The evidence of implant-supported restoration on patients in physical development stages is scarce and controversial. The loss of permanent teeth in children and adolescents, usually caused by trauma or agenesis, can have a negative impact on aesthetics, function, and even social acceptance. The patient presented the need for replacement of both maxillary incisors due to increased mobility and recurrent infection. Cephalometric analysis, hand, and wrist radiographs were analyzed to identify the physical development stage of the patient. Surgical and rehabilitation treatment planning was performed. Teeth extraction was performed, and thorough socket debridement followed by implant insertion with primary stability and ISQ values > 60 for both implants. Guided bone regeneration was performed to fill the peri-implant gap and immediate loading was performed. The patient's natural teeth were used to create the provisional screw-retained crowns. The permanent restorations were delivered one year after the assessment of undisturbed skeletal growth. The scientific literature on the subject is limited, therefore, the development of clinical guidelines and recommendations are required to increase predictability. Patient periodic monitoring treatment, including adjustments to the implant-supported prostheses, is mandatory to ensure implant success. There is no sufficient evidence to contraindicate this procedure, nevertheless, dental clinicians should not contraindicate implant placement in contrast to the benefits of esthetics, function, and patient self-esteem.
Adolescents, Dental implants, Provisional restoration, Immediate dental implant loading, Esthetic dentistry
ISQ: Implant Stability Quotient is an objective world standard for measuring implants stability. The clinical range of ISQ is normally 55-80; GBR: Guided Bone Regeneration; CBCT: Cone Beam Computarized Tomography; CAD-CAM: Computed Aided Design-Computed Aided Manufacturing
The loss of permanent teeth in children and adolescents, usually caused by trauma or agenesis, can have a negative impact on aesthetics, function, and even social acceptance. A conservative prosthetic rehabilitation may be the ideal approach in a patient going through physical development, but it may not meet the patient's needs. Dental implants have been proposed as an alternative to tooth-supported fixed or removable restorations with variable short and long-term follow up outcomes [1-3].
The use of a cephalometric analysis, hand and wrist radiographs have been recommended to determine skeletal maturity and confirmation of the physical development stage before the dental implant is placed, skeletal mature is desired to minimize infraocclusion [4]. The objective of this analysis is to determine the skeletal age; the osseous structure in the hand and wrist region is made of several small bones. This tool provides a useful means of assessing osseous maturity [5].
These risk factors and implant therapy techniques have to be taken in consideration due to the current criteria for successful implant therapy, which is not only to achieve osseointegration but the harmonious integration with gingival tissues that surround the final prosthetic rehabilitation [6,7].
Careful treatment planning must be executed to acquire positive hard and soft tissue architecture that array implant aesthetics. The following prerequisites should be considered: Proper prescription of systemic antibiotics, use of an oral rinse before and after surgery, thorough debridement of the extraction sockets, and effective load management of interim and final restorations [8,9]. The aim of this study is to show the immediate implant placement and their rehabilitation to replace the central incisors of an adolescent due to the poor prognosis of both teeth.
A 14-year-old female patient was clinically evaluated and presented the mobility of both maxillary incisors and was diagnosed as an endodontic-periodontal lesion due to recurrent infection (Figure 1).
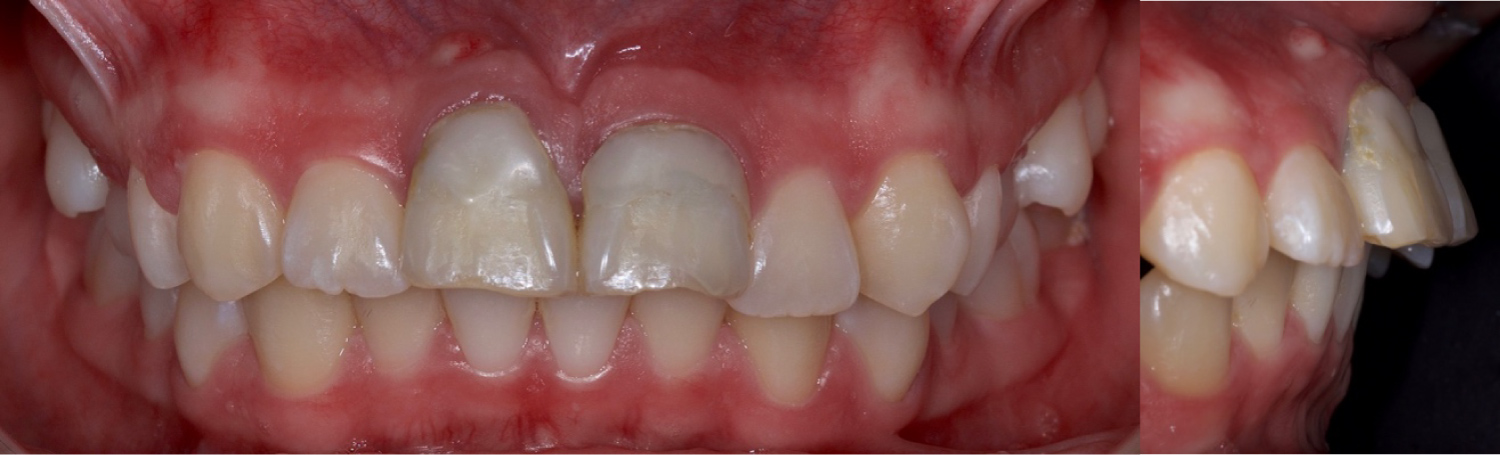 Figure 1: Initial view (A) Frontal view; (B) Sagittal view.
View Figure 1
Figure 1: Initial view (A) Frontal view; (B) Sagittal view.
