Premenstrual asthma (APM) is often confused by the patient and/or doctor with the symptoms of asthma in general. The purpose of our study is to investigate the clinical and spirometric characteristics of APM.
Prospective descriptive study from 2011 to 2017, on 95 non-menopausal asthma patients, divided into 2 with and without APM. They benefited on a single menstrual cycle of spirometry during the follicular phase, luteal and premenstrual and cutaneous tests.
APM is found in 42.1% of cases. It is more common between 16-35 years old. The main symptom is dyspnea in 97.5% of cases. Premenstrual syndrome is present in 92.5% of APM. No relationship was found between the severity of asthma and APM (P = 0.41). In contrast, uncontrolled asthma is more common in women with APM (75%). No difference in the spirometry of the 3 phases of the cycle between the 2 groups. In case of APM, the CV is higher during the luteal and premenstrual phases and the PEF is decreased during the premenstrual phase and this in 60% of the cases.
The results on a single menstrual cycle reinforce the hypothesis of the role of sex hormones in APM.
Asthma, Woman, Menstrual cycle, Sex hormones
Premenstrual asthma (APM) is defined by the exacerbation of asthma before menstruation [1], requiring fast-acting beta 2 mimetics [2]. Some authors have reported a third diagnostic element is the drop in the DEP of more than 20% premenstruation [3]. APM is often confused by the patient and/or doctor with the symptoms of asthma in general. The purpose of our study is to investigate the clinical and spiometric characteristics of APM.
It is a prospective descriptive study from 2011 to 2017, on 95 patients with non-menopausal asthma, divided into 2 groups according to the presence or absence of premenstrual asthma (APM). These patients are aged between 16 and 55-years-old. They benefited on a single menstrual cycle, spirometry during the follicular phases (between the 3rd and 5th day), luteal (between the 19th to 21st day) and premenstrual (between the 26th and 28th day). Skin tests were done for the most common allergens. We excluded from this work the comorbidities that can influence asthma such as heart disease. Premenstrual asthma was defined as the onset or worsening of asthma symptoms in the last week before menstruation [4]. The exploitation of the results made use of the software Epidata analysis and epi-info 6.
Premenstrual asthma was found in 40 patients (42.1%). It is more common between 16 and 35 years of age (Figure 1) with an average age of 34.78 ± 8.97 years (Table 1). There was no significant difference in average age between those who have and those who do not have premenstrual asthma (Table 1).
Table 1: Clinical characteristics of the two groups. View Table 1
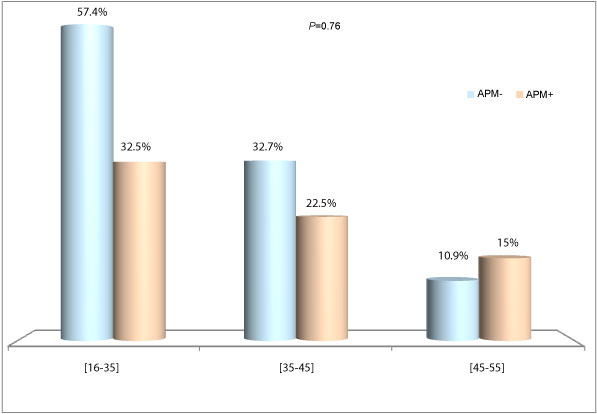 Figure 1: Premenstrual asthma according to age groups.
Figure 1: Premenstrual asthma according to age groups.
(APM +: With premenstrual asthma, APM-: Without premenstrual asthma).
View Figure 1
The symptoms of premenstrual asthma are represented almost exclusively by an increase in dyspnea requiring beta2 mimetics in 97.5% of cases (Figure 2).
