of the verbally imprinting score on pain. It was not considered ethical to withhold written information from the patient, so we could not correct for this possible bias. The scores may be different when other means of information providing were explicitly addressed (instruction video, written information).
In conclusion, patient information on the postoperative course of third molar removal seems to be best remembered when given after the surgery. The timing of instructions did not affect postoperative pain.