View Figure 1
An extensive oral examination was conducted on the patient full periodontal probing, phenotype evaluation, and a cone-beam computed tomography scan for precise assessment of the bone quality and quantity, and its relation with the root of each tooth. In addition, CBCT cross sectional evaluation of both central incisors was made (Figure 2).
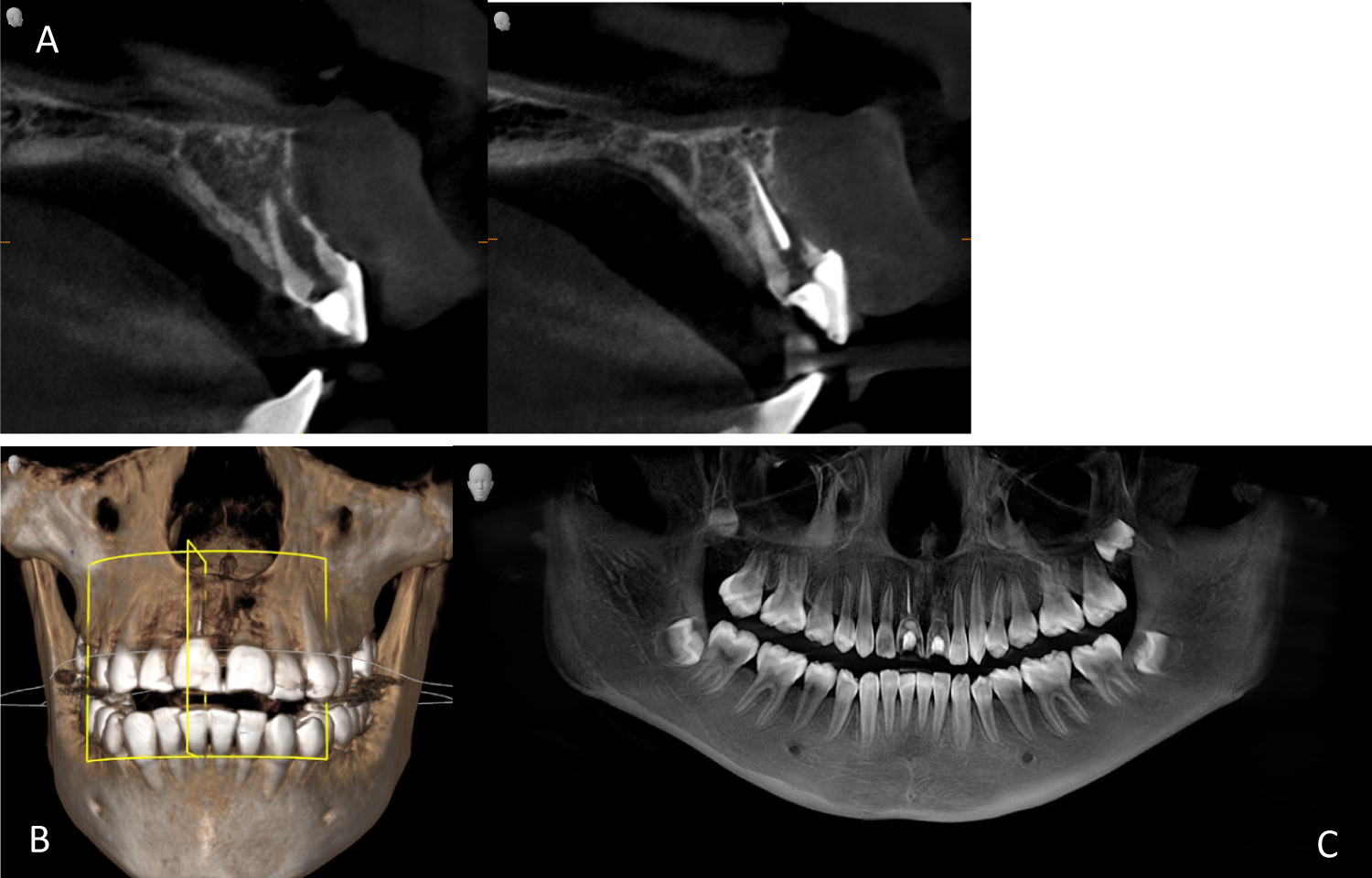 Figure 2: CBCT (A) Cross sectional of both central incisors; (B) Volumetric CBCT view; (C) Panoramic CBCT view.
View Figure 2
Figure 2: CBCT (A) Cross sectional of both central incisors; (B) Volumetric CBCT view; (C) Panoramic CBCT view.
View Figure 2
Additionally, cephalometric analysis and hand/wrist radiographs were analyzed to identify the physical development stage of the patient and correlate them to the chronological age. (Once skeletal maturity was assessed and appropriate surgical and prosthetic treatment plan was outlined, surgical procedure could be performed) (Figure 3).
 Figure 3: (A) Lateral radiograph; (B) Hand and wrist radiography; (C) Cephalometric analysis.
View Figure 3
Figure 3: (A) Lateral radiograph; (B) Hand and wrist radiography; (C) Cephalometric analysis.
View Figure 3
Skeletal growth status can be appraised fairly accurately by comparing a conventional radiograph of the hand and wrist against a standardized atlas of hand and wrist bone development. Hand wrist radiograph indicators can be used to place a patient in the general area of the growth curve. Capping of the middle phalanges of the third finger (MP3cap) usually occurs after maximum growth velocity is completed and indicates a deceleration in the pubertal growth spurt. Once pubertal growth is completed, consideration of implant placement can begin. However, some risks still exist. When epiphysis of the radius fuses and forms a bony union with the diaphysis, the adult level of skeletal growth has been attained and no further increase in structural height can be expected [10].