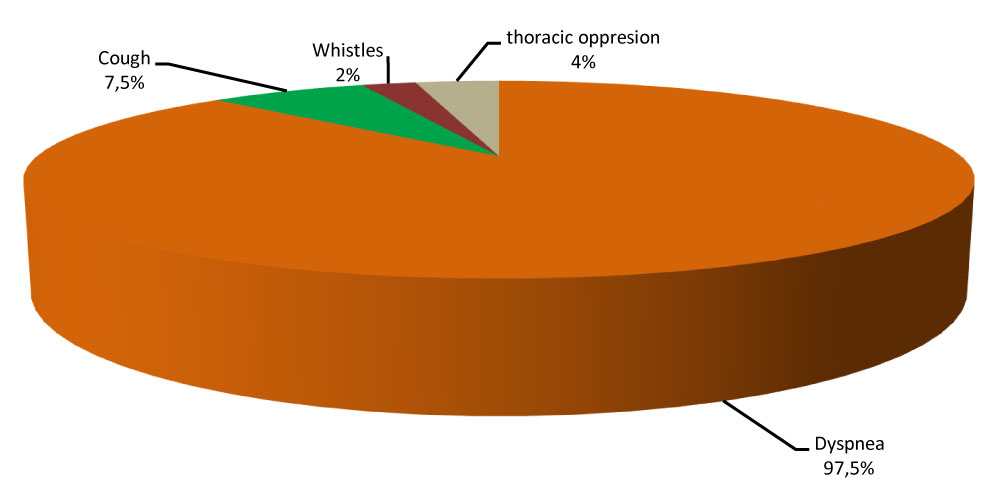 Figure 2: Respiratory Symptoms in premenstrual asthma.
View Figure 2
Figure 2: Respiratory Symptoms in premenstrual asthma.
View Figure 2
Regarding the number of symptoms in premenstrual asthma, the majority of asthmatics had only dyspnea in 85% (Figure 3).
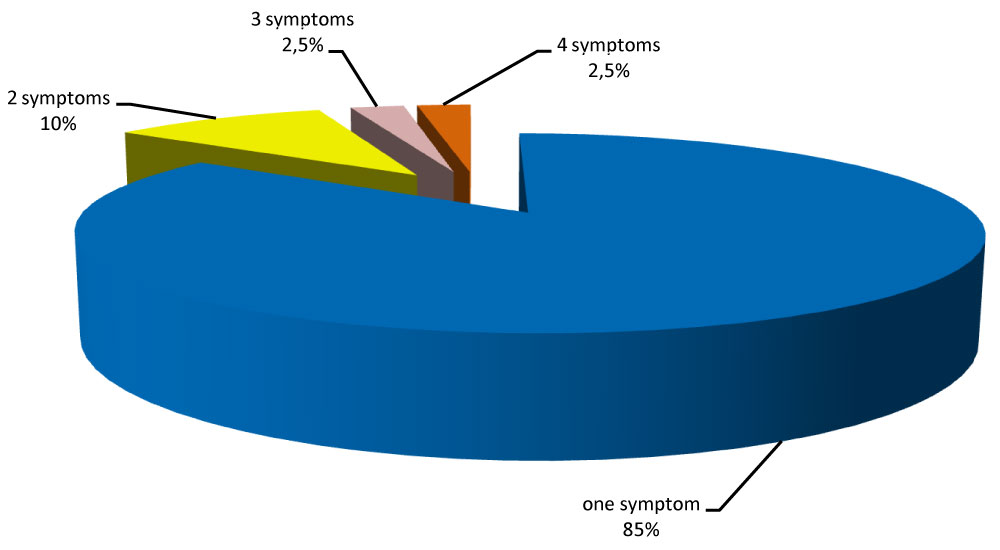 Figure 3: Number of symptôms in premenstrual asthma.
View Figure 3
Figure 3: Number of symptôms in premenstrual asthma.
View Figure 3
Premenstrual syndrome is present in almost all patients with premenstrual asthma (92.5%). As for premenstrual dysphoric syndrome, it is uncommon. It is found in 16.2% of cases.
Like premenstrual asthma, premenstrual syndrome is more common in young women under 35 in 56.4% of cases. Women in the age group [35-45] and those aged 45-55 reported premenstrual symptoms of asthma in 30.7% and 12.8% respectively.
All symptoms of premenstrual syndrome are common in premenstrual asthma with headache irritability in 87.5% of cases (Figure 4).