The long-term prognosis was hopeless for both teeth, therefore were indicated for extraction. Occlusion analysis of the position of the teeth and their current relation with the opposing arch was evaluated to be able to develop provisional and final restorations.
Three days before surgery the patient has prescribed a dose of 875 mg of amoxicillin, and 125 mg of clavulanate acid every 12 hours for 7 days and she was indicated to rinse for 1 minute using oral chlorhexidine 0.12% three times a day every 8 hours to minimize oral bacterial load for 21 days.
Local anesthesia was delivered with 4% articaine with adrenaline 1:100,000 in the infraorbitary and nasopalatine nerves as well as local infiltration immediate to each tooth. Once anesthesia was achieved, extraction of the teeth followed using an atraumatic technique with the help of periotomes using a flapless approach.
After the teeth were extracted, thorough debridement of the extraction sockets was accomplished using surgical curettes and a Hirschfeld file with copious irrigation (Figure 4).
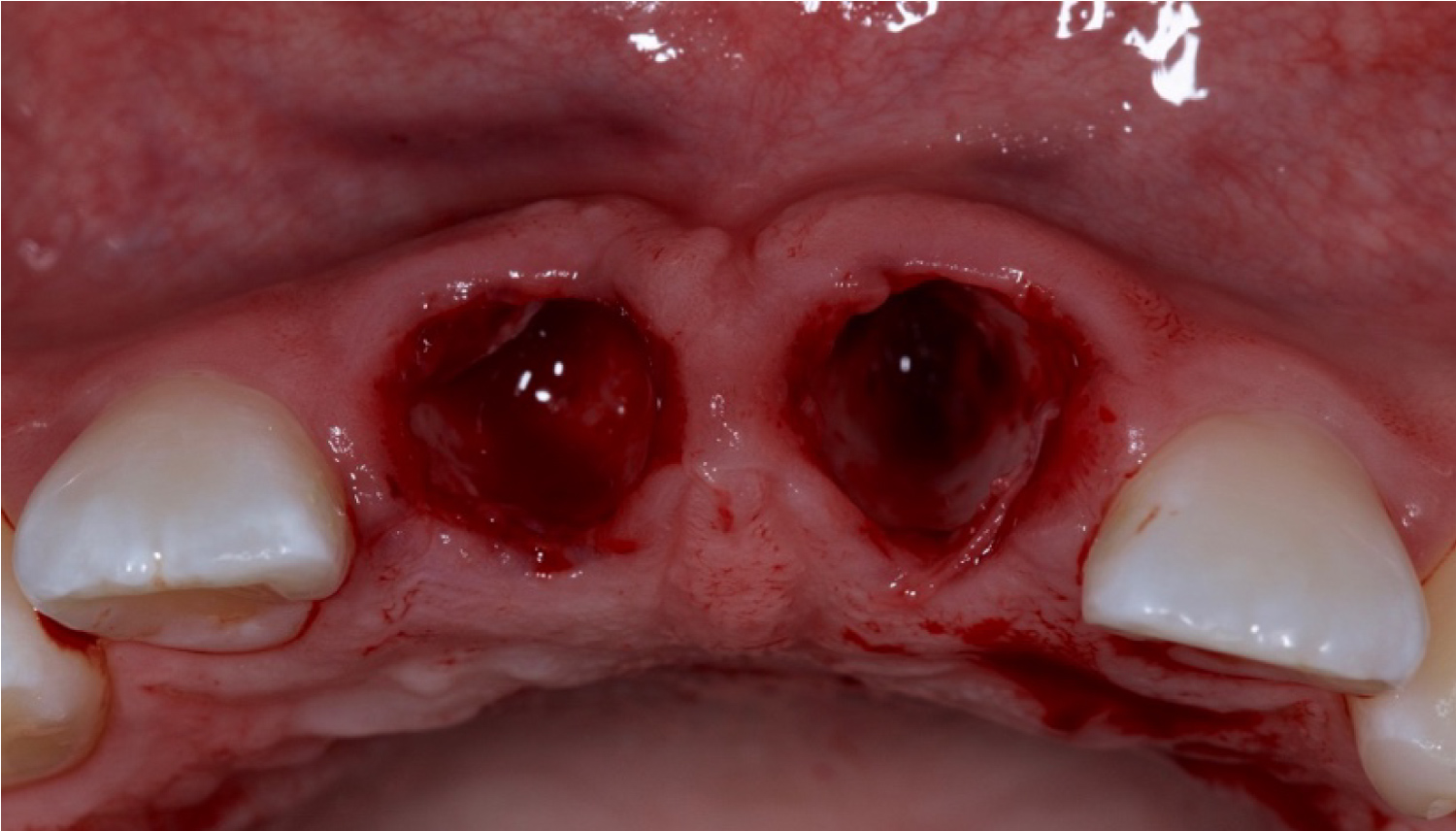 Figure 4: Post-extraction alveolar socket.
View Figure 4
Figure 4: Post-extraction alveolar socket.
View Figure 4
A duplicate of the study model was obtained which was used to fabricate a surgical guide using a 0.80 caliber rigid acetate sheet to perform the drilling protocol at the cingulum level of the adjacent teeth, allowing a three-dimensional positioning of the implant ensuring correct emergence profile and screw access hole for provisional and final restoration. The dental implant system used was ADIN (Touareg™ - OS), two 4.2 × 11.5 mm conical, self-tapping implants were used with an OsseoFix™ surface treatment, a high purity surface with calcium phosphate with a roughness that favors primary stability and increases the implant-bone interface.