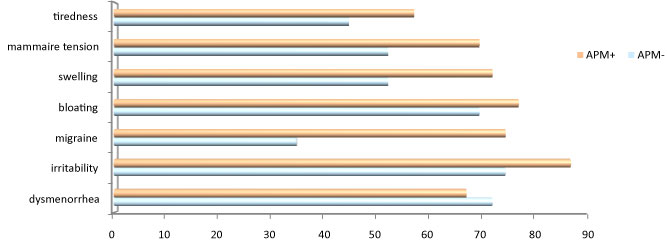 Figure 4: Symptoms fréquency of premenstrual syndrome.
Figure 4: Symptoms fréquency of premenstrual syndrome.
(APM +: with premenstrual asthma, APM-: without premenstrual asthma).
View Figure 4
Women with premenstrual asthma were overweight with an average BMI of 26.63 ± 5.24 kg/m2 but no difference with those without premenstrual asthma (p = 0.39) (Table 1).
There was no difference between women with and without premenstrual asthma regarding smoking exposure, co-morbidities and intensity of physical activity (Table 1).
- Asthma started after puberty in most women with or without premenstrual asthma (Figure 5).
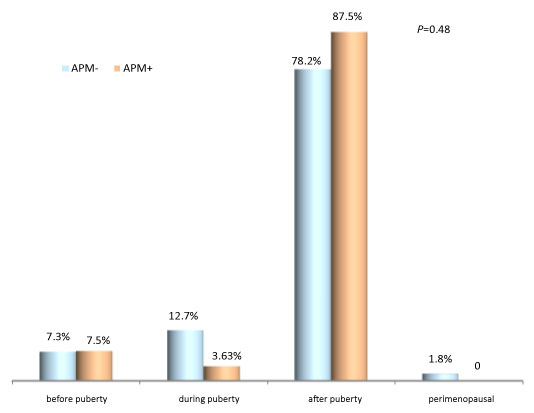 Figure 5: The period of asthma beginning.
Figure 5: The period of asthma beginning.
(APM +: With premenstrual asthma, APM-: Without premenstrual asthma).
View Figure 5
The duration of asthma is 8.88 ± 8.85 years in the presence of premenstrual asthma and is 8.4 ± 9.05 years in the absence of premenstrual asthma (p = 0.79).
-Asthma severity: Patients with premenstrual asthma have moderate asthma in 52.5% and mild in 35% of cases. Severe asthma is uncommon (Figure 6).
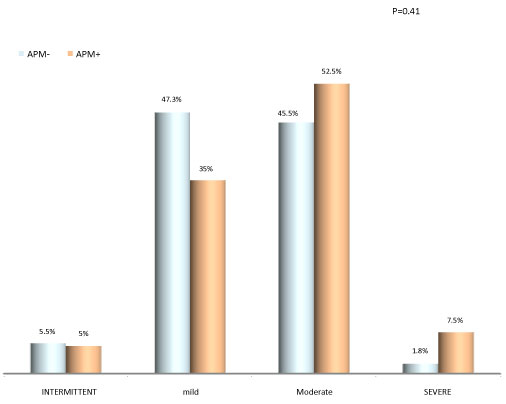 Figure 6: Asthma severity with and without premenstrual asthma.
View Figure 6
Figure 6: Asthma severity with and without premenstrual asthma.
View Figure 6
Uncontrolled asthma was observed in 3/4 of patients with premenstrual asthma and just over ½ of patients without premenstrual asthma (p = 0.02) (Figure 7).
 Figure 7: Asthma control with and without premenstrual asthma.
Figure 7: Asthma control with and without premenstrual asthma.
(APM +: with premenstrual asthma, APM-: without premenstrual asthma).
View Figure 7
The concept of familial atopy, the combination of rhinosinusitis and/or other types of skin, food or drug allergies are identical in groups with and without premenstrual asthma. There was no difference in skin test results with or without premenstrual asthma. (Table 2).
Table 2: Allergy and cutaneous tests with and without premenstrual asthma. View Table 2
In addition, patients with premenstrual asthma have a higher risk of premenstrual syndrome and premenstrual dysphoric syndrome. In addition, they are 4 times more likely to have allergic conjunctivitis (Table 3).