The implant insertion was according to the manufacturer's proposed protocol for drilling sequence with a minor modification using one less bur to under prepare the osteotomy site to improve anchorage and primary stability for the implants. The implants were placed in the prepared site toward the palatal wall of the extraction sockets to a depth of 3 mm from the free gingival margin and their final fit was assured to 40N cm and measured the ISQ for each implant. ISQ values for both were ISQ 67, for the right incisor and ISQ 69 for the left incisor (Figure 5).
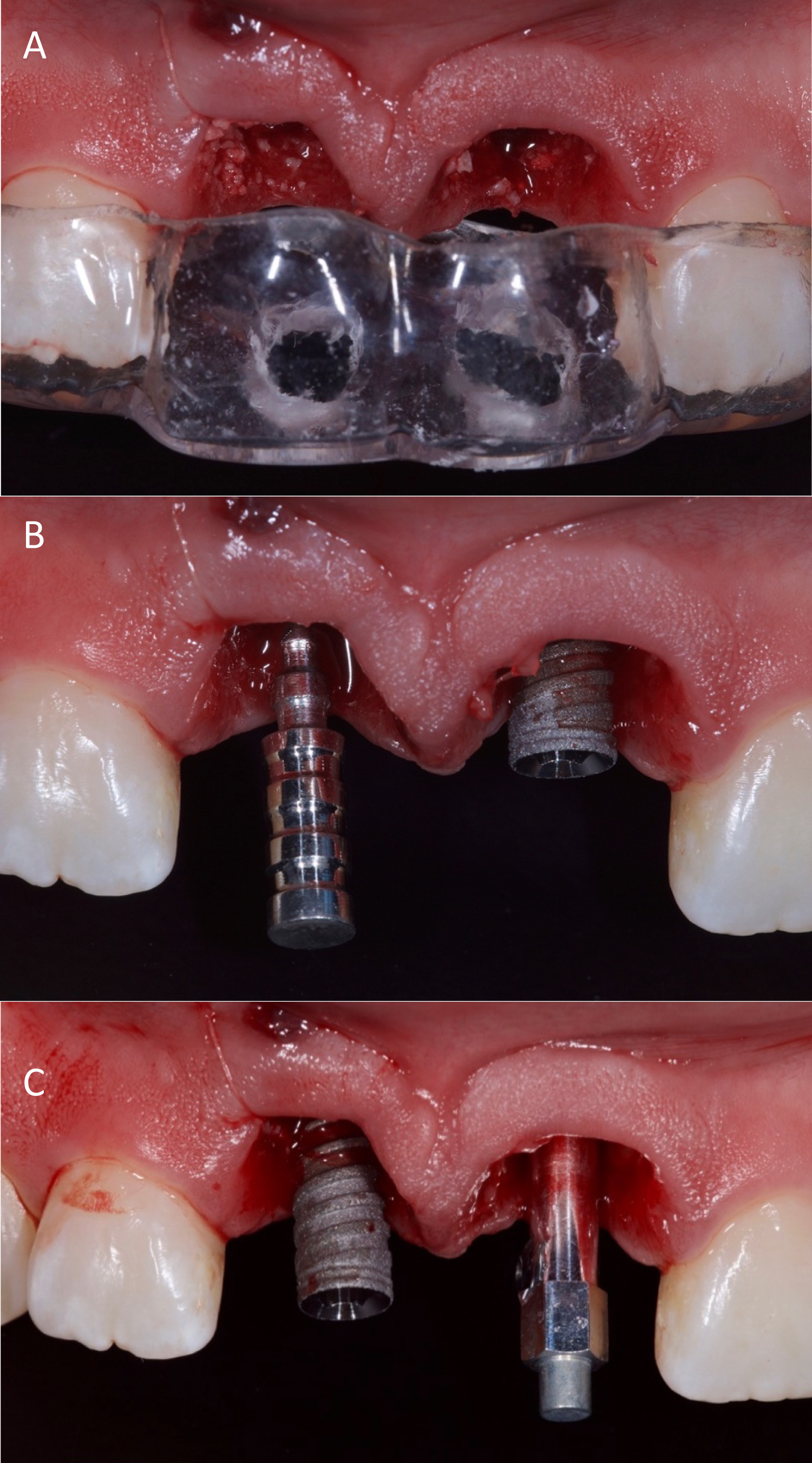 Figure 5: (A) Surgical guide; (B) Implant placement and parallelism verification; (C) Implant placement and ISQ measurement.
View Figure 5
Figure 5: (A) Surgical guide; (B) Implant placement and parallelism verification; (C) Implant placement and ISQ measurement.
View Figure 5
The distance between the implant platform and the marginal soft and hard tissue supported the decision to graft the alveolus using synthetic porous hydroxyapatite 50-50 mixture with autologous bone graft harvested with the burs during the drilling sequence. This graft mixture was placed in the alveolar-implant gap surrounding the implant. (Figure 6).