Table 3: Risque factor of premenstrual asthma. View Table 3
The comparison of spirometers during different phases of the menstrual cycle between groups of asthma with and without premenstrual asthma, did not find any significant difference.
The only difference found in premenstrual asthma is CV, which is higher during the two luteal and premenstrual phases compared to the follicular phase (Table 4). On the other hand, the comparison of the last two luteal and premenstrual phases only shows a significant decrease in DEP and DEM25 during the premenstrual phase compared with the luteal phase (Table 5).
Table 4: Spirometry results of 3 menstrual cycle phases in premenstrual asthma. View Table 4
Table 5: Spirometry results of the 2 late menstrual cycle phases in premenstrual asthma. View Table 5
This decrease in PEF was observed in 23 patients with premenstrual asthma (60% of cases). It is estimated at 0.52 l/s, which corresponds to an average decrease of 8.44% in DEP during the premenstrual phase.
Premenstrual asthma was found in 40 patients with asthma among the 95 premenopausal patients (42.1%). It is less common than in the Vega series [5] which published the highest rate of 52.54%. The incidence of premenstrual asthma is higher in women younger than 35 (32.5%), but tends to decrease with age. The average age is 34.78 years almost identical to that reported by SABRY [6] and RAO [7]. In contrast, Shames and Thornton found a higher incidence of premenstrual asthma in peri-menopausal women [1,8].
The symptoms of premenstrual asthma are variable. In our series, premenstrual asthma was expressed only by respiratory discomfort in 85% of cases. This result is close to that of AGARWAL who studied the different symptoms in premenstrual asthma. He found dyspnea in 96% with wheezing in 52% of cases, chest tightness in 43% of cases, cough in 39% of cases and sputum in 13% of cases [9].
Most patients with premenstrual asthma have moderate asthma in 52.5% of cases, or mild in 35% of cases. There was no high incidence of severe asthma in asthmatics with premenstrual asthma (7.5%). The same finding was reported by VEGA [5]. In contrast, Rao reported severe asthma in 50% of women with premenstrual asthma [7]. Several other studies have found a link between premenstrual asthma and the severity of asthma [6,8,10,11].
In addition, premenstrual syndrome in our series is present in almost all patients with premenstrual asthma (92.5%). The frequency of premenstrual syndrome observed in our series is close to that of Dorhofer [12] but higher than that reported by ENSOM [13] and Vega [14]. Skrzypulec found a low incidence of this syndrome in adolescent asthmatics (20%) compared with non-asthmatics (46.67%) [15].
In our series, premenstrual syndrome is statistically significantly associated with uncontrolled asthma (85.2%). This frequent association suggests a common mechanism of occurrence of these two entities including the psychic component which has been frequently found in the literature as a factor associated with premenstrual asthma [12], as is premenstrual syndrome [16]. Although the psychic component was not studied in this work, the irritability marking the premenstrual syndrome in 87.5% of patients could cause a suspicion of a psychic cause in the occurrence of premenstrual asthma.
The symptoms of premenstrual asthma are accompanied by a significant increase in VC from the follicular phase to the premenstrual phase. Knowing that progesterone increases during the luteal phase and reaches its maximum in pre-menstruation, the increase in ventilation represented by an increase in VC is most likely related to the increase of this hormone [17].
On the other hand, the analysis of the last two phases of the cycle during which patients are symptomatic, found low levels of PEF in 60% of cases. In the literature, low levels of DEP in pre-menstruation were reported by OGUZULGEN [18], KAUR [19] and MURPHY [20] while ARORA found significantly elevated flow and volume values during the luteal phase, compared to the premenstrual phase [21].
This suggests that the anti-inflammatory effect of estradiol at normal levels [22] can become pro-inflammatory at high levels [23,24]. These elevated levels observed during the luteal and even premenstrual phase may be responsible for bronchial obstruction marked by a decrease in PEF during premenstrual asthma.
Variations in the symptoms of asthma and respiratory function during the menstrual cycle strongly suggest the role of sex hormones on the bronchial tree. Although the mechanism of action of the sex hormones on the woman's respiratory system is unclear, premenstrual asthma, which is felt subjectively in 42.1% of our patients, is of particular interest, especially since the prevalence of asthma is increasing in the world.