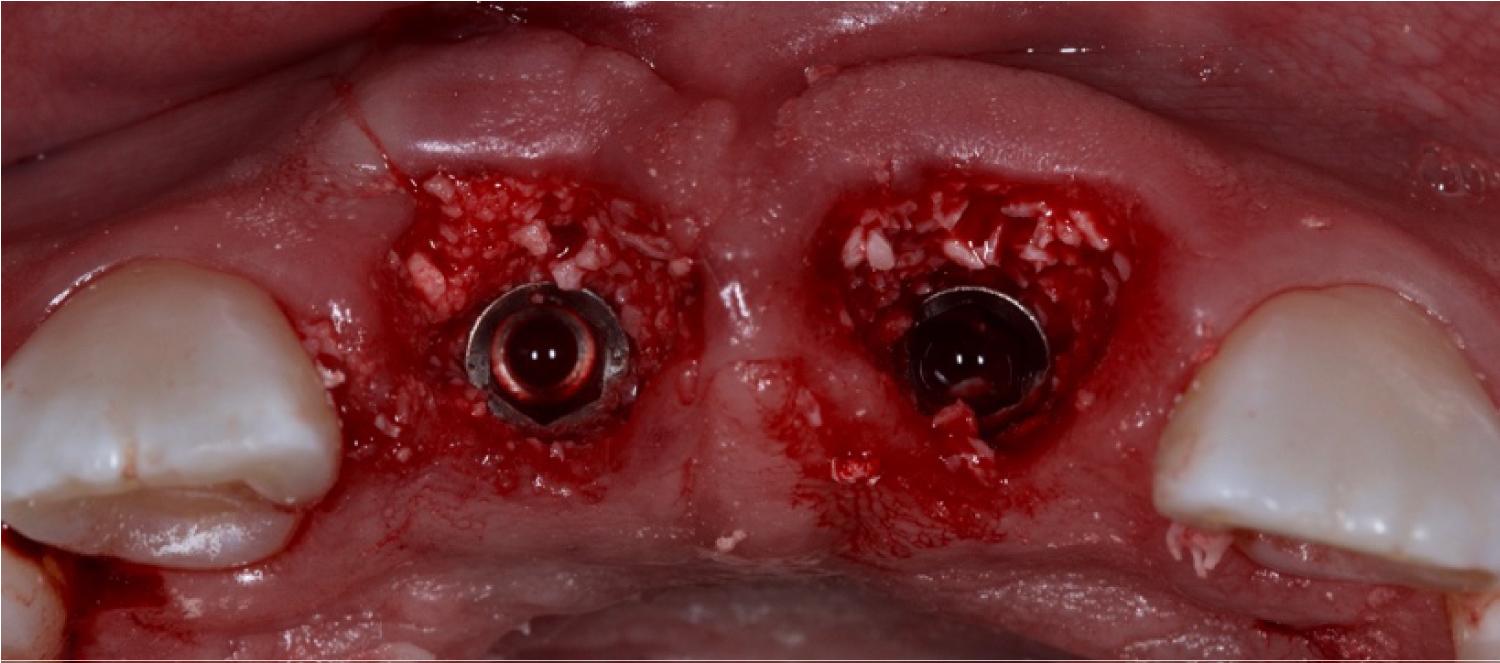 Figure 6: Guided bone regeneration and implants in place.
View Figure 6
Figure 6: Guided bone regeneration and implants in place.
View Figure 6
The extracted crowns of both maxillary incisors were used as the provisional restorations to develop soft tissue architecture that was almost identical to the patient's original. The crown and partial root of the extracted tooth was trimmed to a subgingival length of 3 mm, and an ovoid pontic base created using provisional composite resin and temporary plastic abutments. The restorations were inserted and torqued to 15N cm for the final seating with a calibrated torque adjustable wrench, and the occlusion was checked to avoid contact with the opposing arch (Figure 7).
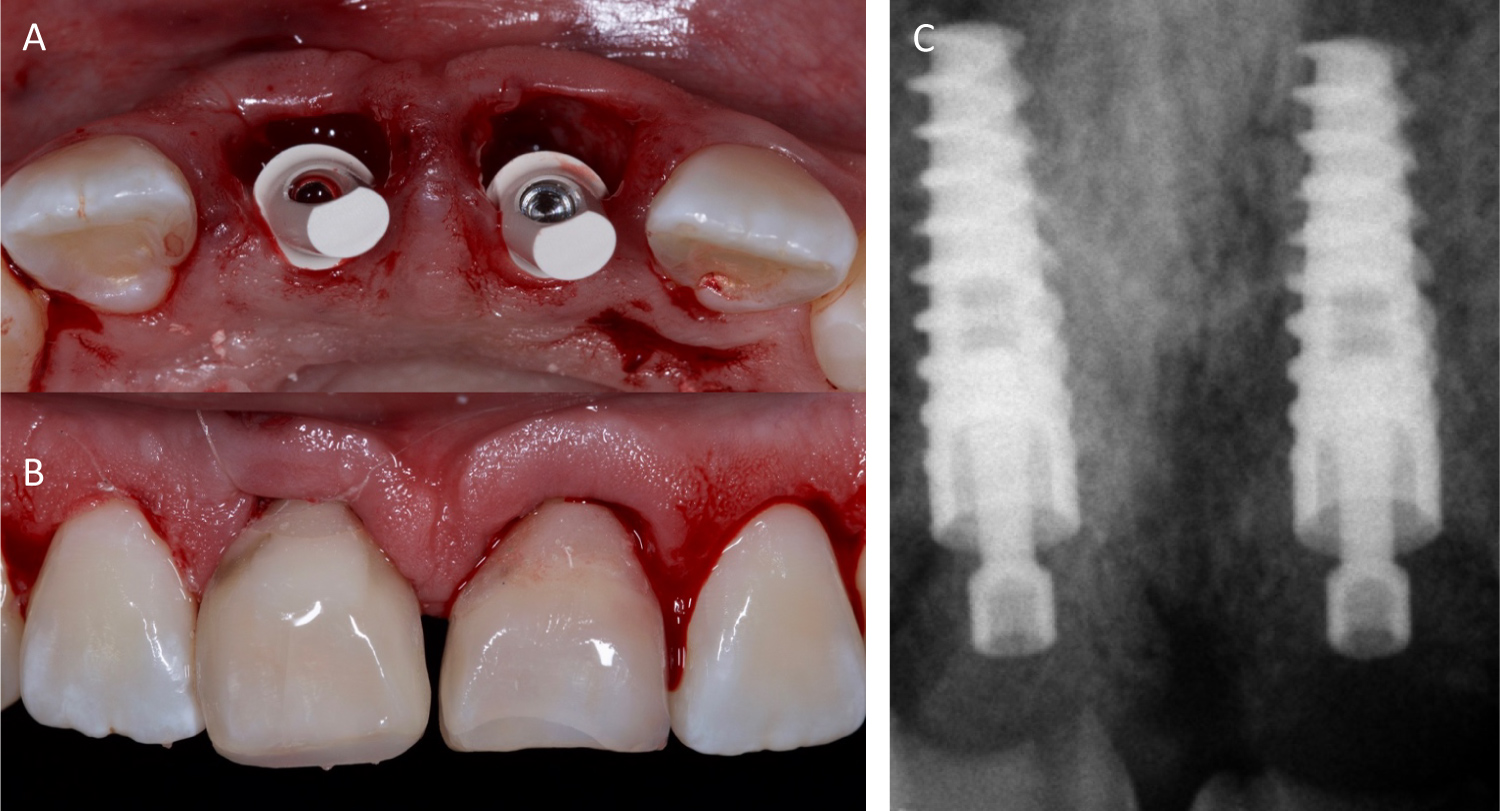 Figure 7: (A) Peek abutments for provisional screw-retained restorations; (B) Natural teeth employed for provisional screw-retained restorations; (C) Periapical radiograph to assess correct seating.
View Figure 7
Figure 7: (A) Peek abutments for provisional screw-retained restorations; (B) Natural teeth employed for provisional screw-retained restorations; (C) Periapical radiograph to assess correct seating.
View Figure 7
The patient was instructed to maintain a liquid diet for the first three days after the surgery and a soft diet during the next three weeks. She was also instructed to refrain from chewing on the implant-provisional retained esthetic zone for the following 12 weeks. The patient was called upon every week for the first month and every two weeks for the following month.
Before final restorations, follow up CBCT scans were instructed for implant assessment and their relation within the anterior maxillary ridge (Figure 8).
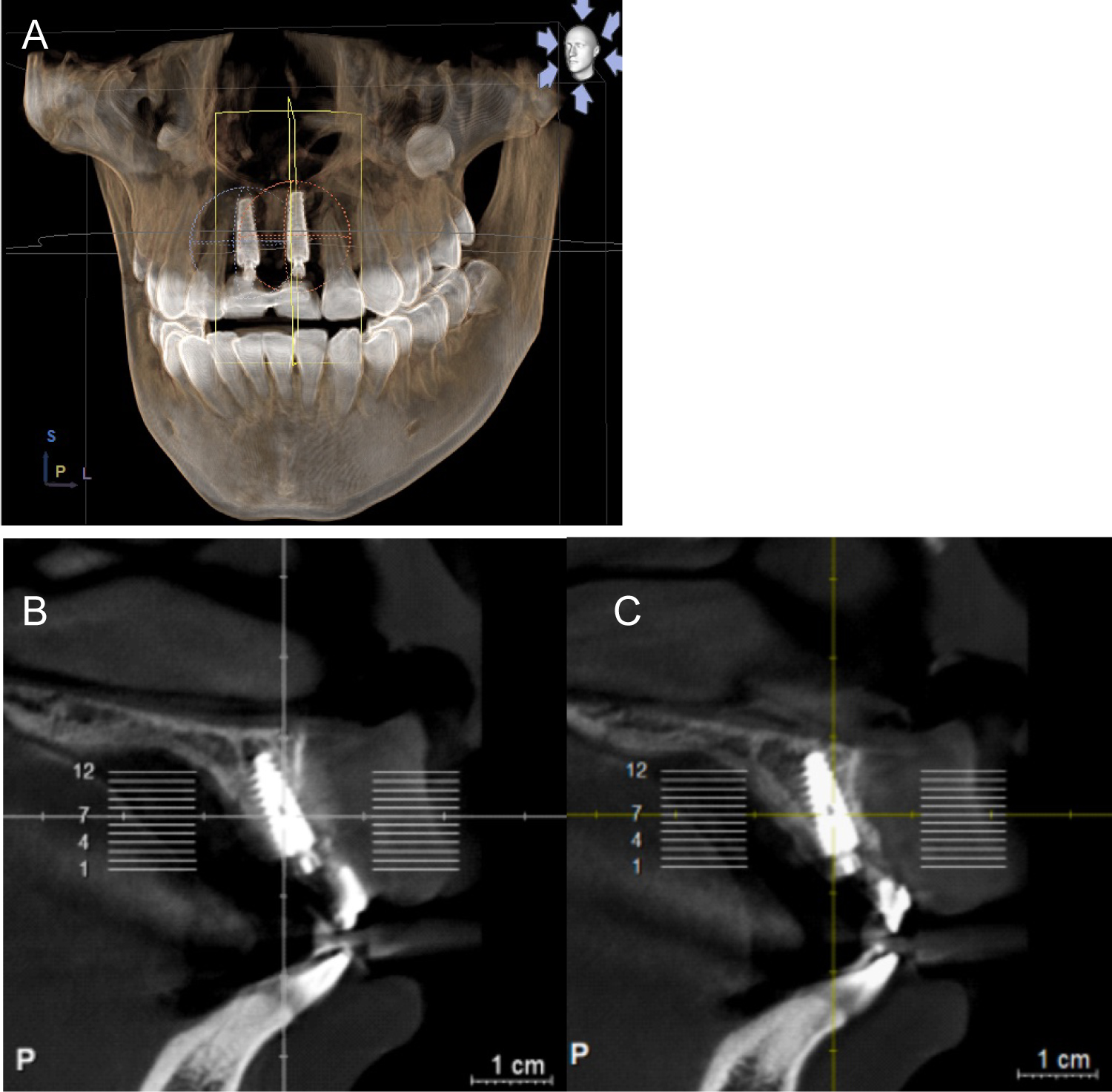 Figure 8: (A) Volumetric CBCT; (B) Sagittal view implant right incisor; (C) Sagittal view implant left incisor.
View Figure 8
Figure 8: (A) Volumetric CBCT; (B) Sagittal view implant right incisor; (C) Sagittal view implant left incisor.
View Figure 8
The final restorations were delivered one year after the assessment of undisturbed skeletal growth. Screw retained lithium disilicate crowns were fabricated by CAD-CAM without complications and in compliance with the patient's aesthetic and functional expectations (Figure 9 and Figure 10).
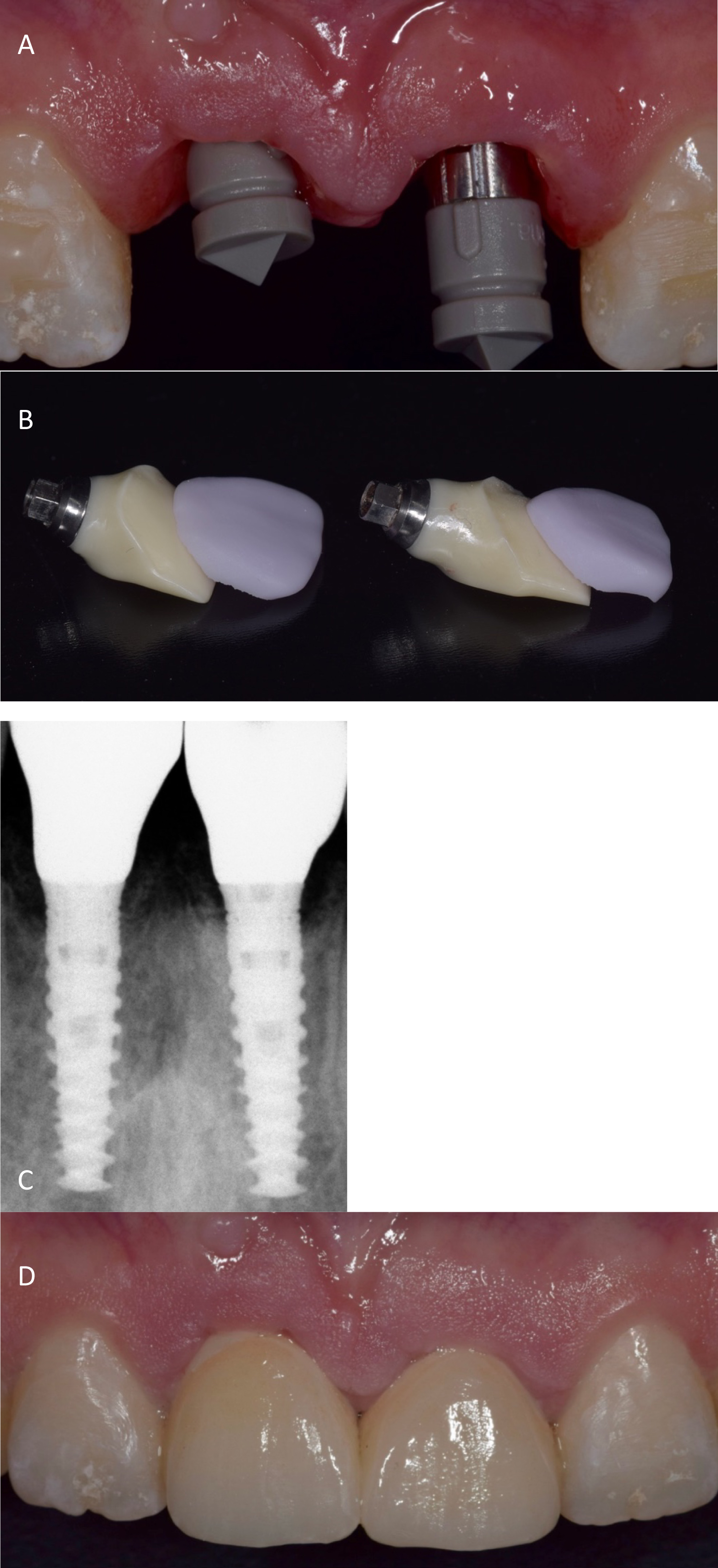 Figure 9: (A) Scan body and scan post in place for digital impression; (B) CAD-CAM milled restoration; (C) Final restoration; (D) Periapical radiography.
View Figure 9
Figure 9: (A) Scan body and scan post in place for digital impression; (B) CAD-CAM milled restoration; (C) Final restoration; (D) Periapical radiography.
View Figure 9
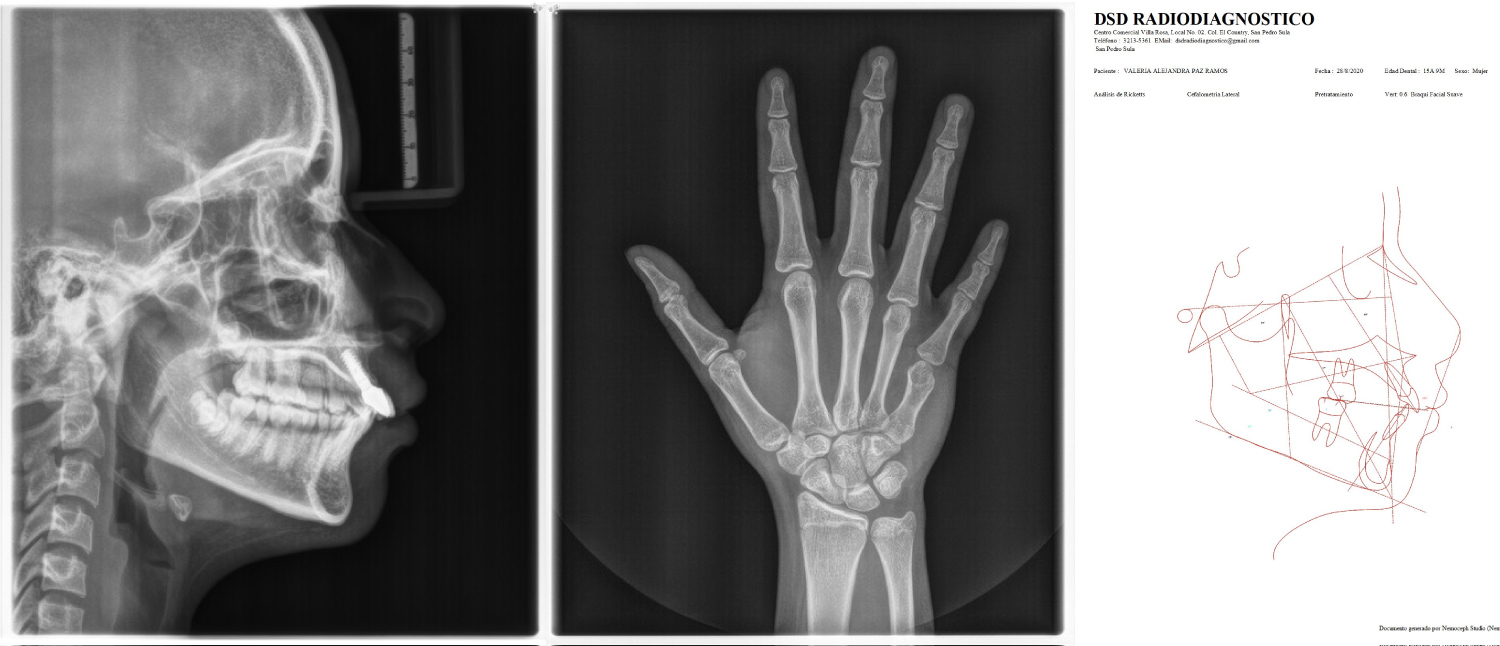 Figure 10: (A) Lateral radiograph; (B) Hand and wrist radiography; (C) Cephalometric analysis.
View Figure 10
Figure 10: (A) Lateral radiograph; (B) Hand and wrist radiography; (C) Cephalometric analysis.
View Figure 10
After immediate implant placement, structural changes of the soft tissue contour are ongoing and cannot be completely avoided [11].
Flapless approach and immediate loading have also been recommended to minimize the amount of ridge contour change [12].
According to several studies of type 1 implant placement, the greatest dimensional change of soft tissue occurs within the first three months of surgery. The protocol of the present study using flapless tooth extraction with a bone substitute in the jumping gap plus immediate loading benefits the preservation of the peri-implant tissue [13-15].
The use of dental implants in children and adolescents is susceptible to surgical and prosthetic complications during the physical development stages. These are mostly related to the growth of the maxilla and mandible, which can lead to changes in the position of the implant in both vertical and horizontal directions and must be considered in treatment planning.
Despite these complications, rehabilitation with dental implants has been considered a controversial but reliable treatment option for adolescents [16,17]. Implant-supported prostheses are well-accepted by young patients and may benefit from the blood supply and uncomplicated healing provided by growing bone.
To date, there is no consensus about the ideal age, positioning, or the number of implants that are required for safe treatment. Clinicians must be aware of the limitations and possible complications related to placing implants in these patients [18]. Anterior implant esthetics is one of the most challenging tasks in implant dentistry, and a proper soft tissue contour is difficult for any clinician to achieve.
The use of the patient's natural tooth will allow a reproducible interproximal contact and proper shaping of the soft tissues, relative tooth position is kept, the form of the periodontium is modeled based on the patient's natural tooth, the original tooth shape is retained and the position of the crestal bone can be kept high with an immediately placed implant [19].
To use the crown of the extracted natural tooth as an immediate implant-retained provisional restoration helps to maintain soft tissue contour after extractions, reaching satisfactory outcomes in the emergence profile. In this clinical report, crowns of the natural teeth were used as provisional screw-retained restorations to improve the soft tissue contour, however, implants must be placed in a specific position to allow access hole orientation to be placed in the cingulum of the provisional crown; and benefit from the technical and biological advantages exhibited by screw-retained prostheses.
Additionally, bone augmentation and soft tissue presented stability at both implant sites. Also, regarding the shape and color of the gingival tissues and restoration throughout the provisional phase was well tolerated by the patient and fulfilled expectations during the treatment and as an outcome.
A follow-up was carried out one year after the definitive restoration. By detailed analysis of the CBCT scans, no changes were found in the position of the implant platform in the maxilla or in relation to the adjacent teeth. Only one year of follow-up is a limitation of this report; therefore, a clinical and radiographic evaluation should be performed every year to confirm that there is no movement of the implants.
Post-extraction dental implant placement and immediate loading of them in adolescent patients could be an alternative in cases where aesthetics, function, and self-esteem are severely compromised. However, long-term studies are required, to increase predictability. As authors, we expect to present long-term outcomes of this patient in the next 5-10 years after the patient has completely finished developmental growth.